Abstract
The development of pulmonary hypertension is a poor prognostic sign in patients with obstructive sleep apnea (OSA) and affects both mortality and quality of life. Although pulmonary hypertension in OSA is traditionally viewed as a result of apneas and intermittent hypoxia during sleep, recent studies indicate that neither of these factors correlates very well with pulmonary artery pressure. Human data show that pulmonary hypertension in the setting of OSA is, in large part, due to left heart dysfunction with either preserved or diminished ejection fraction. Longstanding increased left heart filling pressures eventually lead to pulmonary venous hypertension. The combination of hypoxic pulmonary vasoconstriction and pulmonary venous hypertension with abnormal production of mediators will result in vascular cell proliferation and aberrant vascular remodeling leading to pulmonary hypertension. These changes are in many ways similar to those seen in other forms of pulmonary hypertension and suggest shared mechanisms. The majority of patients with OSA do not receive a diagnosis and are undertreated. Appreciating the high prevalence and understanding the mechanisms of pulmonary hypertension in OSA would lead to better recognition and management of the condition.
Pulmonary hypertension (PH) is a hemodynamic and pathophysiological state that can be found in multiple clinical conditions. These have been classified by the World Health Organization (WHO) into five clinical groups with specific characteristics (Table 1). 1 WHO group 2 is the most common cause of PH in Western countries and is due to left heart disease—systolic and diastolic dysfunction and valvular disease.2–4 Obstructive sleep apnea (OSA) is commonly complicated by left heart disease and is associated with PH. 4 OSA is a form of sleep-disordered breathing that is increasingly prevalent, in part due to the increasing rate of obesity and enhanced public awareness. An estimated 40 million Americans experience OSA, with a 3%–7% prevalence among men and a 2%–5% prevalence among women. 5 OSA is an independent risk factor for systemic hypertension, stroke, myocardial ischemia, congestive heart failure, arrhythmias, and sudden cardiac death.6–11 PH is present in 12%–34% of patients with OSA.12–15 However, the role of OSA in the development of PH and its mechanisms, independent of left ventricular failure, are not entirely clear. Patients with PH present with symptoms of dyspnea on exertion, fatigue, lightheadedness, chest pain, syncope, palpitations, and/or lower extremity edema.
Updated clinical classification of pulmonary hypertension (PH), Nice, France, 2013

Note: Adapted from Simonneau et al. 1 ALK1: activin-like receptor kinase-1; BMPR2: bone morphogenic protein receptor type II; CAV1: caveolin-1; KCNK3: a gene encoding potassium channel super family K member-3; PAH: pulmonary arterial hypertension; SMAD9: mothers against decapentaplegic 9.
When PH occurs as a consequence of OSA, however, symptoms may not be present because of obesity and a lack of physical exertion, or symptoms of PH may be overshadowed by those of other cardiovascular abnormalities. Nevertheless, it is paramount to confirm the presence of PH in patients with OSA for three reasons: (1) OSA is associated with a higher mortality among patients with PH than without PH, (2) a treatment modality specific to OSA should be formulated, and (3) the possible coexistence of another etiology of PH that may require a different management strategy should be determined. In this review, we discuss the epidemiology and pathophysiology of PH in the setting of OSA and its management strategies.
EPIDEMIOLOGY
Establishing the prevalence of PH due to OSA is challenging owing to the range of hemodynamic parameters and diagnostic tests used as well as the potential inclusion of patients with confounding diseases. In a large series of 220 consecutive subjects with OSA who had undergone right heart catheterization using a mean pulmonary artery pressure (Ppa) of >20 mmHg as diagnostic criterion for PH, Chaouat et al. 12 observed PH in 37 (17%) of 220 patients. However, of these 37 patients, 19 (51%) had pulmonary function testing demonstrating a forced expiratory volume in 1 s/forced vital capacity of <65%, indicative of obstructive lung disease. In a multiple regression analysis, PH was strongly linked to the presence of an obstructive (rather than restrictive) ventilatory pattern, hypoxemia, and hypercapnia in this cohort. To determine whether PH can be present in OSA in the absence of hypoxic lung disease, Sajkov et al. studied 32 patients with OSA and found PH (estimated mean Ppa ≥20 mmHg on Doppler echocardiography) in 34% of the subjects. Hetzel et al. 17 studied 49 consecutive patients with OSA with normal pulmonary function testing and found six (12%) with resting PH using a mean Ppa >20 mmHg criterion on right heart catheterization. None had pathologically elevated pulmonary vascular resistance, and a majority had notable elevations in pulmonary artery occlusion pressure (PAOP), implicating left-sided heart disease as the mechanism of the PH. 17 In a study involving 44 patients with OSA without chronic obstructive pulmonary disease (COPD) or left ventricular dysfunction, Bady et al. 13 found PH (mean Ppa >20 mmHg and PAOP <15 mmHg) in 12 patients (27%).
The prevalence of sleep-disordered breathing in PH was investigated by several groups. Ulrich et al. 18 observed sleep apnea, mainly central sleep apnea (CSA), in 17 (45%) of 38 patients with different etiologies of PH. The prevalence of OSA in patients with PAH and chronic thromboembolic PH (CTEPH) with New York Heart Association functional class II–III without COPD or left ventricular dysfunction was 89%. 19 In a study of 169 patients with PAH, 45 patients (26.6%) had an apnea–hypopnea index (AHI) >10 events/h. Of these, 27 patients (16%) had OSA, and 18 patients (10.6%) had CSA. 20 Among 28 patients with idiopathic PAH, 7% had OSA and 14% had CSA. 20
All in all, patients with PH of various etiologies have high prevalence of OSA. Likewise, patients with OSA are also at increased risk of having PH. 15 In general, 27%-30% of patients with OSA without left ventricular dysfunction or hypoxemic lung disease have PH.13,16 A conservative estimate of the overall prevalence of PH associated with OSA in the United States is 2.5 million cases. Of importance is that the patients with OSA and PH have lower quality of life 21 and higher mortality than those without PH. 22
PATHOPHYSIOLOGY
Structure and function of the pulmonary circulation under normal conditions
Anatomically, the pulmonary circulation is divided into arteries, arterioles, capillaries, venules, and veins. The pulmonary circulation is a low-resistance system with the normal Ppa systolic/diastolic being ≈25/8 mmHg compared with 120/70 mmHg for the systemic circulation, with similar blood flow. The main pulmonary artery has smaller wall thickness and less organized elastic lamina despite having the same size as the main aorta. The capillary system that is not in contact with alveoli has basement membranes that are not fused and has more collagen, proteoglycan matrix, and fibroblasts, some of which may contain actin-myosin complex. Pulmonary circulation is almost always dilated with negligible resting tone and low resistance and hence would not be able to dilate further, as evident by the lack of vasodilatory response to inhaled nitric oxide (NO) in those subjects breathing air, 23 which indicates that the only regulation is by vasoconstriction. Increased cardiac output during exercise is accommodated by recruitment of vessels, thereby increasing the size of the vascular bed. The later mechanism can keep the pressure low in spite of marked increase in flow.
Structure and function of the pulmonary circulation under abnormal conditions
The reduction in alveolar oxygen tension, such as in low ventilation/perfusion units (high altitude, lung parenchymal, or airway disease), can lead to pulmonary vasoconstriction. Depending on the magnitude of the alveolar hypoxia (focal vs. global), pulmonary vascular resistance can increase by up to 300%. 24 Hypercapnia and acidosis, which independently cause pulmonary vasoconstriction, tend to augment the effect of hypoxic pulmonary vasoconstriction.25,26 Differential lung ventilation of normal human subjects with hypoxic gas decreases blood flow to the same lung by 22% through hypoxic vasoconstriction, shifting the blood flow to the normoxic lung. However, redistribution of blood flow is not powerful enough to overcome the gravitational effects of blood diversion from the upper lung to the lower lung in the lateral decubitus position.27,28 Hypoxic pulmonary vasoconstriction, although regarded as a physiological process that preserves systemic oxygenation, is also regarded as a pathophysiological entity predisposing to heightened pulmonary artery tones and subsequent PH. 29 Wu and colleagues 30 have shown that, although acute hypoxia (partial pressure of oxygen, 25–30 mmHg for 5–10 minutes) stimulates a reduction in reactive oxygen species (ROS), chronic hypoxia (48 hours) actually increases ROS production in human pulmonary artery smooth muscle cells. This points to a potential difference at the subcellular level response to acute and chronic hypoxia, which may explain the phenotypical changes seen in acute hypoxia (vasoconstriction) and chronic hypoxia (vascular remodeling). Acute hypoxia constricts precontracted human pulmonary artery rings in a manner that is dependent on the presence of the endothelium, because denuding the endothelium resulted in a markedly reduced hypoxic vasoconstrictive response. 31 Because NO is a potent vasodilator, endothelial NO synthase (eNOS) inhibition would logically suggest that the vasoconstriction-vasodilation balance may be shifted in chronic hypoxia toward constriction by reducing NO production. Chronic hypoxia is associated with an increase in Rho kinase A expression with a simultaneous decrease in eNOS messenger RNA and protein expression in human pulmonary endothelial cells. 32 However, there is a compensatory mechanism by increasing inducible NOS and NO production of human pulmonary endothelial cells.33,34 Key regulators of vascular remodeling in response to chronic hypoxia include the Rho GTPase family of proteins, which are involved in cell adhesion, migration, and proliferation. 35 Native inhabitants of Peru are often born with right ventricular hypertrophy and elevated resting Ppas; those children who remain at sea level demonstrate a rapid reversal of these phenomena, whereas those who remain at high altitudes show little regression of these characteristics. 36 Autopsy of these individuals revealed that the PH was likely attributable to the thickening of the muscular layers of the pulmonary arterial tree. 37 These investigators measured arterial partial pressure of oxygen and saturation in these inhabitants and concluded that there was a direct causal relationship between hypoxia and PH.
MECHANISMS OF PH IN OSA
The majority of patients with OSA experience cyclical oxygen desaturations during sleep. These episodes can last from 10 seconds to more than 40 seconds several times an hour followed by arousals and complete or partial recovery of oxygen saturation. The cumulative effect of intermittent hypoxia can lead to polycythemia and PH. Most patients with OSA have normal oxygen saturation while awake, with the exception of those patients who also have obesity hypoventilation syndrome or underlying lung disease. Patients with obesity hypoventilation syndrome are at greater risk of having PH due to the additional effect of hypercapnia, with a prevalence 59% greater than that among those with OSA alone.21,38 Based on several studies, the average prevalence of PH among those with OSA is approximately 20%. This is in contrast to the prevalence of systemic hypertension, which can be as much as 60%. As a result of the high frequency of diurnal hypertension and intermittent surges in arterial blood pressure due to respiratory events during sleep, 39 patients with OSA have high prevalence of left ventricular hypertrophy 40 and dysfunction.41–43 Left ventricular dysfunction accounts for a large proportion of PH in patients with OSA.17,22 However, PH and right heart failure can develop in patients with OSA with preserved left ventricular ejection fraction. 44 The prevalence of PH in heart failure with preserved left ventricular ejection fraction was in the range of 52% (defined as mean Ppa >25 mmHg by right heart catheterization). 45 This was comparable to 62% in a cohort of 379 patients with heart failure with reduced ejection fraction, who had a mean Ppa >20 mmHg by right heart catheterization. 46 Mitral valve disease–associated PH shares some features with the PH seen in OSA—elevated left atrial filling pressure—in the presence of either diastolic or systolic left ventricular dysfunction. In a study of nine patients with mitral regurgitation and PH undergoing valve replacement, Du et al. 47 demonstrated pulmonary vascular changes similar to idiopathic PAH in the form of proliferation of vascular smooth-muscle cells and asymmetric neointimal hyperplasia in small pulmonary arteries and arterioles. These observations suggest that initial pulmonary venous hypertension due to left ventricular dysfunction can lead to PH indistinguishable from the idiopathic PAH form and further suggest shared cellular and molecular pathways in the pathogenesis of PH. Mathematical models exploring this paradigm demonstrate that there is an initial passive increase in pulmonary blood volume secondary to the hydrostatic forces resulting from heart failure with either reduced or preserved systolic function. 44 The result of this initial insult is a passive postcapillary PH with a normal transpulmonary pressure gradient and, consequently, relatively normal pulmonary vascular resistance. In addition to this pressure-dependent mechanism, hypoxia-sensitive inflammatory and proliferative pathways may be involved in the development of PH in OSA. 48 Animal models have clearly demonstrated that brief, repetitive exposure to hypoxemia over a duration of just a few weeks, a situation akin to intermittent hypoxia in OSA, is sufficient to cause pulmonary arteriolar remodeling and right ventricular hypertrophy.49,50 In a recent study, Sheikh et al. 51 demonstrated that exposure of mice to 10% hypoxia for 3 weeks resulted in muscularization of distal pulmonary arterioles.
In experiments in which mice were exposed to chronic intermittent hypoxia for 8 weeks, the induced PH was associated with increased lung levels of the NADPH oxidase subunits, Nox4 and p22phox, as well as increased activity of platelet-derived growth factor receptor β and its associated downstream effector, protein kinase B (the latter is involved in apoptosis, cell proliferation, transcription, and cell migration). 52 NADPH oxidase is an important source of superoxide production in the vasculature. Superoxide generation in the vascular wall is a well-recognized stimulus for vascular wall cell proliferation and vasoconstriction. 53 These chronic intermittent hypoxia-induced derangements were attenuated in similarly treated gp91phox knockout mice with disabled NADPH oxidase system, suggesting that NADPH oxidase-derived ROS contribute to the development of pulmonary vascular remodeling and hypertension caused by chronic intermittent hypoxia. 52
Several studies have implicated involvement of serotonin in the etiology of PH.54,55 A study by Launay et al. 56 showed that hypoxia-induced PAH in mice was associated with an increase in serotonin and its receptor expression, resulting in serotonin-dependent vascular remodeling. As a potent pulmonary vasoconstrictor, serotonin, released from pulmonary neuroendocrine cells and neuroepithelial bodies, might have a dual effect on pulmonary circulation, contributing to both hypoxia-induced acute vasoconstriction and chronic vascular remodeling by activating its cognate receptors.
Angiopoietin-1 (Ang-1) originating from vascular smooth muscle cells is an endothelial selective receptor tyrosine kinase (Tie2) agonist that stabilizes the development of newly formed blood vessels and promotes quiescence and structural integrity of mature vessels. 57 Hypoxia disrupts the constitutive Ang-1–Tie2 signaling by preventing Ang-1 from binding to the receptor. Consequently, loss of Tie2 signaling destabilizes the endothelium and induces an angiogenic response in the presence of vascular endothelial growth factor. 58 Human lungs from patients with nonfamilial PH of various causes, including mitral valve stenosis-associated PH, show high expression of Ang-1 in the smooth muscle cell lining of small pulmonary vessels and tyrosine phosphorylation of the Tie2 receptor in pulmonary vascular endothelium. These data led the authors to conclude that all forms of PH are linked by defects in the signaling pathway involving Ang-1 and Tie2. 47 The role of the Ang-1–Tie2 ligand-receptor system in the pathogenesis of PH is controversial. Other studies using transgenic mice models with overexpression of Ang-1 had shown a protective effect in monocrotaline-induced PH.59,60 Furthermore, serum levels of Ang-1 had an inverse correlation with pulmonary systolic pressure in patients with mitral stenosis. 61 Because biological roles of angiopoietins may depend on the presence of other angiogenic growth factors, the functional significance of the Ang-1–Tie2 system may be different in various pathophysiological conditions of PH. It is not known whether dysregulation of the Ang-1–Tie2 system is operative in PH associated with OSA. However, the findings that hypoxia or left heart dysfunction (mitral stenosis) are associated with pulmonary vascular remodeling will make Ang-1–Tie2 system involvement in OSA plausible.
Endothelin-1 (ET-1) is a member of a family of peptides produced primarily by the endothelium with a key regulatory role in vascular homeostasis and has potent vasoconstrictor properties. In the pulmonary arteries of rats exposed to chronic intermittent hypoxia, ET-1 expression was increased, and ET-1 more potently elicited constriction of the pulmonary artery due to increased expression of ETA receptors compared with normoxic rats. 62 In these animals, exposure to chronic intermittent hypoxia induced marked endothelial cell damage associated with a functional decrease of endothelium-dependent vasodilation in the pulmonary artery. 62 Plasma levels of ET-1 are elevated in several forms of PH.63,64 Individuals with PH due to left ventricular dysfunction demonstrate vasodilation of pulmonary vasculature with infusion of sitaxsentan, a selective ETA receptor antagonist, that is not seen in controls, which suggests a contributing role of ET-1 in PH related to left heart dysfunction. 65 However, endothelin receptor antagonists have not been proven to be beneficial in clinical trials involving patients with left heart dysfunction.66,67 The role of endothelin in PH of OSA is not known. Circulating levels of ET-1 in patients with OSA are no different from those in control subjects.68,69 In view of the effect of endothelin on the pulmonary vasculature in models of intermittent hypoxia and left heart dysfunction, it is conceivable that it might play a role in some patients with OSA and PH. Additional studies are needed to investigate the role of endothelin in PH of OSA.
NO is a potent vasodilator of pulmonary and systemic circulation. It is generated by the enzymatic action of NO synthase on L-arginine in endothelial cells, and the gaseous NO acts on soluble guanylate cyclase in vascular smooth muscle cells to generate cyclic guanosine monophosphate (cGMP), causing vasodilation. Chronic intermittent hypoxia causes suppression of eNOS and impairment of endothelial-dependent vasodilation by an NF-κB-dependent mechanism. 70 In humans with OSA, alveolar NO is reduced. 71 Furthermore, circulating cGMP is reduced in patients with OSA with endothelial dysfunction. 72 Riociguat, a stimulator of soluble guanylate cyclase–increasing cGMP, has recently been approved by the US Food and Drug Administration on the basis of its efficacy in preclinical and clinical trials of PAH (and in CTEPH), supporting the role of NO-cGMP system dysregulation in PAH and OSA.73,74
Obesity, through metabolic dysregulation and vascular inflammation, is associated with increased risk of PAH, independent of OSA and left heart dysfunction. 75 Adiponectin is secreted from adipose tissues and has anti-inflammatory and vascular homeostatic functions. 76 Circulating levels of adiponectin are decreased in individuals with obesity and OSA.77,78 Given the known effects of adiponectin on pulmonary vascular inflammation and remodeling,79,80 it seems likely that relative deficiency of adiponectin, as seen in obesity and OSA, could be an important mechanistic link between OSA and PH.
In summary, the mechanisms of PH in OSA are multifactorial and due to both increased left heart pressures and hypoxia-related processes with involvement of numerous pathways involving ROS, perturbation of NO, angiogenic factors, and vasoactive agents, resulting in partially reversible vasoconstriction and increased Ppa (Fig. 1).
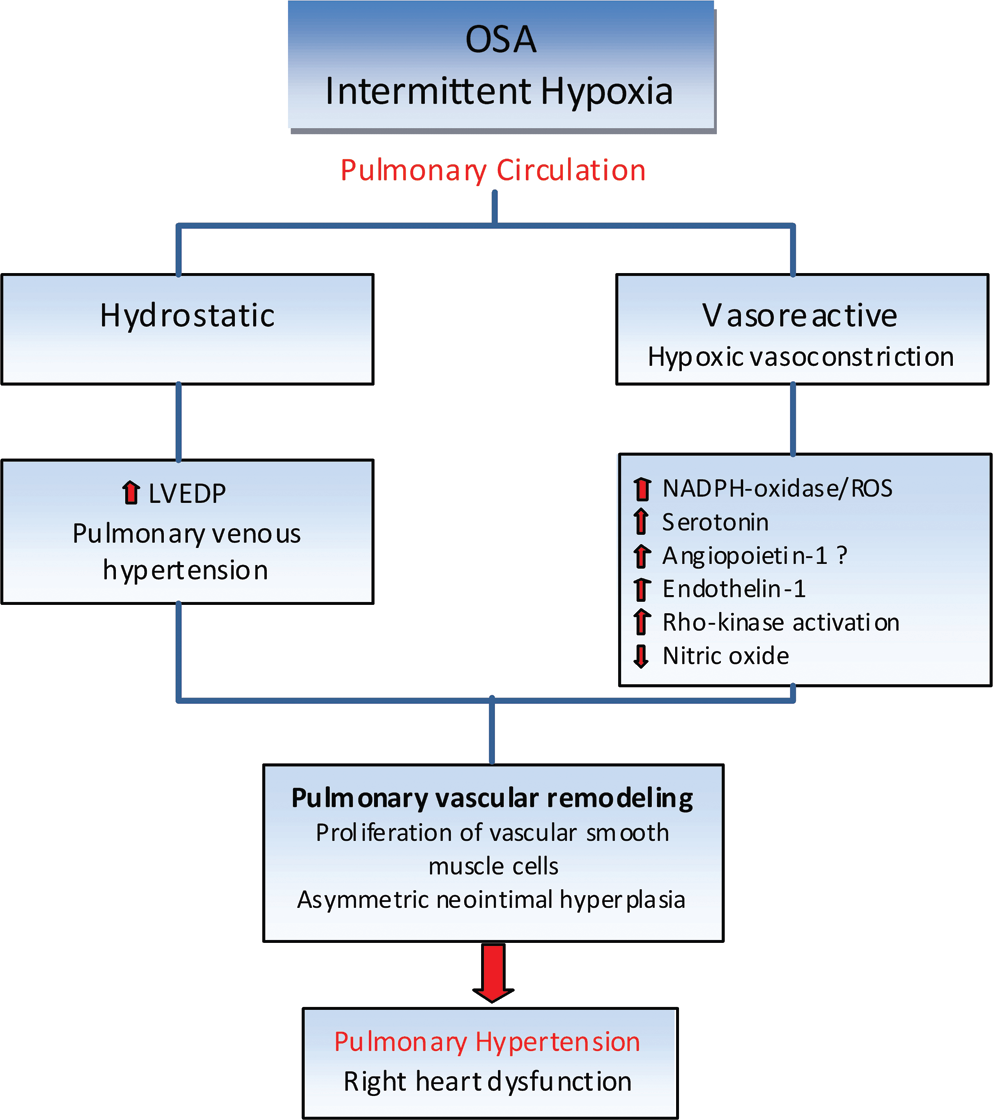
Obstructive sleep apnea (OSA) causes pulmonary hypertension through hypoxia pathway with activation of vasoactive factors and hydrostatic mechanism due to increase in left atrial pressure leading to pulmonary venous hypertension. Both pathways eventually cause vascular remodeling, pulmonary arterial hypertension, and right heart dysfunction. LVEDP: left ventricular end-diastolic pressure; NADPH: nicotinamide adenine dinucleotide phosphate; ROS: reactive oxygen species.
DIAGNOSTIC CONSIDERATIONS
The evaluation process for a patient with suspected PH requires a series of investigations intended to confirm the diagnosis, which is best done in a multidisciplinary pulmonary vascular center. The details of the workup for patients with suspected PH is beyond the scope of this review.1,81 However, the key studies will be discussed here. Patients with PH present with symptoms of dyspnea, lightheadedness on exertion, fatigue, chest pain, syncope, palpitations, and/or lower extremity edema. Transthoracic echocardiography provides several variables that correlate with right heart hemodynamics, including estimated pulmonary arterial systolic pressure, and should always be performed in the case of suspected PH as a screening modality. A systematic review and meta-analysis of 29 studies with a total patient population of 1,998 demonstrated an overall correlation coefficient of 0. 7 (95% confidence interval [CI], 0.67–0.73) for estimated systolic Ppa between color Doppler echocardiography (tricuspid regurgitant jet method) and right heart catheterization, with a sensitivity and specificity of 83% (95% CI, 73%–90%) and 72% (95% CI, 53%–85%), respectively. 82 Of note, the agreement between Doppler echocardiography and right heart catheterization data was similar at both mild and moderately elevated systolic pulmonary arterial pressure values. Furthermore, echocardiography is a useful and noninvasive modality not only for estimating pulmonary pressure but also for determining underlying anatomical and functional cardiac abnormalities in patients with suspected PH. However, the diagnosis of PH and the assessment of vasodilatory capacity of pulmonary vasculature require right heart catheterization. Other diagnostic tests may include serologic testing for collagen vascular diseases, pulmonary function tests, chest imaging, ventilation-perfusion scanning, and arterial blood gases for underlying pulmonary diseases. There are no formal guidelines for routine sleep study in patients with PH; however, in view of the high prevalence of nocturnal hypoxemia and OSA in PH, patients with PH should be screened for sleep-disordered breathing by sleep study. 19
EFFECT OF TREATMENT OF OSA ON PH
In one of the first studies of the effect of continuous positive airway pressure (CPAP) treatment on pulmonary hemodynamics in OSA, Sforza et al.
83
evaluated seven patients with PH with right heart catheterization before and after 1 year of CPAP treatment. Despite some improvement in oxygen saturation, mean Ppa did not change. A decade later, Alchanatis et al.
14
examined the effect of CPAP therapy in six patients with OSA and PH diagnosed on echocardiography and confirmed by right heart catheterization with normal PAOP values. After more than 6 months of CPAP therapy, there was a significant reduction in mean Ppa value from 25.6 ± 4.0 mmHg to 19.5 ± 1.6 mmHg (
SUMMARY
PH is prevalent in OSA and is commonly associated with left ventricular dysfunction. Pulmonary vascular changes are due to both hypoxic vasoconstriction and vascular remodeling. PH tends to improve with the treatment of OSA, and the more severe the PH the greater the response to CPAP. However, treatment of OSA may not completely resolve PH. These patients should be evaluated for other etiologies and considered for pharmacologic therapy.
