Abstract

Introduction:
The anatomical endoscopic enucleation of the prostate is considered the gold standard in the treatment of benign prostatic obstruction. Despite the numerous energy options available for this procedure, the holmium laser stands out as the most widely used and established technology in clinical practice. One of the disadvantages of low-power lasers is a reduction of laser cutting power on prostatic tissue, leading to difficulties in releasing the adenoma from the bladder neck. We developed a technique modification to minimize this disadvantage of low-power lasers. 1,2
Materials and Methods:
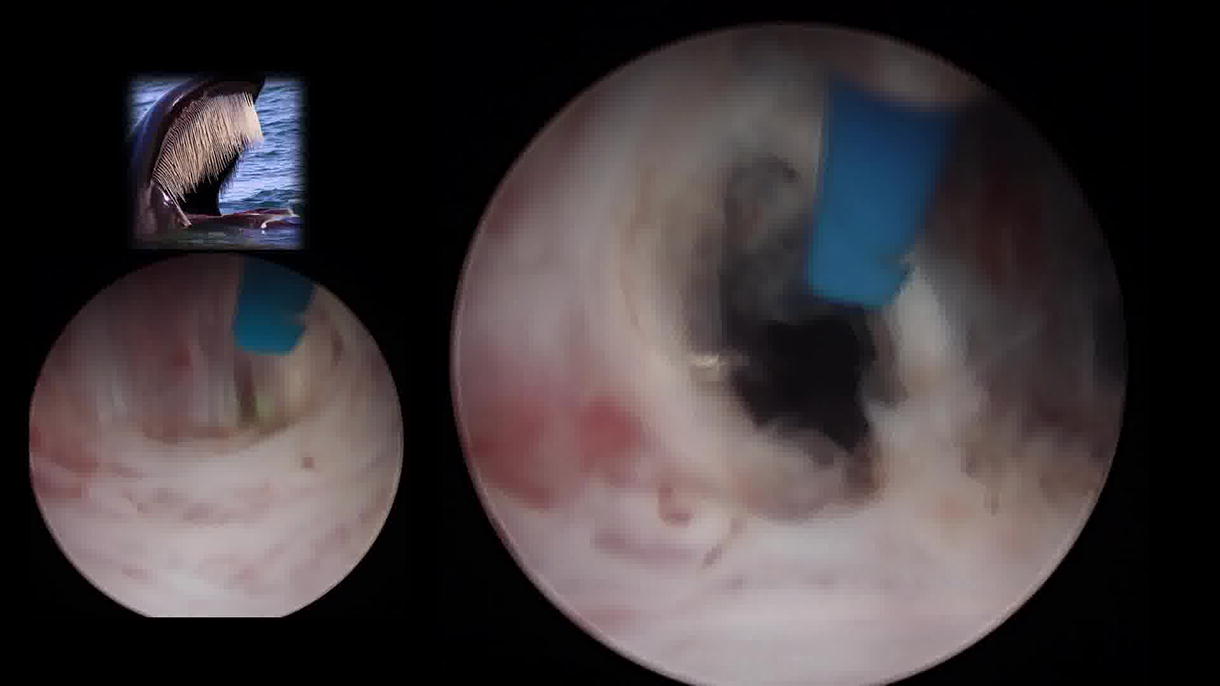
A retrospective review was conducted on 100 consecutive patients who underwent low-power holmium laser enucleation of the prostate (HoLEP) between January 2022 and December 2022. Patient selection criteria included prostates ranging from 40 to 120 cc in volume. Surgical procedures were performed utilizing a 26 Fr Storz scope and Hawk morcellator with the Auriga XL 50W holmium (Ho:YAG) laser system and a 550 µm laser fiber. The technique involves the following surgical steps: identification of the dissection plane with a lateral incision next to the verumontanum, release of the urinary sphincter following the apical morphology of the prostatic lobe, unification of the lateral planes over the verumontanum, access to the bladder via the superior dissection plane, lateral release of the bladder neck, incision of the bladder mucosa at its junction with the prostatic adenoma, and en-bloc release of the adenoma. Descriptive statistical analysis was employed to evaluate preoperative baseline characteristics, intraoperative parameters, and postoperative complications.
Results:
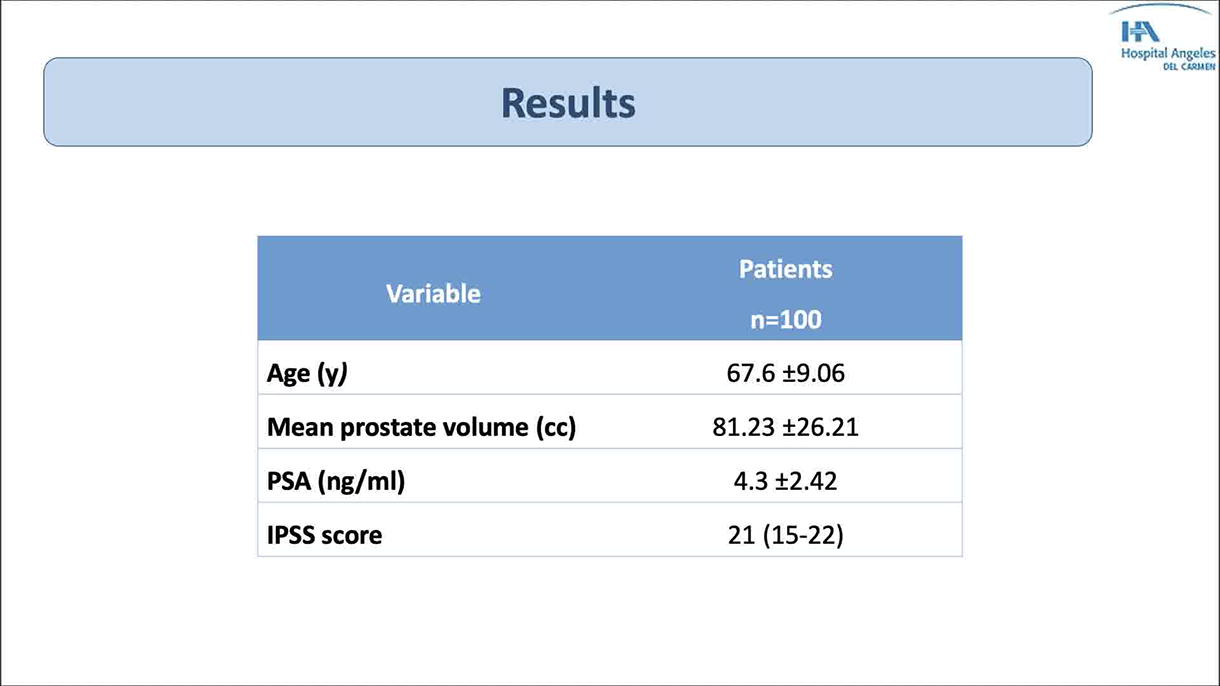
Mean age was 67.6 years. Preoperative mean prostate volume was 81.23 cc and preoperative prostatic specific antigen was 4.3 ng/mL. The preoperative mean International Prostatic Symptoms Score was 21. Low-power HoLEP with vesical mucosal release was performed on 100 patients. The mean surgical time was 99.97 minutes, with a mean enucleation time of 72.94 minutes, and morcellation time of 13.73 minutes. An average of 66.44 grams was enucleated. Complications were present in 3% of the patients. There were two Clavien–Dindo grade 1 complications and one ClavienDindo grade 3 complication. Incontinence at 1 month was present in 4 patients (4%), with no incontinence at the 3-month follow-up. None of the patients presented with injuries to the ureteral orifices.
Conclusions:
In our experience, this modification to the technique allows for maintaining a good safety profile and low complication rates. Focusing on defined anatomical structures could assist in the learning curve of new surgeons.
Patient Consent Statement:
The authors have received and archived patient consent for video recording/publication in advance of video recording of procedure.
Funding Statement:
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Runtime of video: 8 mins 11 secs.
Running Title: Modified Vesical Mucosal Release in HoLEP.
Get full access to this article
View all access options for this article.
