Abstract
Insulin resistance is highly prevalent in pulmonary arterial hypertension (PAH) patients. However, the long-term impact of diabetes mellitus (DM) on survival in PAH is unclear. Insulin resistance and DM are associated with left ventricular steatosis and dysfunction, but whether the right ventricle (RV) might be affected by DM in PAH is unknown. We hypothesized that PAH patients with DM would have worse survival than PAH patients without DM and that this would be due to impaired RV compensation. From a large registry of PAH patients at our institution, we analyzed the effect of DM on survival in patients with idiopathic or heritable PAH. Clinical and hemodynamic differences were compared between PAH patients with DM and those without DM. Twenty-nine patients with DM and 84 without DM were included. Gender, body mass index, PAH type and duration, and 6-minute walk distance were similar between groups. PAH patients with DM had significantly lower survival at 10 years than PAH patients without DM. Right atrial pressure, pulmonary arterial pressure, and cardiac output did not differ significantly between the two groups. However, right ventricular stroke work index (RVSWI) was lower in the PAH DM group than in the no-DM patients. Among PAH patients with DM, patients who died had a lower RVSWI than survivors. In conclusion, survival in PAH patients with DM was reduced compared to that of patients without DM; impaired RV compensation may underlie this finding. Further study is needed to understand this effect.
INTRODUCTION
Pulmonary arterial hypertension (PAH) is a rare disease characterized by remodeling and obliteration of the pulmonary vasculature, which in turn leads to progressive right ventricular (RV) dysfunction and death.1,2 While there have been major advances in the knowledge of the pathogenesis3,4 and treatment5–7 of the disease, PAH still carries a very high rate of morbidity and mortality. 8 Recent data have begun to highlight patient subpopulations at particularly high risk of death, including older patients, men, and those with connective tissue disease; 9 however, the impact of comorbid conditions such as hyperlipidemia and diabetes mellitus (DM) on the prognosis of PAH is an area of debate. If these common medical conditions are demonstrated to alter disease progression or survival, then aggressive therapy with already-approved medications may offer potential improvements in PAH-related outcomes.
Previous work has shown high rates of glucose intolerance and insulin resistance in patients with PAH.10,11 However, there are at present conflicting data on the impact of DM on survival in patients with pulmonary arterial hypertension.9–12 Animal and cell culture models have suggested that insulin resistance plays a role in promotion of pulmonary vascular disease and is likely not just a bystander signifying end-stage PAH.13–15 Alternatively, insulin resistance and DM are associated with left ventricular steatosis and left heart dysfunction; the impact of these disorders of glucose homestasis on RV function is unknown.
We hypothesized that idiopathic- and heritable-PAH (IPAH and HPAH, respectively) patients with DM would have worse survival than their PAH counterparts without DM. We used a large single-center registry of PAH patients to determine whether the presence of DM in PAH patients affects mortality. We further explored a potential negative impact of DM on RV compensation, using invasive hemodynamic measures.
METHODS
PAH patients
This study was approved by the Institutional Review Board at Vanderbilt University Medical Center (IRB no. 9401). We utilized data collected in a registry of PAH patients seen at our institution, the Vanderbilt University Pulmonary Hypertension Research Cohort (VPHRC), that has been previously described.16,17 Study data were collected and managed with the REDCap electronic data capture tool hosted at Vanderbilt University. 18
For the purposes of our study, patients were included only if they carried a diagnosis of HPAH or IPAH. 2 PAH was diagnosed according to consensus criteria, 6 including a mean pulmonary artery pressure of ≥25 mmHg and a pulmonary capillary wedge pressure (PWP) of ≤15 mmHg. IPAH or HPAH were diagnosed by experienced clinicians according to consensus guidelines. 2 Patients with HPAH had at least one confirmed family member within their bloodline with PAH. The VPHRC includes subjects not directly treated for clinical care at Vanderbilt University. For those subjects with PAH followed externally, diagnostic data were reviewed by clinicians at Vanderbilt University to confirm the diagnosis and type of PAH. To avoid confounding by treatment era, cases were restricted to those with diagnostic hemodynamic and clinical data between January 1,1996 (when intravenous epoprostenol became commercially available), and March 1, 2011. Because this is an observational study, treatment decisions were at the discretion of the attending physician and not dictated by the study.
Demographic data, as well as data regarding patients' comorbidities—such as systemic hypertension and coronary artery disease (CAD)—at the time of PAH diagnosis, were also collected and recorded. For the purposes of our study, patients were defined as having systemic hypertension if they (1) had a blood pressure greater than 140/90 mmHg, (2) were on a Food and Drug Administration (FDA)–lapproved medication for hypertension, or (3) had a diagnosis of hypertension listed in the medical record. Likewise, hyperlipidemia was recorded if patients were on a medication to treat hyperlipidemia or if hyperlipidemia was listed in their past medical history. Patients were defined as having CAD if they had undergone coronary artery bypass grafting or percutaneous coronary intervention or if they had CAD listed in their past medical history.
From the diagnostic right heart catheterization, heart rate, systemic systolic and diastolic blood pressures, right atrial pressure, pulmonary artery pressures, PWP, cardiac output, and cardiac index (CI) were recorded. Stroke volume, pulmonary vascular resistance (PVR), pulmonary capacitance (PC), and RV stroke work index (RVSWI) were calculated according to standard formulas.17,19,20
DM definition
DM was defined as any of the following: random plasma glucose value of >200 mg/dL, self-reported diagnosis of DM, or treatment with an FDA-approved medication for DM. For the purposes of this analysis, patients with prediabetes, defined by glycosylated hemoglobin (HbA1c) of ≥6.0%,21,22 were considered to be in the DM group. Patients who met none of these criteria were defined as “no DM.”
Statistical analysis
Data are presented as mean ± standard deviation (SD) unless otherwise noted. Categorical variables were compared using the χ2 or Fisher exact test according to specifications. Continuous variables were analyzed with unpaired, 2-tailed Student's t tests. Values for 6-minute walk distance (6MWD), PWP, CI, and PVR were all compared via t tests. The primary endpoint was all-cause mortality, as it was not always possible to determine an exact cause of death. Survival curves were constructed according to the Kaplan-Meier method, with differences compared by the Gehan-Breslow-Wilcoxon test. Cox proportional-hazards regression, stratified for presence or absence of DM, was used to determine predictors of death in the cohort. Logistic regression analysis was performed to examine pre-specified predictors of death in the DM cohort (age, PVR, CI, and RVSWI). For all analyses, a P value of <0.05 was considered significant. All statistics were performed with GraphPad Prism and SPSS software (GraphPad Prism, ver. 5 for Mac, GraphPad Software, La Jolla, CA, www.graphpad.com; IBM SPSS Statistics, ver. 20 for Mac, IBM, Armonk, NY).
RESULTS
PAH characteristics
One hundred thirteen patients with IPAH or HPAH were identified from the registry. Of these, 29 were classified as having DM and 84 as no DM. Demographic data for the two groups are presented in Table 1. The study population was predominantly female, with relatively equal distributions of IPAH and HPAH between the two groups. At diagnosis there were no differences in comorbidities of systemic hypertension, hyperlipidemia, or CAD between the two groups. As expected, HbA1c was elevated in the patients with DM (P < 0.0001). Of the patients with diabetes, 15 (52%) received a diagnosis of DM before their diagnosis of PAH and 14 (48%) afterward. Of the patients with DM, 8 were on no medical therapy. Of the 21 patients treated with antidiabetics, 15 were taking biguanides, one thiazolidinedione, one glucagon-like peptide agonist, 6 dipeptidyl peptidase-4 inhibitors, and 11 insulin. Combination therapy was used in 11 patients. HbA1c data showed a mean value of 7.3% ± 2.4% in the diabetic patients. Although fasting glucose was not available in this cohort, the random plasma glucose value in the DM cohort was 136 ± 83 mg/dL.
Pulmonary arterial hypertension (PAH) patient characteristics
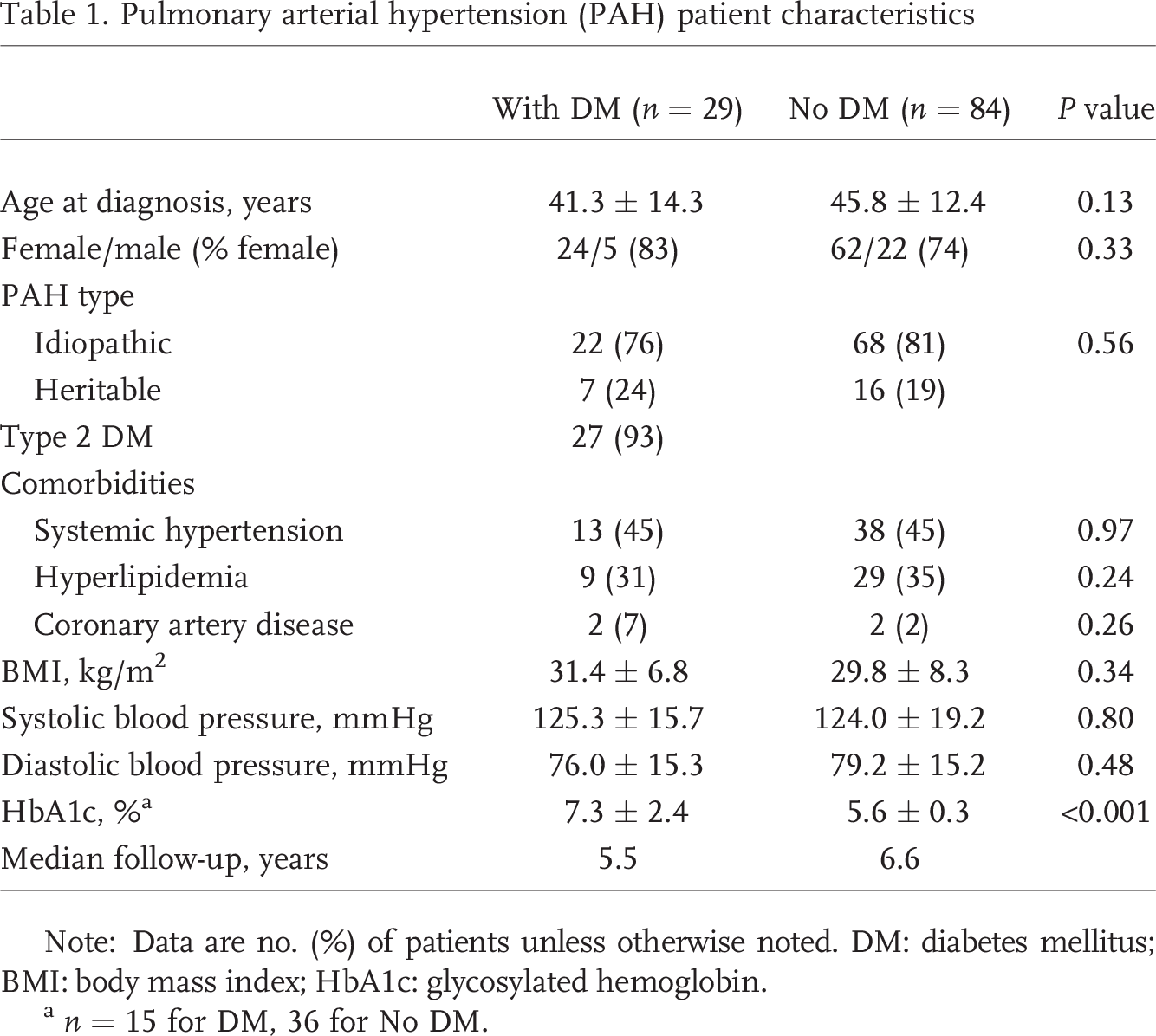
Note: Data are no. (%) of patients unless otherwise noted. DM: diabetes mellitus; BMI: body mass index; HbA1c: glycosylated hemoglobin.
n = 15 for DM, 36 for No DM.
There were no differences in PAH disease duration, treatment, or 6MWD between the patients with DM and those without (Table 2). Functional class was equally distributed between the two groups.
Pulmonary arterial hypertension (PAH) patient treatment and disease severity
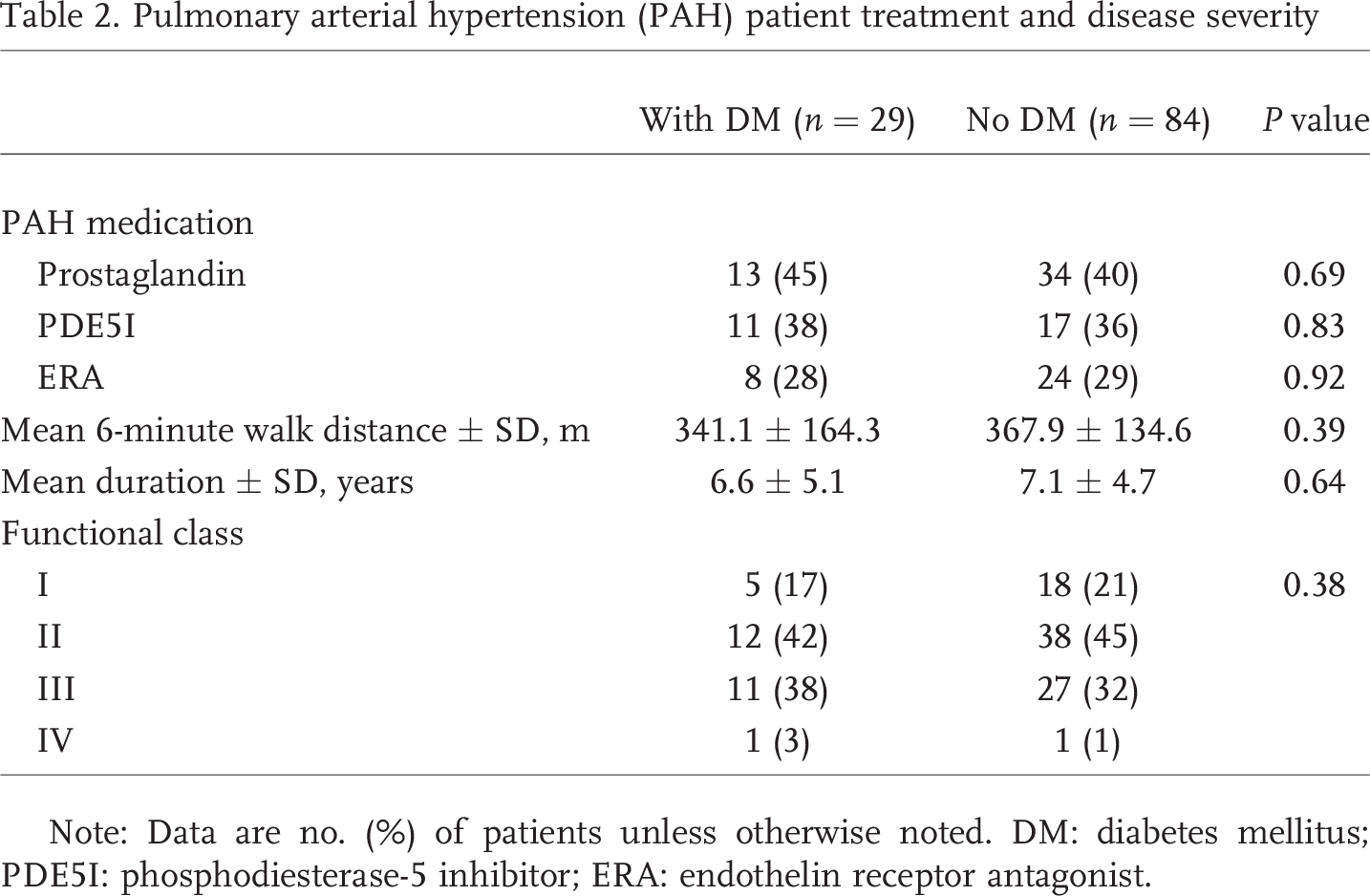
Note: Data are no. (%) of patients unless otherwise noted. DM: diabetes mellitus; PDE5I: phosphodiesterase-5 inhibitor; ERA: endothelin receptor antagonist.
Diagnostic right heart catheterization did not demonstrate any differences in conventional hemodynamics between patients with DM and those without (Table 3). There was a trend for higher right atrial pressure and lower PVR in the patients with diabetes, but this did not reach statistical significance.
Pulmonary arterial hypertension patient hemodynamics
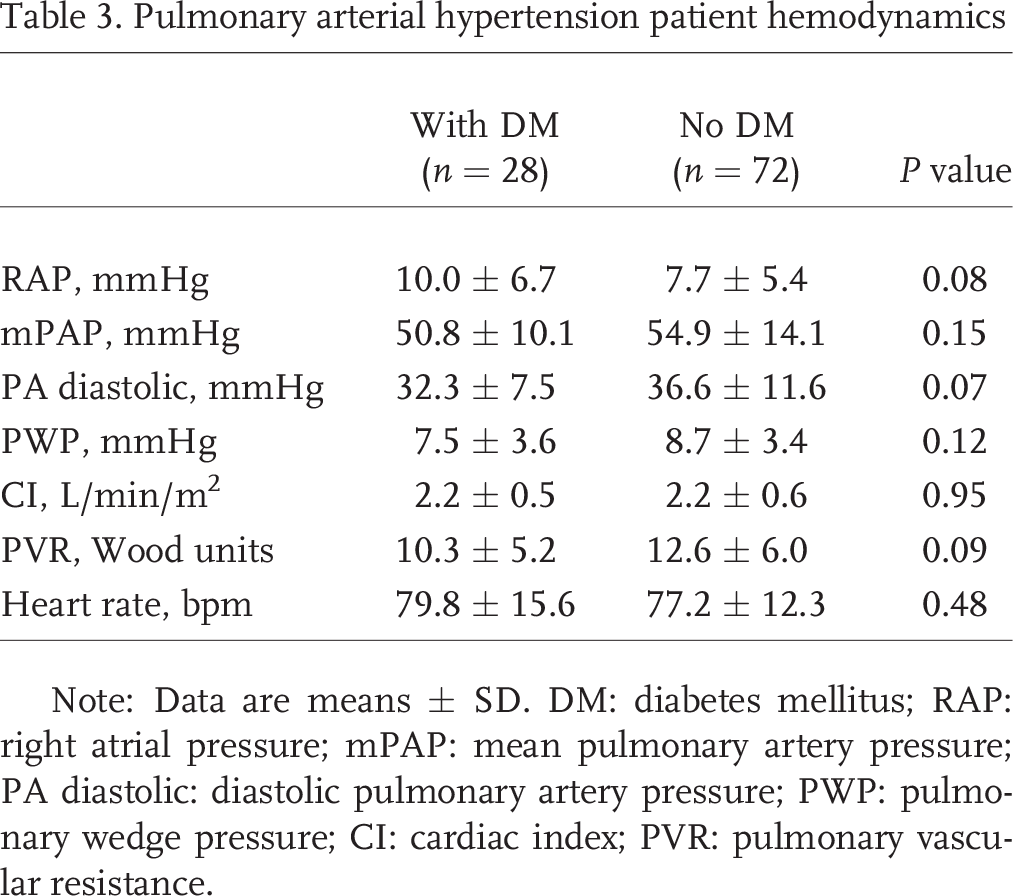
Note: Data are means ± SD. DM: diabetes mellitus; RAP: right atrial pressure; mPAP: mean pulmonary artery pressure; PA diastolic: diastolic pulmonary artery pressure; PWP: pulmonary wedge pressure; CI: cardiac index; PVR: pulmonary vascular resistance.
Survival analysis
During a median follow-up of 76 months, there were 15 deaths overall, 7 in the group with DM and 8 in the no-DM group. Kaplan-Meier survival analysis was performed on the cohort and is shown in Figure 1. No patients underwent lung transplant. Despite the lack of observed differences in demographics or traditional risk factors such as 6MWD, hemodynamics, or therapy, there was a significantly lower 10-year survival among PAH patients with DM, compared to their counterparts without DM (P = 0.04).
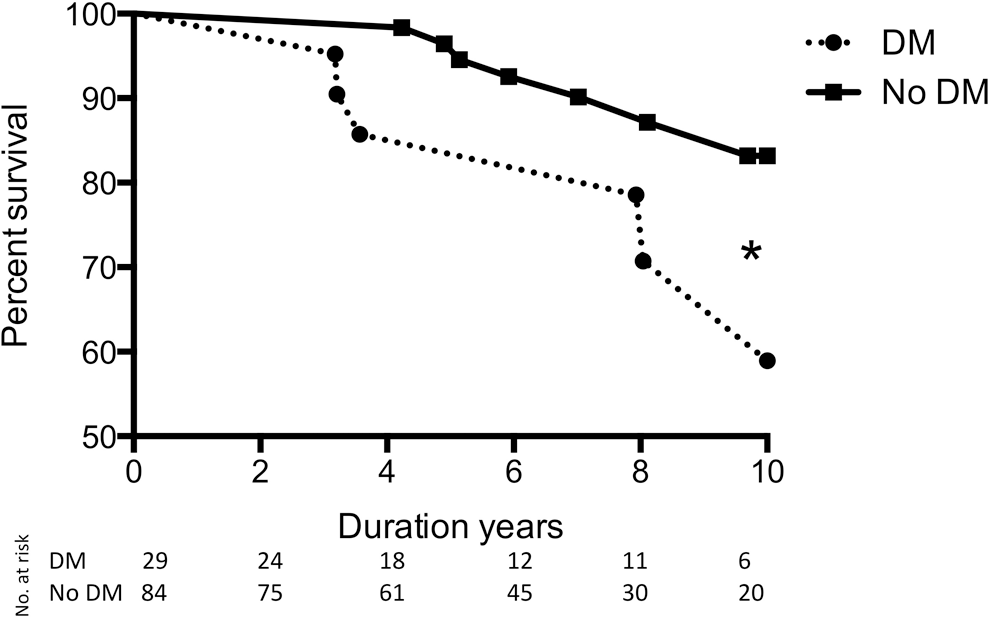
Survival analysis. Kaplan-Meier survival curves in pulmonary arterial hypertension patients with diabetes mellitus (DM) and without diabetes mellitus (No DM). P = 0.04.
RV function in diabetic PAH patients
Because traditional risk factors for mortality in PAH did not explain the observed mortality differences, we explored the hypothesis that RV dysfunction may underlie increased mortality in PAH patients with DM by examining RVSWI, a direct measure of RV work load (Fig. 2). In order to differentiate the effects of DM on the myocardium and the pulmonary vasculature, we examined PC as a composite measure of vascular resistance and elastic recoil. RVSWI was significantly lower in PAH patients with DM (15.26 ± 5.63 g m/m2/beat) than in those without (18.13 ± 7.01 g m/m2/beat; P = 0.03), suggesting impaired RV compensation in PAH patients with DM. There was, however, no significant difference in PC between patients with DM and those without DM (P = 0.33).
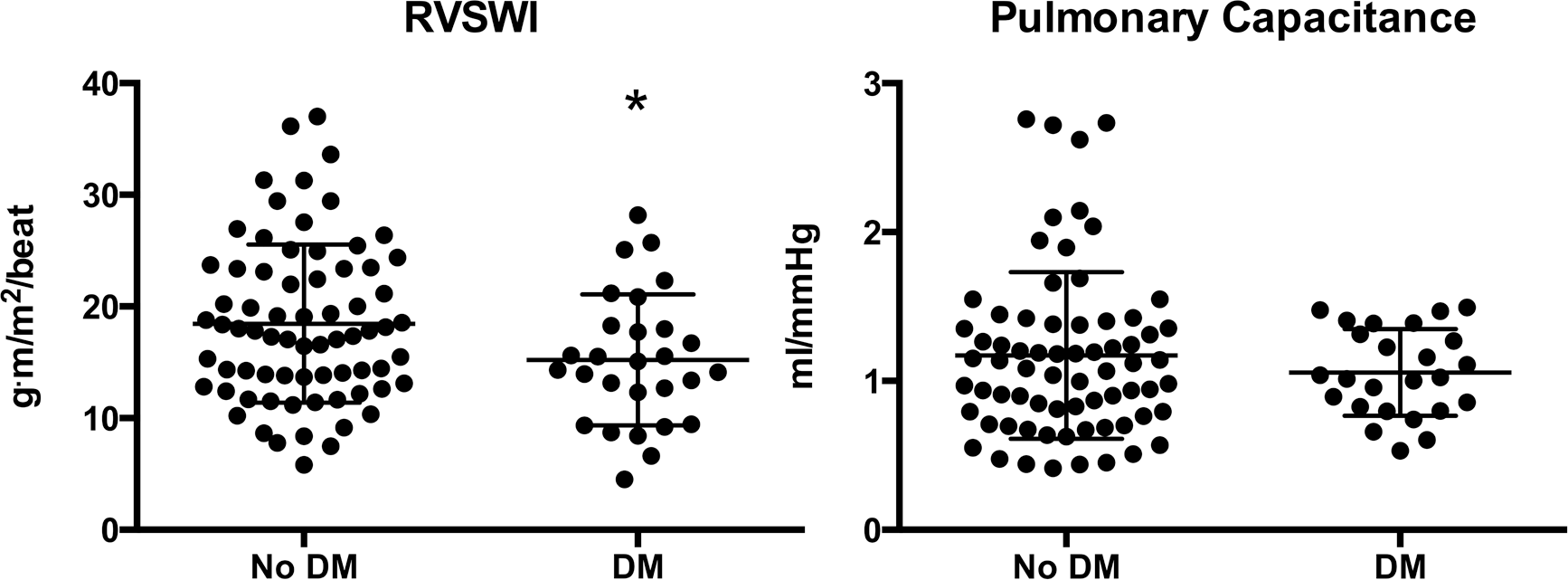
Right ventricular hemodynamic compensation. Right ventricular stroke work index (RVSWI) and pulmonary capacitance in pulmonary arterial hypertension patients with diabetes mellitus (DM) and without diabetes mellitus (No DM). RVSWI was significantly lower in patients with DM (asterisk; P = 0.03). No differences were observed between the two groups in pulmonary capacitance (P = 0.33). n = 28 (DM), 72 (nNo DM).
In the diabetic PAH patients specifically, RVSWI was lower in nonsurvivors than in survivors (P = 0.03; Fig. 3). There was, however, no difference in PC between survivors and nonsurvivors with DM (Fig. 4). There were no significant differences in either RVSWI or PC between nondiabetic patients who survived and those who did not, although the event rate was lower in this population.
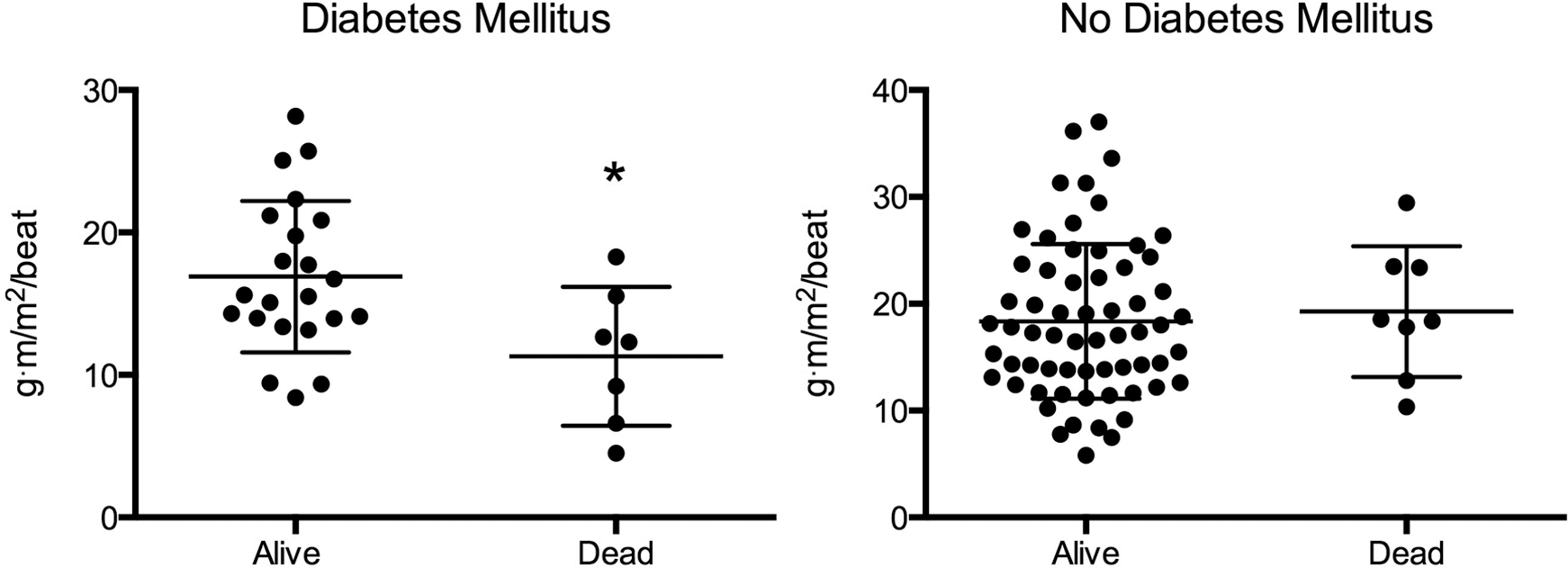
Right ventricular stroke work index in survivors and nonsurvivors among pulmonary arterial hypertension patients with and without diabetes mellitus (DM). Asterisk indicates P = 0.02. n = 22 DM alive, 7 DM dead, 63 no-DM alive, 8 no-DM dead.
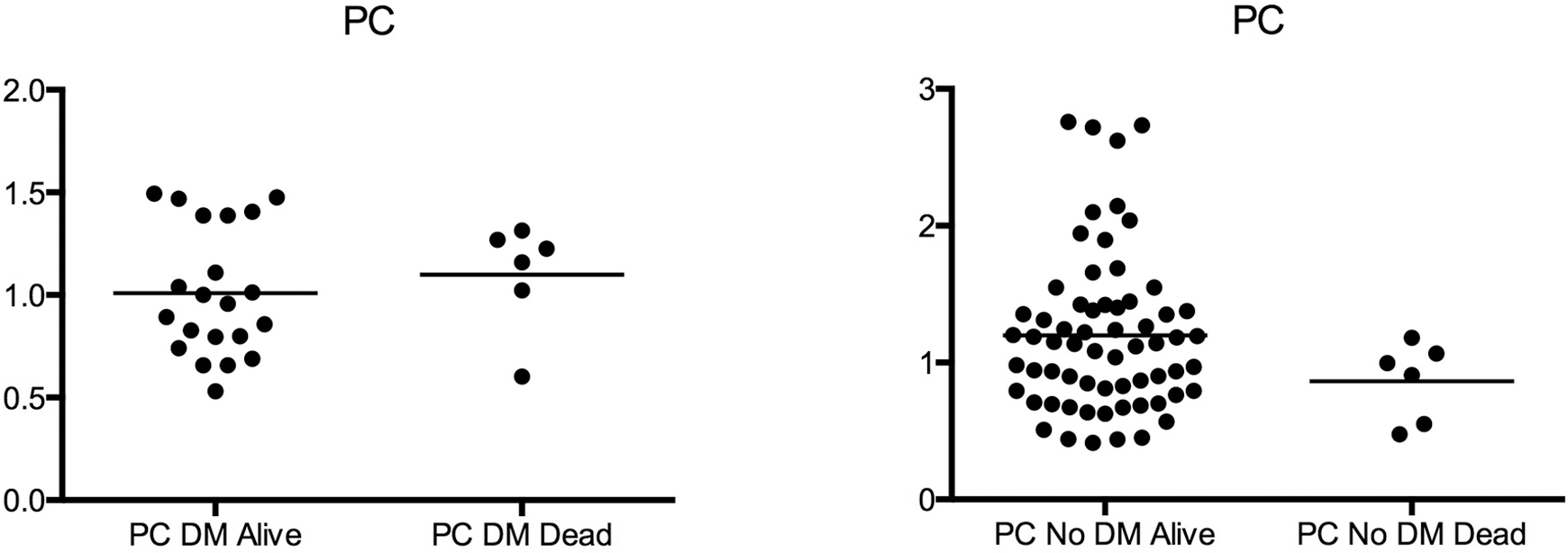
Pulmonary capacitance (PC) in survivors and nonsurvivors among pulmonary arterial hypertension patients with and without diabetes mellitus (DM and No-DM, respectively). No significant differences were found. n = 21 DM alive, 6 DM dead, 64 no-DM alive, 6 no-DM dead.
On the basis of clinical experience and prior publications,8,23,24 we examined the following variables' association with survival among the diabetic PAH patients: age, PVR, CI, and RVSWI. Age and PVR were not associated with survival, but higher RVSWI and higher CI were favorably associated with survival in the diabetic patients (P = 0.019 and 0.023, respectively; Table 4).
Variables associated with survival in diabetic pulmonary arterial hypertension patients
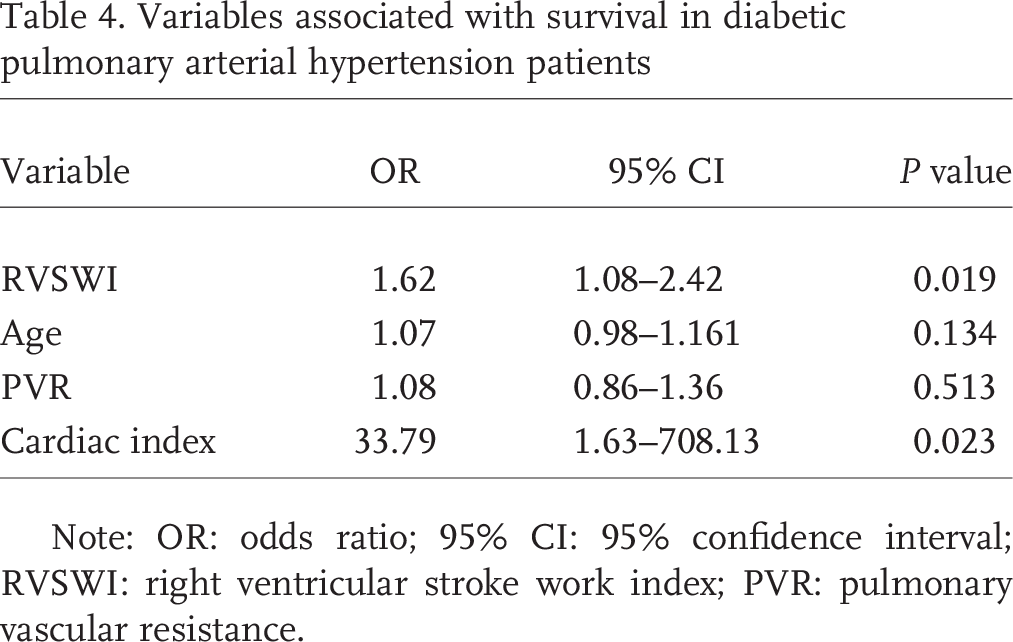
Note: OR: odds ratio; 95% CI: 95% confidence interval; RVSWI: right ventricular stroke work index; PVR: pulmonary vascular resistance.
DISCUSSION
In this study, we have demonstrated a significantly reduced 10-year survival in PAH patients with DM. Traditional markers of poor survival, such as demographics, reduced 6MWD, and standard hemodynamic markers of severity, were not different between PAH patients with diabetes and those without. Because RV function is a major determinant of survival in PAH, we examined RVSWI, an invasive hemodynamic measurement of RV workload. We found that RVSWI was lower in PAH patients with DM, which supports the hypothesis that RV function may be more impaired in the DM group.
Our data are in line with findings of other recent studies from our group and others that have investigated the interaction of DM and pulmonary vascular disease. We and others have demonstrated development and worsening of pulmonary vascular disease in mice after induction of insulin resistance.13,15 However, human data on the potential impact of DM on outcomes in patients with established PAH are less clear. Our prior data 11 showed a high prevalence of unrecognized glucose intolerance in PAH patients, but patients with known DM were excluded from that study analysis. Our present study showed no difference in short-term mortality between diabetic and nondiabetic PAH patients. Work by Zamanian and colleagues 10 has shown that insulin resistance, as measured by the triglyceride/high-density lipoprotein (HDL) ratio, is more prevalent in the PAH population than in the general population and is associated with a lower 6-month event-free survival. Again, PAH patients with known DM were not included. Finally, large-scale registry studies such as REVEAL (Registry to Evaluate Early and Long-Term Pulmonary Arterial Hypertension Disease Management) did not collect information, such as triglyceride/HDL ratio or HbA1C, that might identify undiagnosed DM in PAH patients. 25 Although REVEAL did record data regarding comorbid DM and has recently suggested that DM may negatively affect survival in PAH, 12 DM was not included in the REVEAL risk calculator, 9 perhaps suggesting that a more sensitive marker of insulin resistance or DM may be needed to define the true effect of altered glucose homeostasis on PAH outcomes.
Because there are emerging data that insulin resistance and DM may negatively affect myocardial function26,27 and because no traditional survival factors appeared to differ between PAH patients with DM and those without DM, we explored a possible association of worse RV function in PAH patients with DM. RVSWI is a composite measure of RV workload that may better reflect RV compensation than cardiac output in certain clinical settings.28–32 We have recently shown that RVSWI in PAH is closely associated with stroke volume, not heart rate, and thus likely is a metric of RV function in this disease. 33 It is interesting to note that both PAH populations, with and without DM, had supranormal values of RVSWI (normal range: 4–8 g m/m2/beat 34 ), reflecting necessary compensation for the increased load stress of PAH. However, we found that RVSWI was depressed in PAH patients with DM, compared to those without DM, and that higher RVSWI is associated with lower hazard of death in DM patients but not in PAH patients without DM. Further, in PAH patients with DM, RVSWI was lower in patients who died than in survivors. These data suggest that PAH patients with DM may be less able to compensate for pulmonary vascular disease–associated load stress. In contrast, we found no differences between PAH patients with and without DM in PC, a hemodynamic measure of the ability of the pulmonary vascular tree to dilate and store blood during RV systole and to then recoil and expel it during RV diastole that was previously shown to be an independent predictor of mortality in PAH. 35
There are limitations to our study. We did not include patients with connective tissue disease– or congenital heart disease–associated PAH, because these patients may be phenotypically different from IPAH or HPAH patients and DM may differentially affect survival in these conditions. We also stringently excluded patients with significant lung or left heart disease according to strict diagnostic criteria and thus lowered the total number of IPAH or HPAH patients that met our criteria. 36 This observational study incorporates data after diagnosis of PAH and thus cannot inform on the risk of PAH associated with DM. As the study was observational, we did not test the no-DM group for HbA1c or other markers of DM, and it is possible that some members of this group did have DM or insulin resistance. If true, however, this would bias toward the null hypothesis and thus strengthen our findings. We did not collect data on the exact date of DM diagnosis in adequate numbers of patients to draw meaningful conclusions on the impact of duration of DM on PAH outcomes. Our study did not collect echocardiographic data on sufficient patients to translate our findings to noninvasive measures of RV function or to comment on possible effects of DM on left heart function, although all patients were required to have normal left ventricular ejection fraction in order to receive a diagnosis of PAH. There were relatively few events in the no-DM group, and cause of death is unknown for many, which limits our power for multivariate analysis. The mortality reported here in the no-DM group is relatively low but is likely similar to that experienced in other single-center registries with high rates of prostaglandin use 37 or favorable risk categories. 9
In conclusion, survival in IPAH and HPAH patients with DM is lower than that in PAH patients without DM. Differences in RV compensation may underlie these mortality differences. The results of this study raise further questions, specifically, how insulin resistance and DM may have a detrimental effect directly on the right ventricle. Future basic science efforts should be directed at understanding the impact of insulin resistance on RV function.
Footnotes
ACKNOWLEDGMENTS
The contents are solely the responsibility of the authors and do not necessarily represent official views of the National Center for Advancing Translational Sciences or the National Institutes of Health.
