Abstract
Introduction:
During dismembered pyeloplasty, anterior crossing vessels are usually transposed posteriorly before anastomosis. However, recent studies on minimally invasive dismembered pyeloplasty have demonstrated similar success rates without transposition in selected cases. 1,2
Methods:
Nine cases of minimally invasive dismembered pyeloplasty (five robot assisted, four laparoscopic) performed by a single surgeon in the past 16 months were reviewed. Six cases were found to have lower pole anterior crossing vessels and one had posterior crossing vessels. There were three cases (one robot assisted, two laparoscopic) where after mobilization of anterior crossing vessels, no transposition was deemed necessary. One robot-assisted case and one laparoscopic case demonstrating this technique were selected for this video.
Patients and Surgeries:
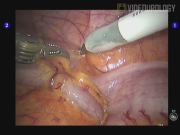
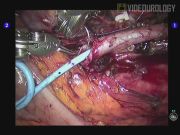
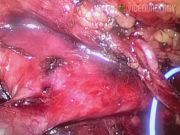
The first case was a 52-year-old male who presented with symptomatic left ureteropelvic junction obstruction (UPJO). He underwent robot-assisted laparoscopic left dismembered pyeloplasty. Intraoperatively, the left gonadal vein was identified to be crossing the ureteropelvic junction (UPJ) causing proximal obstruction. The gonadal vein was dissected free from the ureter up to the mid-ureter where the gonadal vein entered the deep inguinal ring. Dismembered pyeloplasty was completed without transposition. Postoperative diuretic renogram at 3 months showed resolution of UPJO. He is scheduled for repeat diuretic renogram at 1 year after surgery. The second case was a 23-year-old male who similarly presented with right symptomatic UPJO. He underwent laparoscopic right dismembered pyeloplasty. Intraoperatively, a set of crossing artery and vein was found at the level of the UPJ. After dissection, the crossing vessels were found to lie cephalad to the UPJ without causing obstruction. Thus, transposition was not performed and dismembered pyeloplasty was completed. No postoperative diuretic renogram was performed, but a computed tomography urogram done at 8 months after surgery showed good excretion of contrast and significantly reduced hydronephrosis. For the third case, where transposition of crossing vessel was not performed (not shown in the video), postoperative renogram at 3 months showed persistent outflow obstruction with no significant difference in split renal function. The patient underwent endoscopic laser ureterotomy 5 months after her initial surgery. Repeat diuretic renogram 3 months after repeat surgery showed both improved outflow and split renal function. Overall, for our nine cases, the clinical follow-up has been for a mean of 10.4 months (range 3–16 months). As previously stated, seven cases had crossing lower pole vessels (six had anterior crossing vessels and one had posterior crossing vessels). In three of the cases, no transposition was performed (already detailed above). Two cases had transposition performed and in the other two cases, the crossing vessel was divided. All our patients returned for clinical follow-up, but only six had postoperative diuretic renograms performed. In these six cases, three showed resolution of outflow obstruction. Two cases had persistent outflow obstruction. One of them underwent successful repeat intervention (detailed above as one of the cases with no transposition of crossing vessels). The other patient declined further intervention. The last patient had persistent poor uptake in the affected kidney due to pre-existing very poor renal function, which was present before her surgery.
Conclusion:
Routine transposition of crossing vessel during minimally invasive pyeloplasty may not be necessary and should be an intraoperative decision by the surgeon after adequate dissection.
The authors declare that no competing financial interests exist.
Runtime of video: 6 mins 53 secs
Keywords
Get full access to this article
View all access options for this article.
