Abstract
Abstract
Introduction:
Temporary and permanent hypoparathyroidism with resulting hypocalcemia is the most common complication after total thyroidectomy and seen in up to 30% and 10% of patients undergoing total thyroidectomy, respectively. That condition may result in prolonged hospitalization and multiple clinic visits, neuromuscular symptoms, need for life-long calcium and vitamin D supplementation, and long-term complications. The incidence depends on the technical difficulty of the procedure and expertise of the surgeon; with the introduction of near-infrared technology permitting autofluorescence and angiography of the parathyroid glands, the management of parathyroid glands has been improved. Intraoperative angiography for the evaluation of adrenal glands is also possible when sparing adrenalectomy is performed to assess the vascularization of the adrenal remnant.
Methods:
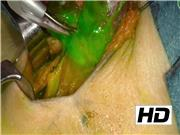
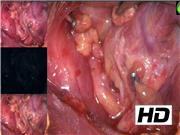
Different neck endocrine surgical situations are shown, using autofluorescence to identify parathyroid gland (PG) and using angiography with indocyanine green dye to assess parathyroid gland perfusion and functional status. Then, a case of PG dissection under live intraoperative angiography is presented and then a case using a combination of both techniques. Finally, indocyanine green (ICG) angiography to assess the perfusion of a PG remnant during subtotal parathyroidectomy in a patient with secondary hyperparathyroidism is shown and, applying the same principles, a case of sparing adrenalectomy for a patient with Conn Syndrome is also shown. For autofluorescence images, Fluobeam® (Fluoptics, Grenoble, France) was used and for angiographic evaluation both Stryker devices PINPOINT and SPY-PHI (Novadaq, Ontario, Canada) were used.
Results:
The postoperative course was uneventful for all patients. In cases in which autofluorescence device was used, all parathyroid glands were identified, including when a parathyroid gland was missing and was easily found in the central neck dissection. In cases in which parathyroid angiography was used to evaluate the PG perfusion, some PGs were visually well perfused, but the angiography showed that it was not the case and a small incision showed indeed no active bleeding; this allowed the extraction and subsequent reimplantation of the PG in some cases, and limited contralateral thyroid resection in other cases. When angiography was used to evaluate the perfusion of the parathyroid remnant, no patient developed hypoparathyroidism. As far as the adrenal gland is concerned, the perfusion of the adrenal remnant was evaluated but without being able to evaluate the overall adrenal function (the contralateral adrenal gland remaining in situ). Three months after the cortical-sparing adrenalectomy, the radiologic study confirmed the presence of the remnant with good perfusion characteristics.
Conclusion:
Autofluorescence and ICG angiography have been the latest acquisitions in endocrine surgery and they are the only available real-time tools able to intraoperatively change the course of the surgery; they are now being widely used and performed in endocrine neck surgery to identify, preserve, and understand PG perfusion and so to help surgeons with intraoperative decision-making. As for adrenal gland evaluation, new applications are being evaluated.
No competing financial interests exist.
Runtime of video: 9 mins 19 secs
Presented at the International Association of Endocrine Surgeons meeting in August 2019.

Get full access to this article
View all access options for this article.
