Abstract
Introduction:
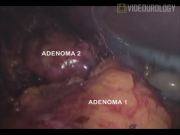
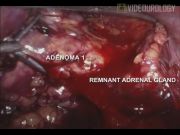
Adrenalectomy through laparoscopic approach (LA) has been appraised for excellent morbidity profile. 1 In comparison to laparoscopic total adrenalectomies, laparoscopic partial adrenalectomies have been sparingly reported. 2 We narrate our experience with both techniques. The accompanying video demonstrates an exercise of simultaneous unilateral total and contralateral partial adrenalectomy.
Methods:
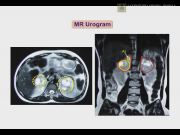
Patients were evaluated in detail. Functional status of the adrenal lesion was assessed. Imaging included ultrasonogram, computed tomogram urography, or magnetic resonance urogram. All procedures were performed by the same surgeon via transperitoneal access. Four ports were used for left LA and five for right LA. In benign pathologies and bilateral affections, if sufficient adrenal parenchyma was preservable on one side, partial adrenalectomy was attempted. The line of cleavage between the pathological and healthy adrenal was point-mapped using electrocautery. Partial adrenalectomy was conducted along this line using harmonic shears. Vascularity to the preserved adrenal was uninterfered. In large lesions (≥3.5 cm) with negligible preservable healthy adrenal, unilateral pathologies with contralateral healthy adrenal or probable malignant etiology, total adrenalectomy was undertaken. Operative and postoperative parameters and histopathological impressions were recorded. Patients underwent periodic follow-up with clinical and biochemical assays. Hormonal supplementation was administered as necessary.
Results and Discussion:
Since January 2003 till October 2011, 27 cases of LA (25 unilateral total, 1 unilateral partial, and 1 simultaneous unilateral complete and contralateral partial adrenalectomy) were performed. Mean age was 34.3 years; 19 were males and 8 were females. Mean body mass index was 23.13 kg/m2. Mean American Society of Anesthesiologists score was 2.4. Left adrenal was involved in 15 cases, and right, in 11. Longitudinal tumor dimension ranged from 2.5 to 6.5 cm. Mean duration of operation was 125.34 minutes. Mean blood loss was 85.67 mL. Three patients with pheochromocytoma experienced intraoperative hemodynamic fluctuations that were tackled conservatively. Both partial adrenalectomies revealed benign etiology. Pathologies included pheochromocyoma (n=11), aldosteronoma (n=2), hypercortisolism (n=3), nonfunctioning adenoma (n=7), pseudocyst (n=1), hemangioma (n=1), and metachronous clear cell carcinoma (following contralateral radical nephrectomy and adrenalectomy, n=3). Surgical margins were disease free in all. Mean time to oral tolerance was 18 hours. Mean visual analog pain score on the first postoperative day was 2.2. Mean time to drain removal was 1.4 days. Mean hospital stay was 3.8 days. One patient experienced retrieval-site infection that mandated secondary suturing. Mean follow-up duration was 11.4 months (range 3–36 months). Hormonal supplementation could be withheld in patients undergoing partial adrenalectomy. Also, no disease recurrence was identified till last follow-up. Despite technical challenges, LA could be accomplished in all circumstances. In partial adrenalectomies, vascularity of the preserved gland should be meticulously preserved and satisfactory hemostatsis should be achieved. Nonrequirement of supplemental hormones is a key advantage of partial adrenalectomy. LA offers early pain-free recovery and acceptable oncological outcome.
No competing financial interests exist.
Runtime of video: 6 mins 41 secs
Keywords
Get full access to this article
View all access options for this article.
