Abstract
Aims and Objectives:
Holmium laser enucleation of prostate (HoLEP) is one of the important modalities in surgical treatment for obstructive benign prostatic hyperplasia (BPH). Classically it was described as three-lobe technique by Peter Gilling et al. 1 One of its significant drawbacks is steep learning curve. We hereby describe a single-lobe technique simplified in four easy steps for enucleation of adenoma.
Methods and Patients:
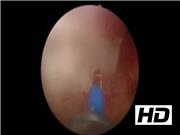
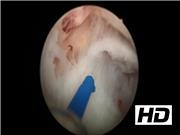
Forty patients were included in our study of single-lobe technique for HoLEP between December 2014 and July 2016. All procedures were done by a single surgeon (A.D.B.) who had vast experience of >2000 cases. Average volume of prostate in our study was 79.82 cc (35–195 cc). All patients were evaluated preoperatively by International Prostate Symptom Score (IPSS), uroflowmetry, sonography of prostate and urinary tract for prostate volume and postvoid residual volume estimation, prostate-specific antigen and quality of life score. Postprocedure follow-up was done at 1 month, 3 months, 6 months, and 1 year. Procedure was done by 550 µm quartz fiber, 100 W holmium-YAG laser (Lumenis) at the settings of 2 J × 40 Hz frequency and 26 F Karl Storz continuous irrigation resectoscope set. Morcellation of enucleated adenoma was done by Wolf morcellator. Procedure was divided into four steps: (1) apical lobe enucleation around verumontanum, (2) incision at 12 o'clock and defining anterior capsule, (3) lateral lobe enucleation, and (4) peeling off adenoma from bladder neck and “en bloc” enucleation.
Results:
Mean enucleation time for the prostate was 30.88 minutes (10–80 minutes) and estimated blood loss during the procedure was 49 mL (16–350 mL). Mean catheterization time was 45.25 hours and mean hospital stay was 47.65 hours. None of the patients required blood transfusion. Only one patient needed two-stage procedure. Clavien grade 1 complications were seen in five patients, grade 2 in three, and one patient needed prolonged irrigation for intermittent hematuria. Four patients had transient (<2 weeks) stress urinary incontinence. Two patients needed cystoscopy+visual dilatation of membranous urethral stricture. Significant improvement in IPSS, Qmax, and QoL was seen on follow-up of 3, 6, and 12 months.
Conclusions:
HoLEP significantly relieves obstructive changes occurring because of BPH. Modifying technique of enucleation to single lobe helps in reducing operative time of enucleation. One may argue that vast experience of our operating surgeon (A.D.B.) may have contributed to lower morbidity in our study. We hypothesize that our simplified technique described in four steps can become useful in reducing the learning curve. Single-lobe technique with early recognition of important landmarks and repeating same steps for all sizes of prostate can ease the learning of this wonderful procedure.
Runtime of video: 9 mins

Get full access to this article
View all access options for this article.
