Abstract
Pulmonary arterial hypertension (PAH) results from severe remodeling of the distal lung vessels leading irremediably to death through right ventricular (RV) failure. PAH (Group 1 of the World Health Organization classification of pulmonary hypertension) can be idiopathic (IPAH) or associated with other disorders, such as connective tissue diseases. Prominent among the latter is systemic sclerosis (SSc), a heterogeneous disorder characterized by endothelium dysfunction, dysregulation of fibroblasts resulting in excessive collagen production, and immune abnormalities. For as-yet-unknown reasons, SSc-associated PAH (SSc-PAH) carries a significantly worse prognosis compared with any other form of PAH in Group 1, including IPAH. We have previously shown that patients with SSc-PAH have a median survival of only 3 years, compared with 8 years for IPAH, despite modern PAH therapy. Because death is principally due to RV failure, we speculated that RV adaptation to PAH differed between the two entities due to disparate pulmonary artery loading, perhaps from vessel stiffening, or intrinsic RV myocardial disease that might limit function and adaptation to high afterload. In SSc, RV function may also be impaired by inflammatory processes, excess fibrosis of the myocardium, or altered angiogenesis, which may all contribute to impaired contractile reserve exacerbating cardiopulmonary impedance mismatch. This is now suggested by recent findings from our group that demonstrate that, although pulmonary vascular load may be similar between patients with IPAH and those with SSc-PAH, the latter display reduced myocardial contractility as assessed by pressure-volume loop measurements. This review focuses on fundamental hemodynamic, structural, and functional differences in RV from patients with SSc-PAH compared with IPAH, which may account for survival discrepancies between the two populations. Possible underlying basic mechanisms are discussed.
Pulmonary arterial hypertension (PAH) is a leading cause of mortality in patients with systemic sclerosis (SSc), a heterogeneous disorder characterized by dysfunction of the endothelium, dysregulation of fibroblasts resulting in excessive production of collagen, and abnormalities of the immune system. PAH leads almost uniformly to death through right ventricular (RV) failure. However, for reasons that remain unclear, SSc-associated PAH (SSc-PAH) carries a significantly worse prognosis compared with any other form of PAH in Group 1 of the pulmonary hypertension classification. 1 Indeed, we and others have shown that patients with SSc-PAH are four times more likely to die than patients with idiopathic PAH (IPAH) and have a median survival of only 3 years, compared with 8 years for IPAH, despite modern PAH therapy.2,3 From a broad perspective, a disparate RV adaptation to PAH between these two entities could actually result from a greater load, perhaps due to pulmonary arterial stiffening, as reported in systemic arteries. Alternatively, the RV myocardium could be diseased, limiting function and its adaptive capacity to afterload. SSc may also impair reserve mechanisms, exacerbating cardiopulmonary impedance mismatch and thus limiting functional capacity.
We have recently identified specific prognostic factors in patients with SSc-PAH, which all reflect RV performance, including tricuspid systolic plane excursion (TAPSE), 4 stroke volume index, and stroke volume/pulse pressure, 5 and have further recently demonstrated alterations in intrinsic RV myocardial contractility in these patients. 6 These observations raise several important questions focused essentially on RV function in SSc-PAH: (a) Does the RV in SSc-PAH versus IPAH respond differently to physiologic stress? (b) What molecular/cellular mechanisms may underlie cardiac limitations in PAH? (c) Are myocardial abnormalities present with SSc alone or do they require PAH?
PULMONARY HYPERTENSION AND SYSTEMIC SCLEROSIS: MAGNITUDE OF THE PROBLEM
PAH (defined as a mean pulmonary artery pressure [mPAP] >25 mmHg with pulmonary capillary wedge pressure <15 mmHg), 7 is a progressive disorder of the pulmonary vasculature characterized by obliteration of the distal vessels and leading to RV failure and death. 8 Among its causes, patients with SSc have a particularly poor prognosis. PAH affects 10%–12%9,10 of patients with SSc and is a leading cause of death associated with SSc. 11 The prevalence of SSc-PAH in the United States may be as high as 24 cases per million, nearly fourfold greater than the prevalence of IPAH, 12 with many patients likely underrecognized. 7 SSc-PAH is associated with a mortality rate fourfold higher than that of IPAH despite seemingly being associated with less severe hemodynamic impairment as assessed by traditional methods. 3 RV failure5,13,14 is a major cause of PAH-associated mortality, raising the hypothesis that the SSc RV may have underlying disease rendering it particularly vulnerable to PAH. However, characterization of RV function in PAH in general, and SSc-PAH more specifically, remains very limited. Data from tissue-Doppler echocardiography and cardiac magnetic resonance imaging (cMRI) parameters have shown subtle changes, although overall RV (and left ventricle [LV]) function appears similar between SSc-PAH and IPAH.2,3 In fact, information regarding what may be wrong in SSc myocardium, the RV more generally with PAH, and how this impacts not only rest function but also physiologic reserve, is critically lacking.
Pathogenesis of vascular changes and injury in scleroderma
Some clues for myocardial disease pathophysiology in SSc-PAH come from vascular disease with changes in pulmonary vessels with SSc-PAH, and systemic vessels with SSc more generally. In the lung, SSc-PAH shares many similarities with IPAH, including intimal hyperplasia, medial hypertrophy, adventitial fibrosis, small vessel concentric obliteration, and angioproliferative lesions. SSc-PAH has fewer plexiform lesions, more intimal fibrosis, more venoocclusive disease,15,16 and more heterogeneity 15 versus IPAH. SSc alone displays endothelial apoptosis with activation and expression of adhesion molecules, inflammatory cells, and a procoagulant state with intimal proliferation and adventitial fibrosis.17–20 Autoimmunity involving antifibrillarin and antiendothelial cell antibodies, which stimulate cell adhesion and apoptosis,21,22 and antifibroblast antibodies, which induce proinflammatory/fibrotic responses linked to cytokines and growth factors, 23 enhancing collagen synthesis,24,25 is present in both SSc-PAH and IPAH. Lastly, circulating factors (e.g., soluble vascular cell adhesion molecule, vascular endothelial growth factor, and angiostatic factors) are observed in SSc, suggesting endothelial injury 26 and abnormal angiogenesis,27–31 and may play a key role in SSc-PAH.32,33 Growing evidence for proper myocyte-microvascular crosstalk as an essential component of ventricular compensation to load further supports a link between these changes and RV function. Together, these data suggest a prominent role for inflammation, autoimmunity, and dysregulated angiogenesis in PAH and SSc-PAH pathogenesis.
Prevalence of primary cardiac involvement in scleroderma
The prevalence of primary cardiac involvement in patients with SSc is most likely underestimated because of multiple factors that include the occult nature of signs and symptoms, frequent coexistence of lung involvement, and the relative inaccuracy of diagnostic procedures. In a meta-analysis, the prevalence of clinically evident cardiac disease in SSc was 10%, 34 whereas autopsy studies report extensive cardiac involvement in over half of patients with SSc. 35 However, more sophisticated imaging techniques and the search for subclinical cardiac involvement in patients with SSc have resulted in prevalence figures close to and even higher than those reported in autopsy studies. 36
Several cardiac abnormalities affecting all layers of the heart (endocardium, myocardium, and pericardium) as well as the conduction system have been observed in patients with SSc in the absence of coexisting systemic or pulmonary hypertension. Alterations include myositis, pericardial effusion and fibrosis, arrhythmias, left ventricular systolic and diastolic dysfunction, right heart failure, and perfusion abnormalities. 37 Focal fibrosis involving the myocardium and extending to the pericardium, typically the predominant pathologic finding,38,39 can also involve the conduction system resulting in various degrees of heart block and atrial and ventricular arrhythmias. Whether fibrosis contributes to the relatively high prevalence of systolic or diastolic dysfunction in this population is unclear at this time.
Atherosclerosis, thought to be a chronic inflammatory disorder, may be more common or may be accelerated in autoimmune rheumatic diseases. Although increased prevalence of coronary artery disease in patients with SSc 40 remains quite controversial, atherosclerosis and/or fibrosis may result in excessive stiffness of the proximal pulmonary arteries in SSc, thus theoretically contributing somewhat to RV-pulmonary vascular uncoupling.
Taken together, these findings suggest that cardiovascular involvement in SSc is most likely multifactorial, originating from micro or macro vascular disease with subsequent inflammation and fibrosis and resulting in systolic and diastolic dysfunction, conduction alterations, and possible RV-pulmonary vascular uncoupling in situations of increased pulmonary vascular load, such as in pulmonary hypertension.
Predicting survival in scleroderma-associated PAH: limitation of traditional RV performance indexes
Despite improvements in PAH therapies and their efficacy for other PAH-associated diseases, median survival for SSc-PAH remains dismal at less than 4 years,3,9,41–43 compared with 8 years for IPAH. The capacity of the RV to adapt to increased pulmonary vascular load is the overwhelming determinant of survival in PAH. 44 However, we and others have shown that traditional hemodynamic measures of disease severity, such as cardiac index and right atrial pressure (RAP), both strongly predicting survival in IPAH, 13 are weaker predictors of outcome in SSc-PAH.3,5,41 Using RV pressure-volume relations, our group has recently shown that a major difference between IPAH and SSc-PAH resides in depressed RV performance rather than greater pulmonary afterload in SSc-PAH (vide infra). 6 RV dysfunction may only manifest when PA-vascular load is enhanced (such as in pulmonary hypertension), because the latter itself predicts SSc-PAH survival 5 , but underlying this is likely the ability of the RV to remodel. Unfortunately, understanding of RV function and functional reserve currently remains extremely limited, whether measured invasively or noninvasively. The latter is ultimately essential to follow patients chronically and to predict risk and therapeutic response. Echocardiography is a standard screening tool for PAH, but it has serious limitations. Routine measurements, such as right atrial size, septal displacement (i.e., eccentricity index), and pericardial effusion, have limited value in PAH45,46 and limited value for SSc-PAH. We have shown that TAPSE is a systolic measure that has proven useful to assess RV performance in PAH 47 and SSc-PAH, 4 although it is impacted by load and structure. Rigorous prospective assessment of noninvasive markers of RV performance in PAH, particularly SSc-PAH, is lacking. New measures based on cMRI are showing promise48–51 but have been little studied in the United States beyond recent work from our group and others52–55 and have not yet been applied in a prospective manner to test risk assessment and differentiation of SSc-PAH and IPAH.
NONINVASIVE ASSESSMENT OF THE HEART IN SCLERODERMA
Transthoracic echocardiography (TTE)
TTE, by far the most widely available imaging modality, provides estimates of pulmonary artery pressures and of RV structural changes, such as hypertrophy, and RV overload (e.g., RV dilatation and septal wall motion abnormalities). In a study of patients with SSc, two-thirds were found to have abnormalities such as elevated RV systolic pressure, pericardial effusion, increased RV dimensions, and left atrial enlargement. 56 In a larger cohort of several hundred patients with SSc, PAH was suspected in 33 patients but was confirmed by right heart catheterization (RHC) in only 18 patients. 57 LV systolic dysfunction was only observed in a small minority of patients, whereas LV diastolic dysfunction was much more common. Other abnormalities, including mitral regurgitation, aortic regurgitation, and aortic stenosis, were found in relatively few patients. Using transthoracic contrast-enhanced echocardiography with adenosine infusion 58 and dobutamine stress echocardiograph, 59 decreased LV coronary artery reserve was also detected in patients with SSc.
We previously examined demographic characteristics and hemodynamic, echocardiographic, and survival differences between two cohorts of patients with IPAH and with SSc-PAH. 3 Regarding echocardiographic parameters, we found that both groups had a similar prevalence of right-sided chamber enlargement. However, left chamber morphologic and functional abnormalities (diastolic dysfunction) were more common in patients with SSc-PAH despite normal LV systolic function. Left atrial dilation and size were also significantly more prevalent in the SSc-PAH group. Pericardial effusion was almost three times more common among patients with SSc-PAH than among patients with IPAH (34.7% vs. 13.2%; P < 0:05). The presence of pericardial effusion portended a poor survival in both groups.
The Tei index (or myocardial performance index), the sum of the isovolumetric contraction and relaxation times divided by ejection time, 60 has been used as a measure of RV performance. Patients with pulmonary hypertension have increased isovolumetric contraction and relaxation times and a decreased ejection time. In combination with standard TTE measures of pulmonary artery pressure, a Tei index >0.36 was found to be more highly predictive of PAH in patients with SSc. 61
TAPSE, another simple measure of global RV performance that can be obtained with TTE, has the advantage of being independent from the RV complex geometry, although it is dependent on load. In PAH, TAPSE measurements correlate with RHC parameters and predict survival. 47 We have recently demonstrated that, for a similar pulmonary afterload, patients with SSc-PAH have significantly lower TAPSE measurements, compared with patients with IPAH, and worse survival, again indicating a poor RV performance for this population irrespective of afterload. 62 For both patients with IPAH and patients with SSc-PAH, as well as other patients with PAH, the use of these imaging studies as outcome measures in response to pharmacologic interventions has yet to be adequately evaluated.
Tissue Doppler and Doppler strain imaging
Tissue Doppler imaging (TDI) allows echocardiographic measurement of myocardial velocities for determination of global as well as segmental systolic and diastolic ventricular dysfunction. 63 Originally developed for LV assessment, this technique is gaining momentum for assessment of RV function. Although TDI has many advantages over conventional Doppler for assessment of myocardial performance indices, its major drawback is that nonfunctioning segments may be overlooked due to interdependence with functioning segments. 64 In contrast, Doppler strain imaging allows for examination of segmental deformation regardless of normal surrounding segments. 64 Therefore, the addition of TDI and Doppler strain and strain rate imaging to standard TTE provides additional information; TDI detects abnormalities not shown on TTE, and strain imaging finds discrepancies not found on TDI. As an example, comparison of patients with SSc with control subjects via standard TTE showed no LV or RV systolic dysfunction, a decreased E/A ratio suggestive of diastolic dysfunction, but no difference in RV isovolumetric relaxation time (an additional measure of diastolic dysfunction). 65 TDI findings confirmed a decrease in early diastolic velocity to myocardial atrial diastolic wave (Em/Am) consistent with diastolic dysfunction of the RV lateral wall. Additionally, myocardial relaxation time was increased in patients with SSc, which provided more support for RV diastolic dysfunction in this RV segment. Strain imaging was able to detect abnormalities in both LV and RV systolic motions with decreased strain rates in the middle and basal segments of the LV free wall and decreased strain rates in the RV free wall basal, middle, and apical segments. 65 Furthermore, Kepez et al. 66 showed that patients with SSc without pulmonary hypertension or overt clinical cardiac involvement had reduced myocardial strain and strain rate despite normal 2D, conventional Doppler, and TDI velocity measurements. Strain and strain rate imaging are thus promising new sensitive and accurate modalities to evaluate patients with SSc for early cardiac involvement.
Nuclear imaging
Nuclear imaging may be helpful in assessing the heart in the early stages of SSc. Radionuclide imaging with 99mTc ventriculography demonstrates a significant decrease in RV ejection fraction in patients with SSc (in the absence of PAH) when compared with control subjects, 67 whereas thalium 201 scintigraphy and single-photon emission tomography demonstrate reversible myocardial perfusion defects induced by cold stimulus or exercise almost uniformly in patients with SSc.68,69 Patients with SSc and myocardial perfusion defects have a specific phenotype with diffuse rather than limited scleroderma, positive anti-Scl70 antibody, more extensive and rapid progression of skin involvement, and a trend toward longer disease duration and greater severity.69,70 One study determined that thallium perfusion defect scoring was the single most powerful predictor of both mortality and subsequent development of clinical cardiac disease in patients with either limited or diffuse scleroderma. 71 Clearly, more is to be learned from these imaging modalities.
cMRI
cMRI has become the gold standard for quantitative evaluation of RV function and structural changes; it allows accurate and reproducible measurements of ventricular dimensions, wall thickness, and myocardial mass without relying on geometric assumptions. It enables precise analysis of the different patterns of heart involvement in SSc by differentiating morphological, functional, perfusion, and delayed contrast enhancement abnormalities. Compared with other imaging modalities, cMRI was more sensitive in detecting altered RV function in asymptomatic patients with SSc. 72 In another study, 75% of patients with SSc had at least one abnormality on cMRI, providing higher sensitivity compared with echocardiography. 73 Among the most commonly reported abnormalities are increased myocardial signal intensity in T2, altered LV and RV ejection fractions, LV diastolic dysfunction, LV kinetic abnormalities, RV dilatation, and pericardial effusion.
Delayed-enhancement cMRI can identify areas of ventricular fibrosis in SSc. 74 These areas have invariably a noncoronary midwall distribution and mostly involve the interventricular septum and the LV free wall. 75 cMRI also provides imaging of the coronary arteries and information regarding myocardial viability. Finally, cMRI can also be used to monitor therapeutic effects, which is an area of intense investigation at this time. For example, a recent report demonstrated that RV function (i.e., RV ejection fraction) assessed by cMRI was a strong predictor of survival in a cohort of patients with PAH followed up over time. 76
Taken together, these results suggest that cMRI is a reliable and sensitive technique to diagnose heart involvement in SSc and identify potential mechanisms, such as inflammation, fibrosis, and altered perfusion.
RECENT INSIGHTS INTO RV FUNCTION AND RV-PULMONARY VASCULAR COUPLING
Pulmonary vascular load and resistance-compliance relationship in PAH
We recently undertook a systematic analysis of pulmonary vascular loading in patients with PAH, based on recent reports from Vonk-Noordegraaf and colleagues,77,78 who found a consistent inverse dependence between pulmonary vascular resistance and compliance in small populations of patients with pulmonary hypertension. Our analysis assessed data from more than 1,000 patients with suspected or known precapillary PH (mean PA pressure, ≥25 mmHg; mean pulmonary capillary pressure, ≤15 mmHg) observed at Johns Hopkins over a 10-year period. 79 Clinical diagnoses included IPAH, SSc-PAH, interstitial lung disease, and chronic thromboembolic disease. Pulmonary vascular resistance (RPA, defined as mean PA-pulmonary capillary wedge pressure divided by cardiac output [CO]) and total pulmonary arterial compliance (CPA, defined as stroke volume divided by pulmonary artery pulse pressure) were plotted versus one another. Figure 1A shows the hyperbolic relation, CPA = 0.564/(0.047 + RPA), which was strikingly different from than that in the systemic circulation, where compliance varied over a broader range for any mean resistance (Fig. 1B, with pulmonary fit shown for comparison). In systemic vessels, the primary compliance resides in the thoracic aorta and is anatomically removed from the major source of resistance in peripheral vessels. However, in lung, the proximal PA provides far less compliance; estimates are 15%-20% of total compliance, 80 in contrast to 80%-85% from the aorta. Thus, pulmonary compliance is distributed peripherally in the lung, underlying tight coupling to RPA. The RPA × CPA product (time constant) defines the rate of diastolic arterial pressure decay, and the disparity between circulations is striking (Fig. 1C), with a near constant value for the pulmonary system, but marked dispersion in systemic vessels (P < 10−5).
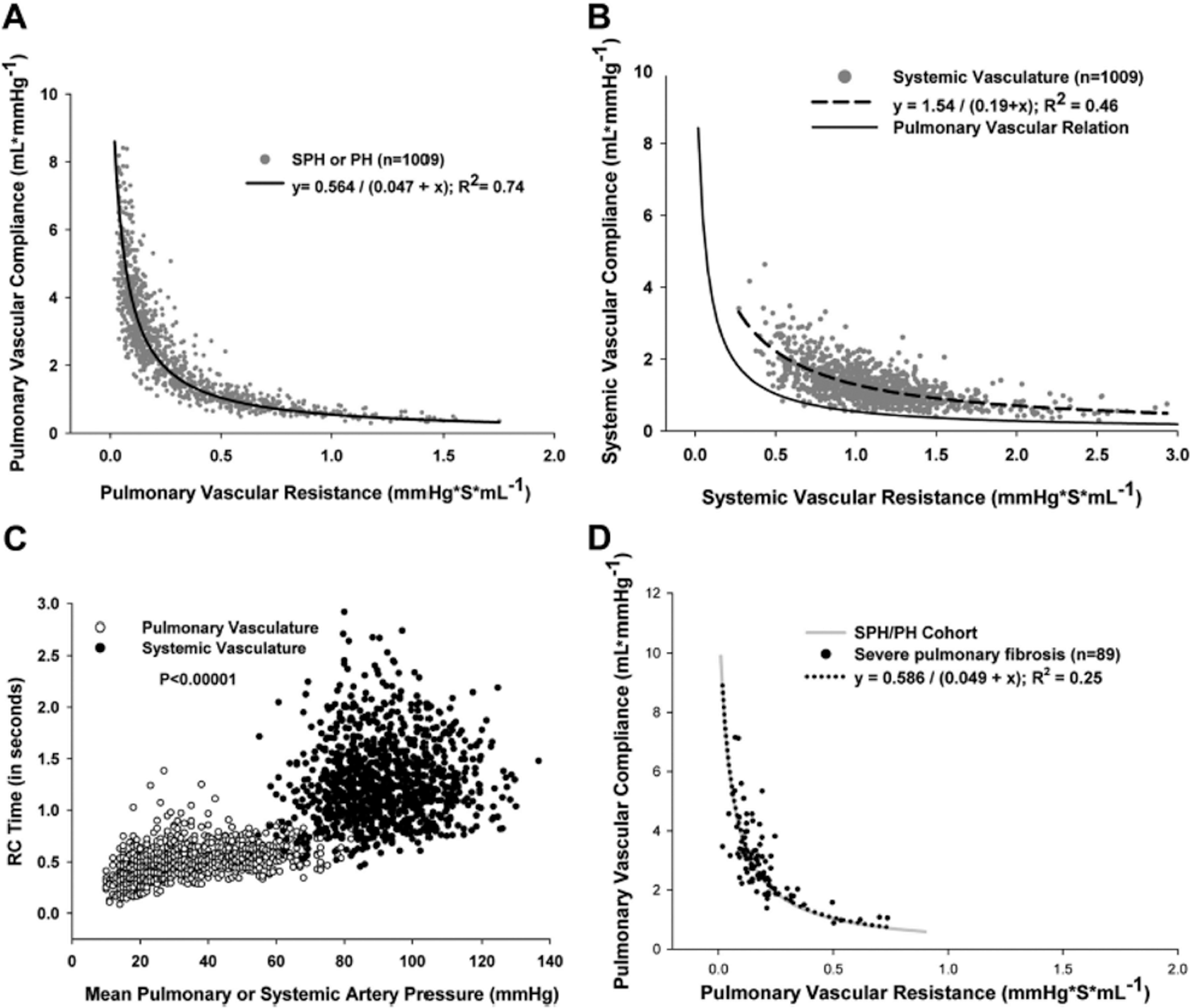
Pulmonary vascular resistance-compliance (RC) relationship (A) in the pulmonary circulation and (B) in the systemic circulation. C, Resistance-compliance product for the pulmonary and systemic vasculature plot against mean arterial pressure. D, Resistance-compliance relationship in patients with severe pulmonary fibrosis. SPH = secondary pulmonary hypertension; PH = pulmonary hypertension. Reproduced with permission from Tedford et al. 79
This analysis provided a novel yet simple way to test a key hypothesis regarding SSc-PAH, which we formulated several years ago: Is there greater PA stiffening in patients with scleroderma (due for instance to excess vascular fibrosis in this syndrome) that in turn augments total RV load, thus contributing to greater failure in this patient group? In a follow-up study, 6 we probed our database, identifying 67 patients with IPAH and 166 patients with SSc-PAH; both groups were predominantly female. SSc-PAH had slightly lower pulmonary pressures yet similar CO compared with patients with IPAH. Notably, NTpro-BNP levels were more than 2.5 times higher (as previously demonstrated for these patients) 81 and 6-minute walk test was lower in patients with SSc-PAH compared with IPAH. Mean CPA was slightly higher in patients with SSc-PAH, and the RPA-CPA plots for both groups were essentially superimposable (Fig. 2), with the same hyperbolic dependence observed in our larger group of patients with pulmonary hypertension (Fig. 1A). This study helped us to conclude with confidence that patients with SSc-PAH do not have lower total pulmonary compliance for a given mean resistive load 6 and that proximal pulmonary arterial stiffening is an unlikely contributing factor in the dismal prognosis observed in these patients.
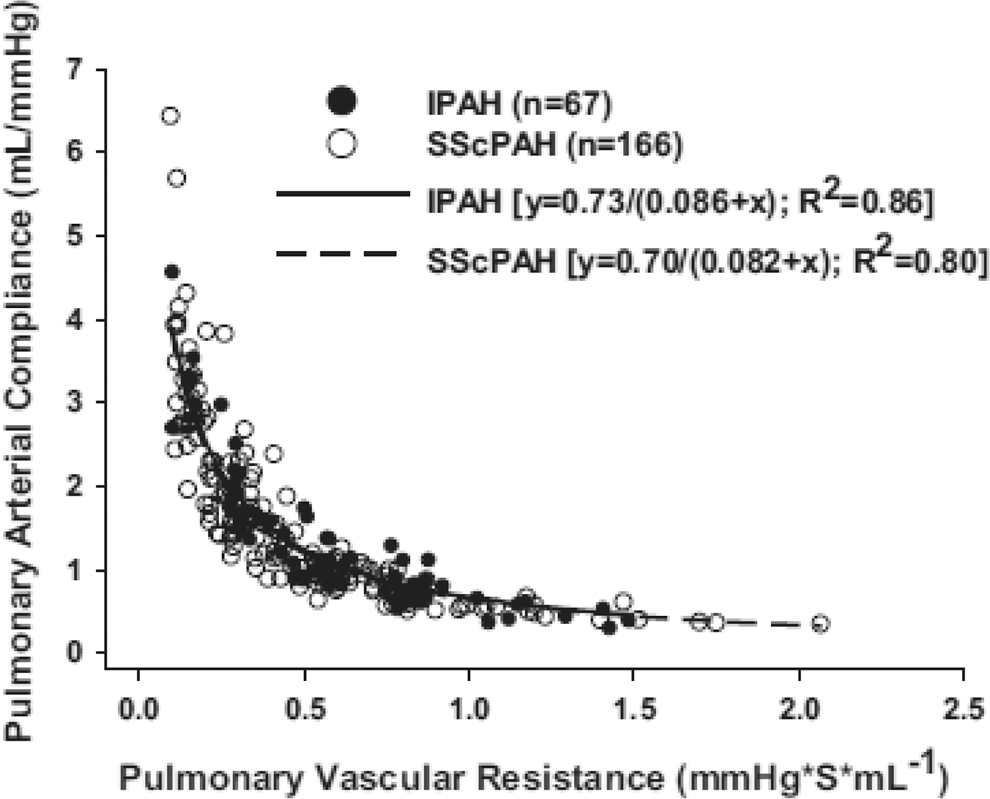
Pulmonary vascular resistance-compliance relationship in patients with systemic sclerosis–associated pulmonary arterial hypertension (SSc-PAH) versus patients with ideopathic pulmonary arterial hypertension (IPAH). Reproduced with permission from Tedford et al. 6
Intrinsic myocardial dysfunction in SSc-PAH versus IPAH
Because the disparate prognosis in patients with SSc-PAH could not be ascribable to differential pulmonary loading, we turned our attention to intrinsic myocardial function. We recently analyzed pulmonary artery pressures and mean flow in over 280 patients with pulmonary hypertension (patients with SSc with PAH or interstitial lung diseases–related PH and patients with IPAH) and found, as previously described, 6 an inverse relationship between RPA and CPA that was very similar for all three groups with a near constant RPA × CPA product. In addition, RV pressure volume loops were measured in a subset of patients with SSc-PAH and IPAH to derive contractile indices (end-systolic elastance [Ees] and measures of RV load such as arterial elastance [Ea] as well as RV-pulmonary arterial coupling [Ees/Ea]). 6 RV afterload was similar in this particular subgroup of patients with SSc-PAH and IPAH (approximately 7 Wood units, consistent with moderately severe PAH), although RV contractility (Ees) was significantly more depressed (Ees = 0.8 ± 0.3 vs. 2.3 ± 1.1; P < 0.01), and there was significantly more RV-pulmonary arterial uncoupling (Ees/Ea = 1.0 ± 0.5 vs. 2.1 ± 1.0; P = 0.03) in SSc-PAH compared with IPAH (Table 1). We concluded from this study that RV dysfunction is worse in SSc-PAH compared with IPAH at similar afterload and may be due to intrinsic systolic function rather than enhanced pulmonary vascular resistive and/or pulsatile loading. 6
Decreased intrinsic right ventricle (RV) contractility in patients with systemic sclerosis (SSc) and pulmonary arterial hypertension (PAH) compared with patients with ideopathic PAH (IPAH)
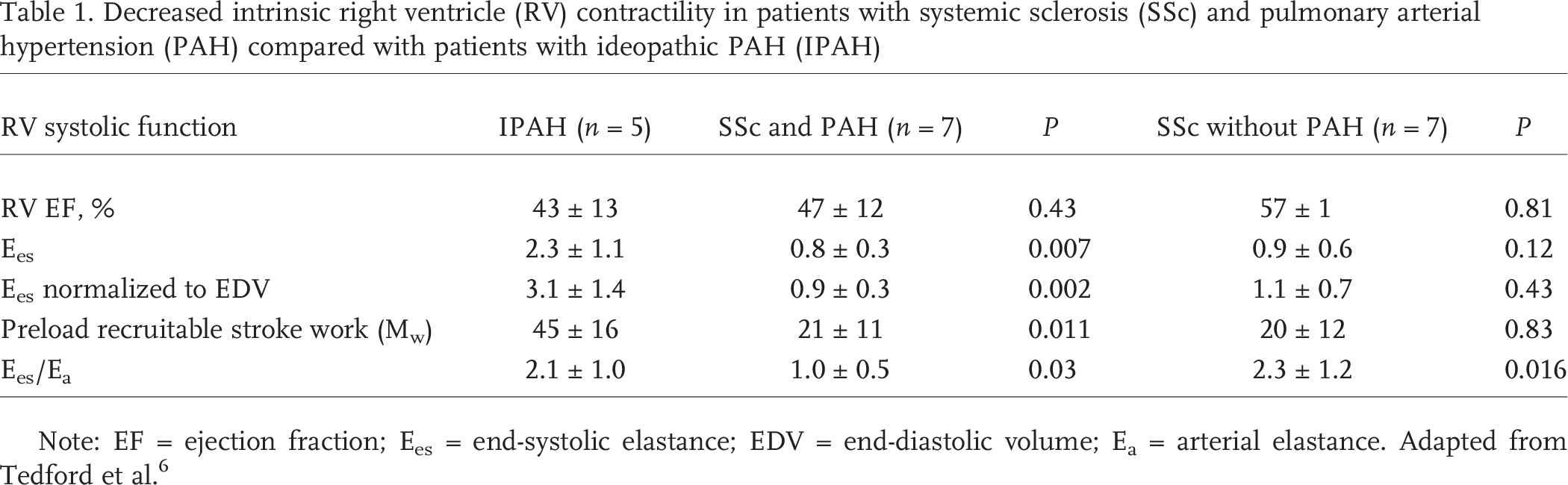
Note: EF = ejection fraction; Ees = end-systolic elastance; EDV = end-diastolic volume; Ea = arterial elastance. Adapted from Tedford et al. 6
Myocardial perfusion in SSc-PAH
Given the potential role of microvascular disease in PAH, and particularly SSc-PAH, as well as the potential worsened impact of high RV afterload, we recently assessed myocardial perfusion reserve (MPR) in 25 patients referred for PAH evaluation who underwent RHC and cMRI within a few hours of each other and compared them with healthy matched control subjects and patients with scleroderma in whom PAH was ruled out. The MPR indices (for both RV and LV) in the PAH group were significantly lower than those in the scleroderma non-PAH and control groups (Fig. 3A). 53 Furthermore, RV and LV MPR indices were inversely associated with mPAP (Fig. 3B) and RV stroke work index, as well as other measures of RV workload, systolic function, and remodeling (not shown). 53 These data suggest that reduced myocardial perfusion may contribute to poor RV performance in patients with PAH. The decrease in LV MPR index was also notable; we hypothesized that this was related to decreased coronary perfusion in PAH, as demonstrated by van Wolferen et al., 50 rather than a global decrease in CO, because there was no correlation between MPR index and CO. Alternatively, because the population we studied was overwhelmingly patients with SSc-PAH (18 patients with SSc-PAH vs. 6 patients with IPAH), we cautiously hypothesized that these findings could reflect myocardial microvascular disease, 53 which is prevalent in SSc, as suggested by others.82,83
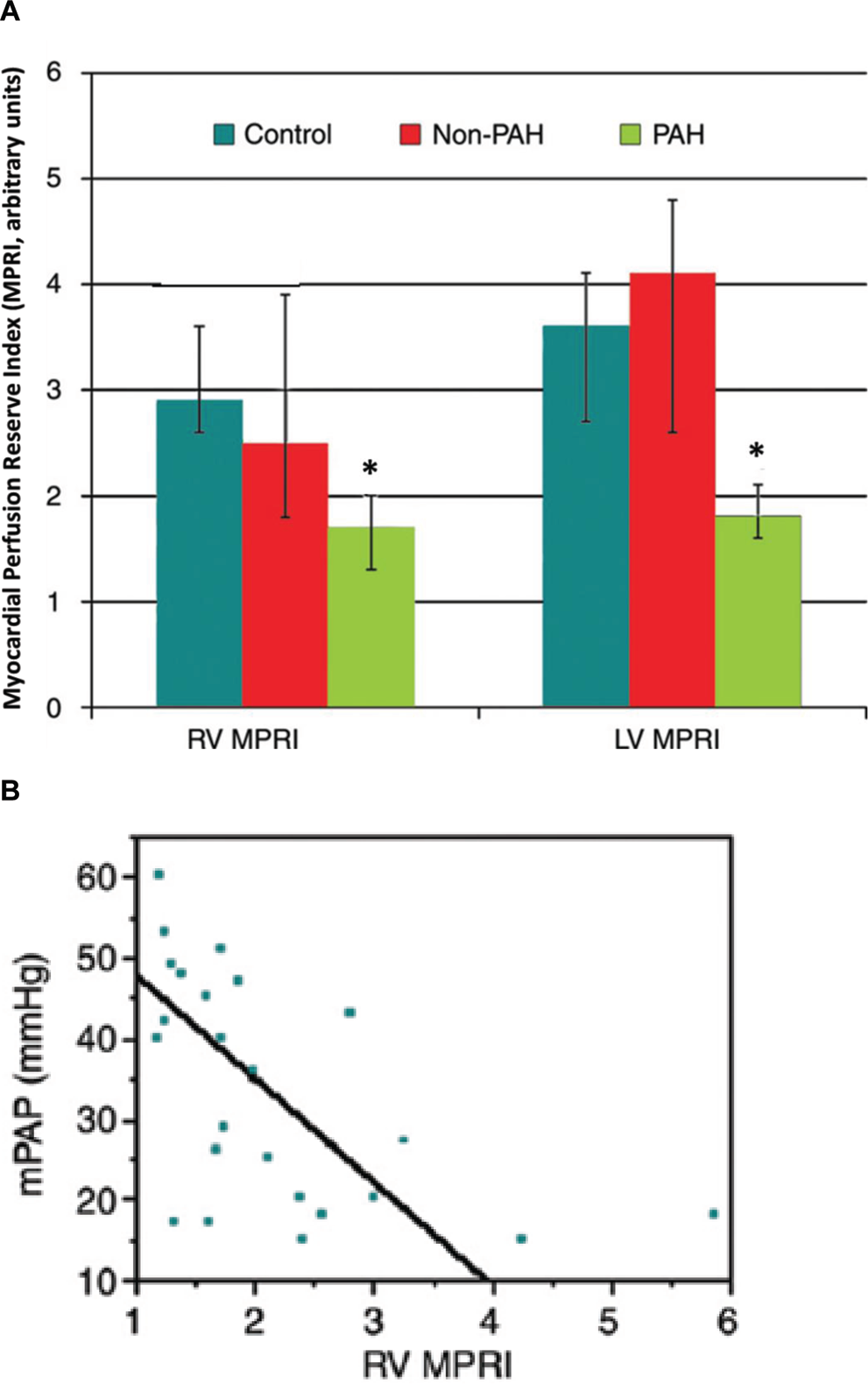
A, Right ventricle (RV) and left ventricle (LV) myocardial perfusion reserve index (MPRI) in control, non–pulmonary arterial hypertension (PAH), and PAH groups. Asterisk indicates P < 0.05 versus control group. There was no difference in RV MPRI between control subjects and patients with SSc but unconfirmed PAH (the non-PAH group). B, Relationship between mean pulmonary artery pressure (mPAP) and RV MPRI (ρ = −0.59; P = 0.036) in 25 patients with known or suspected PAH. A similar relationship was found with LV MPRI and between RV MPRI and RV mass and ventricle mass index (not shown). Reproduced with permission from Vogel-Claussen et al. 53 Copyright the Radiological Society of North America.
RV remodeling in PAH: distinct phenotype between IPAH and SSc-PAH
We recently examined 60 prospectively obtained cMRIs in 34 patients with SSc-PAH and 26 patients with IPAH, all of whom received a diagnosis by RHC. 84 Concomitant cMRI and RHC measurements were recorded for all patients. Regression analysis was used to assess the association between diagnosis and RV measurements after adjusting for age and RV load. There were no significant differences in unadjusted comparisons of cMRI measurements. Univariate regression showed RV mass index (RVMi) was linearly associated with measures of RV load. ANCOVA analysis showed a significant interaction between diagnosis and RVMi adjusting for pulmonary vascular resistance, age, sex, and treatment status (P = 0.024). RV end-diastolic volume index did not appear to be associated with measures of RV load, age, sex, or treatment status. This model showed a decreased amount of hypertrophy in the SSc-PAH group compared with patients with IPAH per unit increase in pulmonary vascular resistance. From this preliminary study, we concluded that RVMi varies linearly with measures of RV load. After adjusting for differences in RV load, age, and sex, patients with SSc-PAH demonstrated significantly decreased hypertrophy per unit increase in pulmonary vascular resistance. This difference in adaptive hypertrophy may, in part, explain poorer survival associated with SSc-PAH despite lower measures of load. The obvious limitations of this study include the cross-sectional nature of the study, the lack of repeated measures, and the overall small sample size. 84
Endomyocardial biopsy to unravel pathophysiological mechanisms in the failing RV in scleroderma
Endomyocardial biopsy has been used extensively in left heart failure for diagnosis of underlying pathologies and for routine assessment of cardiac rejection after transplantation. It is safe and may be used to detect cardiac involvement in patients with SSc. In addition, myocardial biopsies can be used in this patient population to exclude cardiac pathologies related to specific treatment (e.g., hydroxychloroquine) or complications (e.g., cardiac amyloid) and to distinguish between inflammatory and fibrotic forms of heart involvement in patients with SSc, which might lead to specific therapies. 85
In preliminary and unpublished results, our group performed RV biopsies for patients with heart failure with preserved ejection fraction (HFpEF), patients with scleroderma who were referred to our center for evaluation of PAH who turned out not to have PAH after RHC, and patients with SSc-PAH (with mild PAH as a start for safety purposes). We assessed capillary density and correlated these measurements with hemodynamic data. Capillaries were identified with immunohistochemical staining of the endothelium in cross section with endothelial specific antibodies against CD34. 86 Image acquisition and analysis of capillary density was done blinded to sample identifiers. The density of capillaries (capillaries number per 1 mm 2 ) was assessed and quantified. As illustrated in figure 4A (from one patient with HFpEF, one patient with SSc without PAH, and one patient with SSc-PAH), there is no appreciable difference in capillary density between the patient with HFpEF and the patient with SSc without PAH. However, capillary density appears clearly decreased (see magnification) in the patient with SSc-PAH. Figure 4B demonstrates that, when patients with SSc were divided into two groups on the basis of their median RAP or right ventricular diastolic pressure, there were significant differences in capillary density. Quite surprisingly, although one might expect an increase in vessel density in the setting of RV adaptation to an increased load, there was a significant decrease in myocardial capillary density in these patients with SSc-PAH with increased RAP. These very preliminary results demonstrate that RV biopsy can reveal significant alterations in capillary density in response to increased pulmonary vascular load, a finding consistent with imaging studies discussed above and which revealed decreased myocardial perfusion in PAH. 53 These techniques are safe and likely to yield strong mechanistic data to support our original hypothesis of altered myocardial function in SSc-PAH.
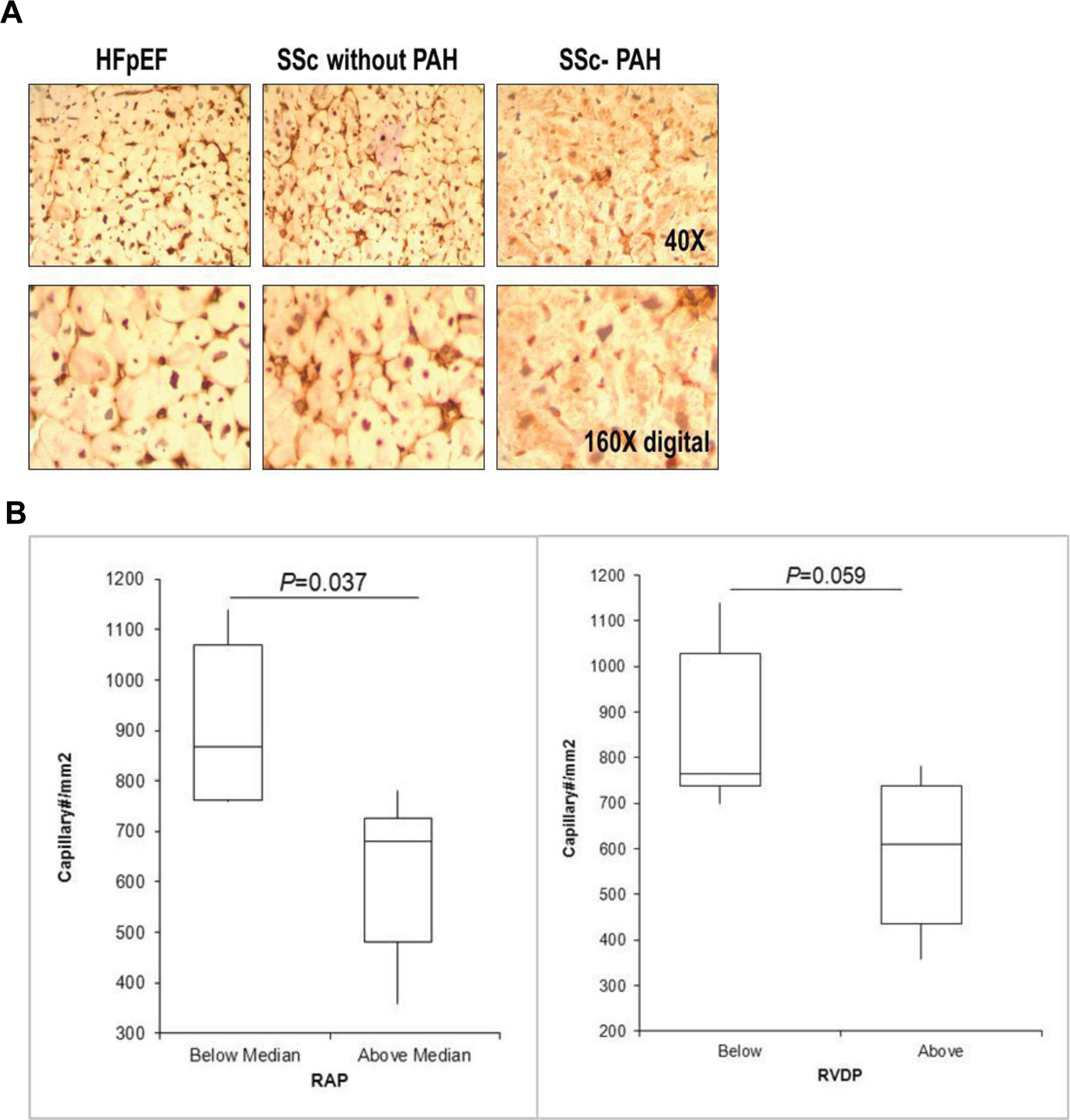
A, Immunostaining of myocardial capillaries in patients with heart failure with preserved ejection fraction (HFpEF), systemic sclerosis (SSc) without pulmonary arterial hypertension (PAH), and SSc-PAH, at low (upper panels) and high (lower panels) magnification. B, Capillary density (capillary#/mm 2 ) in patients below or above the median value for right arterial pressure (RAP) and right ventricular diastolic pressure (RVDP).
CONCLUSION AND FUTURE PERSPECTIVES
Intrinsic RV involvement in SSc seems to be a common complication with very serious consequences; it is often clinically occult, and detection depends on the sensitivity of the imaging modality. The etiology of cardiac involvement is multifactorial and may involve various degrees of inflammation, fibrosis, and microvascular abnormalities. These changes may explain the ominous RV-pulmonary vascular uncoupling recently observed in patients with SSc in the setting of pulmonary pressure overload 6 and their overall poor outcome. 3 Early diagnosis of heart disease 87 based on reliable biomarkers is essential for appropriate management of this patient population. However, major challenges remain in validating current assessment strategies and determining the effect of early therapeutic interventions in large and well-designed longitudinal studies. Furthermore, a more fundamental understanding of cellular and molecular mechanisms that govern the adaptation of RV to increased pulmonary vascular pressure is also needed to design adequate RV-targeted therapy.
