Abstract
Iloprost is a selective pulmonary vasodilator approved for inhalation by the Food and Drug Administration. Iloprost has been increasingly used in the management of critically ill neonates with hypoxic lung disease. This in vitro study was designed to test the hypothesis that aerosol drug delivery could be effectively administered to infants with both conventional ventilation and high-frequency oscillatory ventilation (HFOV). A neonatal test lung model configured with newborn lung mechanics was ventilated with a conventional ventilator and an HFOV with standard settings. A vibrating-mesh nebulizer was placed (1) proximal to the patient airway in the inspiratory limb between the humidifier probe and patient wye (conventional) as well as between the vent circuit and the endotracheal tube (ETT) for HFOV and (2) between the ventilator and humidifier (distal). Iloprost was nebulized in three separate runs using three new nebulizers in each of the circuit locations. A collecting filter was placed at the distal end of the ETT for each trial. Iloprost was quantified using high-performance liquid chromatography. The percentage of nominal dose delivered was greater with the nebulizer placed proximal to the airway for conventional ventilation (10.74% ± 2%) and HFOV (29% ± 2%) than with it placed in the distal position (2.96% ± 0.2% vs. 0.96% ± 0.8%, respectively; P < 0.05). Drug delivery in proximal position was nearly threefold greater during HFOV than during conventional ventilation. In conclusion, iloprost drug delivery was best achieved when the nebulizer was placed proximal to the patient airway during neonatal mechanical ventilation. Drug delivery appears to be more efficient during HFOV than during conventional ventilation.
Keywords
Iloprost (Ventavis; Actelion Pharmaceuticals US) is a stable prostacyclin analog used in the treatment of pulmonary hypertension. It is pharmacologically similar to epoprostenol, with vasodilatory, vascular remodeling, and platelet inhibitory properties, but it is a more stable compound, with an elimination half-life of 20–30 minutes. 1 The longer half-life than that of other prostacyclin formulations allows the drug to be delivered with less frequency. Iloprost was the first prostacyclin designed specifically for aerosolization and approved for inhalation in ambulatory adults with primary pulmonary hypertension using the I-neb AAD system (Philips Respironics, Netherlands), a vibrating-mesh smart nebulizer. The design of the I-neb precludes its use in a closed ventilator circuit. While researchers have described a strategy for aerosol delivery during adult mechanical ventilation, none have applied such strategies for use with iloprost in infants. 2
Iloprost inhalation has been reported to be of some benefit in the management of critically ill neonates and infants with hypoxic lung disease and pulmonary hypertension.3–17 Many neonates with severe pulmonary hypertension and persistence of fetal circulation require mechanical ventilation, and there are currently no recommendations for selecting aerosol delivery devices or how those devices should be configured within the patient circuit to efficiently deliver iloprost during mechanical ventilation. Findings from recent adult 18 and pediatric19–21 aerosol studies suggest greater inhaled drug mass (albuterol) distal to the endotracheal tube (ETT) when placing the nebulizer in the inspiratory circuit back at the ventilator (prior to the humidifier) than proximal to the patient wye. It is unclear whether a similar relationship exists in neonates during ventilation due to the inherently small circuit volumes, faster respiratory frequencies, and shorter inspiratory times during neonatal ventilation. There have been no forthcoming studies using an infant lung model that have addressed differences in drug delivery between different nebulizer locations during conventional ventilation or high-frequency oscillatory ventilation (HFOV). Moreover, many clinicians are hesitant to administer aerosolized drugs during HFOV on the basis of a previous report that medication delivery to infants is negligible due to the small volumes, short inspiratory times, and high gas flows used with this form of ventilation. 22
We designed this in vitro study to quantify aerosol drug delivery with the hypothesis that effective levels of aerosol drug delivery could be achieved during both conventional ventilation and HFOV and that deposition efficiency would be different using a vibrating-mesh nebulizer (VMN) between each ventilator type and at two different circuit locations.
METHODS
This study was designed and performed and data were analyzed at the Seattle Children's Hospital Respiratory Therapy Department (Seattle, WA) under the direct supervision of the first author (RMD). Aerosol devices were donated by the Respiratory Therapy Department, and laboratory supplies were purchased with funds from a research grant provided by the Center for Developmental Therapeutics, Seattle Children's Research Institute (Seattle, WA). Drug for the study was donated by Actelion Pharmaceuticals US (San Francisco, CA).
Infant lung model
A neonatal test lung model (ASL 5000 with software package ver. 3.2; IngMar Medical, Pittsburgh, PA) was configured for 3–4-kg newborn infants with compliance of 1.5 mL/cmH2O and resistance of 40 cmH2O/L/s. 23 The lung model was ventilated with a conventional ventilator and an HFOV with standard settings and heated humidification (39°C) connected to a 3.5-mm internal diameter (ID) ETT. Two bacterial/viral electret filters (Respirgard II; Vital Signs, Englewood, CO) were connected in series between the distal tip of the 3.5-mm ID ETT and the lung model. One filter was used to collect the drug delivered, while the second filter was used to protect the internal components of the lung model (Figs. 1, 2).
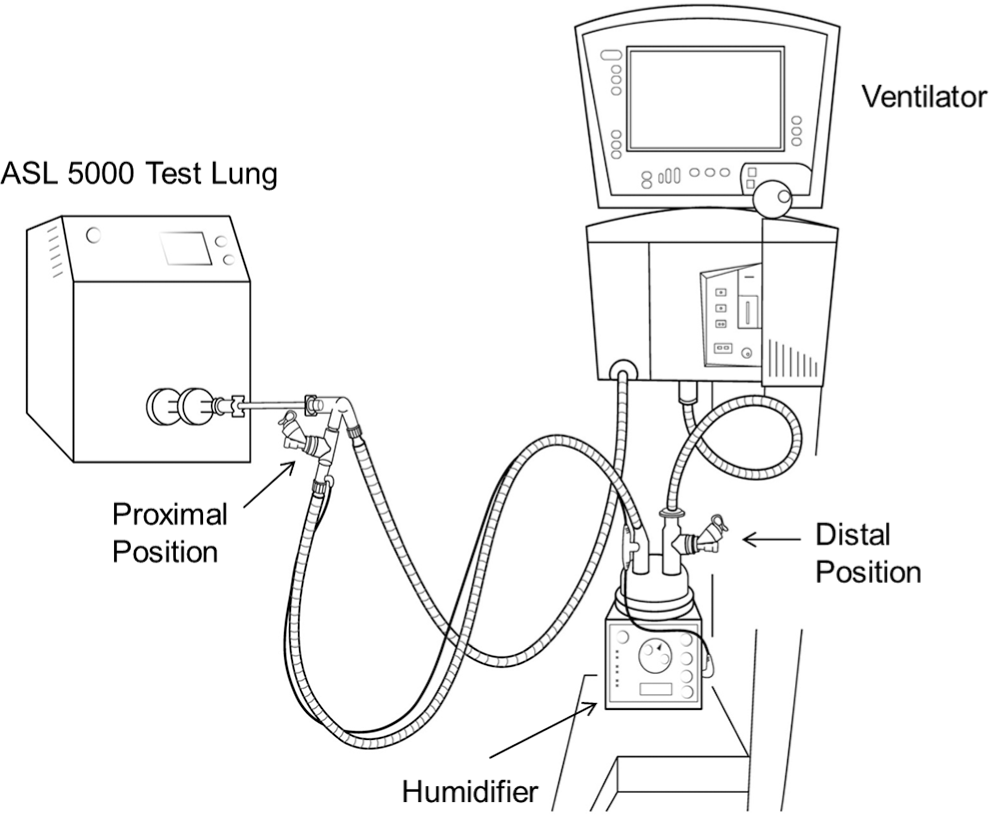
Experimental set-up for conventional ventilation. An infant lung model was devised by attaching a 3.5-mm internal diameter (ID) endotracheal tube connected to a simulated spontaneously breathing infant lung model (ASL 5000; IngMar Medical). Two bacterial/viral electret filters (Respirgard II, Vital Signs) were connected in series between the 3.5-mm ID endotracheal tube and the lung model. An AVEA critical care ventilator (CareFusion) equipped with a heated wire circuit and an MR730 heater (Fisher & Paykel) were used. Following a brief temperature stabilization period, 5 μg of iloprost was nebulized three times at each of the two positions using three new nebulizers (n = 18 measurements), and filters were collected.
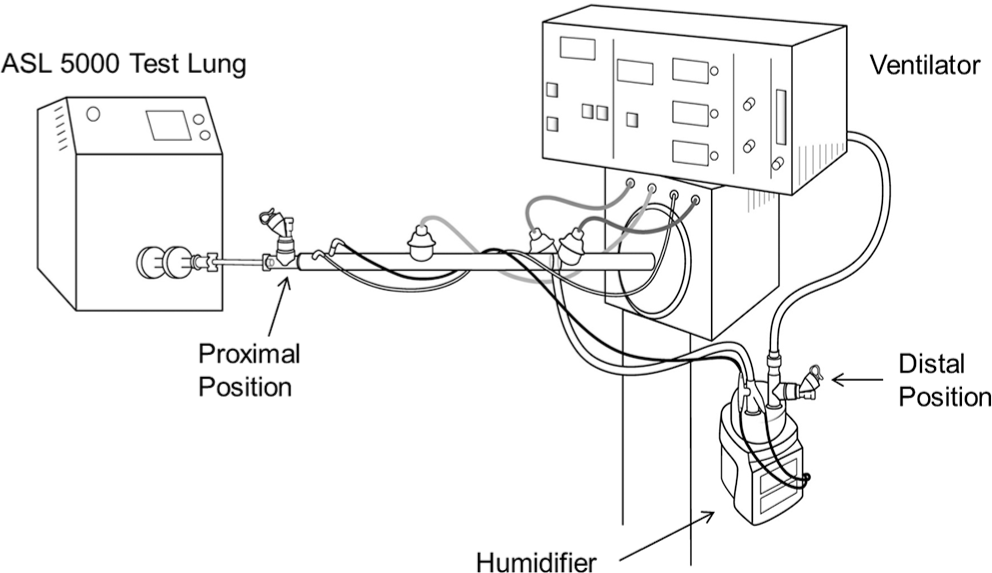
Experimental set-up for high-frequency oscillatory ventilation (HFOV). The experimental process was repeated using the same lung model as stated previously during HFOV. A Sensormedics 3100A HFOV (CareFusion) equipped with a heated wire circuit and an MR730 heater (Fisher & Paykel) were used. Following a brief temperature stabilization period, 5 μg of iloprost was nebulized three times at each of the two positions using three new nebulizers (n = 18 measurements), and filters were collected.
Ventilator and humidification
Two ventilators, an AVEA conventional critical care ventilator and a Sensormedics 3100A HFOV (CareFusion, Yorba Linda, CA), equipped with respective heated wire circuits were used for this study. An MR730 heater (Fisher & Paykel, Auckland, New Zealand) was used for humidification with both devices. The choice of setup and settings were based on what is commonly used in the clinical setting for neonates of this size at our institution. The AVEA ventilator settings with an RT266 infant circuit kit (Fisher & Paykel) were pressure control/assist control: peak inspiratory pressure of 24 cmH2O, positive end-expiratory pressure of 6 cmH2O, respiratory rate of 60 breaths/min, inspiratory time of 0.3 seconds for an I: E ratio of 1:2, Fio2 of 1.0, measured tidal volume (Vt) of 22 mL, mean airway pressure of 10 cmH2O, and bias flow of 2 L/min. The proximal hotwire flow sensor was used initially to confirm delivered Vt and then removed prior to nebulization, per manufacturer recommendations. The Sensormedics 3100A HFOV settings were mean airway pressure of 12 cmH2O, amplitude of 36 cmH2O, frequency of 10 Hz, inspiratory time percentage of 33%, bias flow of 15 L/min, and Fio2 of 1.0. The circuit and system was heated to approximately 37°C, and the lung model was warmed to 37°C for 20 minutes prior to testing. These temperatures were maintained throughout the study.
Nebulizers
Aerogen Solo VMNs (Aerogen, Galway, Ireland) were used for testing. VMNs can be placed in-line using a specialized neonatal T adaptor during mechanical ventilation. A Pro-X controller (Aerogen) was used to power the nebulizers. The recent popularity of VMNs for aerosol delivery during pediatric conventional ventilation is based on the fact that patients do not need to be disconnected from a ventilator and the nebulizer can remain in-line when not being used. Unlike jet nebulizers, no flow is added to the patient circuit by the VMNs, and this may be useful for improved patient triggering and lung protection. In addition, VMNs have been shown to provide nearly two to four times greater drug delivery than jet nebulizers during pediatric mechanical ventilation. 19
Nebulizer positions
The VMN was placed in the heated inspiratory limb just prior to the patient wye connector using the infant T-piece connector in the proximal position on the AVEA ventilator (Fig. 1). In the distal position on the AVEA ventilator (Fig. 1), the VMN was placed on the dry side of the heated humidifier using an adult T adapter placed directly on the inlet of the humidifier. In the proximal position on the HFOV (Fig. 2), the VMN was placed on the dry side of the heated humidifier with the adult T adapter as described in position 1. In position 4 (HFOV; proximal position), the VMN was placed between the circuit and the ETT using a 15/15-mm pediatric T adapter (Fig. 2). In the distal position on the HFOV (Fig. 2), the VMN was placed on the dry side of the heated humidifier using an adult T adapter placed directly on the inlet of the humidifier.
Medication delivery
The nebulizers were placed in each of the four respective positions, and the system heat and humidification was allowed to stabilize prior to testing at each condition. Iloprost (5 μg, 0.5 mL) was drawn up with a 1-mL filter needle syringe and mixed with 2.5 mL of normal saline for a total solution volume of 3 mL, placed in the nebulizer reservoir, and nebulized into the circuit. Three doses of iloprost were given in each of three nebulizers tested at each of the circuit positions (n = 9 measurements at each location, or n = 36 total). Special care was taken to position the filter superior to the ETT to avoid fluid condensate from accumulating in the tube and falling into the filter. Testing was completed when all of the solution was nebulized. The bacterial/viral electret filter at the end of the ETT was removed, labeled, and recorded in a laboratory notebook and placed in a refrigerator. In between each change in nebulizer position, drug and humidity fluid accumulation in the ETT was eliminated to reduce the likelihood of large drug molecules reaching the filter.
Iloprost measurement
Iloprost was recovered from the bacterial/viral electret filter following nebulization at each position and quantified using high-performance liquid chromatography (HPLC). Each filter was washed with 20 mL of methanol and thoroughly agitated under negative pressure, and the washing liquid was collected in 50-mL centrifuge tubes. The samples were dried with nitrogen gas flow. The residue was reconstituted by adding of 200 μL of methanol to each sample. The samples were analyzed by liquid chromatography electrospray ionization mass spectrometry (LC-ESI/MS) in positive mode. The LC-ESI/MS included an Agilent 1100 HPLC system coupled with a Sciex API 2000 tandem quadrupole mass spectrometer with an ESI turboionspray source (Applied Biosystems, Foster City, CA). The precolumn (C18, 2 μm) and analytical column (C18, 2.1 × 100 mm, 3 μm) were purchased from Alltech (Deerfield, IL). Analyst software (ver. 1.4.1; Applied Biosystems) was used to control the LC-ESI/MS system and conduct quantitative analysis. Five microliters of each sample was injected into LC-ESI/MS without split. The mobile phase was acetonitrile (0.1% trifluoroacetic acid)–water (0.1% trifluoroacetic acid), 85: 15 (vol/vol) injected at the flow rate of 200 μL/min. Column temperature was set at room temperature. The MS operation conditions were as follows: source temperature, 350°C; curtain gas, 20 psi; nebulizer gas, 25 psi; ion spray voltage, 4,200 V; declustering potential, 20 V; focusing potential, 200 V; and entrance potential, 10 V. MS was performed with a positive turboionspray ion source. The ion m/z 378.5 was monitored under selected ion monitoring mode. The areas under peak were used for quantitative analyses. A standard curve of iloprost was prepared in the range of 1.0 to 25.0 μg/mL. The linear regression coefficient was r 2 > 0.999. This quantitative method of iloprost drug recovery was validated by “spiking” clean filters using a known concentration and volume of drug and eluting drug from the filters with 100% ± 5% of the nominal dose of iloprost recovered from the filter using the aforementioned recovery method.
Statistical analysis
Iloprost concentrations were recorded in an Excel spreadsheet (Microsoft, Redmond, WA). All data were expressed as mass and reported as percentage (mean ± SD) of nominal dose placed in the nebulizer. Statistical analyses were performed using SPSS (ver. 20). One-way analysis of variance was used with a Tukey test for post hoc analysis to compare differences between the mean delivered iloprost mass at the four circuit position conditions. Statistical significance was set a priori at P < 0.05.
RESULTS
Iloprost-delivered mass to each filter (n = 9 filters at each location) was expressed in absolute terms and as a percentage of the 5-μg nominal dose (mean ± SD) at each position (Fig. 3). During conventional ventilation and HFOV, drug delivery was greater with the nebulizer placed in the proximal position than the distal position (P < 0.05). There was nearly a threefold greater increase in drug delivery during HFOV than during conventional ventilation at the proximal location (Fig. 3; P < 0.05). There was no difference in drug delivery between conventional ventilation and HFOV in the distal position. We observed no effect on ventilator function or lung model parameters with nebulization using either form of mechanical ventilation.
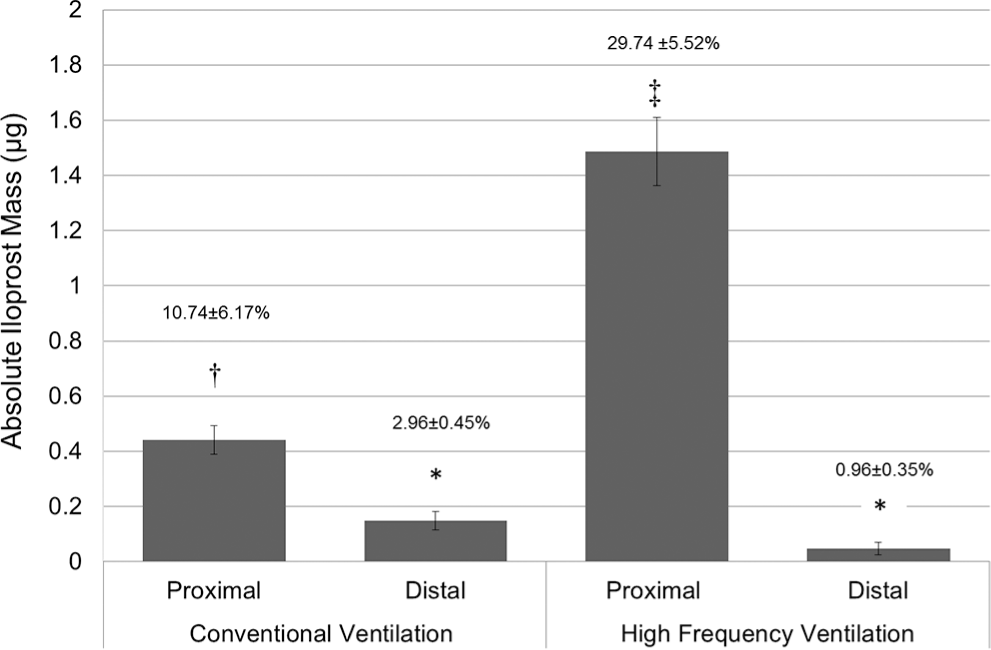
Delivered albuterol expressed as absolute mass and as percentage of nominal dose. With both devices, a proximal circuit position (closest to the patient) and a distal circuit position (dry side of the humidifier) were used for the testing process. All experiments were conducted using 5 μg of iloprost. Values are shown as mean ± SD and as the percentage of the nominal dose (5 μg of iloprost). Data not sharing common symbols are different from each other (P < 0.05).
DISCUSSION
This is the first in vitro study of infant ventilation reporting a double-digit percentage of the nominal dose of an aerosolized drug delivered distal to the ETT with both conventional ventilation and HFOV. Other studies have addressed medication delivery independently during conventional ventilation (Table 1) in adult and larger pediatric models, but this is the first to compare differences between two different forms of neonatal ventilation. Quantifying delivery of iloprost, an inhaled pulmonary vasodilator, to intubated infants is a key early step in establishing target lung doses to achieve reliable clinically effective doses across conventional ventilation and HFOV platforms.
Pediatric conventional ventilation aerosol studies
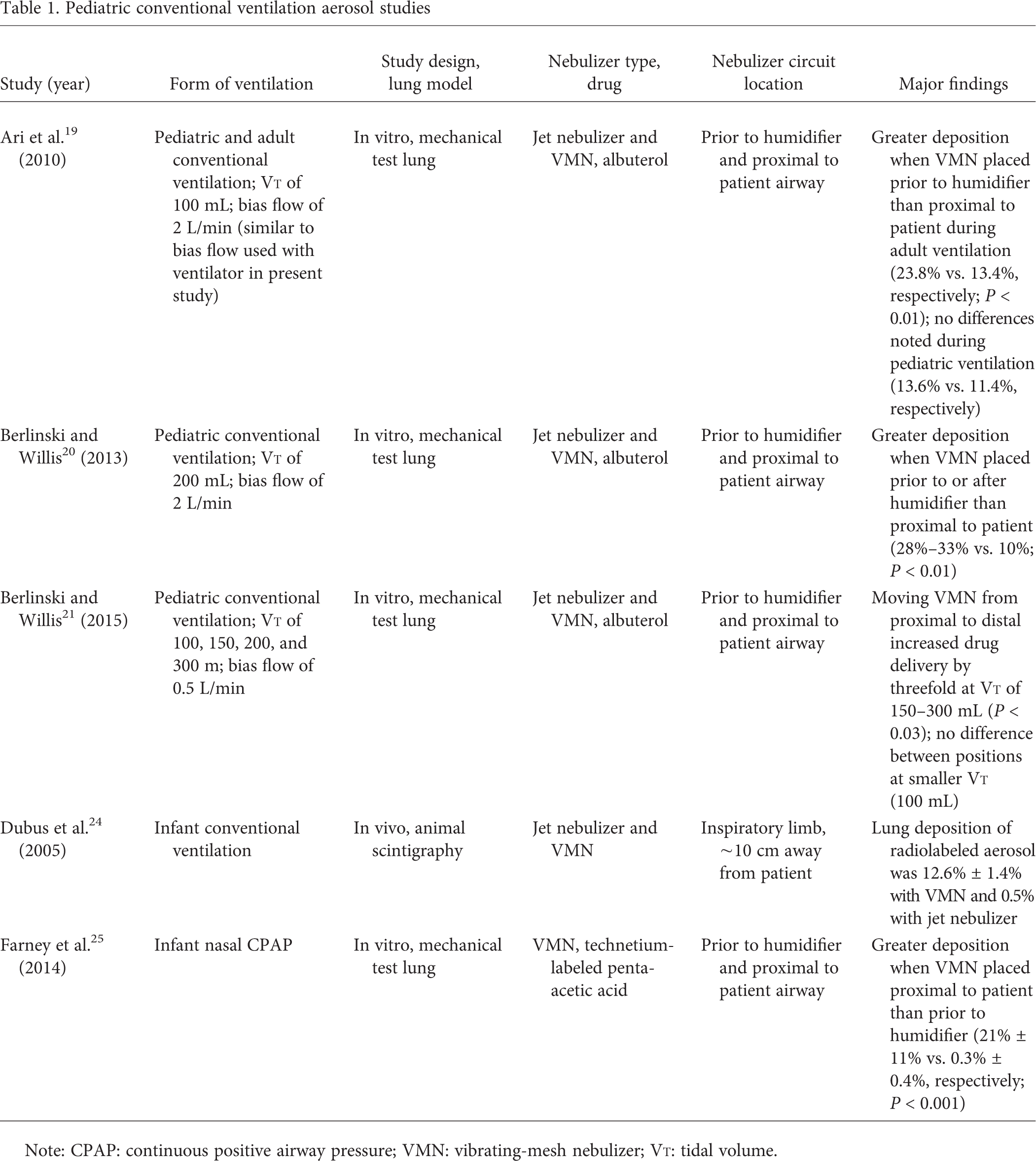
Note: CPAP: continuous positive airway pressure; VMN: vibrating-mesh nebulizer; Vt: tidal volume.
Our findings are similar to lung dose efficiency reported by Dubus et al. 24 in an infant animal model of conventional infant ventilation. The positional differences noted in the present study are also similar to findings of Farney et al., 25 who evaluated radiolabeled aerosol delivery with a VMN to an infant test lung during continuous positive airway pressure and found that placing the VMN proximal to the patient airway resulted in significantly greater drug delivery than when placed back at the humidifier.
Multiple investigators have described the impact of placement of a VMN in distal and proximal positions during simulated pediatric19–21 and adult 18 mechanical ventilation. In an adult model without bias flow, Ari et al. 18 reported twofold greater drug delivery with proximal versus distal position (prior to the humidifier). However, in a companion study using bias flow of 2 and 5 L/min, Ari et al. 19 reported a nearly threefold increase in medication delivery with the VMN in the distal position with bias flow of 2 L/min versus the proximal position during adult ventilation. The authors noted that, in the absence of bias flow, the aerosol bolus formed by the VMN remains in the vicinity of the nebulizer between ventilator breaths and that bias flow transports the aerosol through the inspiratory limb of the ventilator circuit, creating a reservoir charged with aerosol. The relationship between proximal and distal nebulizer positions and medication delivery was similar with adult and pediatric parameters, but the difference between positions was smaller with the pediatric circuit. 19
In a similar pediatric model, Berlinski and Willis,20,21 with bias flow of 2 L/min and Vt of 200 mL, reported greater delivery when the VMN was placed prior to or after the humidifier compared with proximal placement. With bias flow of 0.5 L/min, the authors reported more than twofold greater delivery with the nebulizer position placed before the humidifier than proximal to the patient with Vt of 150, 200, and 300 mL, but no positional difference was noted with the smaller Vt (100 mL). These studies suggest a relationship among drug delivery, circuit size, nebulizer position, bias flow, and Vt.
In contrast to findings in adult and pediatric models of conventional mechanical ventilation,18–21 we found greater drug delivery with proximal placement of the VMN during infant conditions. The difference in findings can be explained in part by the circuit, Vt, and breathing patterns used with different patient populations. In brief, an adult 22-mm ID ventilator circuit has an internal volume of 600 mL, compared with 180 mL for a 10-mm ID infant circuit and 80 mL in the humidifier chamber. A bias flow of 2 L/min provides 33 mL/s gas moving through the ventilator circuit during the expiratory phase. For the adult with Vt of 500 mL and 3 seconds between breaths, aerosol emitted prior to the humidifier travels 99 mL into the inspiratory limb, so most gas entering the airway is rich in aerosol at the onset of a breath. Assuming Vt of 20 mL and 1 second between inspirations during infant conventional ventilation, gas moves the aerosol bolus 53.3 mL with each breath when placed prior to the humidifier, requiring more than four breaths and 3.3 seconds for aerosol to travel from the VMN to the patient airway. During that time, the transition from baseline to peak inspiratory flow creates turbulence, resulting in impactive losses of aerosol in the circuit, while the 3.3 seconds allows aerosol to settle out of suspension due to gravitational sedimentation, further reducing the amount of aerosol delivered. In contrast, positioning the nebulizer in the inspiratory limb proximal to the airway requires fewer breaths and less time to provide drug from nebulizer to patient, allowing a greater proportion of the aerosol bolus to be delivered to the airway.
Future studies are needed to better understand the interaction among volume, inspiratory time/rate setting combinations, circuit size, and bias flow that results in differences in medication delivery between the different nebulizer locations during conventional ventilation.
Early reports suggested negligible aerosol delivery with HFOV compared with conventional ventilation. As such, we were surprised to see the high level of drug delivered with HFOV (29.74%) with placement of the VMN at the airway during HFOV. Very few studies have evaluated aerosol delivery during HFOV. Using a pressurized metered-dose inhaler with the holding chamber placed at the airway, Garner et al. 22 reported negligible delivery of albuterol to a filter placed distal to the ETT. In contrast, Alzahrani et al. 26 demonstrated that albuterol delivery during HFOV was significantly greater than that during conventional ventilation using an adult cast model.
Using a low-flow jet nebulizer with aerosolized prostaglanding E1 placed in the inspiratory limb of a of neonatal ventilator circuit, Sood et al. 27 reported drug delivery efficiency of 32%–40% of the nominal dose during conventional ventilation and only 0.1% during HFOV. A potential issue with their model is that they collected drug as condensate at the end of the ETT deposited in a closed bottle. In contrast, we collected aerosol on a filter placed in a superior position to the ETT to prevent condensate from reaching the filter, limiting our collection to aerosol. Our findings using the VMN placed at the airway delivered only one-third of the drug reported by Sood and colleagues with conventional ventilation and nearly threefold greater drug delivery with HFOV than with conventional ventilation. The position for nebulizer placement within the HFOV circuit is unclear, but based on the low deposition (0.1%) they observed and the fact that HFOV settings were similar to those of our study, it is likely that the nebulizer was placed back prior to the humidifier.
In a separate study, Sood et al. 28 compared aerosol delivery using a low-flow jet nebulizer (MiniHEART; Westmed, Tucson, AR) between conventional mechanical ventilation, HFOV, and high-frequency jet ventilation in an infant test lung model with a 3.5-mm ID ETT. In this model, the distal tip of the ETT was placed in a sponge that was open to atmosphere. They reported greater deposition with conventional ventilation than with high-frequency jet ventilation and HFOV. Their model was not designed to differentiate aerosol delivery drug containing condensate dripping into the sponge but shows the reduction of drug delivered distal to the ETT with a low-flow jet nebulizer during HFOV versus conventional ventilation.
We believe that placing the nebulizer proximal to the patient during HFOV (between the ETT and the patient circuit) may have resulted in improved drug delivery because the aerosol bolus was largely isolated from the bias flow, reducing the amount of drug driven by the bias flow directly into the expiratory limb of the ventilator. During HFOV, placement of the aerosol generator at the humidifier allows mixing and dilution of the aerosol with the high continuous flow of 15–25 L/min. This dilutes the aerosol into a volume of gas that is much greater than the minute ventilation of the infant, ensuring that only a small percentage of the aerosol will be inhaled. Our findings confirm that placement of the VMN at the humidifier during HFOV is ineffective for aerosol delivery with the Sensormedics 3100A. Negligible drug delivery in the distal position during HFOV may also be related to inertial impaction within the circuit resulting from relatively high resistive properties created by short inspiratory times and high flows during HFOV.
Placement of the nebulizer at the airway adds several milliliters of mechanical dead space, which could result in hypercarbia during conventional ventilation, but it less likely to be a problem with HFOV as long as the nebulizer/adapter remains in the circuit. Future clinical studies should evaluate the impact of placement between the circuit and the ETT in terms of CO2 rebreathing.
To date, no aerosol drug for inhalation has ever been approved for administration to infants, no less mechanically ventilated, intubated infants (or adults). The motivation for this study was to understand the implications of dosing with different device configurations and placement, not to promote administration of a specific drug. The dosage used in this study was selected on the basis of the current label (for adults) and to provide sufficient deposited dose of drug to reliably detect with available analytical methods. Clinically relevant doses should be based on future clinical studies with this and other drugs, and such studies are essential before any clinical endorsement should be made.
These findings emphasize the need to study a broader range of specific ventilator support systems used with infants to better understand how they impact the efficiency of aerosol delivery with a broad range of medications. Future investigations will be needed to better understand why drug delivery appears to be more efficient during HFOV than during conventional ventilation. The complex gas flow mechanisms that govern HFOV may be a likely explanation, but the combination of much shorter inspiratory times, higher frequencies, and active exhalation may make it less likely for drug to be delivered to the expiratory limb, resulting in greater delivery to the lungs than during conventional ventilation.
Limitations
In this in vitro study, we took careful measures to simulate a realistic infant clinical environment by using a heated, actively breathing test lung configured with mechanics values similar to those measured in infants requiring ventilatory support. As with most aerosol studies in vitro, the results of this study must be approached with some caution. The amount of drug delivered to the filter represents the total mass of available drug delivered distal to the artificial airway, but it does not take into account the amount of aerosol that would normally be exhaled or the distribution of drug particles that might be delivered to the peripheral airways of the lungs, where they are needed most. In addition, our model used a secure, no-leak connection between the distal tip of the ETT and the filter, likely overestimating delivery under all conditions. However, unlike inhaled bronchodilators, whether delivering iloprost to the peripheral airways is necessary for clinical effect is still unknown. Thus, it is extremely important to mention that, despite making every attempt to avoid large droplets of accumulated liquid medication (combined with humidity) from reaching the filter, it is still possible that this fluid can condense anywhere in the airway model and be delivered to the filter media during inhalation. While we noted some fluid accumulation in the ETT, we positioned the tube to keep that fluid from draining into the collection filter. Thus is it unlikely, on the basis of the variability of iloprost mass (SD), that large droplets were introduced into the filter.
Additional limitations include using only one particular brand of critical care conventional and high-frequency ventilator, humidifier, and circuit. We did not do sufficient testing to determine the impact of iloprost on ventilator performance over an extended period of time, but in general we recommend that filters be placed in the expiratory limb of the ventilator circuit to avoid downstream contamination of this or any nebulized drug. We also used one lung model configuration and a single combination of conventional ventilation and HFOV settings on the ventilators, on the basis of our clinical practice for this size of infant. Finally, we only tested one particular type and model of nebulizer, and we did not compare the VMN to the jet nebulizer. Improvements in device technologies and additional research are needed to determine whether changing these variables has any effect on aerosol delivery during simulated infant mechanical ventilation. Additional clinical studies are required to determine whether these varying levels of delivered dose make a difference in both therapeutic and adverse responses to iloprost.
Conclusion
Given these findings, it would seem that clinicians should avoid placing the nebulizer back between the ventilator and humidifier during neonatal ventilation. If these bench data can translate into clinical practice, then the VMN may represent a novel approach for providing more efficient drug delivery to infants receiving respiratory support via conventional ventilation or HFOV.
