Abstract
Pulmonary hypertensive crisis is an important cause of morbidity and mortality in patients with pulmonary arterial hypertension secondary to congenital heart disease (PAH-CHD) who require cardiac surgery. At present, prevention and management of perioperative pulmonary hypertensive crisis is aimed at optimizing cardiopulmonary interactions by targeting prostacyclin, endothelin, and nitric oxide signaling pathways within the pulmonary circulation with various pharmacological agents. This review is aimed at familiarizing the practitioner with the current pharmacological treatment for dealing with perioperative pulmonary hypertensive crisis in PAH-CHD patients. Given the life-threatening complications associated with pulmonary hypertensive crisis, proper perioperative planning can help anticipate cardiopulmonary complications and optimize surgical outcomes in this patient population.
Keywords
INTRODUCTION
The current 2008 Dana Point clinical classification of pulmonary arterial hypertension (PAH) recognizes congenital heart disease (CHD) associated with systemic-to-pulmonary shunts as an important cause of PAH in both children and adults.1,2 In adult patients, PAH is diagnosed as a resting mean pulmonary arterial pressure (mPAP) greater than 25 mmHg with a pulmonary vascular resistance (PVR) greater than 3 Wood units and a pulmonary capillary wedge pressure of 15 mmHg or less. 2 In pediatric patients (especially those younger than 24 months), where transthoracic echocardiography is often used instead of cardiac catheterization, PAH-CHD is diagnosed when the ratio of systolic pulmonary arterial pressure (PAP) to systolic systemic arterial pressure is greater than 0.5. 3 While early surgical repair can prevent the development of PAH in CHD, PAH has become one of the leading but unresolved medical conditions that, like primary myocardial failure, significantly increases mortality in cardiac surgery. 4 The increased perioperative mortality is largely due to the high incidence of perioperative pulmonary hypertensive crisis (PH crisis), a clinical entity that develops when the mPAP acutely exceeds mean systemic arterial pressure (mSAP). Because of the current lack of firm diagnostic criteria, the incidence of perioperative PH crisis has been estimated to range between 2% and 5% and appears to be higher in patients who require cardiopulmonary bypass (CPB).5,6 The most likely causative mechanism is abrupt pulmonary vasoconstriction, causing right heart failure and systemic hypotension, which can result in death from severe tissue hypoxia. The systemic inflammatory response syndrome, endothelial cell injury, inhibition of nitric oxide (NO) production, and increases in endothelin levels all play roles in the genesis of PH crisis.6–8
Fundamental management of PH crisis after cardiac surgery includes two aspects: (1) appropriate assessment and treatment of right ventricular failure and (2) acute interventions to compensate for extreme acidosis and tissue hypoxia. 6 PH crisis often requires an aggressive combination of therapies for right ventricular failure, and we should carefully manage inotropes and vasopressors (e.g., dobutamine, norepinephrine), prudent fluid balance, and maintenance of sinus rhythm and atrioventricular synchrony.9–12 In fact, the challenge is to find the optimal preload to avoid the detrimental effects of ventricular inter-dependence. 9
The general treatment of acidosis and hypoxia includes oxygenation, alkalinization, hypocapnia, and muscle relaxation. For instance, hypoxic pulmonary vasoconstriction may contribute to pulmonary hypertension after cardiac surgery. 13 Thus, supplemental oxygen should not be overlooked as a key component of PH crisis therapy in the intensive care unit (ICU). 9 Furthermore, adequate respiratory support with gentle tracheal suction and cautious use of analgesics should be brought into the standardized management.14,15 However, hypovolemia and hypervolemia both can lead to suboptimal preload and decreased cardiac output. 9 Current clinical studies support the efficacy of gentle ventilation (smaller tidal volumes, limited inspiratory plateau pressure), instead of moderate hyperventilation, for the management of perioperative PAH in pediatric patients. 16 On the other hand, care should be taken to avoid permissive hypercapnia and ensuing acidosis, which may have untoward hemodynamic effects, even causing increased PVR and mPAP.17–19
In recent years, once hemodynamic deterioration and hypoxia are not improved by general therapies mentioned above, some PAH-specific vasodilators are usually considered. The introduction of these agents, such as prostacyclin analogs, endothelin receptor antagonists (ERAs), and phosphodiesterase-5 (PDE-5) inhibitors, has led to a significant increase in the life expectancy of PAH-CHD patients undergoing reparative or palliative surgery for congenital cardiac lesions. However, even with advances in cardiac surgery and expanding PAH-specific therapy, the mortality of PAH-CHD patients with PH crisis still remains unacceptably high, ranging between 22.2% and 54.5%. 5 Moreover, consensus on the optimal strategies with which to manage this devastating clinical entity does not exist. 5
The aims of this review are to discuss recent advances in pharmacological therapies for perioperative PH crisis and to review the literature that supports their efficacy. We also provide an algorithm for clinical management of PH crisis based on the strength of available data, to help physicians who may encounter this clinical entity in their medical practice. We caution that there are no established guidelines and no well-designed trials to demonstrate the utility of these drugs as the standard of care in patients with PH crisis in surgery. Most studies have been done in nonsurgical settings, and the applicability of some of these drugs (i.e., ERAs, PDE-5 inhibitors) in surgical patients is speculative. However, we believe that discussion of these agents is reasonable and should lead to future studies that would determine whether any one or a specific combination of them would lead to improved outcomes in these patients.
INHALED NO
Inhaled NO (iNO) works by activating cyclic guanosine monophosphate (cGMP)–dependent signaling pathways in pulmonary vascular smooth muscle cells, resulting in selective pulmonary vasodilation. 20 Several clinical studies have suggested a role for iNO in the treatment and prevention of PH crisis in PAH-CHD patients after cardiac repair. In a placebo-controlled study, Miller et al. 21 found that infants with PAH-CHD receiving iNO had fewer PH crises and shorter postoperative courses without concomitant side effects related to the medication. On the basis of their experience, they recommended that iNO at a dose of 10 ppm could be used in infants at high risk to prevent the development of PH crisis. In a similar fashion, Journois and colleagues 22 showed that the use of iNO is associated with lower postoperative mortality in children with PAH-CHD who underwent complete repair of atrioventricular canal defects, by reducing the rate of PH crisis preoperatively.
Although the exact effect of prophylactic iNO on the mortality of PAH-CHD patients has been a matter of debate,23,24 iNO has been the standard therapy for the postoperative control of PAH and the prevention of PH crisis, as recommended by European guidelines from 2004.25,26 However, the dosage and duration of iNO administration vary among institutions. Generally, iNO should be considered first-line therapy for perioperative refractory PAH. If iNO is not effective, the use of extracorporeal membrane oxygenation (ECMO) should be considered. 27 The iNO treatment is usually initiated at doses of 5–20 ppm, and the dosage may be increased to a maximum of 80 ppm within minutes. However, therapeutic levels of iNO below 0.8 ppm have been reported to demonstrate pulmonary vasodilatory effects, 20 and it is important to administer the lowest effective dose, to minimize toxicity. 28 The duration of administration is typically days to weeks and should exceed 72 hours in patients with PVR exceeding 6 Wood units. 27 The utility of iNO can be enhanced by precise patient selection, supplemental agents (such as sildenafil), and gradual withdrawal to avoid the possibility of rebound pulmonary hypertension.29,30
Although iNO is recommended for the treatment of postoperative pulmonary hypertension, its use may not be feasible in all medical centers. Inherent limitations to its use include the significant cost, the complex delivery system required, and the typical delay in administration when an acute crisis appears. Two other potential risks include methemoglobinemia and fatal rebound pulmonary hypertension after discontinuation, which is especially common after rapid weaning. 31 Therefore, there is ongoing interest in comparing newer pulmonary-specific vasodilators with standard iNO therapy in the management of PAH with congenital heart surgery, as discussed below.32–34
PROSTACYCLIN ANALOGS
The clinical use of prostacyclin and its analogs for the management of PAH-CHD was reported as early as 1980.35,36 Long-term prostacyclin therapy has been shown to improve quality of life and hemodynamic parameters in PAH-CHD patients when conventional therapy failed. 37 Since then, prostanoids have been used to treat patients with moderate to severe PAH-CHD. At present, there are 4 commercially available prostanoids: alprostadil, epoprostenol, treprostinil, and iloprost.
Alprostadil
Intravenous (IV) alprostadil (prostaglandin E1 [PGE1]) is often used as the first-line drug for maintaining and/or reopening the ductus arteriosus in neonates with ductusdependent cardiac malformations until surgical correction can be performed. 38 Alprostadil, in conjunction with balloon atrial septostomy and iNO therapy, has been applied as a standard initial combined treatment for persistent PAH complicated with transposition of the great arteries and an intact ventricular septum (TGA/IVS). 39 Moreover, IV alprostadil is associated with a reduction in mPAP and a lower risk of death in postoperative PAH-CHD.40,41 However, the lack of pulmonary specificity of IV alprostadil and the short half-life (5–10 min) of aerosolized alprostadil limit its widespread use as a therapy for perioperative PAH in cardiac surgery. 42 Recently, the development of novel nebulized nanoparticle carriers, such as liposomes, poly(lactic-co-glycolic) acid (PLGA), and polyethyleneimine (PEI), has renewed interest for inhaled alprostadil as a possible alternative to treat PAH-CHD populations in a perioperative setting.43,44
Epoprostenol
The most important advance in the management of patients with PAH was the introduction of epoprostenol (PGI2, Flolan, prostacyclin) in the 1990s. Long-term IV epoprostenol therapy leads to an improvement in hemodynamic measures, exercise capacity, and quality of life in PAH-CHD patients. 45 The effects of epoprostenol in PAH-CHD are comparable to those in patients with idiopathic PAH (IPAH), for both corrected and uncorrected defects.37,45,46
While its benefit in the perioperative setting is less well characterized, there are reports suggesting that the postoperative use of epoprostenol in PAH-CHD can improve outcomes. For example, one case report recently described successful atrial septal defect (ASD) closure in a patient with severe PAH (PAP > 110 mmHg). After closure and 2 years of oral PGI2 therapy, PAP decreased from 110/31 to 65/35 mmHg. 47 Similarly, Frost and colleagues 48 reported another patient with apparently inoperable PAH-CHD who experienced significant reversal of PAH and conversion to an operable state with judicious use of epoprostenol. The patient underwent successful closure of an ASD following 4-year-long IV epoprostenol therapy. Although the patient's PAP remained high (60–70 mmHg) in the immediate postoperative period, the pressures decreased progressively over the next 6 months. The patient was weaned off epoprostenol after 6 months and was followed uneventfully for 8 years postoperatively. 48 While clinically efficacious, routine epoprostenol use is limited by the need for continuous IV infusion, the possibility of high cardiac output failure, paradoxical embolization, and possible life-threatening sepsis related to central-line infections.
Given the limitations associated with use of IV prostanoids, it is appealing to consider whether inhaled forms of these drugs may also serve as potential alternatives in the clinical setting. Currently, there is some literature concerning the off-label use of epoprostenol administered via inhalation for severe PAH after adult cardiac surgery, such as coronary artery bypass grafting, cardiac valve surgery, and orthotopic heart transplantation.49–51 Furthermore, some studies have shown that inhaled epoprostenol can be a feasible option for PAH-CHD patients, with neonates benefiting more consistently than older infants and children from this therapy.52,53 In 1995, Zwissler 54 described the successful intra- and postoperative use of aerosolized epoprostenol, without causing systemic hypotension or deterioration of gas exchange, in a newborn with total anomalous pulmonary venous connection and severe PAH. Another case report showed a synergistic effect of inhaled epoprostenol and iNO in the treatment of refractory PAH in a 3-month-old male patient with D-TGA and ventricular septal defect after pulmonary artery banding and placement of a Blalock-Taussig shunt. 55 In a prospective interventional pilot study, Carroll and colleagues 56 examined the physiologic effects of inhaled epoprostenol (15-minute course, intraoperatively and postrepair) in 6 children with PAH-CHD. They found that the agent significantly reduced mPAP and improved oxygenation. Therefore, they suggested that inhaled epoprostenol could be used as an alternative pulmonary vasodilator when children with PAH-CHD demonstrate inadequate response to iNO, with a major advantage of the absence of systemic hypotension.51,56 Given the findings of the clinical studies noted above, inhaled epoprostenol has potential utility as an alternative to IV therapy in the perioperative management of PAH-CHD, but more studies are needed to validate these findings.
Treprostinil
In 2002, the Food and Drug Administration (FDA) approved subcutaneous treprostinil for use in PAH; approval of its IV form followed in 2004.57,58 While it has a longer half-life, IV treprostinil has a side-effect profile similar to that of IV epoprostenol, with the exception of the potential for an increased risk of gram-negative line infections. 59 In 2009, treprostinil was approved for inhalation in the outpatient setting. Oral treprostinil is currently being studied but has not yet been approved for clinical use.60,61 Recently, one group has shown that stable PAH patients who are not candidates for long-term systemic prostanoid therapy can be safely transitioned to inhaled treprostinil, provided that they can be monitored routinely for signs of clinical decompensation.62,63 Another clinical trial studying the early safety and efficacy of inhaled treprostinil in children has shown that the agent improves functional capacity and is well tolerated. 64 It remains to be seen whether this agent can be safely incorporated into the surgical setting as an alternative to IV epoprostenol.
Iloprost
Approved by the FDA for inhalation treatment of PAH in 2004, iloprost has been shown to decrease mPAP and PVR by selectively targeting ventilated lung segments and reducing the risk of systemic vasodilation.65,66 In 2008, Limsuwan and colleagues 67 reported aerosolized iloprost to be an effective drug for postoperative PH crisis in 12 cases of children with PAH-CHD without worsening tissue oxygenation. Loukanov et al. 33 compared iNO with aerosolized iloprost for treatment of perioperative PAH-CHD and found no difference between two groups regarding the frequency of PH crisis, mPAP, and duration of mechanical ventilation. Recently, in a randomized, open-label clinical trial, Kirbas et al. 68 compared aerosolized iloprost to iNO perioperatively in children with severe PAH-CHD and found no significant difference in hemodynamic parameters. Aerosolized iloprost may have a favorable safety profile relative to iNO because it is not associated with toxic reactions and can be easily administered by nebulizer instead of a complex delivery system such as that required for iNO. 68
ENDOTHELIN RECEPTOR ANTAGONISTS (ERAS)
Endothelins contribute to PAH pathobiology by promoting pulmonary smooth muscle cell hypertrophy, proliferation, and vasoconstriction through their interaction with the endothelin receptors (ETRs). 69 Although ERAs are attractive therapeutic alternatives for treating PAH-CHD patients, their routine use must be tempered by awareness of the adverse reactions associated with these drugs, such as hepatotoxicity, anemia, teratogenicity, fluid retention, peripheral edema, testicular atrophy, and infertility. 70
Bosentan
Among the currently available ERAs, bosentan has a supportive data set for PAH-CHD. 71 Studies have shown that bosentan significantly improves short-, medium-, and long-term clinical, exercise, and hemodynamic parameters without compromising peripheral oxygen saturation in PAH-CHD patients.72–75 Several case reports have shown that bosentan can effectively reduce the postoperative PVR and mPAP of PAH-CHD patients.76,77
Studies have also shown a role for bosentan in lowering PVR in patients with univentricular physiology. Ovaert and colleagues 78 showed that bosentan improved oxygen saturation at rest and during exercise in patients with failing Fontan circulation. In a case report that included 8 children with univentricular physiology who were not candidates for right-sided heart bypass because of elevated PVR, Hirono et al. 79 demonstrated that use of bosentan significantly lowered PVR and allowed the successful performance of the Fontan procedure. While it is possible that patients with other forms of CHD (e.g., ASD) who are not surgical candidates because of severe PAH may derive benefits from perioperative bosentan therapy, its role in this setting is still a matter of debate.80–82 Further study is needed to determine whether pretreatment with bosentan can influence either morbidity or mortality in patients at high risk for PH crisis.
Ambrisentan
Ambrisentan is a propanoic acid–based ETR-A-elective antagonist approved for once-daily administration by the FDA in 2007. Two pivotal randomized, controlled trials demonstrated significant improvements in 6-minute walk distance and clinical amelioration for adult PAH patients with ambrisentan therapy. 83 However, patients with PAH-CHD were excluded from these studies. Further studies in children (including 15 PAH-CHD patients) suggest that ambrisentan treatment is safe, with pharmacokinetics similar to those in adults, and that patients may show additional improvement on transition from bosentan to ambrisentan.84,85 Ambrisentan may have a more favorable adverse profile than bosentan and sitaxsentan. 86 Given the low rate of transaminase elevations associated with ambrisentan (~2.8%–3.1%), monthly liver transaminase monitoring is no longer mandated by the FDA. 83 Overall, there have been limited data for the use of ambrisentan in PAH-CHD and in the prevention of PH crisis. More study is needed before ambrisentan can be recommended for this purpose.
PHOSPHODIESTERASE INHIBITORS
As intracellular second messengers, cyclic adenosine mono-phosphate (cAMP) and cGMP play an important role in the pathophysiology of pulmonary vascular diseases. Phosphodiesterases (PDEs), especially the isoenzymes PDE-3 and PDE-5, can inactivate cAMP and cGMP to enhance NO signaling. Therefore, PDE-3 inhibitors (e.g., milrinone and enoximone) and PDE-5 inhibitors (e.g., sildenafil and tadalafil) can decrease PVR and increase cardiac index by augmenting endogenous levels of cGMP.
Milrinone
IV milrinone is extensively used to induce positive cardiac inotropy and reduce mPAP in cardiac surgery, but it is associated systemic hypotension and increased vaso-active drug requirements.87,88 Despite its beneficial hemodynamic effects, recent clinical trials showed that oral and IV milrinone led to increased mortality in acute and chronic heart failure. 87 However, clinical outcomes of milrinone used after cardiac surgery remain uncertain. In a recent meta-analysis of 20 randomized trials, Majure et al. 87 found no difference in mortality between milrinone-treated patients and control patients but did find a trend toward improved survival in PAH-CHD patients. This result was consistent with the outcomes of other three clinical trials of pediatric cardiac corrective surgery demonstrating prevention of low-cardiac-output syndrome.89–91
The hemodynamic and oxygenation profiles obtained with inhaled milrinone demonstrated greater safety than those with its IV form after CPB.88,92,93 Possible explanations for this effect are better targeting with an inhaled agent, high local drug concentrations, less systemic hypotension, and better matching of the lung's ventilation and perfusion. 94 As an alternative to iNO and epoprostenol, inhaled milrinone does not require complex apparatus and is less expensive. 95 Animal studies have shown that inhaled milrinone given before CPB prevents reperfusion injury.88,96 In a randomized clinical trial, nebulized milrinone significantly decreased mPAP and PVR in the peri-operative setting in children with PAH-CHD. 97 In our view, it is possible that the physiologic response to milrinone, especially with aerosol delivery, in PAH-CHD patients is distinct from that in patients with acquired heart diseases, such as coronary artery disease and cardiac valvular diseases.
Sildenafil
Sildenafil, a PDE-5 inhibitor, has been shown to induce favorable hemodynamic responses, improve symptoms and exercise capacity, and improve arterial oxygenation in atients with IPAH and Eisenmenger syndrome (ES).98–100 Evidence shows that sildenafil is an effective agent for treatment of postoperative PAH associated with left heart disease and is a useful adjunctive therapy to facilitate weaning from inhaled and IV pulmonary vasodilators, such as milrinone, nitroglycerine, nitroprusside, and iNO.101–103 In a controlled, prospective, randomized, double-blind trial, Shim et al. 104 showed that in patients with PAH undergoing valve replacement surgery, oral sildenafil before the introduction of anesthesia resulted in a significant decrease of mPAP and PVR at 30 minutes after ingestion, without any changes in mSAP and systemic vascular resistance (SVR).
Oral sildenafil is now an established treatment for PAH-CHD in children and can attenuate rebound pulmonary hypertension after iNO withdrawal during the early postoperative period.105–107 A retrospective study on the pre- and postoperative effects of oral sildenafil as monotherapy in children with PAH-CHD showed that the preoperative-sildenafil group had significantly lower mPAP, shortened mechanical ventilation time without PH crisis, and shortened sequelae when compared to the postoperative-administration group, particularly when sildenafil is given both preoperatively and postoperatively. 34 However, the pharmacokinetics and optimal dosage of sildenafil in infants remain uncertain. Mourani et al. 108 recommended using an initial dose of 0.5 mg/kg (3–4 times a day) and steadily increasing the dose (to a maximum of 2 mg/kg) over 1–2 weeks until the desired clinical response is achieved in chronic sildenafil therapy.
To avoid impaired enteral absorption, IV sildenafil has been administered in critically ill PAH-CHD patients to prevent PH crisis.109,110 Related preliminary trials have shown that IV sildenafil improves PAP, PVR, time to extubation, and ICU stay in children after cardiac surgery.110,111
Although sildenafil is a preferential pulmonary vasodilator, administration of a higher oral dose of sildenafil (>40 mg 3 times a day) still has a risk of worsening hypoxia by causing ventilation-perfusion mismatch, decreasing SVR, and subsequently increasing right-to-left shunting.109,112 Other side effects of the agent include headache, flushing, dyspepsia, and epistaxis. Vassalos et al. 113 recently found that preoperative oral sildenafil (0.5 mg/kg at 6-hour intervals, administered the day before pediatric cardiac surgery) did not affect postoperative mPAP and PVR and instead negatively affected ventricular function and oxygenation. This result highlights the importance of cautious use in PAH-CHD patients with preexisting hypoxia or myocardial dysfunction.
Tadalafil
Tadalafil is another, longer-acting PDE-5 inhibitor, with the significant advantage of once-daily dosing, that has recently been used for the treatment of PAH in adults. 114 There is some evidence that tadalafil can be safely used for pediatric patients with PAH (including ES) and may attenuate progression of disease, 115 suggesting a potential use in perioperative PAH-CHD patients, but more studies are required before recommending its use in this clinical setting.
COMBINATION THERAPY
Given that pulmonary vasodilators of different classes target different pathologic processes, combination therapy is theoretically attractive in perioperative PAH-CHD patients, as it may have additive or synergistic effects on the pulmonary vasculature by targeting 2 or 3 therapeutic pathways (Fig. 1). The goal of combination therapy should be to maximize efficacy with minimal toxicity. To date, nearly all trials of combination therapy have employed a strategy of adding one or two new agents to patients who failed to respond to or began to deteriorate on their initial therapy. 116 The recently published European Society of Cardiology and European Respiratory Society guidelines on PAH suggest the use of combination therapy in patients deteriorating on monotherapy, despite the absence of firm evidence from randomized, controlled trials. 117
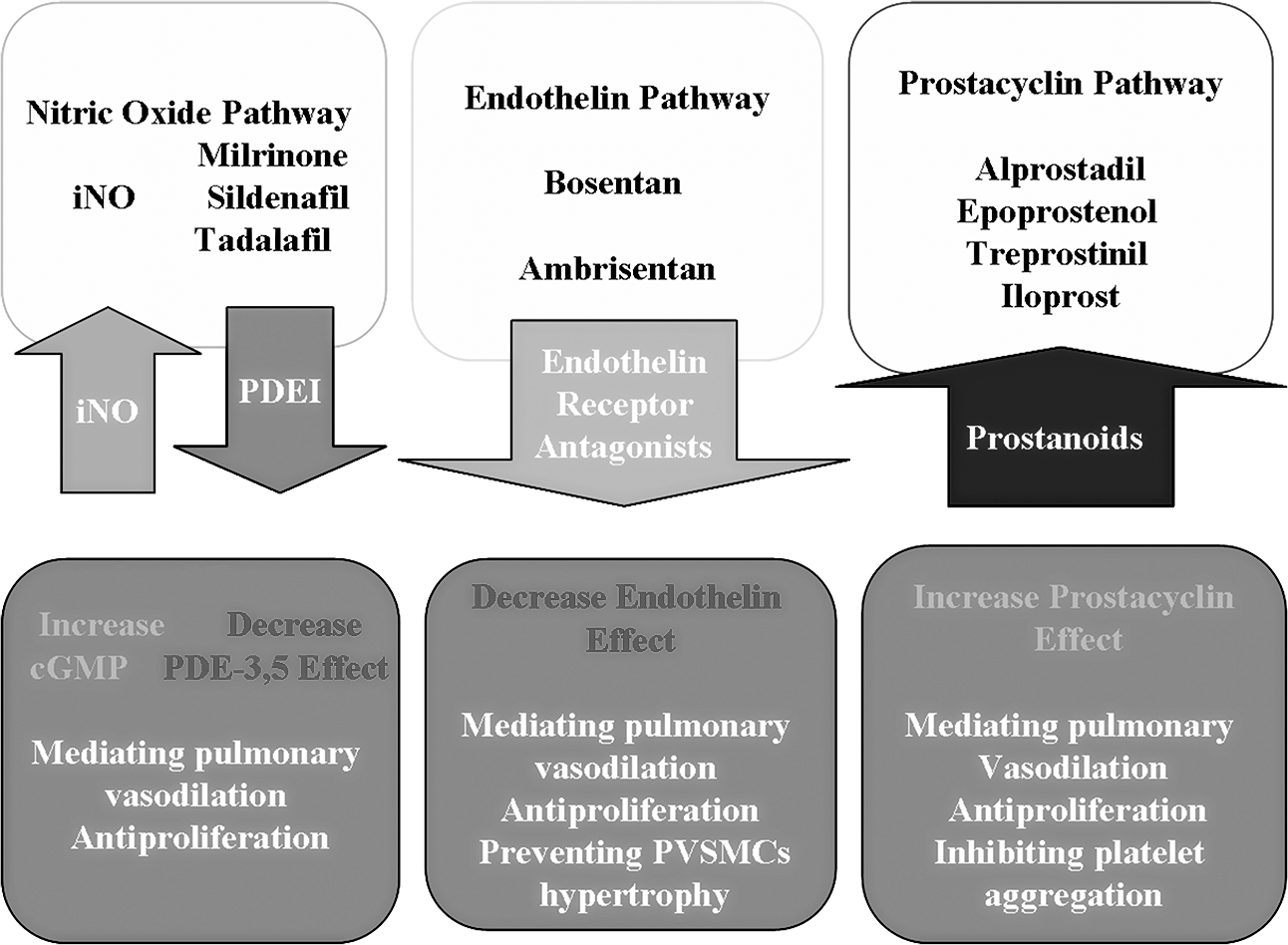
Three therapeutic pathways. iNO: inhaled nitric oxide; PDE: phosphodiesterase; PDEI: PDE inhibitor; cGMP: cyclic guanosine monophosphate; PVSMC: pulmonary vascular smooth muscle cell. A color version of this figure is available online.
There are a variety of therapy combinations that have been tested in general PAH populations; however, only a few clinical studies have focused on perioperative combination therapy for PAH-CHD patients. Recently, studies have demonstrated that a few patterns of coadministration are safe and result in favorable effects after high-risk heart valve surgery, including combinations of iNO with inhaled iloprost 7 and iNO with oral sildenafil. 118
In pediatric patients undergoing heart surgery, oral sildenafil attenuated rebound pulmonary hypertension after iNO withdrawal during the early postoperative period. 105 Furthermore, Stocker and colleagues 110 found that IV sildenafil augmented the pulmonary vasodilator effects of iNO yet produced systemic hypotension and impaired oxygenation. Recently, a study demonstrated that IV sildenafil reduced PAP and shortened time to extubation and ICU stay without significant adverse events, alone or with milrinone coadministration. 119 In summary, combination therapy for PAH-CHD has some scientific rationale and considerable appeal. However, the clinical-trial experience is limited, and the optimal combinations and administration strategies have yet to be clarified.
In addition to combination therapy, powerful circulatory and respiratory support can be provided by EMCO to patients with severe acute cardiac and respiratory failure that is refractory to mechanical ventilation.120,121 ECMO has been the most common form of mechanical cardiopulmonary support for children with refractory cardiac failure, with survival rates varying from 33% to 58% for all pediatric patients.122,123 Through 2008, more than 7,500 pediatric patients have been supported with cardiac ECMO, reported by the Extracorporeal Life Support Organization. 124 Some studies speculated that earlier diagnosis of PH crisis and right heart failure, accompanied by the use of ECMO during the perioperative period, may improve outcomes in adult CHD patients.125,126 However, the clinical results of ECMO support for postcardiotomy cardiac failure in adults are far from satisfactory, with successful weaning from ECMO possible in only 30%–60% of patients. 127 Furthermore, for adult patients, the benefit of ECMO remains controversial because convincing results have never been demonstrated in a large patient cohort.121,128 According to the data from large observational studies and current registries, the survival rates after ECMO therapy are poor, with in-hospital mortality rates of 60%–80%.127,129 Therefore, clear guidelines for ECMO support for perioperative treatment in PAH-CHD patients are still lacking, and the decision about whether to choose ECMO support should be individualized, based on a comprehensive consideration of possible poor outcome, high complication rates, and huge resource consumption.127,130,131
CONCLUSIONS
Recently, there have been numerous advancements in pharmacological interventions for PAH as a whole, but there is scant evidence to support a sudden change in the perioperative drug treatment of PAH-CHD patients.
Evidence suggests that the historical mainstay, iNO, remains the first-line monotherapy, although it is far from ideal.
In our view, when PAH-CHD is noted preoperatively, appropriate PAH-specific therapy should be initiated before cardiac surgery. IV milrinone may be prudently used to decrease PAP and increase cardiac output. Without antecedent evidence of PAH-CHD, but before a major cardiac surgery with potential for inducing PH crisis—such as an arterial switch operation for infants or a Fontan operation for adult patients—it is safer to directly initiate iNO if required. According to a European consensus, a therapeutic trial of iNO entails administration of 20 ppm when postoperative PAH is present. 132 Therefore, routine use of iNO (from 5–20 to a maximum of 80 ppm) is the first choice when patients are at high risk of PH crisis. The optimal dose of iNO is the lowest possible dose that provides control of PAP. Caution should be exercised when administering iNO to patients with left-sided obstructive lesions, such as congenital mitral stenosis or cor triatriatum, or in the setting of nonanatomic corrective surgery. 133
If no significant response to the aforementioned treatment is observed, further pharmacological interventions should be performed. For example, oral sildenafil may be administered by nasogastric tube in order to exert its synergic effect. Furthermore, other pulmonary vasodilators, such as bosentan and inhaled iloprost, may be considered. When patients face life-threatening refractory postoperative PAH, supportive ECMO as a bridge for heart and lung transplantation or lung transplantation, in combination with repair of the underlying cardiac defect, may be the last therapeutic option. Figure 2 outlines our recommended algorithm for perioperative management of PAH-CHD patients in the setting of cardiac surgery.
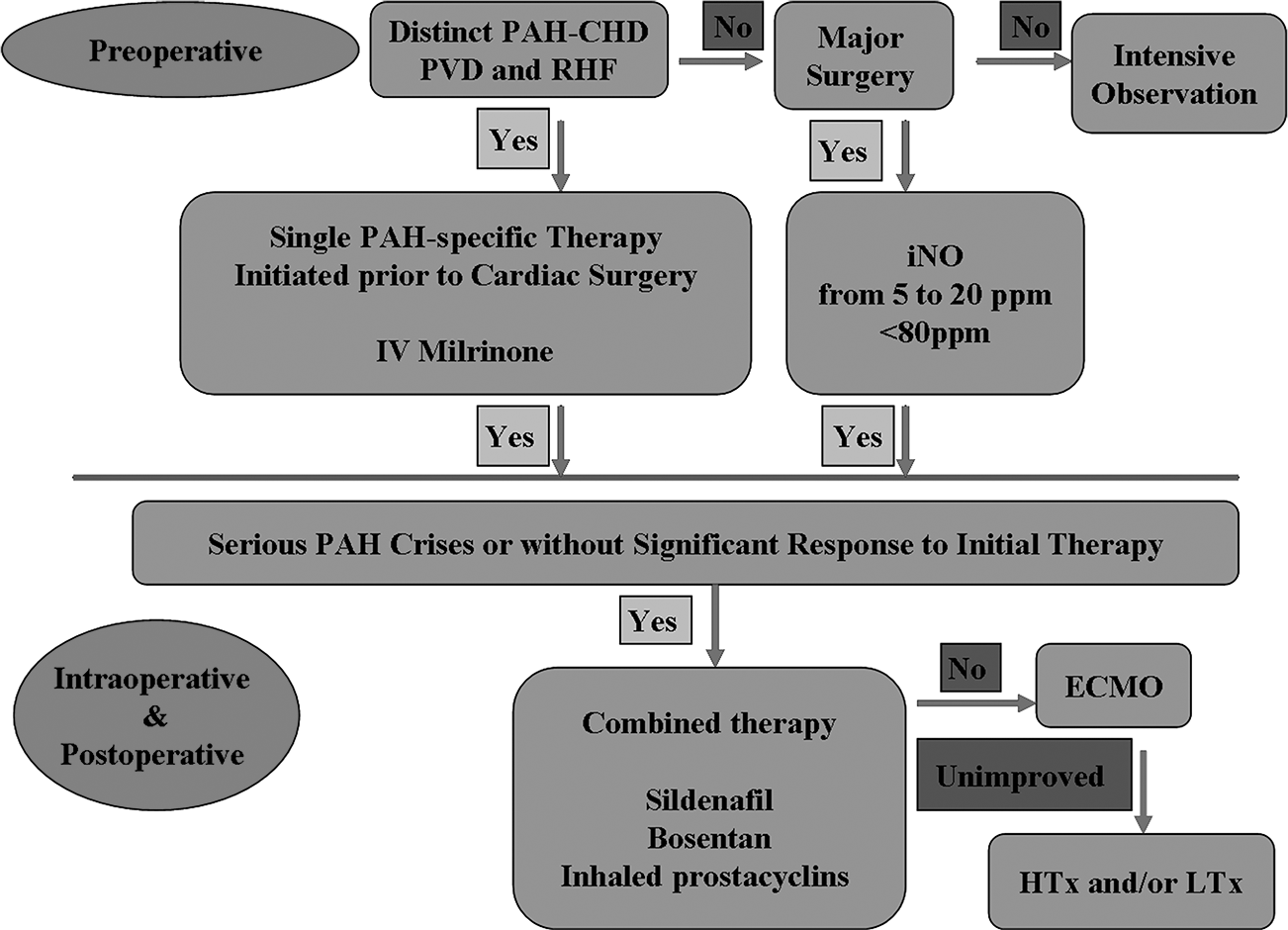
Recommended algorithm for perioperative management of patients with pulmonary arterial hypertension secondary to congenital heart disease (PAH-CHD) in the setting of cardiac surgery. PVD: pulmonary vascular disease; RHF: right heart failure; IV: intravenous; iNO: inhaled nitric oxide; ECMO: extracorporeal membrane oxygenation; HTx: heart transplantation; LTx: lung transplantation. A color version of this figure is available online.
At present, the selection of optimal pharmacological therapy for PH crisis is complex, as the majority of drug information is often extrapolated from studies carried out in adults with chronic PAH. Nevertheless, the vast majority of literature related to the pharmacological treatment for PAH-CHD surgery focuses on children, and there are very few data exclusively aiming at adult patients (Table 1). Furthermore, clinical prospective trials large enough to adequately assess specific dosing regimens, side effects, and potential complications of perioperative PAH-CHD patients are not available. Therefore, well-designed larger trials are needed to further identify the most appropriate therapeutic strategy to treat operative PAH-CHD.
Evidence for benefits of drugs for pulmonary hypertensive crisis after congenital heart surgery in children and adults
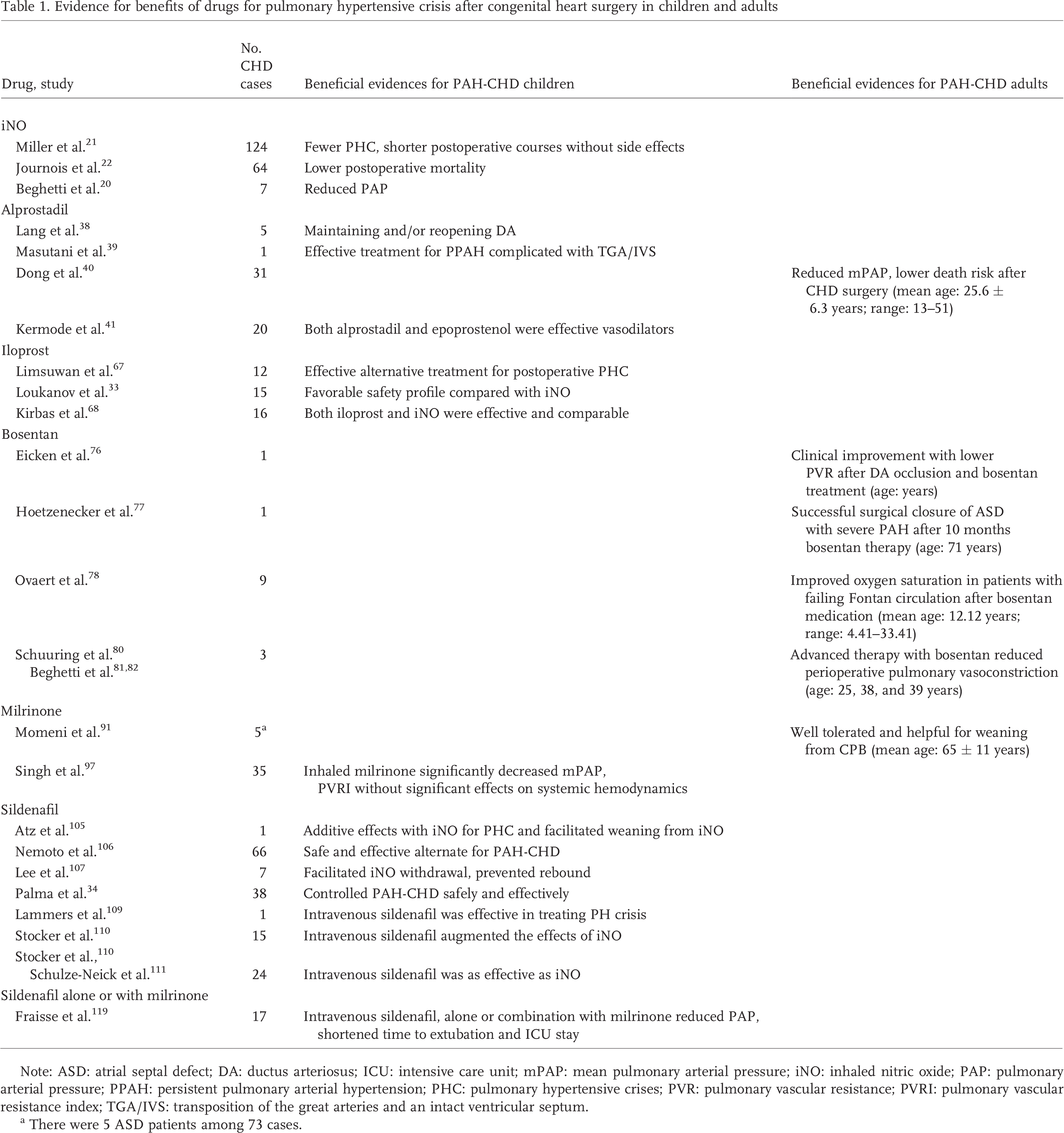

Note: ASD: atrial septal defect; DA: ductus arteriosus; ICU: intensive care unit; mPAP: mean pulmonary arterial pressure; iNO: inhaled nitric oxide; PAP: pulmonary arterial pressure; PPAH: persistent pulmonary arterial hypertension; PHC: pulmonary hypertensive crises; PVR: pulmonary vascular resistance; PVRI: pulmonary vascular resistance index; TGA/IVS: transposition of the great arteries and an intact ventricular septum.
There were 5 ASD patients among 73 cases.
