Abstract
Abstract
Introduction:
Insulinomas are the most common functioning pancreatic neuroendocrine tumors. They are rare with an incidence of approximately four cases per million people per year. They are commonly benign, solitary, and sporadic tumors. In contrast to the benign counterpart, malignant insulinoma accounts for less than 15% of the cases of insulinoma. The diagnosis of insulinoma is mainly based on clinical manifestations of hypoglycemia, the laboratory documentation of a fasting hypoglycemia of <50 mg/dL, and with the demonstration that such symptoms of hypoglycemia are relieved with the administration of glucose (Whipple's triad). Surgical excision is the method of choice for treatment of insulinoma. We present a laparoscopic distal pancreatectomy and splenectomy for an insulinoma in the body of the pancreas. The final pathology report unexpectedly showed a well-differentiated (G2) malignant insulinoma with lymph node metastases.
Case:
A young female (<50 years old) who presented with a 2-month history of episodic dizziness, shaking, and sweating alleviated with eating or drinking carbonated beverages. Her initial random glucose level was 44 mg/dL, insulin 56.1μM/mL, proinsulin 22.7 pM, C-peptide 4.3 ng/mL, and beta-hydroxybutyrate 0.8 mg/dL. An MRI of the abdomen demonstrated a 3.2 × 1.4 cm hypervascular lesion in the body of the pancreas with no involvement of the pancreatic duct.
Surgical Technique:
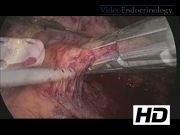
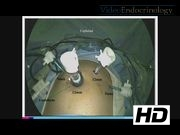
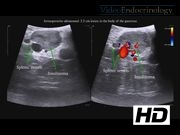
Under general anesthesia, the patient was positioned in the supine-split leg position. A 12-mm Hasson port was placed in the supraumbilical region, a 5- and 12-mm ports were placed in the left upper quadrant, and a 5-mm port in the right upper quadrant. The lesser sac was accessed to allow visualization of the pancreas. The visceral peritoneum overlying the inferior edge of the pancreas was incised, and the pancreas was dissected away from its retroperitoneal attachments. A laparoscopic ultrasound was used to identify the lesion, which was located in the anterior pancreatic body, measuring 3 cm in diameter and had a slightly irregular border. Given the size of the lesion and the irregular appearance, we elected not to do an enucleation and to perform a distal pancreatectomy. We attempted to dissect the splenic vessels from the pancreas to preserve the spleen, but this maneuver was difficult as the splenic vessels were encased within pancreatic tissue. Therefore, we elected to divide the splenic vessels with the specimen and to perform a splenectomy. The spleen was removed from the abdominal cavity en-block with the distal pancreas. A drain was left in the abdominal cavity.
Postoperative Course:
The postoperative recovery was uneventful. On postoperative day 3, the patient was discharged home without complications. The pathology report showed a well-differentiated insulinoma (G2, intermediate grade) with margins of resection negative for tumor and 2/12 lymph nodes positive for metastatic disease. Postoperatively, the patient was placed on postoperative chemotherapy treatment.
Conclusion:
Laparoscopic excision of pancreatic neuroendocrine tumors is a feasible procedure. Regardless of the tumor size or appearance, the diagnosis of malignant insulinoma should always be considered at the time of resection. In this particular case, the diagnosis of malignancy was made after the final pathology report was obtained.
No competing financial interests exist.
Runtime of video: 9 mins 20 secs
Keywords
Get full access to this article
View all access options for this article.
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
