Abstract
Abstract
Introduction:
A young adult female member of a well-characterized Type 2 C Von Hippel-Lindau (VHL) kindred presented for annual surveillance. Her VHL has manifested as organ of Zuckerkandl paraganglioma, thoracic paraganglioma, and left adrenal pheochromocytoma tumors, which have been serially resected. On presentation, she did not report any symptoms of catecholamine excess, but was found to have elevated 24 hours urine normetanephrine and norepinephrine levels. A 2.3 cm enhancing right adrenal mass with delayed washout was present on abdominal CT. Owing to prior left total adrenalectomy and young age, a cortical-sparing approach was recommended.
Materials and Methods:
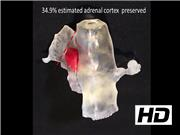
For surgical planning, three-dimensional (3D) radiographic reconstructions were made from digital segmentations of the inferior vena cava, right adrenal gland, and pheochromocytoma using Mimics and 3-Matic software (Materialise, Belgium). A color model of the structures was made using a Form2 3D printer (FormLabs, Cambridge, MA). The 3D model showed the tumor mass centered in the medial limb of the adrenal gland. A resection plane was apparent, allowing for preservation of an estimated 34.9% of normal gland.
Results:
The surgery was completed with preservation of the lateral limb and superomedial cortex. Intraoperative ultrasonography was not required. Final pathology analysis showed a 2.6 cm pheochromocytoma with clear margins. She had an uneventful recovery and was discharged on postoperative day 1 on minimal glucocorticoid replacement. No episodes of adrenal insufficiency or other postoperative complications occurred. Plasma metanephrine levels were normal 3 weeks after resection. She remains stable on low-dose corticosteroids because of pregnancy.
Conclusions:
Adrenocortical preservation is advocated for selected pheochromocytoma patients with genetic syndromes, including VHL when risk of tumor recurrence and low malignancy rate is weighed against the need for lifelong steroid hormone, risk of Addisonian crisis, and diminished quality of life associated with total bilateral adrenalectomy.1–3 Cortical-sparing adrenalectomy has been described in >300 VHL/MEN2 patients in the literature, with normal glucocorticoid function achieved in 57% to 100% of patients after surgery. 4 Preoperative planning for cortical-sparing adrenalectomy can be challenging, particularly in settings of multifocality and prior partial or total adrenalectomy. Conventional CT imaging is typically used to assess the feasibility of cortex sparing, but 3D anatomic modeling can provide additional spatial information to aid in executing safe dissection, complete tumor resection, and optimal adrenal remnant volume. 3D modeling is also a useful adjunct in preoperative surgical discussion with patients and in education of surgical learners of all levels. 3D resin model preparation and printing is affordable and requires little labor. In this case, the model was completed in 90 minutes, at a cost of $3.62 in materials and $82.00 for infrastructure/labor.
No competing financial interests exist.
Runtime of video: 5 mins 55 secs


Get full access to this article
View all access options for this article.
