Abstract
Introduction and Objective:
Ureteral strictures may result from various causes, including endoscopic procedures, stone passage, tuberculosis, endometriosis, malignancies, primary obstructive megaureter, and radiation therapy. Traditionally, open ureteral reimplantation with or without the psoas hitch has been the gold standard for such strictures. Laparoscopic ureteroneocystostomy/Boari flap is indicated in the management of distal ureteral strictures. We present a video demonstration of the two techniques of laparoscopic management of lower ureteral strictures.
Study Methods:
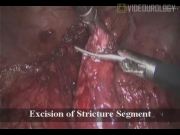
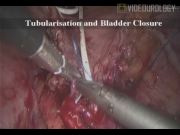
Case 1: A 35-year-old male underwent abdominoperineal resection and multiple right ureteral dilatations earlier. A right long-segment ureteral stricture was diagnosed. The imaging protocol included ultrasound and CT urography. A laparoscopic Boari flap was planned. Four ports were used. The ureter was disconnected before the stricture level and spatulated. Anterior mobilization of the bladder was performed. A wide Boari flap was generated. The apex of the flap was anastomosed to the lower ureteral margin with 3-0 polyglactin suture. A ureteral stent was placed, the flap was tubularized, and then the bladder closure was done. Case 2: A 64-year-old female who underwent right ureterorenoscopy earlier presented with persistent right loin pain. The imaging revealed a right short-segment ureteral stricture. Laparoscopic ureteroneocystostomy was performed. All patients with strictures treated with the laparoscopic approach were analyzed to assess the operative and postoperative outcome.
Results:
A total of 61 patients were treated with the laparoscopic approach for lower ureteral strictures. The mean operative time was 94 minutes. The mean blood loss was around 190 mL. The orals were started on the first day and drain removal on the second day. Most of the patients were discharged on the third postoperative day. There were no intraoperative or postoperative complications. A follow-up USG was performed at 6 months and 1 year. A follow-up CT urography or MR urography was performed at 1 year.
Conclusion:
Minimally invasive management of lower ureteral strictures is feasible and easier with a 3D laparoscopic approach. The principles of laparoscopic approach for management of lower ureteral strictures are similar to that of open surgery. Laparoscopic management has the advantages of early ambulation, rapid convalescence, and a shorter hospital stay, with equivalent functional outcomes compared to open surgery.
No competing financial interests exist.
Runtime of video: 6 mins 38 secs
Keywords
Get full access to this article
View all access options for this article.
