Abstract
Introduction:
Sacrocervicopexy is a procedure similar to sacrocolpopexy, in which a graft material is used to suspend the cervix to the anterior longitudinal ligament of the sacrum. Sacrocervicopexy can be performed either with uterine preservation or after supracervical hysterectomy. 1 –3 This procedure definitely avoids the risk of mesh erosion. Moreover, it preserves the integrity of the uterosacral and cardinal ligaments, which are the main supports of the vaginal apex. 4 Minilaparoscopy limits tissue trauma and improves cosmesis. 5
Design:
We report a video explaining the technique and evaluated the effectiveness of our first four cases of minilaparoscopic subtotal hysterectomy (MLSH) and sacrocervicopexy to resolve isolated pelvic central compartment uterine prolapse, with posterior cul-de-sac specimen extraction. 6 We assessed the reduction of prolapse-related symptoms, operative and postoperative complications, and patient satisfaction.
Setting:
A tertiary university hospital.
Patients:
Four women with symptomatic isolated pelvic central compartment uterine prolapse (pelvic organ prolapse quantitative stage 2) without urinary complaints.
Interventions:
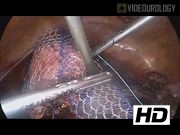
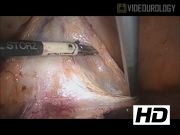
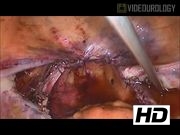
Four ports were made in all patients: a 5-mm infraumbilical port for the laparoscope and three 3.5-mm ports (right and left paraumbilical and suprapubic). MLSH was performed using a 3-mm bipolar grasping dissector device and reusable monopolar scissors. Uterus was transected from cervical stump using monopolar. Sacrocervicopexy was performed using a triangle-shaped polypropylene mesh with one right arm that was fixed on the vagina and on the sacral promontory with a nonabsorbable braided surgical suture. Reperitonealization over the mesh was performed using a running monofilament absorbable suture. Finally, the posterior cul-de-sac was incised, the specimen was removed vaginally, and the cuff was closed.
Results:
The mean age of the patients was 61.3 years. The operation was performed successfully with no intraoperative or postoperative complication in all cases. Mean operative time was 123±28 minutes and mean blood loss was 34 mL. At the patients' fourth week postoperative visits, no prolapse in any compartment was identified. There were no operative complications related to colpotomy incision and no cases of postoperative vaginal cellulitis or pelvic infection were reported. Patients reported only minimal pain on the day after the surgery and were overall very satisfied especially with the cosmetic results. No new onsets of urinary symptoms following the procedure were found.
Conclusion:
This video demonstrates a feasible method for performing supracervical hysterectomy and sacrocervicopexy using minilaparoscopic instruments with specimen removal through the posterior vaginal cul-de-sac.
No competing financial interests exist.
Runtime of video: 8 mins 18 secs
Keywords
Get full access to this article
View all access options for this article.
