Abstract
Pulmonary arterial hypertension (PAH) is associated with aberrant pulmonary vascular remodeling that leads to increased pulmonary artery pressure, pulmonary vascular resistance, and right ventricular dysfunction. There is now accumulating evidence that the renin-angiotensin-aldosterone system is activated and contributes to cardiopulmonary remodeling that occurs in PAH. Increased plasma and lung tissue levels of angiotensin and aldosterone have been detected in experimental models of PAH and shown to correlate with cardiopulmonary hemodynamics and pulmonary vascular remodeling. These processes are abrogated by treatment with angiotensin receptor or mineralocorticoid receptor antagonists. At a cellular level, angiotensin and aldosterone activate oxidant stress signaling pathways that decrease levels of bioavailable nitric oxide, increase inflammation, and promote cell proliferation, migration, extracellular matrix remodeling, and fibrosis. Clinically, enhanced renin-angiotensin activity and elevated levels of aldosterone have been detected in patients with PAH, which suggests a role for angiotensin and mineralocorticoid receptor antagonists in the treatment of PAH. This review will examine the current evidence linking renin-angiotensin-aldosterone system activation to PAH with an emphasis on the cellular and molecular mechanisms that are modulated by aldosterone and may be of importance for the pathobiology of PAH.
Keywords
Pulmonary arterial hypertension (PAH) is an insidious disease with a poor long-term prognosis. In 2009, an epidemiological study estimated the incidence of PAH to be 1.1 cases per million per year and the prevalence to be 6.6 cases per million, with incident survival rates at 1, 2, and 3 years of 85.7%, 69.6%, and 54.9%, respectively, despite medical therapy.1,2 Although the etiology of PAH may vary between patients, the resultant cardiac and pulmonary vascular pathophenotypes are remarkably similar. The disease pathobiology is characterized by aberrant distal pulmonary vascular remodeling resulting from endothelial dysfunction, dysregulated vascular smooth muscle cell proliferation, and inflammation that promotes neointimal formation, thrombosis, and luminal obliteration. 3 The formation of these plexiform lesions contributes to impaired vascular reactivity, elevated pulmonary artery pressure, and increased pulmonary vascular resistance, which, in turn, initiates maladaptive right ventricular (RV) remodeling.4,5 The continued strain imposed on the RV-pulmonary vascular circuit by these remodeling processes ultimately leads to RV failure and death.4,5 Although our understanding of the PAH disease process has advanced over the past few decades, therapeutic targets and evidence-based interventions remain limited, and novel approaches to modify the underlying disease process continue to be pursued. 6
The renin-angiotensin-aldosterone system (RAAS) maintains blood pressure through its effects on the kidney to regulate sodium and water balance and on peripheral blood vessels to increase systemic vascular resistance. 7 In 1963, 10 years after the discovery of aldosterone, investigators infused radioactive aldosterone into rats and demonstrated that, in addition to its localization to the kidney, it was also taken up and metabolized by the lungs, heart, and aorta. Preliminary histological assessment using autoradiography indicated that aldosterone was localized to cardiomyocytes in the heart and to the alveolar walls of the lungs; the methodology used could not distinguish the pulmonary vessels from the alveoli, and it remained unknown for decades whether the pulmonary vasculature participated in aldosterone metabolism. 8 Since that time, there has been extensive investigation of the effects of aldosterone on the kidneys and systemic circulation, with recent interest in its role in modulating the RV-pulmonary vascular axis in PAH. This is not surprising, given that the cardiopulmonary remodeling that occurs with PAH recapitulates, in part, the effects of RAAS activation and, in particular, aldosterone, in the systemic circulation. Aldosterone has been linked to the development of systemic hypertension, left ventricular cardiac and systemic vascular remodeling, and left heart failure.9–11 Community-based longitudinal or cross-sectional studies have shown that higher levels of aldosterone are associated with an increased risk for developing arterial stiffness, incident hypertension, or left ventricular hypertrophy, which suggests that aldosterone is either causative or a disease modifier that facilitates adaptive cardiovascular remodeling.9,10
RENIN-ANGIOTENSIN SYSTEM
The classical teaching is that the primary function of the RAAS is to regulate intravascular volume to maintain blood pressure (Fig. 1). In response to a real (blood loss, dehydration) or perceived (ventricular pump failure) decrease in circulating blood volume, the juxtaglomerular cells lining the afferent arterioles located proximal to the renal glomeruli release renin into the circulation. Renin cleaves angiotensinogen, which is synthesized and secreted by the liver, to angiotensin I. Circulating angiotensin I is then hydrolyzed to angiotensin II by angiotensin-converting enzyme (ACE), which is located primarily in the pulmonary and renal endothelium. Angiotensin II activates the angiotensin type 1 (AT1) receptor to initiate a vasoconstrictor response and stimulate aldosterone synthesis by the adrenal gland. Aldosterone then acts on the renal tubules to initiate sodium and water retention to increase circulating blood volume and, thereby, blood pressure (reviewed in Santos et al. 12 and Briet and Schiffrin 13 ).
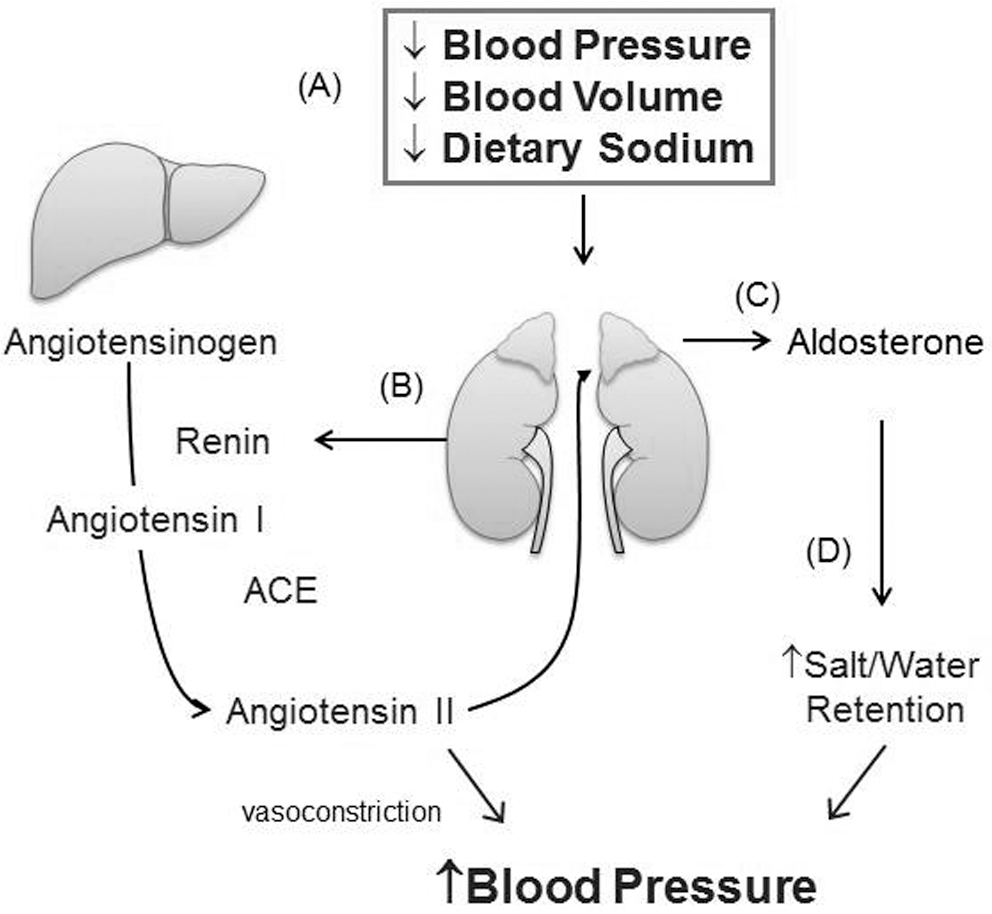
The renin-angiotensin-aldosterone system. In response to a drop in blood pressure or sodium intake (A), renin is released from the juxtaglomerular cells of the kidney to increase angiotensin II levels (B). Angiotensin II increases blood pressure by stimulating the production of aldosterone by the adrenal gland (C) to initiate salt and water retention and vasoconstriction of systemic resistance vessels (D). ACE = angiotensin-converting enzyme.
It is now recognized that the angiotensin arm of this hormonal pathway is far more complex than initially understood (Fig. 2). In fact, there are alternative pathways for angiotensin II generation, a number of vasoactive angiotensin cleavage peptides, and other angiotensin receptors that regulate cardiovascular hemodynamics and remodeling. In these nonclassical pathways, angiotensin II may be generated by the proteases chymase, which is present in mast cells and skeletal muscle, or cathepsin G, which exists in inflammatory cells. 14 Angiotensin II exerts its effects primarily by binding to and activating the AT1 and angiotensin type 2 (AT2) receptors to modulate vascular tone; activation of the AT1 receptor initiates a vasoconstrictor response, whereas AT2 receptor signaling promotes vasodilation. A homologue of ACE, ACE2, hydrolyzes either angiotensin I or angiotensin II to generate the heptapeptide angiotensin-(1–7). Angiotensin-(1–7) may also be generated directly from angiotensin I through the actions of neutral-endopeptidase (neprilysin) and prolyl-carboxypeptidase. 12 Angiotensin-(1–7) binds to the G-protein coupled Mas receptor, opposes the vasoconstrictor effects of angiotensin II, and does not stimulate aldosterone secretion. 12 By contrast, angiotensin III, another heptapeptide metabolite of angiotensin II, does stimulate aldosterone secretion through activation of the AT1 receptor. 15
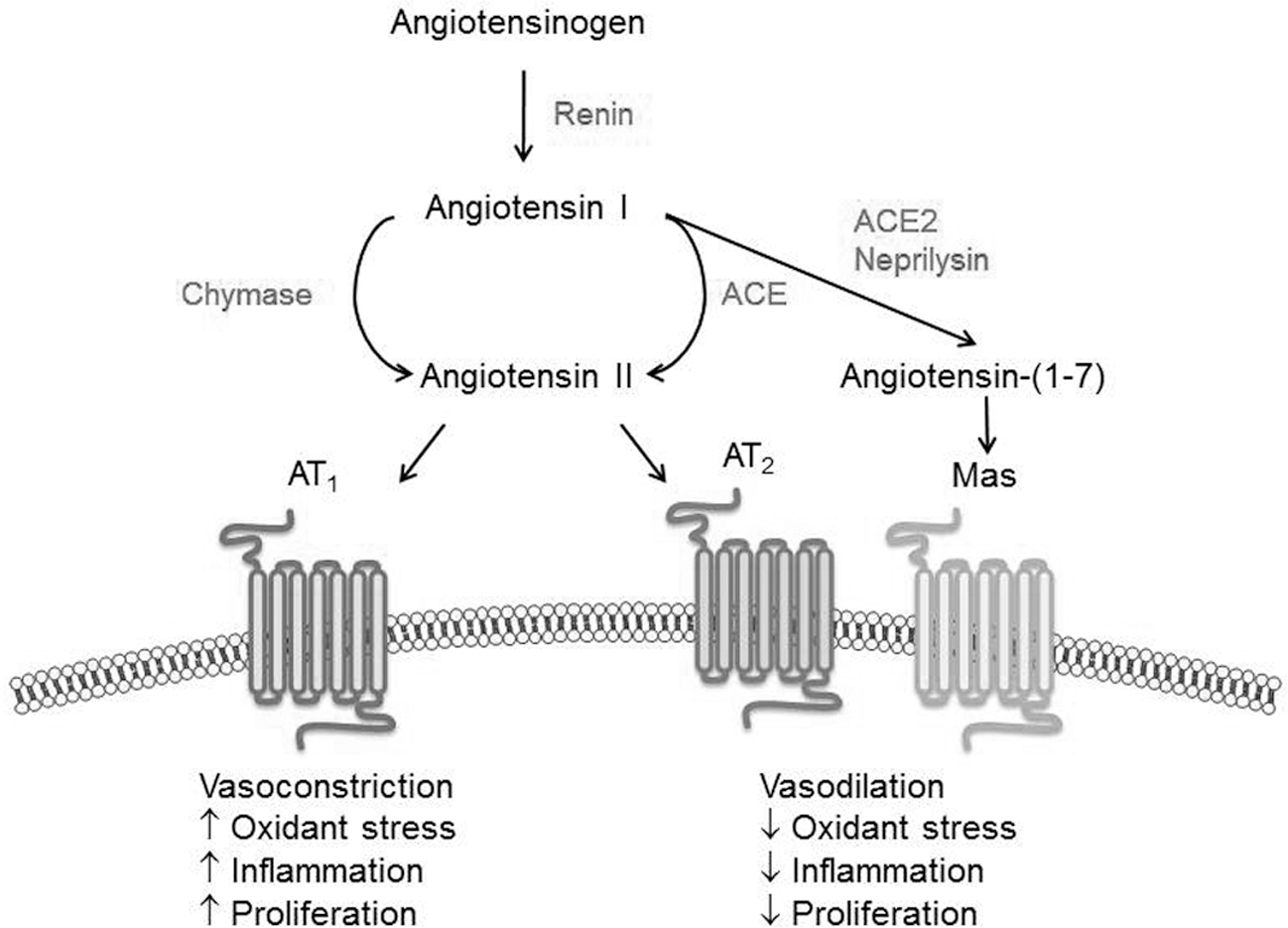
Angiotensin signaling. Angiotensin II may be generated from angiotensin I by the actions of angiotensin-converting enzyme (ACE) or chymase. Angiotensin I may also be cleaved by angiotensin-converting enzyme 2 (ACE2) or neutral endopeptidase (neprilysin) to yield angiotensin-(1–7). Angiotensin II binds to the angiotensin type 1 (AT1) receptor and the angiotensin type 2 (AT2) receptor, which have opposing effects on vascular structure and function. In addition, angiotensin-(1–7), which binds to the Mas receptor, is considered vasculoprotective.
The complexities of the angiotensin pathway indicate that the pathophysiological consequences of renin-angiotensin system activation in PAH may result from an imbalance between angiotensin II and other vasculoprotective angiotensin cleavage peptides that favors vasoconstriction and impairs vascular reactivity. In addition, these angiotensin signaling peptides have opposing effects on modulating other vascular smooth muscle cell functions important for vessel remodeling in PAH. For example, angiotensin II increases intracellular free Ca2+ levels and activates the Na+/H+ exchanger, tyrosine kinase signaling, mitogen-activated protein kinase signaling and reactive oxygen species production to stimulate vascular smooth muscle cell proliferation and migration. 16 By contrast, angiotensin-(1–7) inhibits these signaling pathways, limits proliferation and migration, and maintains vascular smooth muscle cell homeostatic processes. 17
RENIN-ANGIOTENSIN ACTIVATION IN PAH
In PAH, there is clear evidence that the renin-angiotensin signaling system is activated and contributes to the disease pathology. Early preclinical studies performed in the rat hypobaric hypoxia model associated angiotensin with pulmonary hypertension by demonstrating an increase in pulmonary vascular ACE messenger RNA (mRNA) and protein expression with an approximately 50% increase in ACE activity in remodeled pulmonary vessels. 18 Subsequent studies found that angiotensin signaling in remodeled vessels favored pulmonary artery smooth muscle cell proliferation and vasoconstriction with evidence of AT1 receptor upregulation and a concomitant downregulation of ACE2 and angiotensin-(1–7).19–22 The relevance of these findings for human disease was confirmed through pathological examination of lung sections from individuals with PAH. This revealed increased ACE and AT1-receptor but not AT2-receptor expression in remodeled vessels, and pulmonary vascular smooth muscle cells isolated from these samples were found to be hyperproliferative under hypoxic conditions.19,23 Activation of the renin-angiotensin system was not limited to the pulmonary vasculature, and a 3.4-fold increase in ACE activity was detected in the RV after 14 days of hypoxia. Interestingly, increased ACE activity was localized to areas of myocardial fibrosis and occurred only in the RV, as there was a reduction in ACE expression in the free wall of the left ventricle in hypoxic rats. 24
Evidence to support a causal role for angiotensin in PAH disease progression was provided by studies in hypoxic rats treated with the ACE inhibitor captopril or the AT1 receptor blocker losartan that demonstrated a decrease in the mean pulmonary artery pressure and RV hypertrophy as compared with saline-treated rats. 25 Similarly, studies performed in the rat monocrotaline model of PAH found that losasrtan decreased vascular remodeling, improved RV performance by decreasing RV systolic pressure and end-diastolic diameter, but had no effect on RV hypertrophy or cardiac output. Losartan treatment did, however, decrease RV afterload, a marker of improved arterial elastance, to restore RV-arterial coupling, providing further evidence that inhibition of angiotensin signaling improved vascular remodeling. 19
Investigators have also attempted to modulate the RV-pulmonary vascular pathophenotype in PAH by augmenting ACE2 and angiotensin-(1–7) to overcome the deleterious effects of angiotensin II signaling. In a mouse model of pressure overload pulmonary hypertension, the administration of recombinant human ACE2 upregulated expression of the Mas receptor to increase angiotensin-(1–7) signaling, and it improved RV systolic and diastolic function and decreased RV hypertrophy without influencing left ventricular hemodynamics. 26 These findings were supported by results from other studies that increased ACE2-angiotensin-(1–7) signaling by gene transfer using a lentiviral packaged angiotensin-(1–7) fusion gene or ACE2 complementary DNA.27,28 Similarly, a pharmacological ACE2 activator XNT (1-[(2-dimethylamino) ethylamino]-4-(hydroxymethyl)-7-[(4-methylphenyl) sulfonyl oxy]-9H-xanthene-9-one) diminished cardiopulmonary remodeling in PAH by increasing levels of the anti-inflammatory cytokine interleukin-10. 29 The importance of neprilysin as a source of angiotensin-(1–7) was demonstrated in neprilysin null mice. Although there was no adverse effect of gene deletion at baseline, after exposure to chronic hypoxia, the mice developed exaggerated pulmonary pressures and distal arterial muscularization. Pulmonary artery smooth muscle cells isolated from these mice were hyperproliferative owing to Src kinase and platelet-derived growth factor receptor activation, suggesting that angiotensin-(1–7) plays a regulatory role in mediating tyrosine kinase receptor signaling. 30
Findings from clinical studies indicate that RAAS activation occurs in patients with pulmonary hypertension. For example, there is an increased frequency of expression of an ACE gain-of-function polymorphism in patients with pulmonary hypertension compared with healthy individuals. Among 40 patients studied, however, the increase in ACE activity correlated with a higher cardiac output, and it was suggested that RAAS activation was merely a compensatory mechanism to prevent heart failure. 31 More direct evidence for renin-angiotensin activation in patients with pulmonary hypertension was provided recently when investigators measured these components in serum samples obtained from 58 patients with idiopathic PAH (New York Heart Association class II, 60%; class III, 31%; class IV, 9%). In this cohort, serum renin and angiotensin I levels were increased above the upper limit of normal in the majority of patients, whereas angiotensin II levels were elevated only in a smaller cohort. Follow-up studies (median duration, 39 months) indicated that persistently elevated levels of renin-angiotensin activity were associated with PAH disease progression assessed as a greater than 10% decrease in the 6-minute walk distance and an increased risk of lung transplantation or death. 19
Despite the finding that renin-angiotensin levels were elevated in patients with PAH, early clinical studies with the ACE inhibitor captopril in this patient population yielded mixed results. Short-term (48-hour) administration of captopril had no effect on exercise-induced changes in pulmonary pressures, pulmonary vascular resistance, or cardiac output. 32 Similarly, longer-term therapy was evaluated in a study involving 7 women treated with up to 300 mg/day of captopril for as long as 12 weeks. In these patients, captopril decreased blood pressure without influencing pulmonary artery pressure, resistance, cardiac output, or exercise tolerance. 33 These outcomes contrast with findings from a pilot study involving 5 patients that enforced strict metabolic conditions, restricted sodium intake, and found that steady-state captopril dosing of 150 mg/day decreased mean pulmonary artery pressures and improved RV ejection fraction. Neurohormonal profiling in these patients identified a decrease in plasma angiotensin II and aldosterone levels with no effect of the drug on cortisol or norepinephrine levels. 34
Conflicting results from these and other small studies led to a failure to reach a consensus opinion on the use of ACE inhibitors in patients with PAH, and the drugs were not evaluated in larger definitive clinical trials. Nonetheless, the observation that ACE inhibitors ameliorated disease only when aldosterone levels were decreased suggested that aldosterone may be the key component of the RAAS that mediates cardiopulmonary remodeling in PAH. Moreover, the mixed results from trials of ACE inhibition in PAH indicate that targeting the renin-angiotensin arm of the pathway alone may not be sufficient to limit disease progression and that the phenomenon of aldosterone breakthrough occurs in PAH. Aldosterone breakthrough was first described in patients with left heart failure who were treated optimally with β-blockers to inhibit renin and ACE inhibitors or AT1 receptor antagonists yet still had elevated levels of aldosterone. 35 This may occur as a result of incomplete inhibition of ACE activity or angiotensin II–independent synthesis of aldosterone. 36 Aldosterone breakthrough has also been proposed to account for the dramatic results of the Randomized Aldactone Evaluation Study (RALES), which demonstrated that aldosterone antagonism with spironolactone, when added to ACE inhibitors, decreased mortality and improved clinical outcomes. 35
ALDOSTERONE
There are several lines of evidence that converge to identify aldosterone as an integral mediator of the cardiopulmonary vascular phenotype in PAH. Elevated levels of aldosterone have been detected in experimental models of PAH and humans with the disease.37–39 This occurs, in part, due to increased adrenal production of aldosterone as well as extra-adrenal synthesis of the hormone that has been identified in the pulmonary vasculature. 37 These persistently elevated levels of aldosterone activate the mineralocorticoid receptor that is present in vascular and cardiac cells to initiate signaling pathways that promote vascular remodeling, impair vascular reactivity, and contribute to RV cardiac dysfunction associated with PAH.
Aldosterone synthesis in the adrenal gland is stimulated by angiotensin II and endothelin-1, which are elevated in PAH, as well as adrenocorticotropic hormone, plasma potassium levels, and the relative level of serum sodium (reviewed in Beuschlein 7 and Rossi 35 ). Aldosterone is synthesized from cholesterol in a series of catalyzed reactions with two rate-limiting steps; the transport of cholesterol to the inner mitochondrial membrane by steroidogenic acute regulatory protein (StAR) and conversion of 11-deoxycorticosterone to aldosterone by the enzyme aldosterone synthase (CYP11B2). Transcription of the aldosterone synthase gene is calcium-dependent, and known aldosterone secretagogues increase calcium levels; angiotensin II releases calcium from intracellular stores, whereas changes in potassium levels increase calcium influx through voltage-dependent T- and L-type calcium. 7
Although it is accepted that angiotensin II is generated by pulmonary vascular cells, the possibility that local extra-adrenal aldosterone synthesis occurs in the cardiopulmonary vascular system has been highly controversial. 40 At present, there is compelling evidence to indicate that aldosterone synthesis in the heart is extremely limited or nonexistent, based on studies performed with adrenalectomized rats that were administered high- or low-salt diets. In these studies, CYP11B2 expression was examined by mRNA and found to be 1.05 × 10−6 of that measured for the adrenal gland. Aldosterone measured by enzyme-linked immunosorbent assay was detectable in the heart in only 30% of adrenalectomized animals, and the levels detected were less than 30 pmol/L, suggesting either extremely limited synthesis or the detection of residual bound aldosterone.40,41 Other studies that used sensitive mRNA detection methods found no evidence of CYP11B2 mRNA in hearts from rats subjected to a conditions that would stimulate aldosterone production, despite an assay sensitivity of less than 100 copies mRNA/μg total RNA. 42
Aldosterone synthesis by vascular cells has been has been equally as controversial, with early studies detecting CYP11B2 expression in human umbilical vein endothelial cells but not pulmonary artery endothelial cells.43,44 The possibility of pulmonary vascular aldosterone synthesis was readdressed recently using more sensitive methodology, and CYP11B2 expression and aldosterone production were, in fact, detected in pulmonary artery endothelial cells stimulated with endothelin-1 or angiotensin II.37,41,43 These findings are in agreement with studies that analyzed and detected aldosterone production by mesenteric vessels using mass spectrometry and support the plausibility of pulmonary vascular extra-adrenal aldosterone synthesis. 45
ALDOSTERONE IN PAH
Hyperaldosteronism in PAH has been confirmed recently. Endothelin-1, which is upregulated in PAH and a known secretagogue of aldosterone, is likely an important determinant of pulmonary aldosterone synthesis. 46 In the rat monocrotaline model of PAH, plasma and lung tissue levels of endothelin-1 were increased significantly, and this was associated with a 442% increase in plasma aldosterone levels and a 183% increase in lung tissue aldosterone. Endothelin-1 increased pulmonary endothelial expression of CYP11B2 by 2.73-fold, indicating that endothelin-1 stimulated extra-adrenal pulmonary aldosterone synthesis. Once present, aldosterone induced pulmonary artery endothelial dysfunction by increasing oxidant stress to oxidatively modify the endothelin B receptor and disrupt endothelin B receptor–stimulated activation of the endothelial isoform of nitric oxide synthase (eNOS), resulting in diminished nitric oxide production. 37
Hyperaldosteronism was also associated with pulmonary arterial hypertension, pulmonary vascular remodeling, and RV hypertrophy in the rat monocrotaline and Sugen5416/hypoxia models of PAH. 37 In these models, treatment with the mineralocorticoid receptor antagonists spironolactone or eplerenone decreased the number of muscularized vessels, increased cross-sectional luminal area, and limited vascular collagen deposition and fibrosis; decreased pulmonary artery systolic pressure; and decreased RV hypertrophy. 37 Spironolactone has also been shown to prevent pulmonary vascular remodeling and RV dysfunction in the mouse chronic hypoxia model of PAH. 47
Clinically, elevated levels of aldosterone are present in patients with PAH, which indicates that aldosterone has been an underrecognized contributor to the PAH cardiopulmonary vascular phenotype. In a pilot study of patients with unexplained dyspnea who were referred for invasive hemodynamic evaluation, plasma aldosterone levels were found to be increased in patients with PAH, compared with control subjects (5,959.1 ± 2,817.9 vs. 1,200.4 ± 423.9 pg/mL; P < .02), and hyperaldosteronism was associated with a higher mean pulmonary artery pressure (45.5 ± 10.4 vs. 21.4 ± 5.0 mmHg; P < .002) and pulmonary vascular resistance. Furthermore, aldosterone levels correlated positively with pulmonary vascular resistance and inversely with cardiac output in a subset of patients with PAH who had severe disease. 38
As suggested by the preclinical studies evaluating the effects of aldosterone on endothelin-1 signaling in PAH, clinical benefit was observed when spironolactone was added to the selective endothelin receptor A antagonist ambrisentan. This was identified in a retrospective study of patients enrolled in the Ambrisentan in Pulmonary Arterial Hypertension, Randomized, Double-Blind, Placebo-Controlled, Multicenter, Efficacy Study 1 and 2 (ARIES-1 and ARIES-2). In this study, spironolactone use was identified in 21 (15.9%) and 10 (14.5%) of patients randomized to placebo or to ambrisentan (10 mg/kg), respectively.39,48 These trials demonstrated that patients treated with high-dose ambrisentan, compared with placebo, had a significantly improved 6-minute walk distance at 12 weeks. 4 Although patients who had been treated with both ambrisentan and spironolactone were sicker at baseline than patients treated with ambrisentan alone (higher pulmonary vascular resistance and increased levels of plasma B-type natriuretic peptide), patients treated with combination therapy had a 2.3-fold increase in their 6-minute walk distance and a significant decrease in plasma B–type natriuretic peptide levels, compared with patients treated with ambrisentan alone. 39 Although the rationale for the use of spironolactone among selected patients was also unknown in the ARIES studies, it is recognized that ambrisentan use is associated with peripheral edema, which was reported in 17% of patients treated with ambrisentan and only 11% of placebo-treated patients in the trials.48,49 When the definition of edema was broadened, it was discovered that more patients with edema were classified as World Health Organization class III/IV than patients without this adverse effect, suggesting that these sicker patients with edema benefited more from coadministration of spironolactone. 49
CELLULAR AND MOLECULAR MECHANISMS BY WHICH ALDOSTERONE CONTRIBUTES TO PAH
Aldosterone modulates the structure and function of the RV-pulmonary vascular circuit in PAH through several complementary cellular and molecular mechanisms, including increasing oxidant stress to decrease bioavailable nitric oxide, promote endothelial dysfunction, and impair vascular reactivity; enhancing inflammation; and stimulating vascular remodeling and fibrosis (Fig. 3).50,51 In the heart, aldosterone influences cardiomyocyte function through stimulation of the sympathetic nervous system, increased excretion of K+ and Mg+ to render the myocardium proarrhythmogenic, and initiation of cardiomyocyte apoptosis.52,53
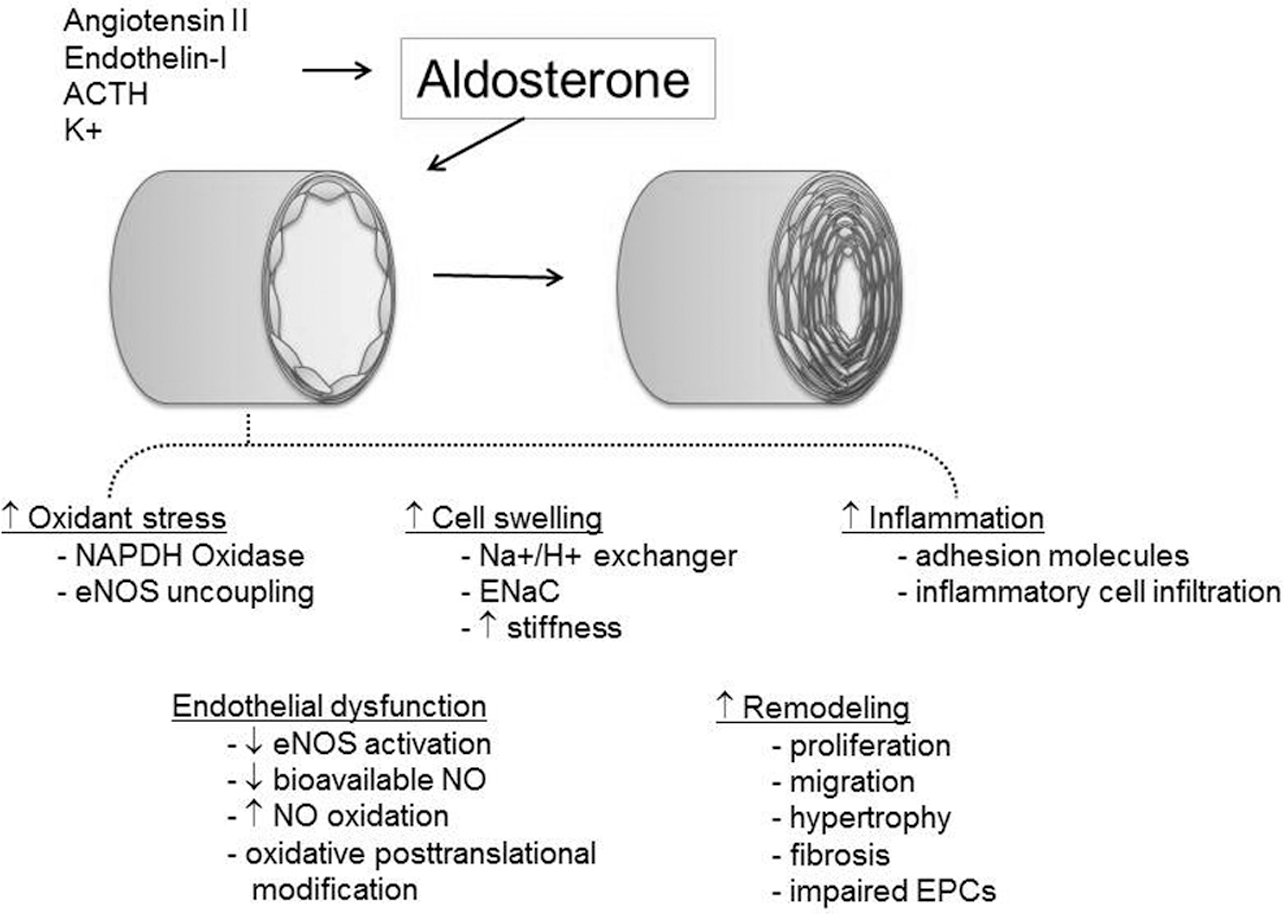
The effects of aldosterone on vascular function in pulmonary hypertension. Elevated levels of aldosterone have deleterious effects on vascular homeostasis, including increased oxidant stress resulting in a decrease in nitric oxide (NO) and endothelial dysfunction, cell swelling, and inflammation. Aldosterone also contributes to vascular remodeling by increasing cell proliferation and migration leading to vascular hypertrophy and by stimulating extracellular matrix remodeling and fibrosis. ACTH = adrenocorticotropic hormone; eNOS = endothelial isoform of nitric oxide synthase; ENaC = epithelial sodium channel; EPC = endothelial progenitor cell.
Aldosterone-induced endothelial dysfunction has been confirmed by flow-mediated dilation studies in healthy volunteers infused with aldosterone, in patients with primary hyperaldosteronism, and in hypertensive patients with high levels of aldosterone.54,55 In vitro studies suggested that endothelial dysfunction was the result of increased reactive oxygen species generation and decreased nitric oxide bioavailability.56,57 In fact, aldosterone increases vascular endothelial and smooth muscle cell oxidant stress, which has been implicated in the pathogenesis of PAH, through several complementary mechanisms. Aldosterone increases oxidant stress by activating NADPH oxidase, uncoupling of eNOS to generate superoxide in preference to nitric oxide, and decreasing cellular antioxidant capacity by downregulating expression and activity of glucose-6-phosphate dehydrogenase.58–63 In pulmonary artery endothelial cells, aldosterone upregulates the NOX4 subunit of NADPH oxidase to increase enzymatic activity and superoxide generation. This, in turn, decreases levels of bioavailable nitric oxide through a reduction in synthesis owing to oxidative posttranslational modification of a cysteinyl thiol, Cys405, which resides in the eNOS-activating region of the endothelin B receptor. 37 Other mechanisms by which aldosterone-stimulated oxidant stress decreases bioavailable nitric oxide include oxidation of nitric oxide to nitrite and nitrate as well as direct reaction with superoxide to form peroxynitrite. 37 In vascular smooth muscle cells, the increase in oxidant stress following aldosterone exposure promotes cell proliferation and migration by activating Akt, mitogen-activated protein kinase, and p70S6kinase signaling and further disrupts nitric oxide signaling by oxidatively modifying Cys122 of the β-subunit of soluble guanylyl cyclase to render the enzyme nitric oxide insensitive.62,64,65
Within the vasculature, aldosterone has been associated with an enhanced inflammatory response, which is a recognized component of vascular remodeling in PAH. Aldosterone increases endothelial cell adhesion molecule expression and facilitates activation and vascular infiltration of monocytes, macrophages, and lymphocytes.66,67 Interestingly, circulating monocytic (early) endothelial progenitor cells are affected adversely by aldosterone through a mechanism that involves increased cellular oxidant stress. These early progenitor cells are functionally impaired with limited vascularization and repair capacity. 68
In PAH, there is increased pulmonary vascular stiffening that occurs as a result of the remodeling process. Aldosterone contributes to vascular stiffening by regulating the salt and water content of vascular cells as well as stimulating profibrotic remodeling. Using atomic force microscopy, it has been shown that aldosterone increases endothelial cell volume by activation of an amiloride-sensitive Na+/H+ exchanger. Aldosterone also directs insertion of the epithelial sodium channel ENaC, which is expressed by vascular cells, into the endothelial cell membrane to increase cell water retention, swelling, and stiffness and this phenomenon has been shown to contribute to a decrease in endothelial cell nitric oxide release.69–73 Aldosterone is known to stimulate perivascular fibrosis by increasing expression of profibrotic mediators, such as galectin-3; transforming growth factor-β, connective tissue growth factor, and type I and type III collagen; and decreasing expression of the anti-fibrotic peptides and bone morphogenetic protein-4 and brain natriuretic peptide.74,75
In the heart, aldosterone increases cardiac NADPH oxidase activity, which, through endothelial-cardiomyocyte crosstalk, leads to myocardial endothelial dysfunction. 76 Aldosterone has also been shown to initiate changes in cardiomyocyte calcium handling and ion channel remodeling by modulating expression of the T-type calcium channel, L-type calcium channel, and ryanodine receptor activities.77–79 Similar to what is observed in the vasculature, aldosterone enhances myocardial stiffness and remodeling by increasing type I and type III collagen deposition, leading to perivascular and interstitial fibrosis. 80 Aldosterone also contributes to cardiac matrix remodeling through a mechanism that involves oxidation of Ca2+/calmodulin-dependent protein kinase II and increased matrix metalloproteinase-9 activity. 81
THERAPEUTIC INTERVENTIONS TO TARGET MINERALOCORTICOID RECEPTOR ACTIVATION
At present, there are no specific recommendations for the use of mineralocorticoid receptor antagonists in the treatment of PAH, and the use of diuretics is suggested as background therapy in symptomatic patients with signs of RV failure and volume overload (Table 1).82,83 For patients with a clinical indication for a mineralocorticoid receptor antagonist, treatment with the drugs should be started only if the patient's serum potassium is less than 5.0 mEq/L and the serum creatinine is less than 2.0 mg/dL for women and less than 2.5 mg/dL for men. Typically, serum potassium and renal function are measured 2 weeks after the initiation of the drug, with the frequency of measurements increased up to 6 months with longer-term use. 53 Concomitant use of supplements that contain potassium or use of other drugs, such as ACE inhibitors or nonsteroidal anti-inflammatory agents, necessitates increased surveillance of electrolytes and renal function. It should also be noted that, for patients with PAH who receive sildenafil, the addition of a potassium-sparing diuretic increases the area under the curve of the active metabolite N-desmethyl sildenafil by 62% (http://www.drugs.com/sildenafil); however, the clinical implications of this interaction are not known.
Mineralocorticoid receptor antagonists
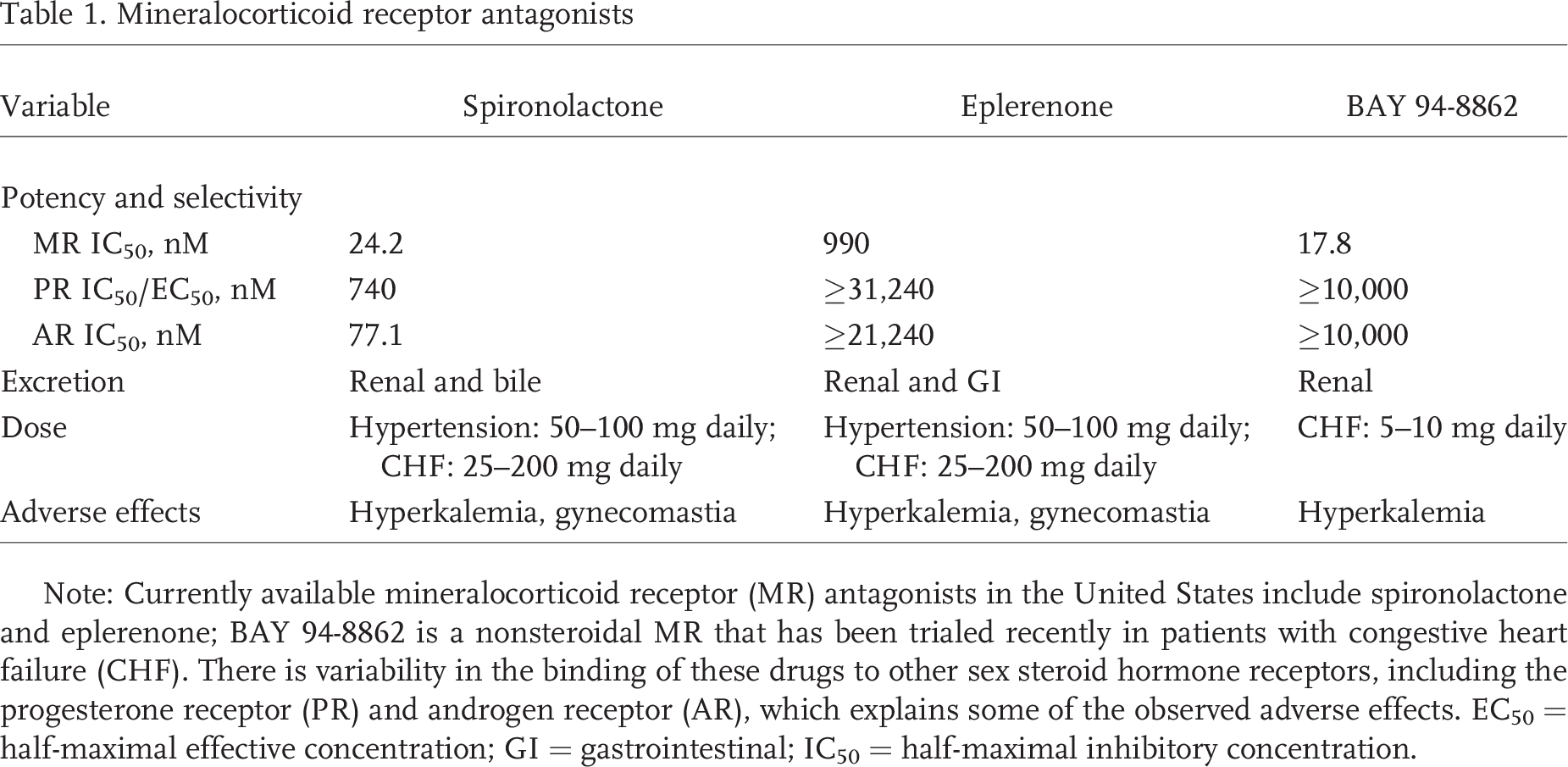
Note: Currently available mineralocorticoid receptor (MR) antagonists in the United States include spironolactone and eplerenone; BAY 94-8862 is a nonsteroidal MR that has been trialed recently in patients with congestive heart failure (CHF). There is variability in the binding of these drugs to other sex steroid hormone receptors, including the progesterone receptor (PR) and androgen receptor (AR), which explains some of the observed adverse effects. EC50 = half-maximal effective concentration; GI = gastrointestinal; IC50 = half-maximal inhibitory concentration.
Spironolactone is a widely available, inexpensive mineralocorticoid receptor antagonist that is nonselective and requires hepatic metabolism to generate its active metabolites. The maximal drug response is observed approximately 48 hours after the first dose. Spironolactone is structurally similar to progesterone, and there is some sex-steroid receptor cross reactivity. This phenomenon accounts for the anti-progesterone and anti-androgen effects observed in some patients treated with the drug. Spironolactone is dosed between 25 and 200 mg daily for congestive heart failure and between 50 and 100 mg daily for hypertension, with dose titration recommended at 4- to 6-week intervals until the desired clinical effect is achieved. 53 Optimal dosing of spironolactone in PAH is not known.
Eplerenone is a selective mineralocorticoid receptor antagonist that was derived from spironolactone but has limited affinity for the progesterone and androgen receptors and therefore lacks the sex-related adverse effects attributed to spironolactone. Eplerenone is metabolized by cytochrome P450 isoenzyme CYP3A4 and, therefore, is subject to drug-drug interactions with inhibitors of this isoenzyme, including ketoconazole, itraconazole, ribonavir, and clarithromycin. Eplerenone metabolism is also influenced by inducers of CYP3A4, such as St John's Wort, which has been shown to decrease levels by 30%. Steady-state drug levels of eplerenone are usually achieved 48 hours after the first dose is administered. When eplerenone treatment is started, it is dosed at 25 mg daily, and the dose is titrated until a clinical response is observed or a maximum dose of 50 mg twice daily is reached. 53
There is now a third-generation nonsteroidal mineralocorticoid receptor antagonist, BAY 94-8662, which is reported to have improved selectivity for the mineralocorticoid receptor compared with spironolactone or eplerenone in preclinical studies.84,85 In models of hypertension-mediated left heart failure and renal dysfunction, BAY 94-8862 provided better cardiorenal end-organ protection than other mineralocorticoid receptor antagonists. 84 In humans, the plasma half-life of BAY 94-8862 is approximately 2 hours in healthy individuals, and the drug is administered once daily. Recently, results from the first randomized clinical trial of this compound in patients with left heart failure, a reduced ejection fraction, and mild or moderate chronic kidney disease were reported. 86 In this pilot study, BAY 94-8862 reduced indices of heart failure to a degree similar to that observed with spironolactone but with fewer episodes of hyperkalemia. This suggests that this agent may broaden the population of patients who can be treated with a mineralocorticoid receptor antagonist. 86
CONCLUSION
There is clear evidence that the RAAS is activated in PAH and modulates cardiopulmonary remodeling and function, which contributes to progression of the disease. Results from preclinical and clinical studies indicate that angiotensin II and, in particular, aldosterone, regulate cellular signaling processes that increase proliferation, migration, and vascular hypertrophy as well as initiate cardiovascular fibrosis and interrupt repair processes. Although the prevailing evidence suggests that mineralocorticoid receptor antagonists will benefit patients with PAH, currently available drugs remain to be studied in a systematic randomized clinical trial. Toward this end, a planned clinical trial of early initiation of spironolactone therapy in 70 patients with PAH without clinical evidence of right heart failure has been announced. In this placebo-controlled study, the effect of spironolactone on disease modification will be examined by evaluating the 6-minute walk distance and clinical progression of PAH at 24 weeks. 87 In addition to oral agents, recent advances with inhaled therapies, including gene transfer using aerosolized adeno-associated virus, suggest that other methodologies to deliver mineralocorticoid antagonists or selectively decrease pulmonary mineralocorticoid receptor expression may also be available as future pharmacotherapies. 88
