Abstract
Statins improve pulmonary vascular remodeling and right ventricular hypertrophy in animal models of pulmonary arterial hypertension (PAH). However, clinical trials assessing the efficacy of statins in patients with PAH have reported mixed results. In this systematic review and meta-analysis, we assess the efficacy of statins in patients with PAH. We included randomized controlled clinical trials (RCTs) that evaluated the efficacy of statins in patients with PAH. Primary outcomes were mortality and change in 6-minute walk distance (6MWD). Data are presented as odds ratio (OR) and weighted mean difference (WMD), with 95% confidence intervals (CIs), for binary and continuous variables, respectively. We included 4 RCTs of high quality. The mean age of participants was 42 ± 13 years, and 70% were women. The statins used were simvastatin at 40–80 mg in two trials, atorvastatin 10 mg in one trial, and rosuvastatin 10 mg in the other. In the pooled-data analysis, there was no statistically significant improvement in mortality (OR: 0.75 [95% CI: 0.32–1.74]), 6MWD (WMD: −9.27 [95% CI: −27.73 to 9.20]), or cardiac index (WMD: 0.11 [95% CI: −0.04 to 0.27]) with statin therapy when compared to placebo. There was no difference in adverse events leading to withdrawal of therapy between statin and placebo groups. These data suggest that statins are not beneficial in the treatment of PAH. There is a need for large, well-conducted clinical trials assessing the effects of statins in patients with PAH. Future trials should include homogeneous patient populations and should be long-term, event-driven trials with combined morbidity and mortality end points.
Pulmonary arterial hypertension (PAH) is a fatal disease characterized by increased pulmonary vascular resistance leading to right heart failure and eventually death. 1 Pulmonary vasoconstriction, thrombosis, small-vessel remodeling with increased proliferation of vascular smooth muscle cells and endothelial cells, and inflammation contribute to increased pulmonary vascular resistance. 2 Although significant progress has been made in the past 2 decades, PAH, unfortunately, continues to remain a fatal disease, with a 1-year mortality of ∼10%–15%.3–5 All currently approved therapies for PAH cause pulmonary vasodilatation by targeting one of three pathways: endothelin, nitric oxide, or prostacyclin. 6 There is an unmet need for novel therapies in PAH that can reverse vascular remodeling by targeting pulmonary vascular smooth muscle and endothelial cell proliferation.
Statins have pleiotropic effects that include antiproliferative, antithrombotic, antioxidant, and anti-inflammatory properties, making them an attractive option for treatment of PAH. As such, statins have been shown to prevent and reverse pulmonary vascular remodeling in several animal models of PAH by virtue of their proap-optotic and antiproliferative effects on pulmonary artery smooth muscle cells.7–10 Subsequently, based on these animal data, several randomized control trials (RCTs) and observational studies have studied the effect of statins in PAH, with mixed results.11–15
One small observational study 12 showed improvements in 6-minute walk distance (6MWD), cardiac output, and right ventricular systolic pressures, along with attenuation of the rate of disease progression, in patients with PAH and secondary pulmonary hypertension treated with simvastatin. RCTs have shown transient improvement in biomarkers and right ventricular mass 14 but mixed results for changes in 6MWD with statins, compared to placebo.14,15 Given these mixed results and small study sizes, we conducted a systematic review and meta-analysis of the randomized studies to evaluate the benefits of statin therapy in patients with PAH.
METHODS
Search strategy
A search of PubMed, EMBASE, and the Cochrane Library was performed, with the following MeSH (medical subject headings) terms and keywords: “pulmonary hypertension,” “pulmonary arterial hypertension,” and “statin” (full search strategy available on request). We hand-searched the abstracts from American Heart Association, American College of Cardiology, American Thoracic Society, CHEST (American College of Chest Physicians), European Respiratory Society, and European Society of Cardiology scientific conferences from 2011 to 2015. We also searched clinicaltrials.gov for ongoing or unpublished trials. An updated literature search was last performed on February 10, 2016. From this list, published clinical trials evaluating the effect of statins in PAH and inoperable chronic thromboembolic pulmonary hypertension were identified. Abstracts without full-text publication were also eligible for inclusion. Only articles written in English and on clinical trials conducted in humans were included. The references cited in the included articles were also examined for additional studies. The search strategy was conducted according to the PRISMA (preferred reporting items for systematic reviews and meta-analyses) guidelines. 16 The protocol of our systematic review and meta-analysis was prespecified but not registered or published.
Study selection and inclusion criteria
We included all RCTs that met the following inclusion criteria in our meta-analysis: (1) patients had any type of PAH (idiopathic; heritable; drug- or toxin-induced; or associated with connective-tissue disease, HIV infection, portal hypertension, congenital heart disease, schistosomiasis, or chronic hemolytic anemia) or inoperable chronic thromboembolic pulmonary hypertension; (2) the trial evaluated the effect of statin therapy on mortality, exercise capacity, hemodynamics, and/or plasma biomarkers. Two reviewers (VA and SG) independently assessed all selected abstracts and titles to identify articles for inclusion in the systematic review and meta-analysis. In case of disagreements, we consulted one of the other authors (TT).
Data extraction and management
Two reviewers (VA and SG) independently extracted the data, using a predefined data extraction form. The details extracted from each study included general characteristics of the study (study design, setting, follow-up, number of patients randomized and analyzed), characteristics of the participants (age, sex, World Health Organization category of pulmonary hypertension), and characteristics of the intervention (statin type, dose, and duration of treatment). Discrepancies between reviewers were resolved through discussion and consensus.
Risk-of-bias assessment
Two reviewers (VA and SG) independently assessed the risk of bias in the included RCTs, using the Cochrane Collaboration's tool for assessing risk of bias. 17 Any disagreements were resolved by consulting with one of the other authors (TT). The following 6 components of the risk-of-bias assessment tool were evaluated: selection bias (sequence generation and allocation sequence concealment), performance bias (blinding of participants), detection bias (blinding of outcome assessors), attrition bias (incomplete outcome data), reporting bias (selective outcome reporting), and other biases (i.e., baseline imbalance). The studies were graded as low, unclear, or high risk of bias for each component, and the findings of the final assessment were included in the risk-of-bias graph (Fig. 2).
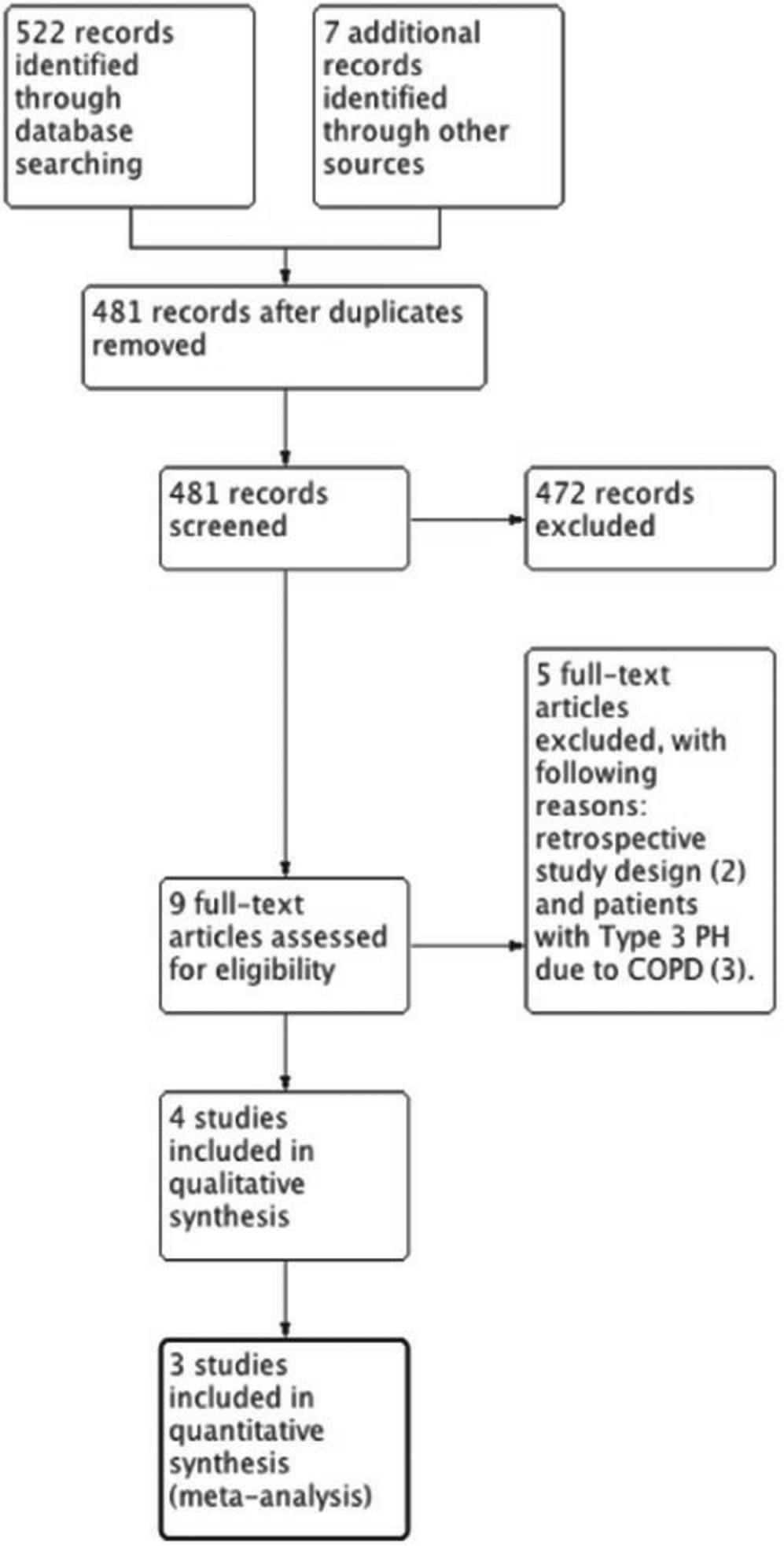
Preferred reporting items for systematic reviews and meta-analyses (PRISMA) study flow diagram. PH: pulmonary hypertension; COPD: chronic obstructive pulmonary disease.
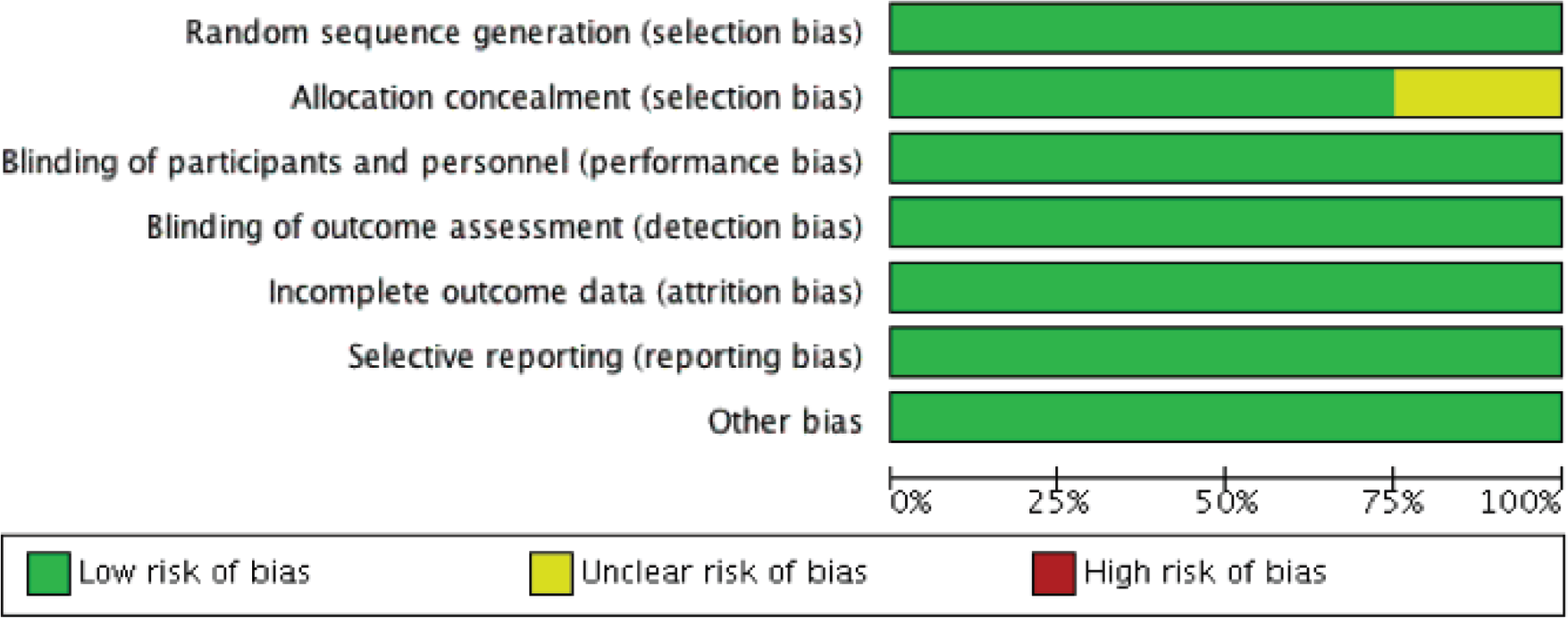
Risk-of-bias assessment.
Outcome variables
Mortality and change in 6MWD from baseline to follow-up were the primary outcomes in this study. Secondary outcomes included in this study were cardiac index, pulmonary artery systolic pressure, Borg dyspnea score, plasma biomarkers, and adverse events leading to discontinuation of study drug.
Statistical analysis
We used the random-effects model to conduct the meta-analysis of the outcomes and assessed for heterogeneity with the I2 statistic. We calculated odds ratio (OR) with 95% confidence intervals (CIs) for the dichotomous outcomes and weighted mean difference (WMD) with 95% CI for the continuous outcomes. In the meta-analysis of mortality, we included studies with no events by adding a correction factor of 0.5 to each cell of the 2 × 2 table. All statistical analyses were performed with Stata software, version 12.1. 18
RESULTS
Our comprehensive search identified 481 studies (randomized and nonrandomized) after duplicates were removed. Of the 481 studies, we excluded 472 by review of the title and abstract. The full text was obtained and reviewed for the remaining 9 studies. Of these 9 studies, there were 4 RCTs,11,13–15 which were included in the systematic review after being assessed against the inclusion criteria. We created a flowchart of study selection, as suggested by the PRISMA statement (Fig. 1). Four studies (by Barreto et al. 11 in 2008, Wilkins et al. 14 in 2010, Kawut et al. 13 in 2011, and Zeng et al. 15 in 2012) were included in the systematic review, and the last three of these were included in the meta-analysis. Table 1 summarizes the inclusion and exclusion criteria of the included studies.
Inclusion and exclusion criteria and baseline characteristics of the studies entered in the systematic review
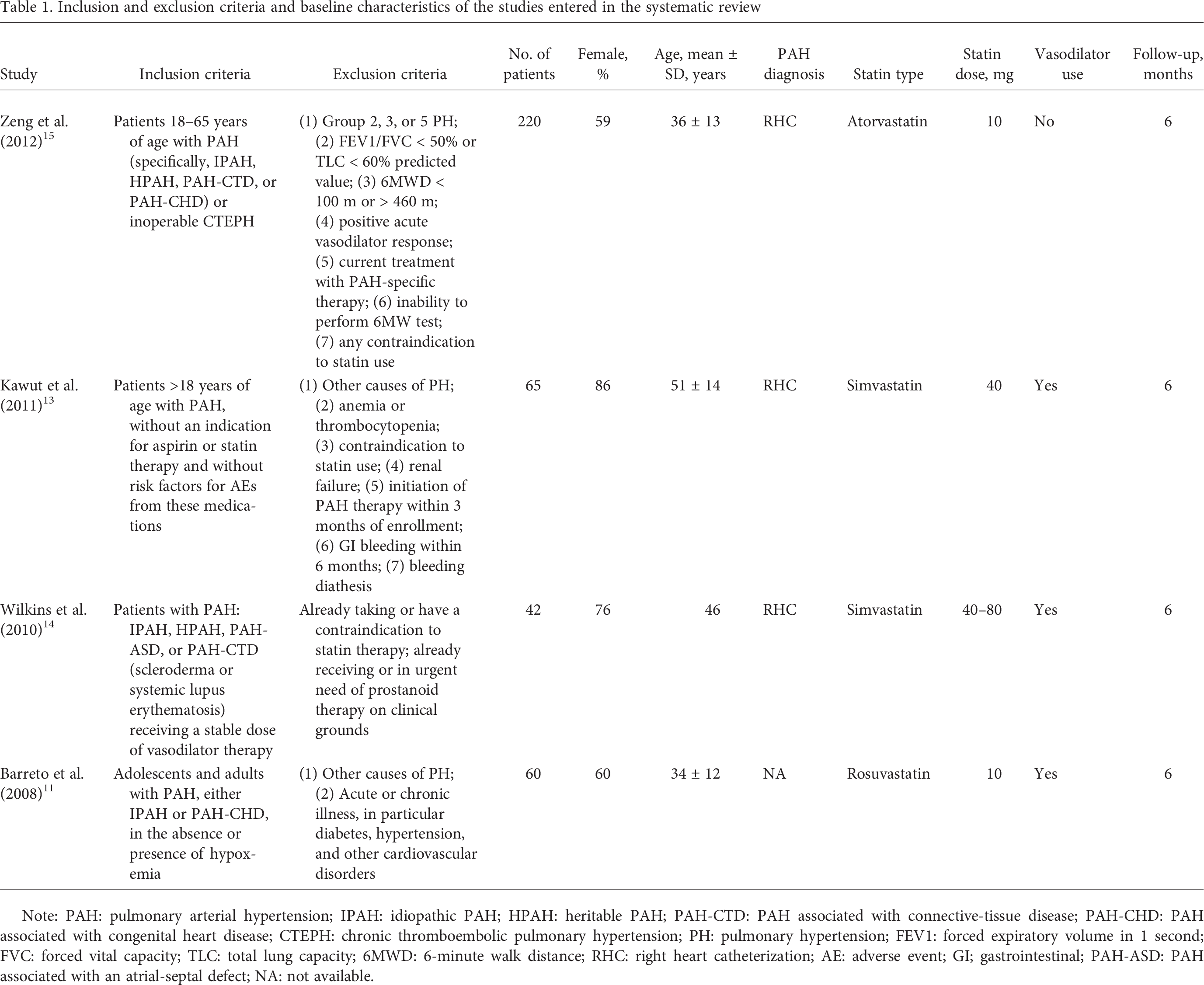
Note: PAH: pulmonary arterial hypertension; IPAH: idiopathic PAH; HPAH: heritable PAH; PAH-CTD: PAH associated with connective-tissue disease; PAH-CHD: PAH associated with congenital heart disease; CTEPH: chronic thromboembolic pulmonary hypertension; PH: pulmonary hypertension; FEV1: forced expiratory volume in 1 second; FVC: forced vital capacity; TLC: total lung capacity; 6MWD: 6-minute walk distance; RHC: right heart catheterization; AE: adverse event; GI; gastrointestinal; PAH-ASD: PAH associated with an atrial-septal defect; NA: not available.
We included 387 patients from 4 studies. Simvastatin 40–80 mg was used in the Kawut et al. 13 and Wilkins et al. 14 studies, atorvastatin 10 mg in the Zeng et al. 15 study, and rosuvastatin 10 mg in the Barreto et al. 11 study. The mean duration of follow-up in the included RCTs was 6 months. The mean age of participants in the RCTs was 42 ± 13 years, and 70% were women. Table 1 summarizes the baseline characteristics of the study participants in the studies included in the systematic review. The ASA-STAT study (Kawut et al. 13 ) was a 2 × 2 factorial randomized trial of statin and aspirin, and we included the statin arm compared to placebo in this systematic review and meta-analysis.
Quality assessment
Overall, the quality of the trials was high (Fig. 2). The random sequence generation was defined in all 4 randomized trials. The allocation was concealed in the Barreto et al., 11 Kawut et al., 13 and Wilkins et al. 14 studies and unclear in the Zeng et al. 15 study. The blinding of participants and outcome assessors was reported in all studies, reflecting an overall low risk of detection bias. Similarly, the dropout rate was low in all studies, reflecting altogether a low risk of attrition bias.
Effect of statins on mortality
The Wilkins et al., 14 Kawut et al., 13 and Zeng et al. 15 studies reported data on mortality. There were 9 deaths in the atorvastatin group and 11 deaths in the placebo group in the Zeng et al. 15 study, and 1 death in the simvastatin group and 2 in the placebo group in the Kawut et al. 13 study. There were no deaths in the Wilkins et al. 14 study. In the meta-analysis of these studies, statin therapy was not associated with a reduction in mortality at 6 months, compared with the placebo-treated group (OR: 0.75 [95% CI: 0.32–1.74]; Fig. 3A). The statistical heterogeneity was small (I2 = 0%).
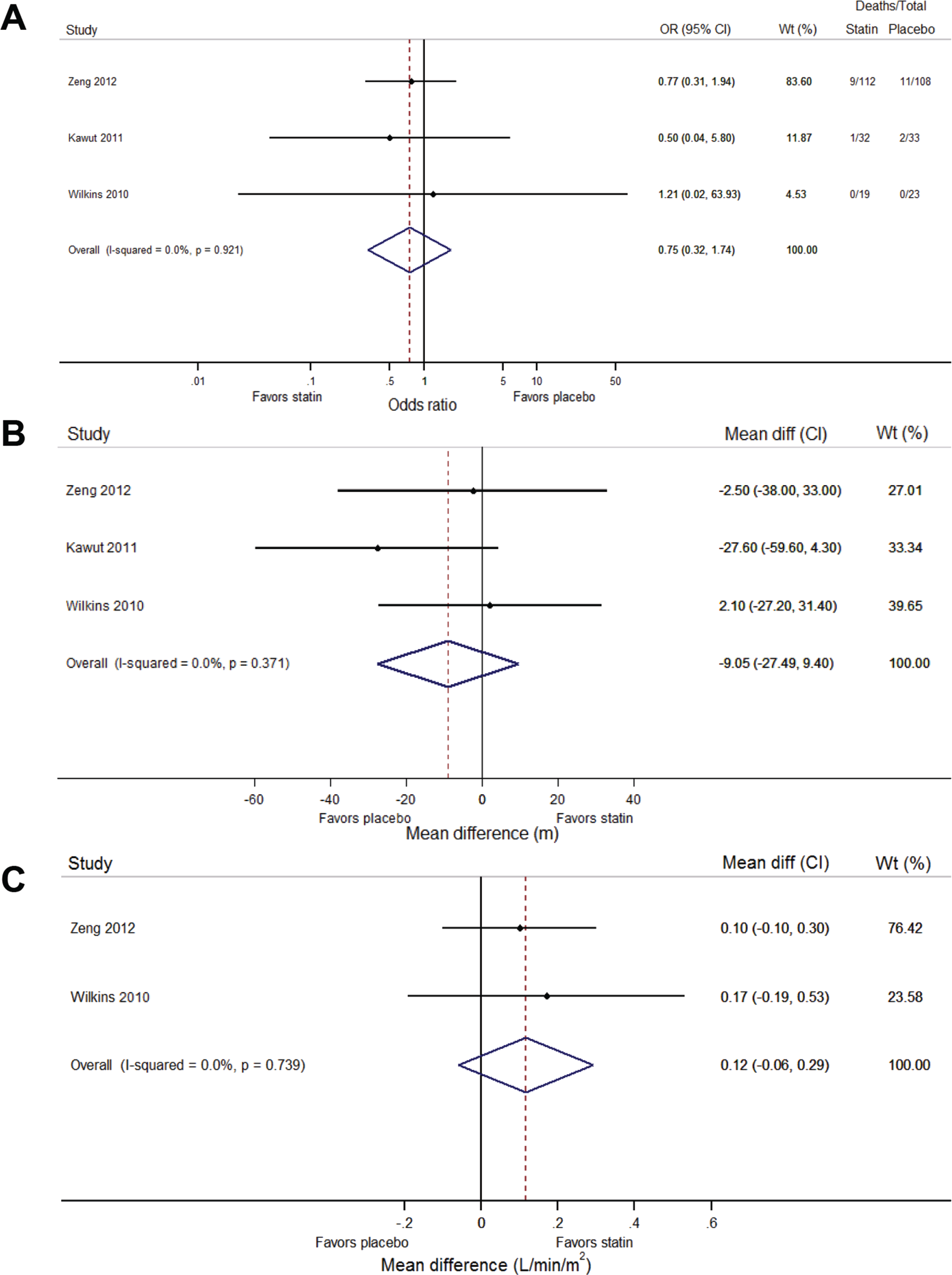
Effect of statins on mortality (A), 6-minute walk distance (B), and cardiac index (C) in patients with pulmonary arterial hypertension. There was no significant difference in mortality, 6-minute walk distance, or cardiac index between statin- and placebo-treated groups. Studies: Zeng et al. (2012), 15 Kawut et al. (2011), 13 and Wilkins et al. (2010). 14 OR: odds ratio; CI: confidence interval.
Effect of statins on 6MWD
The Wilkins et al., 14 Kawut et al., 13 and Zeng et al. 15 studies reported data on 6MWD. There was no statistically significant change in 6MWD with statin therapy, when compared to placebo (WMD: −9.27 m [95% CI: −27.73 to 9.20]; Fig. 3B). The statistical heterogeneity was small (I2 = 1.7%).
Effect of statins on secondary outcomes
The Wilkins et al. 14 and Zeng et al. 15 studies reported cardiac index, which did not improve significantly with statin therapy, compared to placebo (WMD: 0.11 [95% CI: −0.04 to 0.27])] (Fig. 3C). Overall, the statistical heterogeneity was small (I2 = 0%). Only one trial (Zeng et al. 15 ) reported mean change in pulmonary artery pressures, and there was no change compared to placebo (mean: 4 mmHg [95% CI: 0–7] vs. 3 mmHg [95% CI: −1 to 6]; P = 0.94). There was no significant difference in Borg dyspnea score with statin therapy, compared to placebo, in the Kawut et al. 13 and Zeng et al. 15 studies. The median postwalk Borg dyspnea score at 6 months follow-up in the Kawut et al. 13 study was similar in patients assigned to simvastatin (3; interquartile range [IQR]: 2–4)] and placebo (3; IQR: 2–4) treatment. Similarly, the Zeng et al. 15 study showed no change in Borg dyspnea score from baseline in either the atorvastatin (from 3 [IQR: 2–4] to 3 [IQR: 2–5]) or placebo (from 3 [IQR: 2–4] to 3 [IQR: 2–5]) groups. These data were not combined because of different ways of reporting data.
In the study by Barreto et al., 11 rosuvastatin treatment significantly lowered P-selectin levels (mean ± SD: from 39.9 ± 18.5 ng/mL at baseline to 35.4 ± 13.9 ng/mL at 6 months), compared to placebo (from 45.7 ± 26.8 ng/mL at baseline to 45.7 ± 25.6 ng/mL at 6 months). In addition, there was a nonsignificant (P = 0.094) trend toward reduction in tissue-plasminogen activator in the statin group (16% reduction), with no significant changes in von Willebrand factor antigen and tissue-plasminogen inhibitor. The Wilkins et al. 14 study showed a significant decrease in serum N-terminal pro–B-type natriuretic peptide level in patients treated with simvastatin at 6 months, compared to the placebo group (P = 0.041), but this was not sustained over 12 months.
The common adverse effects associated with statin therapy in PAH patients included liver function abnormalities, bleeding, irregular menstrual cycles, abdominal distention, abdominal pain, paresthesia, dizziness, myalgia, elevated creatine kinase, and insomnia. The adverse events leading to withdrawal of statin therapy were abnormal liver function, abdominal discomfort, and dizziness. There was no difference in adverse events between the statin and placebo groups.13–15 Two studies reported adverse events leading to withdrawal of study drug, and there was no statistically significant difference between the statin and placebo groups in the number of patients who discontinued treatment because of adverse events (4 vs. 3 in Zeng et al. 15 and 0 vs. 1 in Wilkins et al. 14 ).
DISCUSSION
In this systematic review and meta-analysis, we assessed the effect of statin therapy in patients with PAH. Statins were well tolerated, but there was no significant improvement in 6MWD, hemodynamics (cardiac index and pulmonary artery pressure), and mortality with statin therapy, compared to placebo. These results do not validate the use of statin therapy for PAH.
Statins have well known anti-inflammatory and antiproliferative effects on the cardiovascular system.19,20 In addition, statins increase prostacyclin and decrease endothelin levels, properties that are beneficial in the treatment of PAH. 21 Consistent with this concept, various animal models of PAH have shown beneficial effects of statins on mean pulmonary arterial pressures, right ventricular hypertrophy, endothelial dysfunction, pulmonary vascular remodeling, and inflammation.7–10 Although the effect of statins on pulmonary vascular remodeling in animal models of PAH is convincing, only a few clinical trials with small sample sizes have studied the role of statins in patients with PAH.11,13–15 In these trials, statins improve biochemical markers of pulmonary hypertension progression, including N-terminal pro–B-type natriuretic peptide and P-selectin levels,11,14,22 but their effect on clinical outcomes has been mixed, with some studies showing improvement in 6MWD at 6 months but not at 1 year. In our pooled analysis of these RCTs, there is no significant improvement in 6MWD or reduction in mortality with statin therapy, compared to placebo. Furthermore, statin therapy neither decreases pulmonary artery pressure nor increases cardiac index.
There are several possible reasons why the beneficial effects of statins observed in animal models of PAH have not been replicated in human studies. First, it is conceivable that statins do not cause significant reverse remodeling of the pulmonary arteries and/or do not improve right ventricular function in human PAH. In fact, unlike other animal studies of statins in PAH, a study by McMurtry et al. 23 questions the role of statins in pulmonary vascular remodeling in monocrotaline-induced PAH. Furthermore, similar to statins, several other therapies that have been shown to be effective in various animal models of PAH have not been shown to be beneficial in human PAH.24,25 Second, the neutral results may also be due to small sample size and short duration of therapy. The mean duration of statin therapy in all 4 RCTs was only 6 months. Unlike therapies causing predominantly pulmonary vasodilatation, which improve symptoms with just 12 weeks of therapy, drugs targeting pulmonary vascular remodeling perhaps need a longer duration of therapy to produce clinically meaningful benefits. Finally, perhaps, the use of different statins at variable doses might have also contributed to lack of significant improvement in clinical outcomes in our meta-analysis.
Studies that have evaluated the role of statins in World Health Organization group III pulmonary hypertension secondary to chronic lung disease have also reported conflicting results. One study with pravastatin in patients with pulmonary hypertension due to chronic obstructive pulmonary disease showed improvement in exercise time, Borg dyspnea score, and pulmonary artery systolic pressure. 22 In contrast, another study with a similar number of patients found no difference in 6MWD, pulmonary artery pressures, or cardiac output. 26
The strengths of our meta-analysis include qualitative and quantitative analysis of all the available data from randomized studies evaluating the role of statins in PAH. However, our study has several limitations. Our meta-analysis included a heterogeneous patient population with all types of PAH. Prognosis is significantly different for different etiologies of PAH. For example, patients with congenital heart disease–associated PAH have a much better prognosis and those with connective-tissue disease–associated PAH have poor survival compared to those with idiopathic PAH. Thus, it is possible that statins are beneficial only in a certain subtype of PAH. We were unable to conduct a subgroup analysis because of the small sample size. The study by Zeng et al. 15 included a small number of patients (n = 34) with inoperable chronic thromboembolic pulmonary hypertension. This could have influenced our results, but we believe that it is less likely to have done so, as those patients accounted for only 8.7% of the total study cohort. Some of the other limitations include small sample size and different ways of reporting clinically relevant outcomes, such as 6MWD and Borg dyspnea score, in the studies included in the meta-analysis. Another potential bias in this meta-analysis is the inclusion of studies in the English language only.
There is a need for large, well-conducted clinical trials assessing the effects of statins in patients with PAH. Future trials should include a homogeneous patient population (idiopathic PAH or connective-tissue disease–associated PAH only) and should be long-term, event driven trials with combined morbidity and mortality end points similar to those of recent PAH clinical trials.18,27,28 The treatment effect of statins on various outcomes, including 6MWD, mortality, Borg dyspnea score, and hemodynamics from current studies, could be used to determine the sample size for future trials evaluating the role of statins in PAH.
In conclusion, statins are well tolerated in patients with PAH, but they are not associated with significant improvement in hemodynamics, 6MWD, or survival. These data do not support the use of statins for treatment of PAH at present.
Footnotes
ACKNOWLEDGMENTS
We would like to acknowledge Dr. Ambarish Pandey, Division of Cardiovascular Medicine, Department of Medicine, University of Texas Southwestern Medical Center, Dallas, Texas, for his advice.
