Abstract
Introduction:
The management of incidentally discovered renal stones in living donor candidates is evolving. Recently, the safety and efficacy of ex vivo ureteroscopy for stone removal in donor kidneys have been described. 1 –3 Here, we present our experience with ex vivo ureteroscopy and laser infundibulotomy for the treatment of a stone contained within a calyceal diverticulum. Calyceal diverticulae are known to harbor bacteria and pose an infection risk for the immunosuppressed recipient, 4 leading us to decide that treatment was prudent before transplantation.
Materials and Methods:
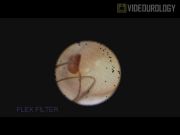
A 38-year-old woman with a previous stone episode presented for the evaluation as a living kidney donor. Preoperative computed tomography angiogram revealed two incidental stones in the left kidney, measuring 6 and 2 mm, with a density of 530 Hounsfield units. Litholink 24-hour urine collection was significant for hypernatremia and hypercalciuria. Following left hand-assisted laparoscopic donor nephrectomy, the kidney was placed on ice and flushed in a standard manner. A flexible ureteroscope was used to visually inspect the collecting system. The 6-mm stone was noted to be within a calyceal diverticulum. Using a 200-μm holmium:YAG laser, infundibulotomy followed by lithotripsy was performed. Stone fragments were removed using a zero-tip nitinol basket.
Results:
Stone treatment time was 26 minutes. The kidney was visually stone free at the completion of the procedure and was successfully transplanted into a pediatric recipient. Total cold ischemia time was 209 minutes. A modified Lich-Gregoir ureteral anastomosis was performed using a double-J ureteral stent, which was removed 2 weeks postoperatively. Recipient creatinine was 1.2 with no postoperative complications at 2 months of follow-up.
Conclusions:
Stones contained within a calyceal diverticulum should not serve as an absolute contraindication to kidney donation. Ex vivo stone removal is technically straightforward and has the added benefit of minimizing the risks of bleeding, infection, and anesthetic complications to the donor. Although recipient renal function may have been negatively affected by a 26-minute increase in cold ischemia time, this was likely minimal as successful transplants are routinely performed with cold ischemia times in excess of 10 hours. 5 Additionally, this risk is partially outweighed by the benefit of reducing potential complications in the donor by consolidating operative intervention to a single setting. Possible complications of this technique include prolonged operative (and therefore cold ischemia) time, inability to locate the calyceal diverticulum, and postoperative bleeding. Potential candidates for this approach should have a sufficiently small stone burden that can be cleared in a timely manner. Had we not been able to localize the diverticulum, transplantation would have proceeded as planned with consideration of stone removal at a later time. Significant post-transplantation bleeding that did not respond to conservative measures, while unlikely, would be managed on a case-by-case basis. Donors require close urologic follow-up and monitoring of their 24-hour urine parameters to decrease the risk of future stone events. Further research should be performed to evaluate the safety and long-term effects of this technique.
Source of work or study: Intraoperative video recorded at the University of Pittsburgh Medical Center.
No competing financial interests exist.
Running time: 4 mins 25 secs


Keywords
Get full access to this article
View all access options for this article.
