Abstract
Introduction:
Despite the uptake of focal therapy for prostate cancer in recent years, challenges remain in the identification of all tumor foci and adequacy of ablative modalities, accounting for the recurrence rate of 20%–50%. We aim to highlight the key steps in the evaluation and treatment planning for effective prostate focal cryotherapy (FCT).
Materials and Methods:
We described a case of intermediate-risk prostate cancer from a phase II trial (NCT04138914) that evaluated prostate FCT in 30 patients with localized prostate cancer. All patients underwent MRI of prostate with MRI-transrectal ultrasound software (TRUS) fusion transperineal prostate biopsy as part of the diagnostic work-up. The key steps in evaluation and treatment planning for FCT are as follows: (1) Comprehensive prostate biopsy sampling with complementary targeted and systematic saturation biopsy to accurately identify all tumor foci. (2) Precise insertion of Cryo Ice Probes with either a grid template or free-hand technique with real-time correlation with MRI-TRUS biopsy maps. (3) Proper protective measures with (a) placement of temperature probes at neurovascular bundles, Denonvillier's fascia and periurethral, (b) cystoscopy to ensure no urethral injury during probes placement, and (c) insertion of urethral warming catheter. (4) Ensure adequate cryoablation with two freeze–thaw cycles and real-time monitoring of ablation fields. The study aims to evaluate the functional outcomes, determined by pre- and post-treatment validated expanded prostate cancer index composite questionnaires, and oncologic outcomes, determined by prostate specific antigen (PSA) monitoring and mandatory repeat MRI of prostate with biopsy at 12 months post-treatment.
Results:
The trial recruited 30 patients, with predominantly intermediate (83.3%) and high-risk (10.0%) prostate cancer. Saturation biopsy complemented targeted biopsy by increasing the extent of index lesion in 11 patients (39.3%), of whom 2 patients had an upstage of index lesion. Additional foci were identified in 14 patients (50.0%), of whom 4 patients had clinically significant disease. Altogether, cryoablation treatment maps were changed in 18 patients (60.0%) after incorporating the saturation biopsy. The free-hand technique of cryoprobes insertion allows better ablation in anatomically challenging areas and avoids injury to surrounding structures. All cases were performed as ambulatory day surgeries with no major complications or readmission. The mean operating time was 75 minutes (range 55–90 minutes). All patients maintained satisfactory functional outcomes post-treatment with preserved urinary and sexual functions. The median PSA decreased from 7.1 ng/mL preoperatively to 1.7 ng/mL at 6 months post-treatment. Interim results demonstrated that of the 10 patients who had undergone the mandatory repeat MRI of prostate and biopsy, only 1 patient (10%) demonstrated clinically significant infield recurrence.
Conclusion:
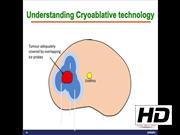
This video shows the key steps in the evaluation of treatment planning for prostate FCT. It highlights the importance of thorough diagnostic prostate biopsy, which can alter treatment planning in over half of patients, understanding the cryotherapy technology to achieve adequate ablation and emphasizing the protective measures to prevent treatment morbidities. By conforming to the above-mentioned key steps, prostate FCT can achieve good oncologic and functional outcomes in well-selected patients.
Patient consent statement:
This is an IRB approved study (Singhealth Institution Review Board 2018/2482) of which the patient has been consented for the study.
The authors have no disclosure or conflict of interest
.
Runtime of video: 7 mins 56 secs