Abstract
Introduction:
Robot-assisted laparoscopic excision of retrovesicular cysts, including prostatic utricle cysts, has been described with success given excellent three-dimensional visualization, easy manipulation of instruments in small working spaces particularly the pelvis, decreased blood loss, and ease of identification of important anatomical structures. 1 Here we present a video demonstrating robot-assisted laparoscopic excision of prostatic utricle in a 3-year-old male.
Methods:
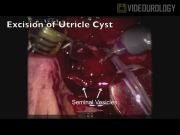
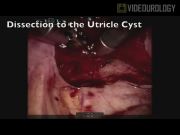
Two patients have undergone robot-assisted laparoscopic excision of a retrovesicular cyst with success at our institution. In this case, the patient was a 3-year-old male who was discovered to have a prostatic utricle cyst during one-stage repair of hypospadias. Following hypospadias repair, he had recurrent urinary tract infections and post-micturition dribbling. An MRI scan and subsequent cystourethroscopy confirmed a 2 cm utricle cyst. Technique: (1) Following placement in the lithotomy position, cystoscopy was performed that showed a huge prostatic utricle from the verumontanum and a normal bladder. (2) Over a guide wire, the prostatic utricle was catheterized with an 8F Foley catheter with 1.5 mL balloon. (3) Keeping the patient in the lithotomy position, the open Hassan technique was used to place a 12-mm umbilical camera port followed by placement of two 8-mm ports on either side in the midclavicular line and a 5-mm assistant port in the left side just below the costal margin. (4) After the robot was docked and a 30° down lens was inserted, the peritoneum was incised and dissected behind the bladder into the Denonvilliers fascia between the rectum posteriorly and the bladder anteriorly. (5) A bladder stitch was placed for bladder retraction. (6) With continued dissection, both seminal vesicles, vas deferentia, and the prostatic utricle were identified with the previously placed Foley catheter in the prostatic utricle. (7) With a 30° up vision lens, the cyst was incised anteriorly to open the cavity. (8) The vas deferentia and the seminal vesicles were on the cyst roof, so the posterior wall was kept intact and the anterior wall was excised, keeping the vas deferentia and seminal vesicles attached to the cyst roof. (9) The posterior wall was approximated with 5-0 PDS suture followed by closure. (10) Under vision, cystoscopy was performed again and a Foley catheter was placed in the bladder over a guide wire. (11) Once this was done, the ports were closed under vision. He was discharged home after normal diet resumption and pain control. The Foley catheter was removed in the clinic 1 week later and noted normal voiding.
Results and Conclusions:
The procedure was uneventful without intraoperative or perioperative complications. Several techniques promote successful execution of the procedure. First, placement of a catheter, for example, Foley into the prostatic utricle cyst allows for proper cyst identification during dissection. Second, a bladder stitch can be used to facilitate bladder retraction and easier cyst visualization. Port placement and positioning are crucial as described previously. 2 Diligent identification of anatomical structures and atraumatic dissection are possible to preserve the vas deferentia and seminal vesicles.
Mohan S. Gundeti, MD: Intuitive Surgical, Inc.–Proctor and course director. For all other authors, no competing financial interests exist.
Video Music:
Perspectives—
Runtime of video: 4 mins 32 secs

Keywords
Get full access to this article
View all access options for this article.
