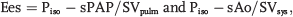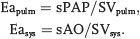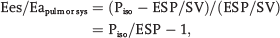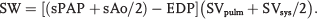Abstract
We describe a 63-year-old patient with unrepaired tricuspid valve atresia and a hypoplastic right ventricle (single-ventricle physiology) who presented with progressive symptomatic hypoxia. Her anatomy resulted in parallel pulmonary and systemic circulations, pulmonary arterial hypertension, and uncoupling of the ventricle/pulmonary artery. Hemodynamic and coupling data were obtained before and after pulmonary vasoactive treatment, first inhaled nitric oxide and later inhaled treprostinil. The coupling ratio (ratio of ventricular to vascular elastance) shunt fractions and dead space ventilation were calculated before and after treatment. Treatment resulted in improvement of the coupling ratio between the ventricle and the vasculature with optimization of stroke work, equalization of pulmonary and systolic flows, a decrease in dead space ventilation from 75% to 55%, and a significant increase in 6-minute walk distance and improved hypoxia. Inhaled treprostinil significantly increased 6-minute walk distance and improved hypoxia. This is the first report to show that pulmonary vasoactive treatment can be used in a patient with unrepaired single-ventricle anatomy and describes the hemodynamic effects of inhaled therapy on ventriculovascular coupling and gas exchange in the pulmonary circulation in this unique physiology.
Keywords
Pulmonary arterial hypertension (PAH) is a progressive disease defined by severe pulmonary vasculopathy resulting in high right ventricular (RV) afterload. Although treatment focus is often on the pulmonary vasculopathy, mortality in this disease is most specifically indicated by RV load adaptation. 1 Therefore, there has been recent research emphasis on methods directed toward recognition of early pump dysfunction. One such method is ventriculovascular coupling, a method that describes the hydraulic transfer of energy from the ventricle to the vasculature. 2 This method is not generally thought of in the context of the “coupling” of gas exchange. Functional improvements with therapy are attributed to a combination of improvements in gas exchange and RV function. However, the extent to which each component contributes is unknown.
Ventriculovascular coupling is most often described by the coupling ratio, the numeric ratio of ventricular elastance (Ees) to vascular elastance (Ea). Ees is often termed contractility and thought of as a component that is independent of acute changes in preload and afterload, or Ea. The RV increases contractility as an adaptation to sustained increases in afterload. 3 The degree of adaptation of the ventriculovascular unit is typically indicated by the coupling ratio, Ees/Ea. While stroke work is optimized at a coupling ratio of 1.0, 4 studies of experimental PAH indicate that the system is coupled under normal conditions to maximum work for minimum energy cost (efficiency) at a coupling ratio of approximately 1.5–2.0. 5
Pulmonary gas exchange in vascular disease can be characterized by increased inequality of ventilation-perfusion (
We present an adult patient with complex, unrepaired congenital heart disease with single-ventricle physiology. This represents a unique clinical situation where a single pump, a morphologic left ventricle (LV), distributes stroke volume to both the pulmonary and the systemic circulation, and the volume distribution is determined by afterload in parallel. In this situation, symptoms may result primarily from gas exchange imbalance, early ventriculovascular uncoupling indicating pump dysfunction, or both. Therefore, this is a unique scenario by which we can study the effects of coupling integrated with gas exchange under changing conditions as well as how this interaction affects functional parameters.
CASE DESCRIPTION
A 63-year-old woman was referred for evaluation of treatment for her pulmonary hypertension and possible embolization of aortopulmonary collateral arteries after suffering recurrent hemoptysis. She was diagnosed as a child with tricuspid valve atresia, a hypoplastic RV, transposition of the great arteries (aorta arising from the hypoplastic RV and pulmonary artery arising from the LV), a ventricular septal defect, and an atrial septal defect (Fig. 1). She had significant hypoxemia for years, was receiving chronic oxygen supplementation, and had subjectively worsening dyspnea. She underwent diagnostic cardiac catheterization with general anaesthesia. A 5F balloon-tipped wedge catheter was advanced through the venous system to the right atrium, across the atrial septal defect, and into the LV. The catheter was then advanced to the pulmonary artery for hemodynamic measurements.
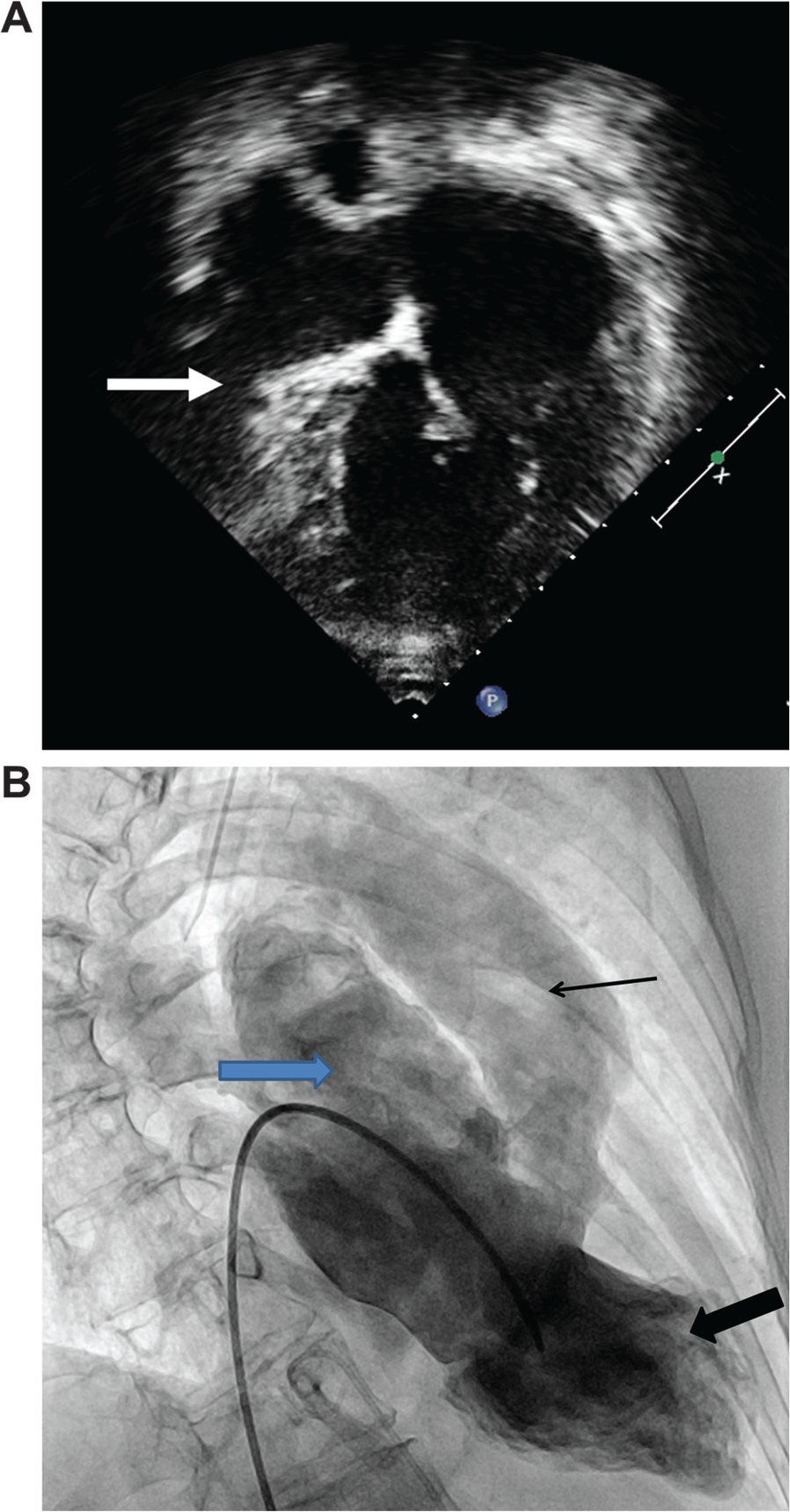
Cardiac anatomy of the patient. A, Two-dimensional echocardiographic apical four-chamber view showing an atretic tricuspid valve (arrow), severely hypoplastic right ventricle, large secundum atrial septal defect, and normal-sized left atrium and ventricle. B, Ventriculography with an angiographic catheter advanced antegrade up the inferior vena cava, across the atrial septal defect, and into the apex of the ventricle (thick black arrow). The great arteries are transposed, and the morphologic left ventricle gives rise to a calcified main pulmonary artery (blue arrow) and, through a nonpressure restrictive ventricular septal defect, to the aorta (thin black arrow).
Ventricular (Ees), pulmonary arterial (Eapulm), and systemic arterial (Easys) systolic elastances were calculated using the single-beat method, as described elsewhere.
3
This method utilizes Piso, the isovolemic pressure of a nonejecting beat, determined by sine extrapolation of the RV waveform near maxima dP/dt and minima dP/dt (Fig. 2). For clarification, contractility,
Pressure-volume relationship of the single ventricle relative to pulmonary and systemic elastance before and after inhaled nitric oxide (iNO) therapy. Maximal isovolemic pressure (Piso) is denoted by asterisks. Shown are pulmonary effects of reduced afterload (Ea), reduced systolic pulmonary arterial pressure, and improved pulmonary flow. Systemic coupling demonstrates a concurrent increase in afterload during therapy with only a slight change in flow. Thus, treatment aided in restoring balance to the system, reducing overall afterload and improving stroke work. Ees: ventricular elastance.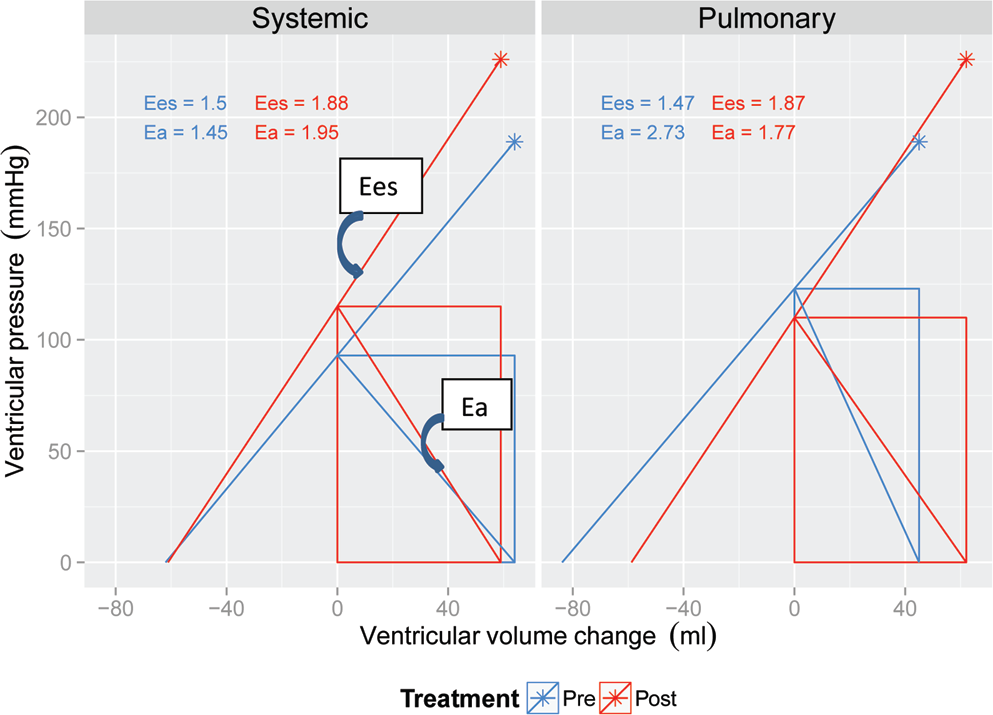
The patient was studied with baseline measurements at 35% FiO2 and repeat measurements under 100% FiO2 and 100% FiO2 and 20 ppm of inhaled nitric oxide (iNO). Metabolic cart analysis was used for direct measurement of oxygen consumption and calculation of dead space. Since there was no outflow pressure restriction, combined afterload in parallel of the ventricle represents the harmonic mean of pulmonary and systemic vascular impedance. Therefore, stroke work, the area bounded by the pressure-volume loop, was taken as the numeric mean of both systolic pressure and SV, giving the equation
After hemodynamics were obtained, the interventional cardiologist (MS) proceeded with embolization of the aortopulmonary collateral arteries that were causing hemoptysis. After discharge, the patient underwent 6-minute walk distance (6MWD) testing before and after inhaled treprostinil. Inhaled treprostinil was titrated to effect, including tolerance, dyspnea relief, oxygenation, and walk distance. Echocardiography, both before and after treatment, demonstrated normal ventricular systolic function (ejection fraction of >60%). She has not had recurrence of hemoptysis.
Hemodynamics and gas exchange
Results during catheterization showed elevated pulmonary pressure, resistance, and elastance. Pulmonary arterial and aortic pressure tracings are shown in Figure 3. The pulmonary arterial waveform showed a hybrid contour (rounded peak similar to an aortic tracing) but a rapid descent to a lower diastolic pressure and a dicrotic notch. Baseline hemodynamics demonstrated a right-to-left shunt (Table 1). Dead space measured 75% at baseline. Measurements were unchanged with 100% FiO2. During iNO inhalation, pulmonary pressure, resistance, and elastance all decreased. The shunt equalized, and there was a small improvement in dead space (Table 1).
Hemodynamic and gas exchange data
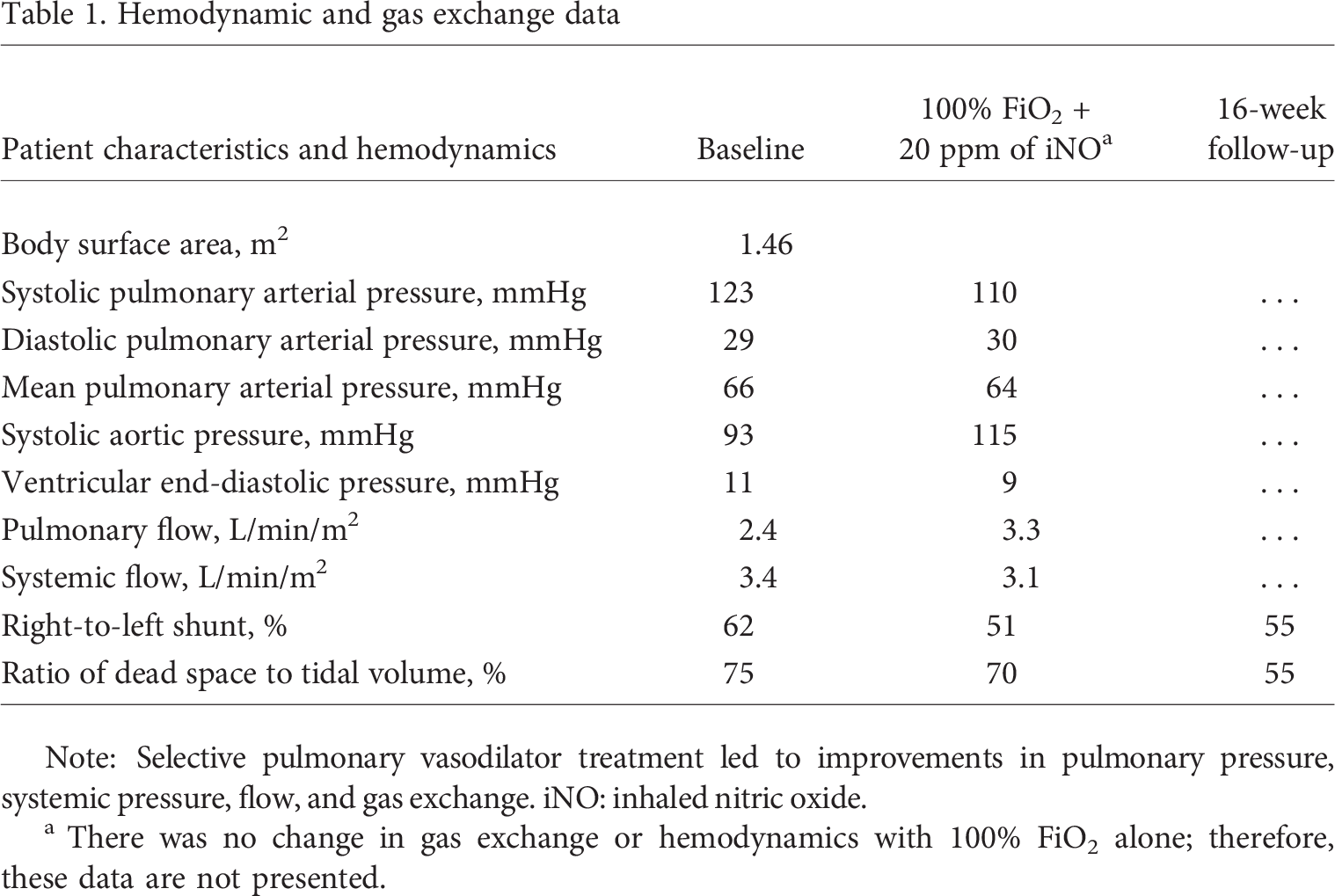
Note: Selective pulmonary vasodilator treatment led to improvements in pulmonary pressure, systemic pressure, flow, and gas exchange. iNO: inhaled nitric oxide.
There was no change in gas exchange or hemodynamics with 100% FiO2 alone; therefore, these data are not presented.
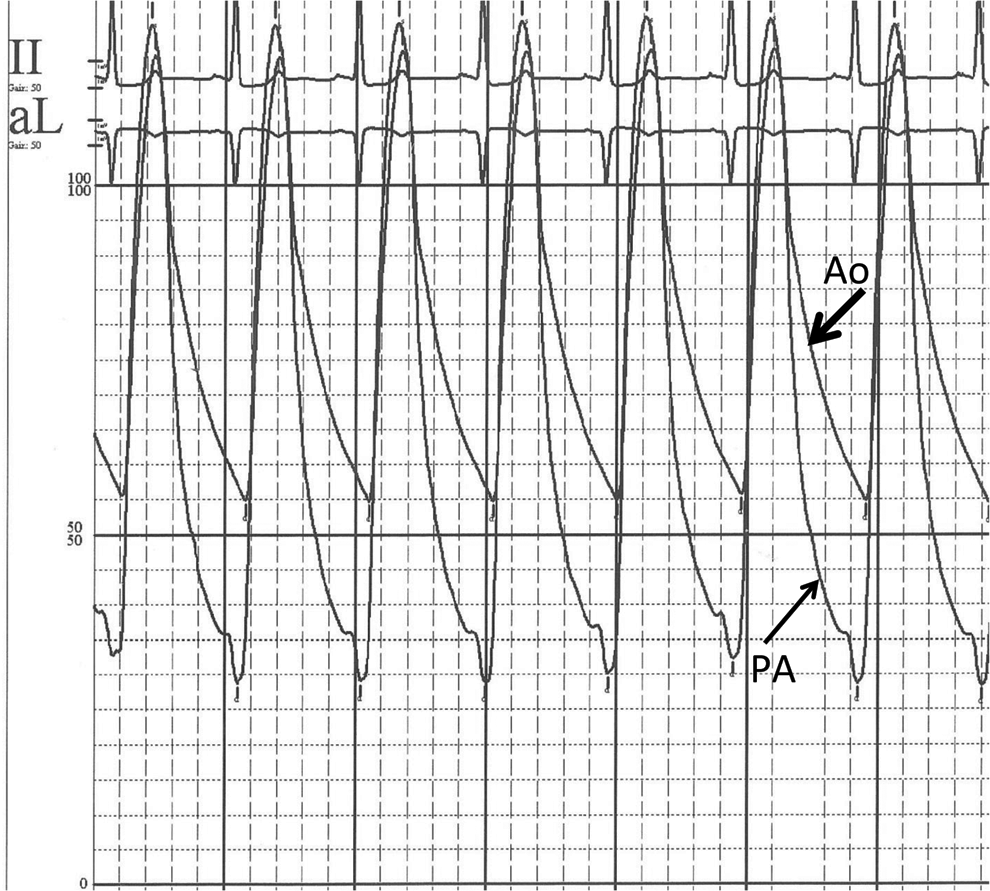
Pulmonary arterial and aortic pressure tracings. The pulmonary arterial waveform (PA; thin arrow) has taken a rounded peak and rapid taper similar to the aortic waveform (Ao; thick arrow), indicating increased pulse-wave reflection and reduced compliance. However, delay in dicrotic notching and reduced diastolic pressure indicate retention of some of the normal pulmonary arterial phenotype.
Ventriculovascular coupling
Baseline pulmonary afterload was very high and decreased considerably during iNO therapy (Table 2). Although contractility was high, the pulmonary ventriculovascular interaction was uncoupled at baseline (0.54). As illustrated in Figure 2, the pulmonary ventriculovascular coupling ratio improved during iNO therapy (1.06), while systemic ventriculovascular coupling was unchanged. This led to improvements in pulmonary stroke volume index, from a baseline of 31 to 43 mL/m2 during iNO therapy.
Coupling and afterload data
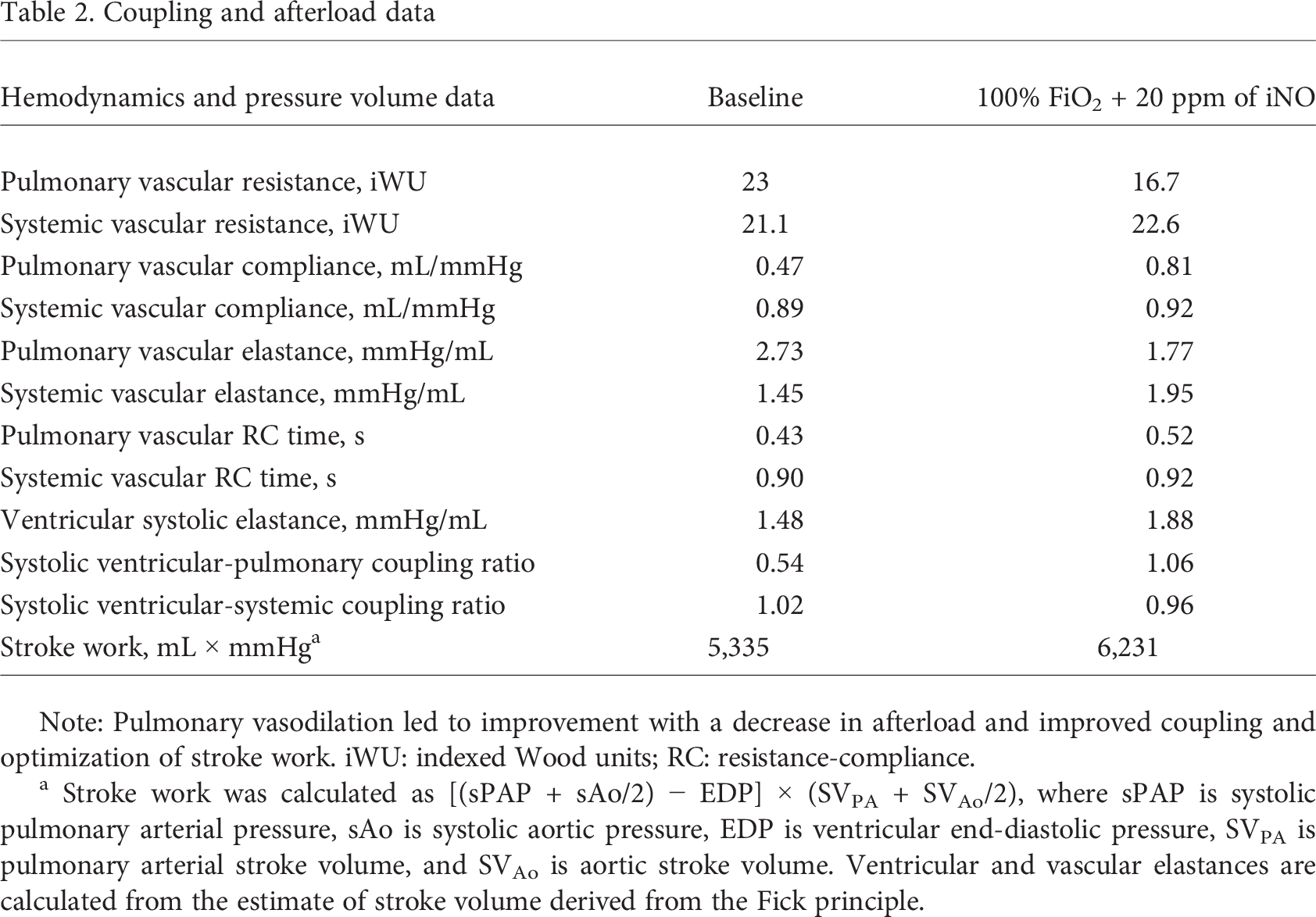
Note: Pulmonary vasodilation led to improvement with a decrease in afterload and improved coupling and optimization of stroke work. iWU: indexed Wood units; RC: resistance-compliance.
Stroke work was calculated as [(sPAP + sAo/2) – EDP] × (SVPA + SVAo/2), where sPAP is systolic pulmonary arterial pressure, sAo is systolic aortic pressure, EDP is ventricular end-diastolic pressure, SVPA is pulmonary arterial stroke volume, and SVAo is aortic stroke volume. Ventricular and vascular elastances are calculated from the estimate of stroke volume derived from the Fick principle.
Long-term therapy and functional improvement
Given the physiological improvements, we attempted to treat the patient similarly in the ambulatory setting. The patient was titrated on inhaled treprostinil to five inhalations four times daily. She had sustained functional improvement measured during submaximal exercise, with a 6MWD increase of more than 100 m (Table 3). She also had sustained benefits in resting right-to-left shunt and large reductions (20%) in dead space relative to baseline (Table 1).
Functional improvement in 6-minute walk distance (6MWD) before and after treatment with inhaled treprostinil
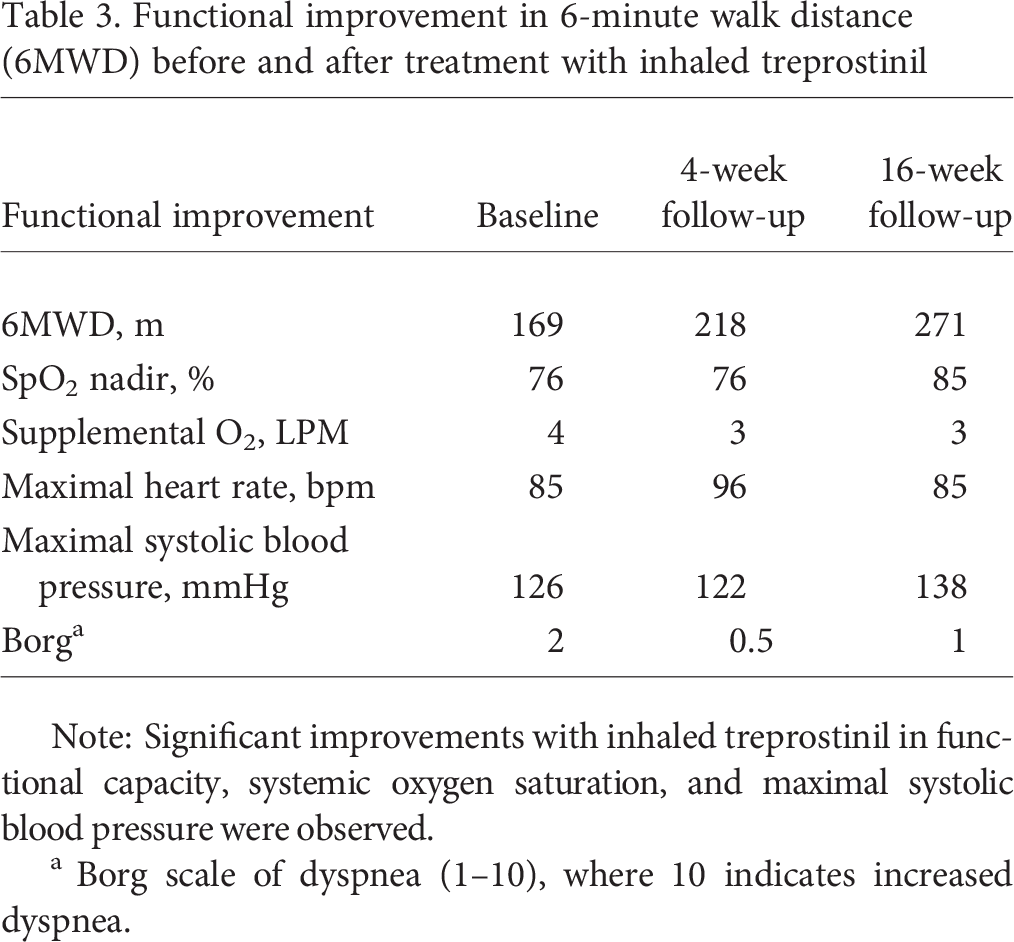
Note: Significant improvements with inhaled treprostinil in functional capacity, systemic oxygen saturation, and maximal systolic blood pressure were observed.
Borg scale of dyspnea (1–10), where 10 indicates increased dyspnea.
DISCUSSION
The results of the present case suggest that selective pulmonary vasodilator treatment aids in the coupling of the ventriculovascular unit for gas exchange and optimization of stroke work. Although animal models of single-ventricle physiology demonstrate similar findings, 8 these findings are unique in that they are the first to show combined physiological and functional benefit in a patient.
Tricuspid valve atresia without outflow obstruction allows a single ventricle to distribute stroke volume to the pulmonary and systemic circulations. Proper balance between pulmonary and systemic afterload ensures adequate gas exchange while maintaining a normal systemic perfusion, but such a balance is difficult to attain. Additionally, combined mean harmonic afterload may substantially increase ventricular work as pulmonary vasculopathy progresses, leading to eventual pump failure.
Decrease in pulmonary vascular afterload results in improved gas exchange and distribution of pulmonary blood flow
Although baseline pulmonary afterload was quite high, the pulmonary arterial pressure waveform morphology demonstrated retained phenotypic characteristics of the normal pulmonary circulation, and RC time remained approximately half that of the systemic circulation. In addition, the patient's intrapulmonary ventilation perfusion matching was likely near normal, as evidenced by the lack of effect of 100% FiO2 on the degree of right-to-left shunting. These two characteristics helped maintain a balance of volume distribution and gas exchange until the gradual onset of pulmonary vasculopathy.
In this context, iNO and treprostinil likely lead to restoration of the optimal balance in gas exchange coupling. Initial improvements in pulmonary blood flow resulted from acute changes in vasoreactivity or distribution to relatively normal
Pulmonary vasodilatation results in improvement in ventricular dysfunction and optimization of stroke work
The patient presented with no signs or symptoms of ventricular failure, and echocardiography demonstrated normal ejection fraction. However, at baseline the ventriculovascular unit had likely reached maximum contractile reserve. The ventricle was uncoupled from the pulmonary circuit in the presence of systemic hypotension. Pulmonary vasoactive treatment led to a balance of coupling, optimization of stroke work, and equalization of flow. These relationships are likely maintained during treatment with inhaled treprostinil. Given maintained systemic blood pressure, shunt fraction, and oxygenation, both coupling and gas exchange were maintained amazingly under dynamic conditions, and significant functional improvement resulted.
Although there was a drop in pulmonary vascular afterload during iNO therapy, the overall load of the ventricle remained relatively unchanged (composite Ea before iNO, 2.09 mmHg/mL; composite Ea after iNO, 1.9 mmHg/mL). This is explained by a compensatory increase in systemic perfusion to a new equilibrium at the optimization of stroke work (coupling ratio, 1.0). This equilibrium was aided by an increase in overall Ees. In experimental models, iNO had variable effects on the myocardium; however, the preponderance of scientific data indicate that its principal effects are on the vasculature.9–11 This suggests that the increase in systolic elastance may have resulted from enhanced coronary perfusion pressure.
Although the coupling data in this case were acquired in the acute setting, the same physiology was likely simulated chronically with inhaled treprostinil. Dead space and shunt were preserved and/or improved during treprostinil therapy, indicating probable vascular remodeling and preserved Ees/Ea. In addition, exercise oxygenation, systemic pressure, and functional status improved during therapy, furthering this concept.
Ultimately, the clinical relevance of this case may perhaps be limited to a select population. This patient suffered from a very rare condition in which nearly all the shunt was intracardiac and therefore improved significantly with pulmonary vasodilation therapy alone. The results cannot be generalized to patients with mixed or predominantly intrapulmonary shunts. Furthermore, the effects of selective pulmonary vasodilation on shunting in patients with normal atrial-ventricular-vascular concordance may not be as impressive.
In summary, treatment-associated improvements in gas exchange in this patient were associated with improvements in ventriculovascular coupling. This phenomenon may indicate a new link between gas exchange and hydraulic work optimization. Additionally, this case highlights a novel use of inhaled treprostinil to establish optimal gas exchange and functional status.