Abstract
Introduction:
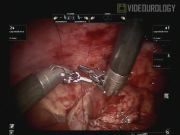
Pediatric urologists are increasingly using robot-assisted laparoscopic pyeloplasty (RAL-PYELO) to treat ureteropelvic junction obstruction (UPJO); however, the procedure is not typically performed in infants due to intracorporeal space constraints. 1,2 Here we present an 8:30 video demonstrating RAL-PYELO for repair of a UPJO in an 11-month-old male.
Methods:
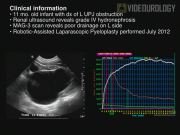
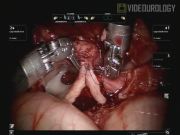
Ten patients (9 male, 1 female) age ≤12 months (mean 7.3 months, range 2–12 months) have undergone RAL-PYELO using the da Vinci Surgical System at our institution. All patients were diagnosed with UPJO based on ultrasound and MAG-3 renal scans. The mean grade of preoperative hydronephrosis was 3.5. All surgeries were performed by a single surgeon (M.S.G.) using the following technique. (1) After positioning the patient, ports were placed transperitoneally using the open Hasson's technique. Four ports were placed: a 12 mm umbilical camera port, an 8 mm working port 4 cm superior to the umbilicus, an 8 mm working port 4 cm superior to the anterior superior iliac spine (ASIS) and a 5 mm assistant port at the midline suprapubic level. Currently, the port placement has been modified to place all ports in the patient's midline. (2) The 8 mm instrumentation set was selected for the procedure. The 8 mm fixed-pivot instrument design is desirable over the 5 mm snake-joint design as the 8 mm instruments have a shorter instrument tip-to-pivot distance (2 cm vs. 3.9 cm) facilitating operation in a limited working space. (3) Once the colon was reflected, the dilated pelvis was identified. Often a transmesenteric approach is feasible depending on the patient's anatomy. (4) A pyelotomy was performed to aid in UPJ identification. Alternatively, in cases, where the pelvis is not hugely dilated, the UPJ may be identified before pyelotomy. (5) The ureter was spatulated and the redundant pelvis was excised. (6) With a 6-0 PDS suture, a continuous, watertight neo-ureteropelvic anastomosis was performed. The posterior layer was closed first. This was followed by the introduction of a cutaneous-pyelo-ureteral (CPU) stent under visualization using the lateral body wall, through the posterior wall of the renal pelvis, and into the proximal ureter. Finally, the anterior layer anastomosis was performed. Six patients received indwelling stents and four received CPU stents. Patients were discharged home after a successful voiding trial, normal diet, and pain control. Follow-up ultrasounds were performed at 1 and 4 months, followed by a MAG-3 scan within 1 year. Average follow-up time was 9 months (range 1–24 months).
Results and Conclusions:
All patients underwent RAL-PYELO without open or laparoscopic conversions. There were no intraoperative complications. One patient developed a trocar site omental hernia on postoperative (PO) day 1, requiring repair. Another patient experienced a dislodged CPU stent during perioperative waking. Subsequent CPU stents were secured to the body wall with a nylon stitch. All patients had resolution or improvement in hydronephrosis, with mean improvement from grade 3.5 preoperatively to 2.8 postoperatively. Foley catheters were removed on mean PO day 1.3; all patients were discharged home on mean PO day 2.1 (range 1–3). All indwelling stents were removed 4–6 weeks PO and CPU stents were removed 7–10 days PO. In our limited experience, we have not observed any infections, increased parental concern, or internal leakages associated with the CPU stent. RAL-PYELO is a feasible option for the surgical management of UPJO in infants. Several techniques promote successful execution of the procedure. First, positioning the patient in the 30° lateral decubitus position allows the bowel to be displaced from the surgical area. It is important to adjust the size of the skin incisions to ensure a snug fit around the port, preventing dislodgement. Furthermore, our trocar-in-camera port technique, in which ports are placed under visualization and directed into the camera port, reduces risk of injury. Use of pyelotomy to deflate the pelvis facilitates identification of the UPJ. Placement of a CPU stent through the lateral body wall rather than through the pre-existing assistant port allowed for minimal turning and kinking of the stent. Finally, the placement of a CPU stent prevents the need for postoperative removal under general anesthesia.
No competing financial interests exist.
Runtime of video: 8 mins 30 secs
Keywords
Get full access to this article
View all access options for this article.
