Abstract
Abstract
Introduction:
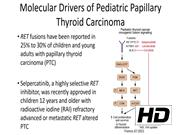
Papillary thyroid carcinoma (PTC) in children and adolescents harbor distinct genetic alterations, and gene fusions occur at a higher frequency when compared to adults. 1 The overall survival for advanced PTC is excellent, however less than 20% will have a complete response to radioactive iodine (RAI). 2 Rearranged during transfection (RET) fusions have been reported in 25% to 30% of children and young adults with PTC. 3 Selpercatinib, a highly selective RET inhibitor, was recently approved in children 12 years and older with RAI refractory advanced or metastatic RET altered PTC. The use of MAPK inhibitors can result in increased thyroid differentiation, sodium-iodine symporter expression, and RAI uptake. 4
Description of the Case:
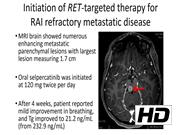
A 13-year-old girl presented at an outside institution with multiple large neck masses. Biopsy of a cervical lymph node demonstrated PTC harboring a NCOA4-RET fusion. CT scan revealed bilateral level II, III, IV, V, and VI lymphadenopathy and pulmonary metastases. Total thyroidectomy and bilateral central and lateral lymph node dissection revealed follicular variant PTC with TNM staging T4aN1bM1. Patient received 40 mCi I-131 and post-RAI whole body scan (WBS) revealed lung metastases and bone metastases involving the spine and pelvis. TSH stimulated thyroglobulin (Tg) was >5000 ng/mL. Patient received two additional RAI treatments with a cumulative dose of 285 mCi. She transferred care to our institution 17 months after her last RAI treatment for persistent RAI refractory disease and increasing dyspnea. She had tachypnea with bilateral rales at rest and worsening dyspnea with exertion. Tg on levothyroxine was 232.9 ng/mL with a thyroglobulin antibody of 2 IU/mL. Fluorodeoxyglucose-positron emission tomography CT revealed extensive lung metastases, sclerotic lesions throughout the spine and left humeral head, and multiple hyperdense lesions in the brain. MRI brain showed numerous enhancing metastatic parenchymal lesions with largest lesion measuring 1.7 cm. I-123 WBS showed avid intracranial and pulmonary lesions and no uptake in bone lesions. Oral selpercatinib was initiated at 120 mg twice per day. After 4 weeks, patient reported mild improvement in breathing, and Tg improved to 21.2 ng/mL. After 8 and 16 weeks, MRI brain showed interval decrease in size of the metastatic lesions and resolution of some lesions, and CT chest revealed stable pulmonary lesions. At 20 weeks, the thyroglobulin remained stable at 20.7 ng/mL. The patient remains on selpercatinib for 6 months with no adverse events and continues to have clinical improvement.
Discussion:
Selpercatinib is effective in children with metastatic RET fusion-positive PTC that is refractory or not amenable to RAI treatment and shows activity against intracranial lesions. Further investigations are necessary to determine length of treatment, durability of response, and effect on RAI avidity.
No competing financial interests exist
.
This case was previously presented as a poster presentation at the 90th Annual Meeting of the American Thyroid Association.
https://www.liebertpub.com/doi/10.1089/thy.2021.29115.abstracts.
Running time of video: 6 mins 19 secs

Get full access to this article
View all access options for this article.
