Abstract
Introduction:
Urachal cysts are the most common urachal anomaly in the pediatric population. 1 There is an increasing body of literature documenting successful management of urachal cysts using laparoscopic techniques. 2 –5 There may be an advantage, however, with the use of robot-assisted laparoscopy for reconstructive cases. We describe the techniques used for robot-assisted laparoscopic excision of a urachal cyst and bladder cuff with bladder repair.
Materials and Methods:
We performed video documentation of a robot-assisted laparoscopic excision of a urachal cyst and bladder cuff in a 4-year-old girl. She initially presented with midline abdominal pain and was found to have a 2.7 cm urachal cyst seen on computed tomography scan. Key steps of the procedure were noted in the final edited video.
Results:
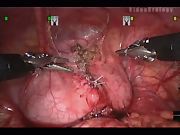
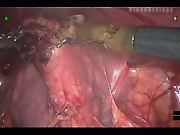
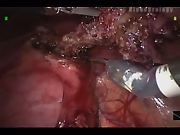
After cystoscopic evaluation of the bladder was performed and a Foley catheter inserted, the patient was placed in supine and mild Trendelenburg position. Initial access was performed using an open peritoneal (Hasson) technique. One 12 mm camera port and two robotic arm ports were used for the procedure. The Da Vinci surgical robot system (Intuitive Surgical, Sunnyvale, CA) was brought over the legs from the caudal direction and engaged with the ports. The urachus was identified and dissected off the anterior abdominal wall to the level of the bladder. A trans-abdominal hitch stitch was used through the anterior bladder wall and adjusted to allow for stabilization of the surgical field. A full-thickness circumferential cuff of bladder was excised along with the urachal remnant and placed in an endoscopic bag for removal. The bladder cuff was closed in two layers with a 3-0 absorbable suture, and the bladder was distended via the Foley catheter to ensure a watertight closure. After inspecting for hemostasis, the ports were removed under direct vision. Catheter drainage is continued for 24–48 h postprocedure.
Conclusions:
Robot-assisted laparoscopy is an excellent management option for urachal anomalies in pediatric patients. This modality offers pediatric surgical specialists and their patients an effective minimally invasive tool for increased precision during complex pediatric surgical procedures that require reconstruction.
Runtime of video: 6 min
Get full access to this article
View all access options for this article.
