Abstract
Introduction:
In patients with urinary diversion, retrograde ureteral access can be technically challenging because of the anatomic distortion and the difficult or impossible identification of the new ureteral orifices. Moreover, failed access is higher in patients with ureteral anastomotic stricture. 1 We present a video of our experience of the ureteral reimplantation using the split-cuff nipple. 2,3 We assess the endoscopic presentation of this reimplantation and show the possibility of a retrograde ureteral endoscopic approach. 4,5
Materials and Methods:
Between September 2005 and February 2008, 28 adult male patients underwent radical cystoprostatectomy and urinary diversion with an orthotopic ileal neobladder 6 –8 (Camey II or Hautmann) in 85.7% (24/28), or a continent cutaneous ileal pouch 9 in 14.3% (4/28) patients. The ureteral reimplantation procedure was achieved by a modified split-cuff ureteral nipple. The ureter is passed through the ileal wall. The ureter is spatulated by a longitudinal ureteral incision of 0.5–1 cm. Then, the ureteral wall is turned back on itself to form a nipple shape. The cuff is fixed with sutures passed between the corners of the turned ureteral walls and the adventitia of the ureter. In case of a large ureter, the ureteral wall is turned back on itself without incision. Then, the ureter is laid in a mucosal trough. The anastomosis is stented using a ureteral catheter or a Double-J stent. The endoscopic presentation was assessed by a cystoscopy at 3 months after the procedure.
Results:
The ureteral reimplantation using the split-cuff nipple was overall possible, independently of the prior caliber of the ureter. The mean duration of the reimplantation procedure was 25 minutes (20–35 minutes). Fifty-three ureteral units were reimplanted with this technique. A ureteral catheter was inserted in 33 ureteral units, and a Double-J stent was inserted in 20 ureteral units. No patient had reflux in the cystographic control. The cystoscopy demonstrated a nipple-shaped ureteral orifice, which was easily identified in all cases. No stenosis was observed, and the placement of a 7F Catheter in the reimplanted ureter was possible. The follow-up was performed using an ultrasound and CT scan, with a mean follow-up of 36 months (6–54 months). Three patients had a retrograde Double-J stent insertion for middle or proximal ureter obstruction due to retroperitoneal lymph node metastasis.
Conclusions:
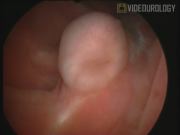
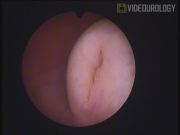
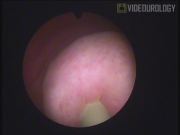
Compared to direct ureteral reimplantation, the ureteral nipple was clearly prominent and visible in the intestinal pouch. The new ureteral orifice was easily catheterized, which suggests the possibility of retrograde endourological manipulations of the ureter.
The authors have no conflicts of interest or financial ties to disclose.
Runtime of video: 7 mins 31 secs
Keywords
Get full access to this article
View all access options for this article.
