Abstract
Pulmonary arterial hypertension (PAH) is a major complication of sickle cell disease (SCD). Low levels of apolipoprotein A1 (Apo-A1) have been implicated in the development of PAH in SCD. We speculate that lower levels of Apo-A1 are related to dysregulation of the ubiquitin-proteasome pathway (UPP). Of 36 recruited patients with SCD, 14 were found to have PAH on the basis of right heart catheterization. Levels of Apo-A1 and Apo-B, polyubiquitin, total protease, and specific and normalized activity of chymotrypsin-like, trypsin-like, and caspase-like proteases in plasma were measured. Levels of Apo-A1 were found to be lower and polyubiquitin levels were found to be significantly higher in the PAH group (P < 0.05) in SCD. Apo-A levels were inversely correlated with polyubiquitin levels (r = −0.499, P = 0.009). These results indicate that lower levels of Apo-A1 in SCD patients with PAH are likely related to enhance degradation by UPP, potentially contributing to pulmonary vascular pathology. These findings may provide significant insight in identifying suitable therapeutic targets in these patients.
Keywords
INTRODUCTION
Pulmonary arterial hypertension (PAH) is a major complication of sickle cell disease (SCD) and a major risk factor for death in this population.1,2 The prevalence of PAH in adults with SCD varies from 6% to 10%, on the basis of right heart catheterization (RHC).3–5 Almost 75% of adult patients with SCD have histological evidence of PAH at the time of death. 6
The specific mechanism by which PAH develops in SCD is not clear, but it is thought to be multifactorial. Serum apolipoprotein (Apo) levels are known to be lower in patients with SCD than in the general population. 7 The most significant of these is Apo-A1, a major protein component of high-density lipoprotein particles (HDL-C) in plasma. A recent study indicated that SCD patients with low Apo-A1 levels have a higher prevalence of PAH. 8 In addition, SCD patients with lower-than-median Apo-A1 levels showed deficient vasodilatory responses to the endothelial agonist acetylcholine. This suggests that SCD patients with low Apo-A1 levels have endothelial dysfunction, which is common to the systemic and pulmonary circulations and is a precursor to vascular diseases.6,9
The exact cause of low levels of Apo-A1 in SCD patients is unknown. The ubiquitin-proteasome pathway (UPP) is known to play a central role in intracellular protein degradation. 10 The pathway employs an enzymatic cascade by which multiple ubiquitin molecules are covalently attached to the protein substrate. The polyubiquitin modification marks the protein for destruction and directs it to the proteasome complex for degradation. 11 The 26S proteasome consists of a catalytic 20S proteasome core and two 19S (cap) regulatory complexes. The 20S proteasome is a 660–700-kDa multicatalytic proteinase complex consisting of seven α subunits and seven β subunits.12,13 The caspase-like activity of the β1 subunit, the trypsin-like activity of the β2 subunit, and the chymotrypsin-like activity of the β5 subunit allow the proteasome to cleave different proteins into oligopeptides.
In the current study, we hypothesize that low levels of Apo-A1 in SCD patients are related to abnormalities of UPP and may play a role in the development of PAH in this population.
METHODS
Study population
Patients with known SCD were recruited from our hospital's SCD clinic. Patients with known causes of secondary pulmonary hypertension, chronic renal insufficiency, pregnancy, smoking or substance abuse, active sickle crisis, or acute chest syndrome at the time of their echo were excluded (Table 1). This study was approved by the Downstate–Kings County Institutional Review Board, and written informed consent was obtained from all individuals.
Demographics and biochemistry in patients with sickle cell disease and pulmonary arterial hypertension (PAH) versus no PAH
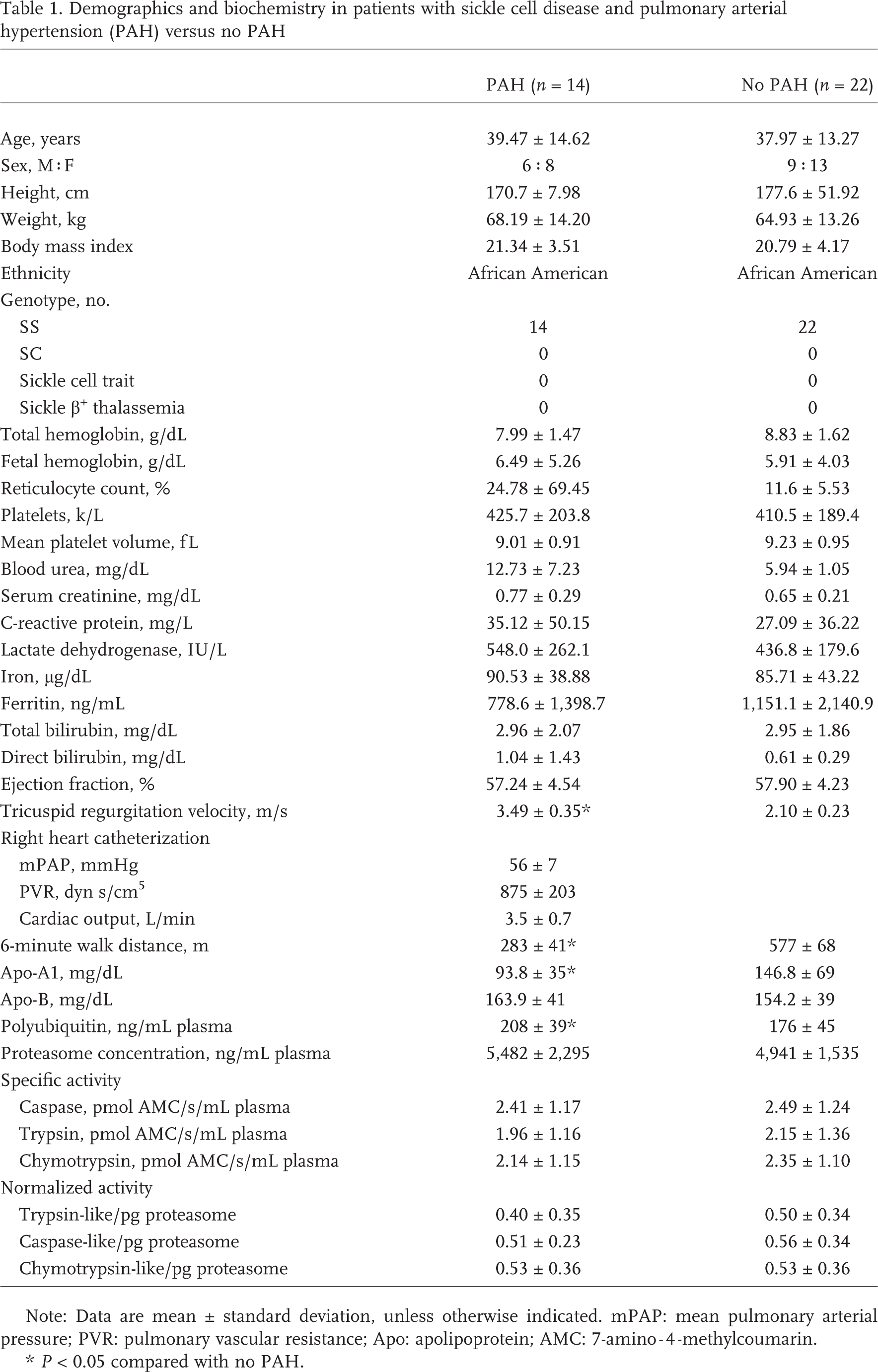
Note: Data are mean ± standard deviation, unless otherwise indicated. mPAP: mean pulmonary arterial pressure; PVR: pulmonary vascular resistance; Apo: apolipoprotein; AMC: 7-amino-4-methylcoumarin.
P < 0.05 compared with no PAH.
Evaluation for PAH
Two-dimensional and Doppler echocardiographic studies (iE33 and 5500; Philips, Andover, MA) were performed according to standard American Society of Echocardiography protocol. We defined tricuspid regurgitation velocity (TRV) of ≥2.5 m/s as a marker of PAH in SCD. The presence of PAH was confirmed in patients with TRV of ≥2.5 m/s via RHC, defined as mean pulmonary arterial pressure of ≥25 mmHg. Cardiac output was obtained using triplicate measurements with the thermodilution method (Agilent, Böblingen, Germany). Fourteen patients were found to have PAH, and 22 patients were found not to have PAH.
Measurement of apolipoproteins and UPP
Serum samples from 14 patients with SCD-related PAH and 22 patients without PAH were analyzed for levels of UPP markers (proteasome, polyubiquitin, and proteasome enzymatic activities [pmol 7-amino-4-methylcoumarin/s/mL plasma] and normalized activity/pg proteasome), as described elsewhere. 14 Methods were adjusted according to the current study. Serum Apo-A1 levels were measured by enzyme-linked immunosorbent assay in triplicate.
Statistical analysis
A statistical software package (SAS, ver. 9.2; SAS Institute, Cary, NC) was used for data management. Results were expressed as mean ± standard deviation. Statistical analyses were performed using the Wilcoxin t test and the Spearman correlation. Multivariate regression analysis was applied to determine the independent relationships of all clinical variables. A P value of <0.05 was considered statistically significant.
RESULTS AND DISCUSSION
This study showed that among patients with SCD, those with PAH had lower levels of Apo-A and higher levels of polyubiquitin than did those with normal pulmonary arterial pressure. Polyubiquitin levels were significantly higher in the PAH group. Caspase, trypsin, trypsin-like normalized proteasome activity per picogram, caspase-like, and, chymotrypsin-like normalized activity levels were similar between the two groups. There was an inverse relationship between Apo-A and polyubiquitin levels, which was confirmed on multivariate analysis after adjustment for pulmonary arterial pressure. These findings support and extend those of prior studies showing lower Apo-A1 levels related to higher pulmonary arterial pressure. To our knowledge, this is the first study investigating the relationship between UPP and Apo-A1 in the setting of SCD-related PAH.
Levels of Apo-A1 were found to be significantly lower in SCD patients with PAH than in those without PAH (P < 0.05). In addition, Apo-A1 showed a significant negative correlation with polyubiquitin levels in blood (r = −0.499, P = 0.009; Fig. 1), which were elevated in the PAH group (P < 0.05). No significant association was observed between Apo-A1 levels and other parameters, such as total proteasome concentration and specific and normalized activity of chymotrypsin-like, trypsin-like, and caspase-like protease levels. Polyubiquitin and Apo-A1 levels did not correlate with age, sex, body mass index, hemoglobin, white blood cell count, reticulocyte count, lactate dehydrogenase, iron/ferritin levels, blood urea nitrogen (BUN), and serum creatinine. Our data indicate that lower levels of Apo-A1 in SCD patients, especially those with PAH, are probably related to enhanced ubiquitination, thereby directing more Apo-A1 to proteolytic chambers.
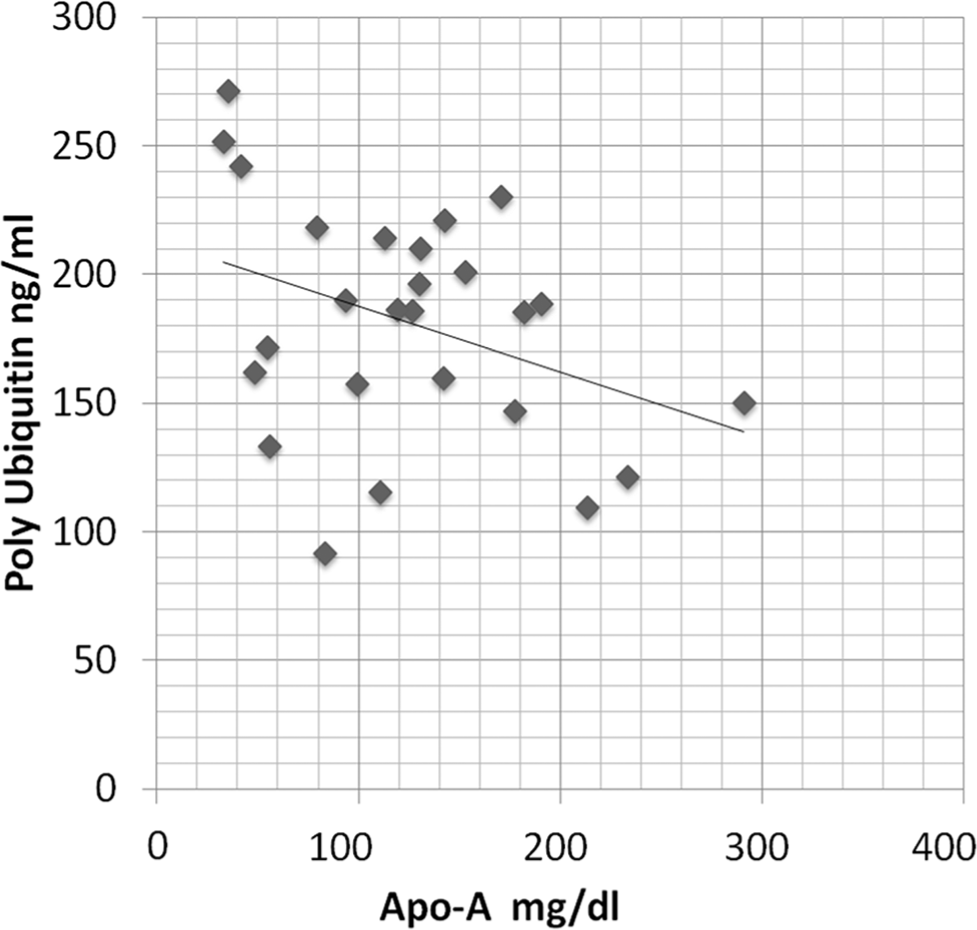
Negative correlation between apolipoprotein A (Apo-A) and polyubiquitin levels in patients with sickle cell disease (r=–0.499, P = 0.009). Multivariate regression analysis was applied to determine the independent relationships of all clinical variables. A P value of ≤0.05 was considered statistically significant.
Plasma cholesterol is transported within lipoproteins by two interrelated cascades that include the Apo-B-containing lipoproteins (chylomicrons and low-density lipoproteins) and the Apo-A1-containing lipoproteins (HDL). Plasma HDL-C level is considered to reflect the efficiency of the reverse cholesterol transport, a mechanism to remove excess cholesterol from the vascular macrophages. Apo-A1, the major structural apolipoprotein of HDL, is synthesized and secreted by the liver and intestine as a lipid-poor apolipoprotein, pre-β-HDL. Pre-β-HDL binds to the adenosine triphosphate–binding cassette (ABC) A1 transporter to initiate cholesterol efflux from cells.16,17 After cholesterol efflux, pre-β-HDL is converted to α-HDL.
α-HDL is the ligand for both the ABCG1 transporter 18 and the scavenger receptor class B type I (SR-BI). 19 SR-BI not only has the capacity to transport the cholesterol in and out of the cells but is also known to activate a poorly understood signal transduction pathway that ultimately stimulates endothelial nitric oxide synthase (eNOS) to release nitric oxide (NO). 20 In hyperlipidemic subjects without SCD, niacin increases Apo-A1 and HDL-C levels, which causes improvement in blood flow physiology and enhanced eNOS expression. 21 Thus, a low Apo-A1 level in SCD patients can result in a decrease in SR-BI activation and finally a decrease in NO release, causing endothelial dysfunction. These findings in humans are supported by animal experiments, where a peptide mimetic of Apo-A1, L4F, ameliorates endothelial dysfunction in a sickle cell mouse model. 22 This defect in vascular function seems to be discrete from and adjuvant to the NO resistance due to NO scavenging. 23
UPP is the major intracellular protein turnover pathway in eucaryotic cells. It regulates central mediators of proliferation, inflammation, and apoptosis that are fundamental for survival. 24 Although it was previously understood that the proteasome was found only intracellularly, 25 it is now known that the proteasome can also exist in extracellular spaces, such as human blood plasma, bronchoalveolar fluid, and sperm.26–28 Apo-A1 is usually cleared from plasma via the kidneys. However, our studies indicate a novel possibility, namely, that some Apo-A1 (and possibly HDL) might be catabolized in the plasma compartment by proteasomes.
Our study is limited, as we performed RHC in patients with TRV of ≥2.5 only to confirm PAH but not in patients with normal TRV. Therefore, patients with PAH but normal TRV on echo may have been misclassified. In summary, we show here for the first time that low levels of Apo-A1 in SCD patients with PAH are related to dysregulation of UPP. Low levels of Apo-A1 may contribute to endothelial dysfunction and pulmonary vascular pathology. Further studies are warranted to explore distinct patterns of UPP in SCD-related PAH. These findings not only might provide potential insight into pathophysiological mechanisms but also might be useful for identifying suitable therapeutic targets in these patients.
