Abstract
Background and Aims:
Unsatisfactory weight loss after gastric bypass or sleeve gastrectomy in super-obese patients (body mass index > 50) is a growing concern. Biliopancreatic diversion with duodenal switch results in greater weight loss, but is technically challenging to perform, especially as a laparoscopic procedure (Lap-DS). The aim of this study was to compare perioperative outcomes of Lap-DS and the corresponding open procedure (O-DS) in Sweden.
Material and Methods:
The data source was a nationwide cohort from the Scandinavian Obesity Surgery Registry and 317 biliopancreatic diversion with duodenal switch patients (mean body mass index = 56.7 ± 6.6 kg/m2, 38.4 ± 10.2 years, and 57% females) were analyzed. Follow-up at 30 days was complete in 98% of patients.
Results:
The 53 Lap-DS patients were younger than the 264 patients undergoing O-DS (35.0 vs 39.1 years, p = 0.01). Operative time was 163 ± 38 min for lap-DS and 150 ± 31 min for O-DS, p = 0.01, with less bleeding in Lap-DS (94 vs 216 mL, p < 0.001). There was one conversion to open surgery. Patients undergoing Lap-DS had a shorter length of stay than O-DS, 3.3 versus 6.6 days, p = 0.02. No significant differences in overall complications within 30 days were seen (12% and 17%, respectively). Interestingly, the two leaks in Lap-DS were located at the entero-enteric anastomosis, while three out of four leaks in O-DS occurred at the top of the gastric tube.
Conclusion:
Lap-DS can be performed by dedicated bariatric surgeons as a single-stage procedure. The use of laparoscopic approach halved the length of stay, without increasing the risk for complications significantly. Any difference in long-term weight result is pending.
Introduction
Despite having had an invasive surgical procedure such as laparoscopic Roux-en-Y gastric bypass (LRYGB) or laparoscopic sleeve gastrectomy (LSG), many bariatric patients still struggle to achieve long-term weight loss (1). In fact, one of the most common problems after bariatric surgery is insufficient weight loss, especially in super-obese patients (body mass index (BMI) > 50 m2/kg) (2). The most efficacious bariatric procedure with regard to weight loss is biliopancreatic diversion with duodenal switch (DS). DS was introduced by Hess and Hess (3) and Marceau et al. (4) in the 1980s as an open procedure (O-DS), but is feasible through laparoscopic procedure (Lap-DS) as a one- or two-stage procedure (5, 6). In bariatric patients, laparoscopy has specific advantages, both regarding pulmonary function and decreased risk of incisional hernias (7). However, all surgery in super-obese patients is technically demanding and comes with specific risks. For example, previous reports on DS surgery have described considerable mortality, 0.6%–7.6% (8–10). This in combination with the perceived high technical demands might explain why DS is only performed in 2% of all bariatric cases worldwide (11). The increased risk of developing nutritional deficiencies after DS compared to other bariatric procedures adds complexity and requires patient selection and careful postoperative follow-up.
Scandinavian Obesity Surgery Registry (SOReg) is a nationwide quality registry covering 98% of all bariatric surgery performed in Sweden since 2007. SOReg contains more than 50,000 procedures, of which less than 1% is DS. Data are entered prospectively: at baseline, perioperatively, and during follow-up, with less than 2% missing values. The accuracy of the variables used in this study is high (12). In addition, the operative techniques used for Lap-DS and O-DS, respectively, at different centers are very similar, because of a national training program.
The aim of this study was to compare Lap-DS with O-DS on a nationwide basis with regard to perioperative outcome and postoperative complications within 30 days.
Material and Methods
Between 2007 and 2014, 317 DS procedures, performed at six centers, were registered in SOReg. Patients undergoing Lap-DS were younger than those having O-DS (34.8 ± 11.2 vs 39.1 ± 9.9 years), as shown in Table 1. No differences were found between the groups regarding BMI, smoking status, hypertension, or diabetes preoperatively; however, sleep apnea was less common among Lap-DS patients (8% vs 28%). Diabetes was defined as elevated fasting blood glucose level or ongoing treatment with anti-diabetic drugs. Sleep apnea was defined as sleep apnea requiring treatment with continuous positive airway pressure. The proportion of male patients was found to be high, 38% and 44% in Lap-DS and O-DS, respectively. The number of O-DS procedures was evenly distributed during the study period while Lap-DS was concentrated in the latter half of the study period, 46 out of 53 Lap-DS cases (87%) were registered from 2011 to 2014.
Pre- and peri-operative data of 317 DS from the Scandinavian Obesity Surgery Registry, SOReg, performed in 2007–2014.
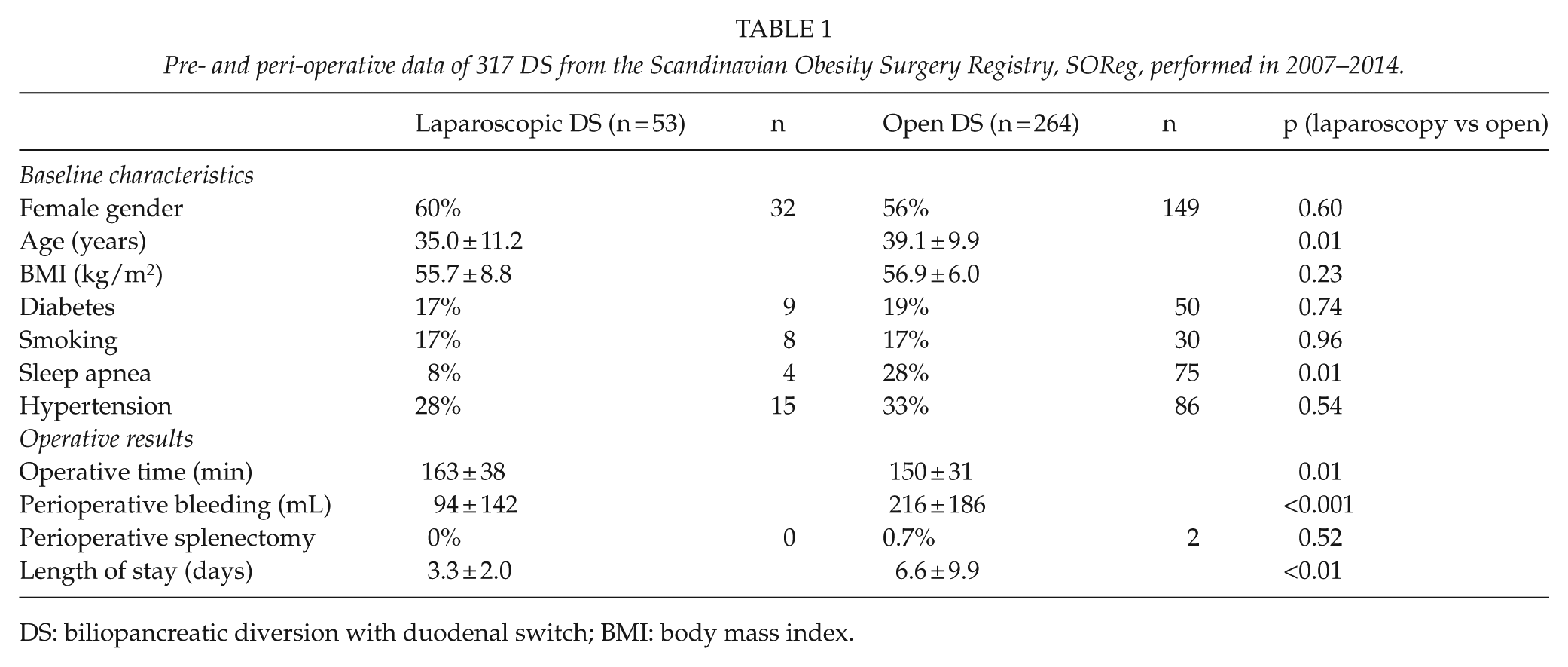
DS: biliopancreatic diversion with duodenal switch; BMI: body mass index.
Surgical Technique
The Lap-DS performed is a 5–6 trocar procedure. The vertical sleeve gastrectomy is performed over a 36 French bougie and the duodenum is divided 3 cm distal to the pylorus. The ileocecal region is identified and the distal ileum measured in 10 cm steps for 100 cm. This is the location of the entero-enteric anastomosis, and it is marked with two sutures of different lengths. The alimentary limb is then measured to 150 cm and the bowel is divided 250 cm from the ileocecal valve. The remaining biliary limb is positioned in the lower part of the abdomen, close to the previously marked location of the entero-enteric anastomosis, and a linear stapled and hand-sewn side-to-side enteroanastomosis is performed. The proximal end of the alimentary limb is brought into an antecolic position and anastomosed to the duodenal bulb by a completely hand-sewn end-to-end duodenoileostomy. The mesenteric defects are routinely left open.
O-DS has been previously described in this journal (13) and the procedure is highly standardized in Sweden. In brief, the procedure is performed through an upper midline incision, sparing the umbilical region. After measuring the whole small bowel, it is divided into a 100-cm common limb and a 150-cm alimentary limb, with the remaining small bowel forming the biliary limb. The sleeve gastrectomy is guided by a 36 French bougie along the lesser curvature and passed retrocolically for an end-to-side double-layered duodenoileostomy. The two mesenteric openings are closed by running resorbable sutures.
Variables
SOReg data were used to study operating time, bleeding, length of stay, and the following postoperative complications: reoperation, anastomotic leak, intra-abdominal abscess, hemorrhage (requiring transfusion or other measures), wound complications, cardiovascular event, pulmonary embolus, and urinary tract infection. Analysis was performed according to intention to treat; thus, one Lap-DS patient converted to open surgery remained in the laparoscopic group. This study was approved by the Regional Ethical Review Board (Dnr 2015/091).
Statistical Analysis
Baseline data were compared using two-tailed Student’s t-test for continuous data (age, BMI, and operative time). Mann–Whitney rank-sum test was used for ordinal data and χ2 for categorical variables. Fisher’s exact test was used for categorical variables with less than five cases in any cell such as complications. A value of p < 0.05 was considered statistically significant. Data were analyzed using Stata® version 13.1 (Statacorp LP, TX, USA). Numeric data are expressed as the mean ± standard deviation, unless otherwise stated.
Results
The operative time was longer for Lap-DS than O-DS, 163 ± 38 min versus 150 ± 31 min, p = 0.01, with less perioperative bleeding in Lap-DS (94 ± 142 mL vs 216 ± 186 mL, p < 0.001). The length of stay was halved in the Lap-DS group compared to the O-DS group, 3.3 ± 2.0 versus 6.6 ± 9.9 days, p < 0.01. During the years 2011–2014 when 87% of Lap-DS cases were registered, length of stay was 3.2 ± 1.9 days for Lap-DS and for O-DS 5.8 ± 9.2 days, p < 0.01 (Table 1).
Complications
No significant differences in peri- or post-operative complications between the two groups were seen. Two splenectomies were performed in the O-DS group due to splenic injury, none were needed in Lap-DS (Table 1). As demonstrated in Table 2, two Lap-DS patients suffered from leaks (4%), both at the enteroanastomosis, while the four leaks in O-DS group (2%) occurred in the upper part of the sleeve gastrectomy (n = 3) and at the duodenoileostomy (n = 1). No postoperative hemorrhage was noted in Lap-DS, compared to two patients requiring blood transfusion after O-DS. Reoperation within 30 days was performed in three Lap-DS patients (6%): two due to anastomotic leaks and one patient required a gastroscopy under general anesthesia due to swallowing difficulties. In O-DS, seven patients were reoperated (3%), due to leaks (n = 3), wound dehiscence (n = 2), and intra-abdominal bleeding (n = 1). The remaining patient was treated with embolization due to intracerebral bleeding, occurring 2 weeks after discharge from the bariatric procedure. No in-hospital or 30-day mortality occurred.
Postoperative complications (0–30 days).
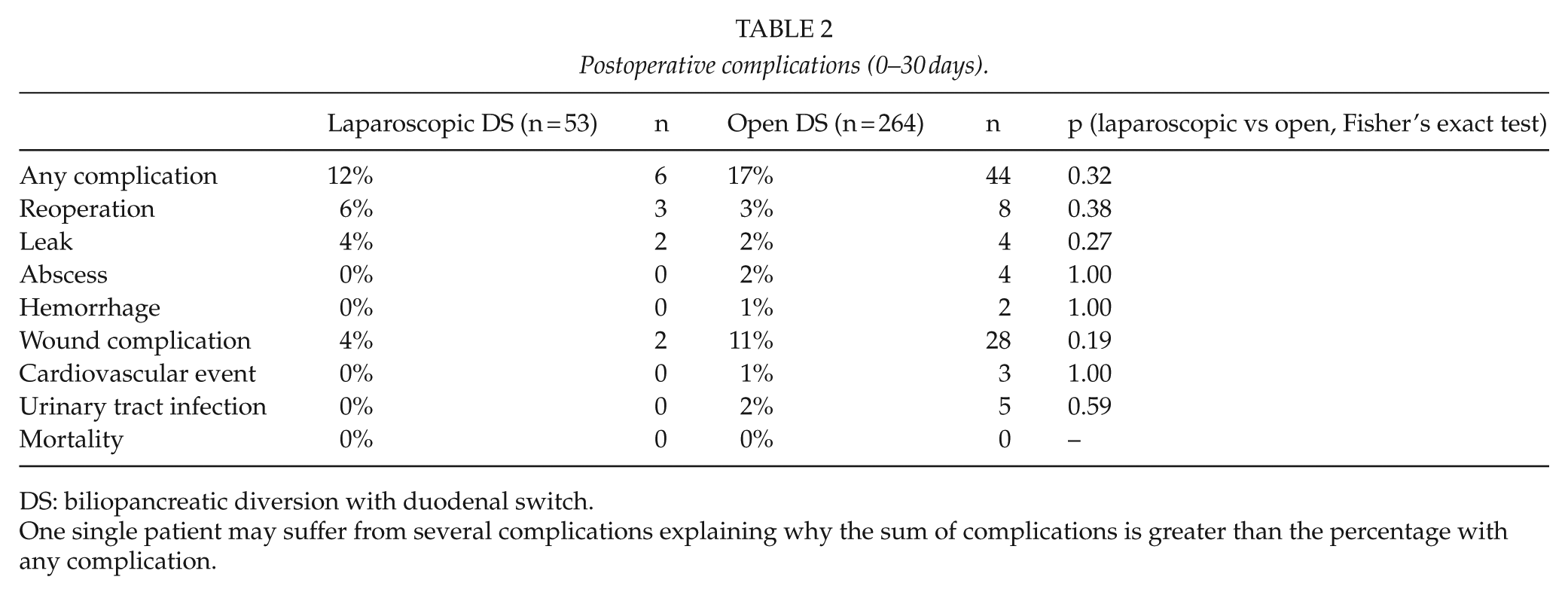
DS: biliopancreatic diversion with duodenal switch.
One single patient may suffer from several complications explaining why the sum of complications is greater than the percentage with any complication.
Discussion
In this nationwide study of 317 DS performed in six centers between 2007 and 2014, the laparoscopic approach was associated with a longer operative time but a halved length of stay without significant difference in postoperative complications.
Lap-DS is a technically demanding procedure. Yet, in experienced hands, the operative time was found to be only 12 min longer than for open surgery in this study. The laparoscopic procedure was, however, not identical to the open procedure as the length of the entire small bowel was not measured, nor were the two mesenteric openings closed. We therefore believe that the difference in operative time under identical circumstances might be somewhat greater. Operative times previously reported for Lap-DS have ranged from 206 to 226 min (6, 8, 9) and 153–259 min for O-DS. Compared to a particularly large single-center series of 1000 DS (Lap-DS: 226 min and O-DS: 176 min) (14), we were pleased with the operative performance in this study (162 vs 150 min).
Perioperative bleeding was lower in Lap-DS than O-DS in this study. A possible explanation for the difference in blood loss is that bleeding during laparoscopy rapidly reduces visibility. Because of this, small oozing vessels are more likely to be immediately addressed in laparoscopy. In addition, visualization of the angle of His, the short gastric vessels, and the spleen is superior during laparoscopy which is implied by the growing number of LSG (11). In line with this, two of the present O-DS patients required splenectomy due to splenic injury compared to none in the Lap-DS group.
A number of different procedures have shown reduction in length of stay when performed laparoscopically. The minimized operative trauma to the abdominal wall and shorter hospital stay are two quickly noticeable advantages of the laparoscopic approach in several procedures, such as cholecystectomy (15), appendectomy (16), and colectomy (17). In this study, length of stay was significantly shorter after Lap-DS than O-DS. However, this may, in part, be influenced by local postoperative regimes as well as surgeons’ expectations of patients. Shorter length of stay with laparoscopic surgery in bariatric patients is reported in several studies (7, 18). Moreover, postoperative small-bowel paralysis is reduced in minimally invasive surgery, especially if only the distal 2.5 m of the small bowel is manipulated during the laparoscopic procedure, as described here. Most Lap-DS were done in the latter half of the study period, and it is possible that improvements in bariatric surgery would result in shorter length of stay; however, when comparing Lap-DS and O-DS during the same period (2011–2014), the difference in length of stay between procedures remained.
When discussing differences, potential drawbacks of laparoscopy must be held in mind. Although infrequent, there is a risk of perforating intra-abdominal structures during the blind or semi-blind entry of the abdomen (19, 20), and prospectively, internal herniation is a problem, particularly in LRYGB (21). It seems likely that the number of wound complications would be lower in patients undergoing Lap-DS, but there is little support for this idea in bariatric literature (7, 8). In comparison between open and laparoscopic surgery regarding these problems, for example, in appendicitis, wound complications were more common in open surgery (22). The rate of incisional hernias and other long-term results, for example, weight loss, small-bowel obstruction, and nutritional deficiencies, are outcomes that remain to be studied for this cohort.
Although the incidence of leaks was similar between groups, interesting findings were made regarding the location of leaks. Three out of four leaks in O-DS were found in the top of the gastric tube, a common site for complications as this area is demanding to reach in super-obese patients. To overcome this, many surgeons leave 1–2 cm of gastric tissue lateral to the left crus, while others have tried using a white cartridge when dividing the most proximal portion of the stomach. The leaks at the enteroanastomosis in Lap-DS may imply different technical difficulties when performing the small-bowel anastomosis in the lower part of the abdomen, a narrow space in a super-obese patient. Drs Axer and Hoffmann (23) in Torsby have therefore recently described the Lap-DS procedure ad modum SOFY (Started Omega-loop Finished Y), using two omega loops to facilitate the construction of the enteroanastomosis. After the enteroanastomosis has been performed close to the duodenoileostomy in the upper part of the abdominal cavity, the remaining small bowel between the two anastomoses is divided by a linear stapler, thus technically identical to the double omega-loop technique used for most of the LRYGBs in Sweden. The SOFY approach also facilitates the closure of the two mesenteric defects. Outcomes from this novel technique remain to be studied.
The proportion patients requiring reoperation in this cohort was low, 3.4% (Lap-DS 6% and O-DS 3%), almost identical to the overall figure in SOReg (3.3%), based on >90% standard LRYGB, during the same time period. We find this interesting as DS is a more complex procedure and the present patients were both heavier (BMI, 56 vs 41 kg/m2) and more often male (43% vs 25%) compared to the complete SOReg cohort. In addition, the absence of 30-day mortality in this nationwide series (0.6%–7.6% in other nationwide cohorts) (8, 10) implies that the quality of Swedish DS surgery is high.
The study has some weaknesses, which should be addressed. Although nationwide, the cohort may not be large enough to detect differences in complications and other uncommon events. It is worth noting that DS is not a high-volume procedure at any center in Sweden, thus the learning curve may affect the results. However, all centers had extensive experience of bariatric surgery in super-obese patients when starting DS. The fact that only one patient (BMI, 96 kg/m2) was converted to open surgery suggests that the laparoscopic technique for bariatric surgery in super-obese patients was well developed. Furthermore, patients in the O-DS group were older than Lap-DS patients which may reflect on the results, as age has been shown to be a risk factor for complications in bariatric surgery (24). A major strength of this study is the use of SOReg, our national quality register, in which all patient data are entered prospectively and in an identical way, irrespective of operating center. Moreover, SOReg data are validated continuously at local site visits by comparing registered figures with medical records, demonstrating more than 98% correct entries (12). The high follow-up rate (98%), together with the collaborative nature of this study, creates a true nationwide result, allowing generalizations.
Conclusion
Lap-DS halved the length of stay without increasing risks for early complications significantly in this nationwide cohort. All leaks in Lap-DS were located at the enteroanastomosis while most leaks in O-DS occurred at the top of the gastric tube, implying that technical difficulties appear in different locations depending on surgical access. Any difference in long-term weight result is pending.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
