Abstract
Hemodynamic measurements provide important parameters for determining prognosis and therapy in patients with pulmonary arterial hypertension (PAH). Current guidelines do not incorporate the possible predictive value of individual changes in hemodynamic variables during the disease time course, and there is no consensus about the time point for hemodynamic reevaluation. We aimed to assess the long-term prognostic value of short-term changes in hemodynamic parameters. The study included 122 patients with PAH from the Giessen Pulmonary Hypertension Registry who underwent hemodynamic evaluation at baseline and at 16 weeks (±2.5 standard deviations [SDs]; range: 4–29 weeks) after initial assessment. At baseline, mean pulmonary vascular resistance (PVR) was 1,109 dyn s cm−5, and 82% of patients were in World Health Organization (WHO) functional class III or IV. Fifty patients died, and 2 underwent lung transplantation during long-term observation (≤10 years; mean: 4.7 years). Kaplan-Meier estimates for transplant-free survival were 93.3%, 76.1%, 57.8%, and 53.1% at 1, 3, 5, and 7 years, respectively. When assigned to prognostic groups, improvements in cardiac output of >0.22 L min−1 (hazard ratio [HR]: 2.05; P = 0.015) and a decrease in PVR of >176 dyn s cm−5 (HR: 1.89; P = 0.044) at 4–29 weeks were associated with long-term transplant-free survival. Changes in mean pulmonary arterial pressure did not predict long-term prognosis. Of 2 noninvasive parameters assessed in this selected patient group, change in WHO functional class, but not in 6-minute walk distance, predicted long-term prognosis. Short-term assessment of changes in hemodynamic parameters at 16 weeks ± 2.5 SDs after initial invasive evaluation is useful to determine long-term prognosis in patients with PAH.
Keywords
INTRODUCTION
Pulmonary arterial hypertension (PAH) is a chronic disease of the small pulmonary vessels. It is characterized by progressive remodeling of the pulmonary vasculature, which may result in increased pulmonary vascular resistance (PVR), leading to right heart failure and death. 1 PAH includes idiopathic PAH (IPAH) and PAH associated with different diseases (pulmonary hypertension [PH] of group 1 according to the Dana Point classification of the World Health Organization [WHO]). 1 Although therapeutic options for PAH have increased in recent years, it still remains a progressive disease with high mortality2,3 that often requires the combination of specific therapies targeted to the pulmonary vasculature.1,4 Thus, increasing emphasis has been placed on assessing predictive prognostic parameters to determine the appropriate treatment for PAH. The importance of hemodynamic parameters as prognostic factors has been shown in the past.3,5–14 It has been known for >20 years that baseline hemodynamic parameters at the time of diagnosis, including right atrial (RA) pressure, cardiac index, and mean pulmonary arterial pressure (mPAP), are predictors of survival. 13 In recent years, much progress has been made in the identification of further prognostic parameters. These include noninvasive parameters, such as WHO functional class, 6-minute walk distance (6MWD), and serum biomarkers (e.g., brain natriuretic peptide [BNP] and its N-terminal fragment, NTproBNP), as well as invasively determined parameters, such as RA pressure, cardiac index, and mixed venous oxygen saturation (Sv̄o2).3,5–14
According to current European guidelines for diagnosis and treatment of PH, the decision to escalate the targeted therapy is based mainly on these prognostic parameters, determined at specific time points of the disease to categorize patients as satisfactorily or nonsatisfactorily treated. 15 Most risk scores use baseline measurements made at the time of diagnosis for determination of survival.3,14,16 However, several studies suggest that the long-term prognosis of patients with IPAH is dependent not only on baseline parameters but also on the individual response to therapy determined by invasive and noninvasive follow-up measurements.6–8,17,18 Changes in WHO functional class, cardiac index, Sv̄o2, and NTproBNP on reevaluation 3–12 months after initiation of PAH-targeted therapy have been suggested to be significant predictors of outcome. 4 However, there is no consensus about the time point for invasive follow-up for evaluation of prognosis and decision making about treatment escalation. 15 In particular, the concept of early treatment escalation to avoid critical progression of PAH has urged the need for prognostic parameters that allow decision making in an early state of the disease or early after treatment initiation. 19 Additionally, with regard to clinical studies, the time point of relevant follow-up catheterization is of major importance, as it is essential for assessing the efficacy of a new therapeutic drug. The time window in the majority of relevant randomized clinical trials for potential new drugs for patients with PAH is currently 12–16 weeks. 20
In the past, it has not been investigated whether short-term changes in hemodynamic parameters after the start of treatment are of predictive value for the long-term outcome of PAH. Thus, in the current study we analyzed whether changes in hemodynamic parameters reassessed after a short interval of 4–29 weeks are predictive for long-term survival after an observational period of up to 7 years.
MATERIAL AND METHODS
Setting and patients
Patients with PAH (17–81 years of age) were identified from the Giessen Pulmonary Hypertension Registry, a registry of >2,500 patients newly diagnosed with PH between 1991 and 2013 at a single specialized referral center (the Giessen Pulmonary Hypertension Center, Universities of Giessen and Marburg Lung Center, University Hospital Giessen, Giessen, Germany). The diagnosis of PAH was made in accordance with the standards in place during the respective time periods,15,21 using clinical examination, transthoracic echocardiography, pulmonary function tests, cardiopulmonary exercise testing, blood gas analyses, screening for human immunodeficiency virus and collagen vascular diseases, coronary angiography, or sleep studies, as clinically indicated. The presence of chronic thromboembolic PH or parenchymal lung disease was excluded using thoracic computed tomography, pulmonary perfusion scintigraphy, and conventional pulmonary angiography for selected patients. The diagnosis of precapillary PH was confirmed on initial right heart catheter investigation on the basis of a mPAP of >25 mmHg, a pulmonary arterial wedge pressure (PAWP) of <15 mmHg, and a PVR of >240 dyn s cm−5. To ensure a homogeneous patient population, patients <17 years old and those >81 years old were excluded.
Patients included in this analysis underwent hemodynamic assessments at baseline before treatment initiation and again 4–29 weeks after treatment was started. Treatment was initiated after the first right heart catheterization (RHC) in accordance with the guidelines in place at the respective time points with either oral calcium channel blockers, phosphodiesterase type 5 inhibitors (PDE5i), endothelin receptor antagonists (ERAs), prostanoids (inhaled or intravenous), or a combination of these therapies when indicated. In addition, patients were started on oral anticoagulation if not contraindicated. All relevant patient data were prospectively gathered on an ongoing basis, beginning at the time of the first RHC.
This study was approved by the Ethics Committee of the Medical Division of the Justus Liebig University of Giessen, Giessen, Germany (approval 266/11).
Statistical analyses
Statistical calculations were performed using SPSS (ver. 21; IBM, Armonk, NY). Patient data are presented as absolute numbers (mean or median) and standard deviations (SDs). The outcome end point was death or lung transplantation. Cox regression analyses were performed to evaluate the predictive value of changes in mPAP, PVR, and cardiac output (CO) for transplant-free survival. Multivariate Cox regression was used to adjust for possible confounders. We considered age, gender, subclass of PAH, and date of diagnosis (date of first catheterization) as possible confounders for each hemodynamic parameter. Analyses were performed on data from the entire study population (16 weeks ± 2.5 SDs) and in a subset who had undergone reevaluation after exactly 12–16 weeks. Patients were subsequently categorized into risk groups according to CO and PVR cutoff values, which were defined as the median value of the respective parameter. These parameters were assessed with single and multivariate Cox proportional hazards analysis hazard ratios (HRs) and are given as point estimates and 95% confidence intervals (CIs). Kaplan-Meier plots were used to illustrate transplant-free survival in relation to the risk groups, and group differences were assessed by log-rank tests. The impact on transplant-free survival of change in WHO functional class and of change in 6MWD was also assessed. The significance of the effect of WHO functional class was assessed by a nonparametric stratified Wilcoxon test. Cox regression analysis was used to assess change in 6MWD. For all analyses, statistical significance was considered at P < 0.05. Statistical analyses were performed using data obtained during the entire observation period (up to 10 years); however, the presentation of survival data over time is restricted to a maximum of 7 years because too few patients had data after this time point.
RESULTS
Patients
A group of ~ 700 individuals with PAH (WHO group 1 according to the Dana Point classification) was identified from the ~2,500 patients recorded in the PH registry. Of these individuals with PAH, 122 had undergone hemodynamic assessments at baseline and again after 16 weeks (±2.5 SDs; range: 4–29 weeks), with 48% (59/122) having been assessed exactly 12–16 weeks after treatment initiation. These 122 patients formed the study cohort.
Overall, 47% of the study cohort had IPAH (including 30 of the 59 patients who were assessed exactly 12–16 weeks after start of treatment), 25% had collagen vascular disease, 10% had portopulmonary hypertension, and 8% had a systemic to pulmonary shunt. The mean age was 51.8 ± 15.5 years, and mean 6MWD was 290.7 ± 122.4 m. Eight patients (7%) were in WHO functional class II, 69 (57%) in functional class III, and 31 (25%) in functional class IV (data were missing for 14 patients). The specific treatment administered between the first and second RHC was a PDE5i in 54 patients, an inhalative prostanoid in 19 patients, an ERA in 19 patients, and a calcium channel blocker in 14 patients; 5 patients were receiving combination therapy and 11 patients did not receive any PH specific therapy before the first follow-up evaluation.
Table 1 lists the baseline hemodynamics of the study cohort (n = 122). Changes in pulmonary hemodynamics between the initial and follow-up RHC after 16 weeks ± 2.5 SDs (n = 122) and after exactly 12–16 weeks (subset of 59 patients) are shown in Table 2. Compared with the initial catheterization, mPAP and PVR had decreased and CO had increased at follow-up. The distribution of change in hemodynamic parameters 12–16 weeks after the first RHC is shown in Figure 1.
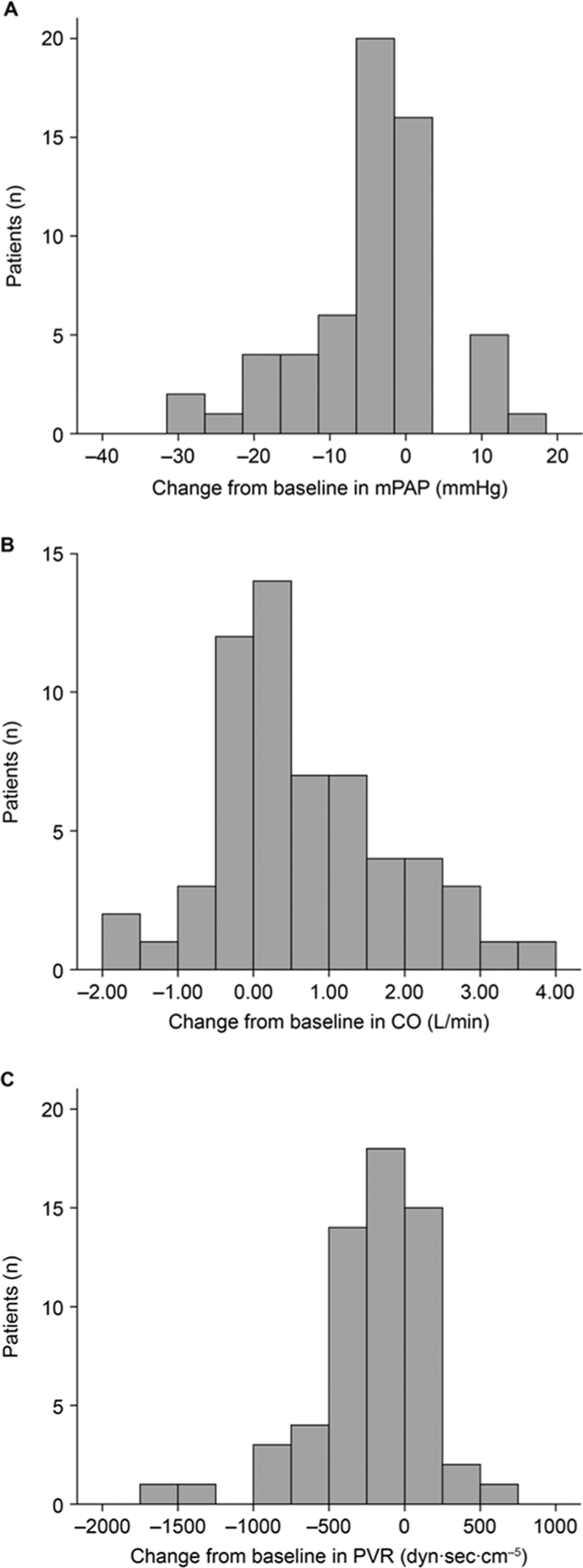
Distribution of change from baseline in hemodynamic parameters 12–16 weeks after the first right heart catheterization. A, Change in mean pulmonary arterial pressure (mPAP). B, Change in cardiac output (CO). C, Change in pulmonary vascular resistance (PVR). A color version of this figure is available online.
Baseline hemodynamic characteristics of patients with pulmonary arterial hypertension (n = 122)
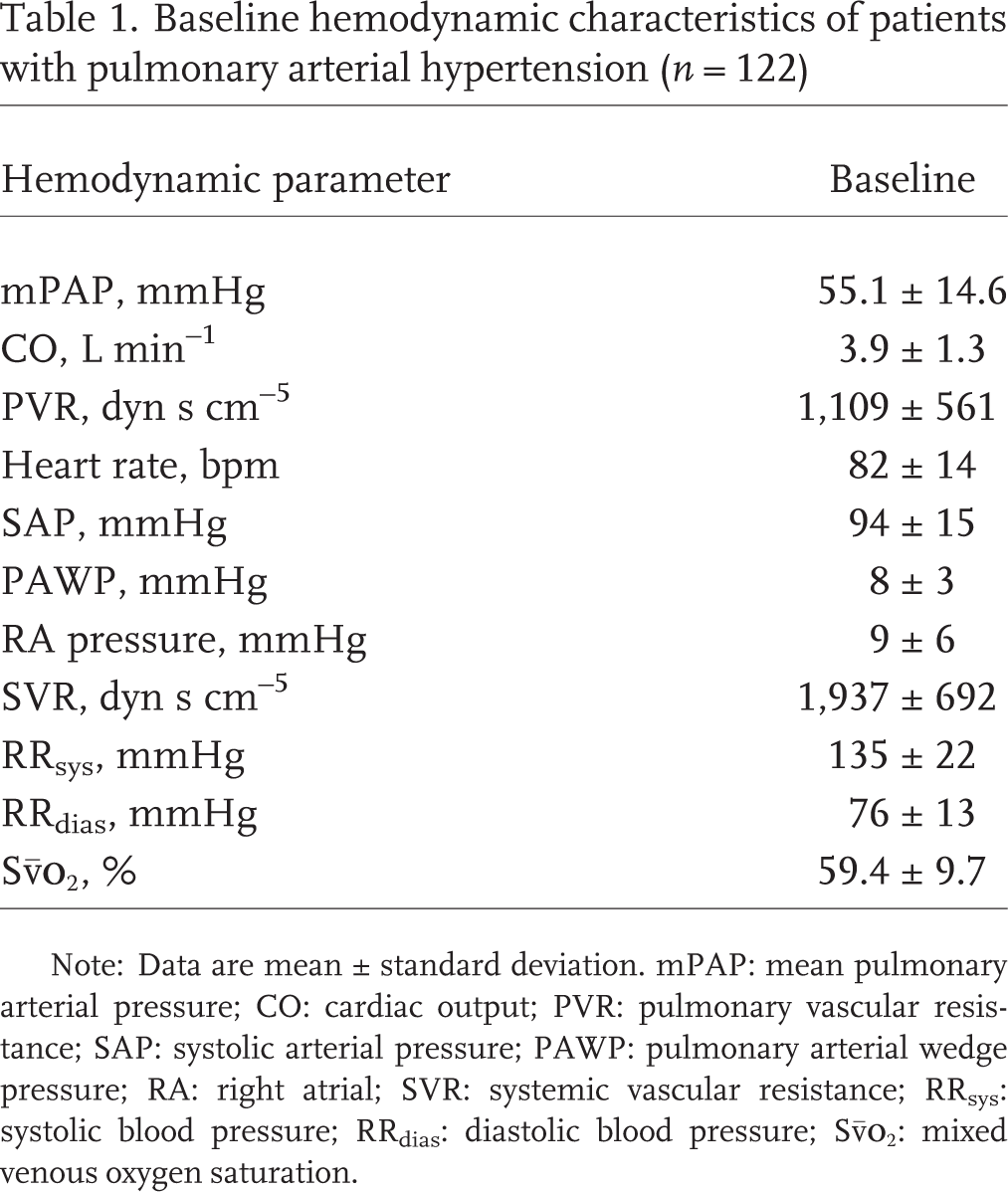
Note: Data are mean ± standard deviation. mPAP: mean pulmonary arterial pressure; CO: cardiac output; PVR: pulmonary vascular resistance; SAP: systolic arterial pressure; PAWP: pulmonary arterial wedge pressure; RA: right atrial; SVR: systemic vascular resistance; RRsys: systolic blood pressure; RRdias: diastolic blood pressure; Sv̄o2: mixed venous oxygen saturation.
Changes in pulmonary hemodynamics at 16 weeks ± 2.5 standard deviations (SDs) and exactly 12–16 weeks after initial right heart catheterization

Note: Data are mean ± SD. mPAP: mean pulmonary arterial pressure; CO: cardiac output; PVR: pulmonary vascular resistance.
Significant change versus baseline (P < 0.001, paired-sample t test).
During the entire observation period (up to 7 years; mean: 4.7), 50 patients (41%) in the study cohort died, and 2 (1.6%) underwent lung transplantation. Kaplan-Meier estimates for transplant-free survival were 93.3%, 76.1%, 57.8%, and 53.1% at 1, 3, 5, and 7 years, respectively (Fig. 2). Survival during the entire observation period was similar in the subset of 59 patients with follow-up RHC at exactly 12–16 weeks (26 patients [44%] died, and none underwent lung transplantation): Kaplan-Meier estimates for transplant-free survival were 93.1%, 74.7%, 58.9%, and 54.0% at 1, 3, 5, and 7 years, respectively.
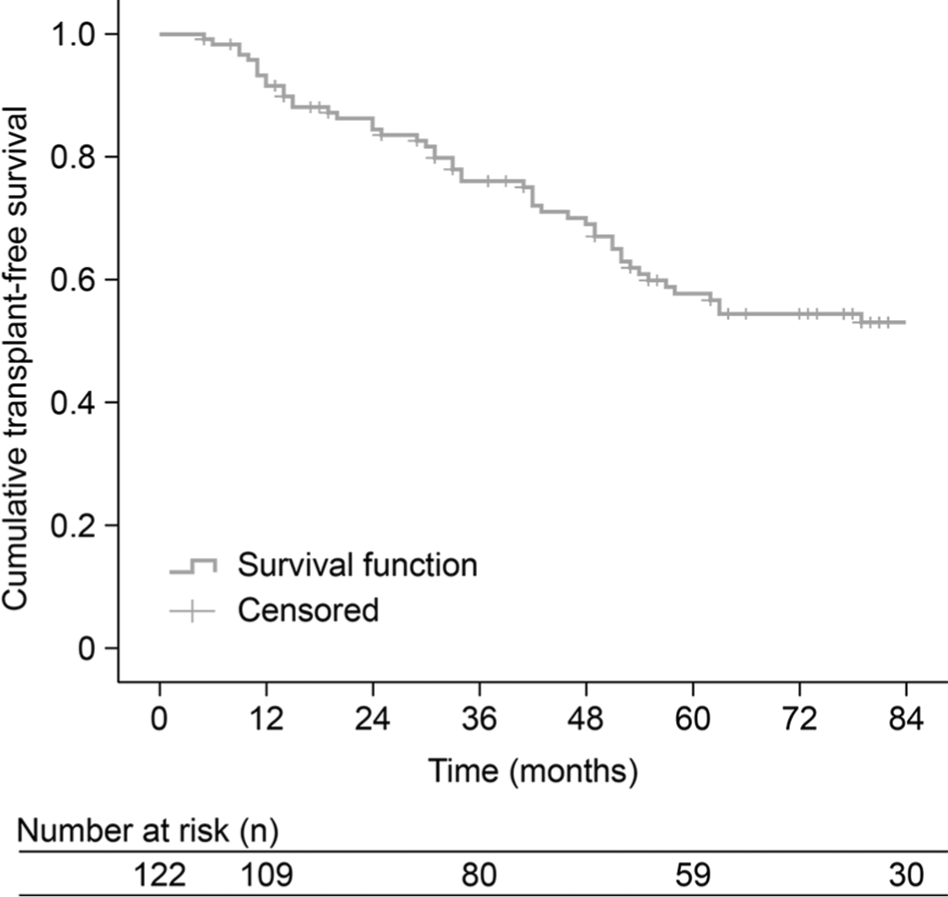
Kaplan-Meier estimates of transplant-free survival among 122 patients with pulmonary arterial hypertension, irrespective of change in hemodynamics. A color version of this figure is available online.
Predictive value of hemodynamic changes for survival
Table 3 lists the results of univariate and multivariate proportional hazards modeling of changes in hemodynamic parameters between baseline and follow-up after 16 weeks ± 2.5 SDs. The improvements in CO from baseline to follow-up, but not the changes in mPAP, were significantly linked to transplant-free survival. This was true for the univariate analyses and the multivariate analyses (which were performed by correcting for the date of diagnosis, diagnostic class, age, and gender).
Univariate and multivariate proportional hazards modeling of changes in hemodynamic parameters between baseline and follow-up of 16 weeks ± 2.5 standard deviations
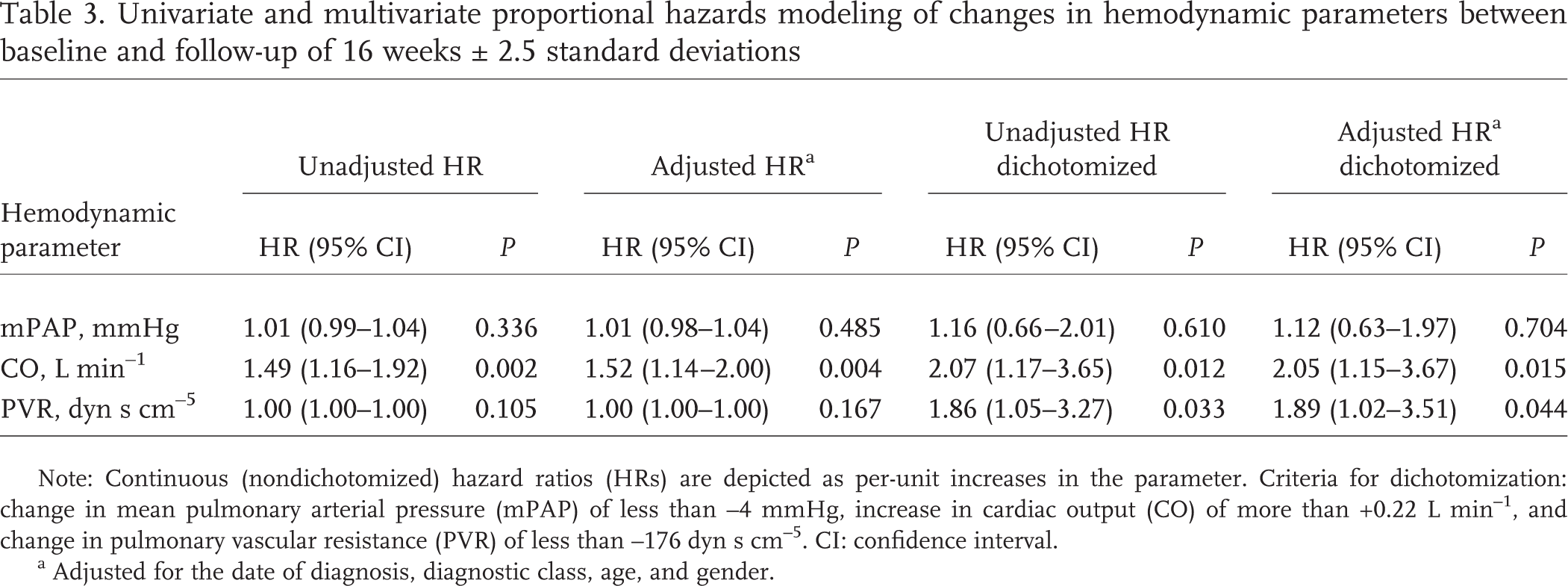
Note: Continuous (nondichotomized) hazard ratios (HRs) are depicted as per-unit increases in the parameter. Criteria for dichotomization: change in mean pulmonary arterial pressure (mPAP) of less than −4 mmHg, increase in cardiac output (CO) of more than +0.22 L min−1, and change in pulmonary vascular resistance (PVR) of less than −176 dyn s cm−5. CI: confidence interval.
Adjusted for the date of diagnosis, diagnostic class, age, and gender.
Cox proportional hazards analyses revealed that the risk group-assigned changes in CO were significantly related to outcome when analyzed in the univariate model and the multivariate model (Fig. 3). Patients who had an increase in CO of more than +0.22 L min−1 (the median observed increase) had a large advantage in transplant-free survival probability compared with patients who had a change in CO of less than +0.22 L min−1. The adjusted HR for dying or undergoing lung transplantation in group 1 compared with group 2 was 2.05 (95% CI: 1.15–3.67; P = 0.015).
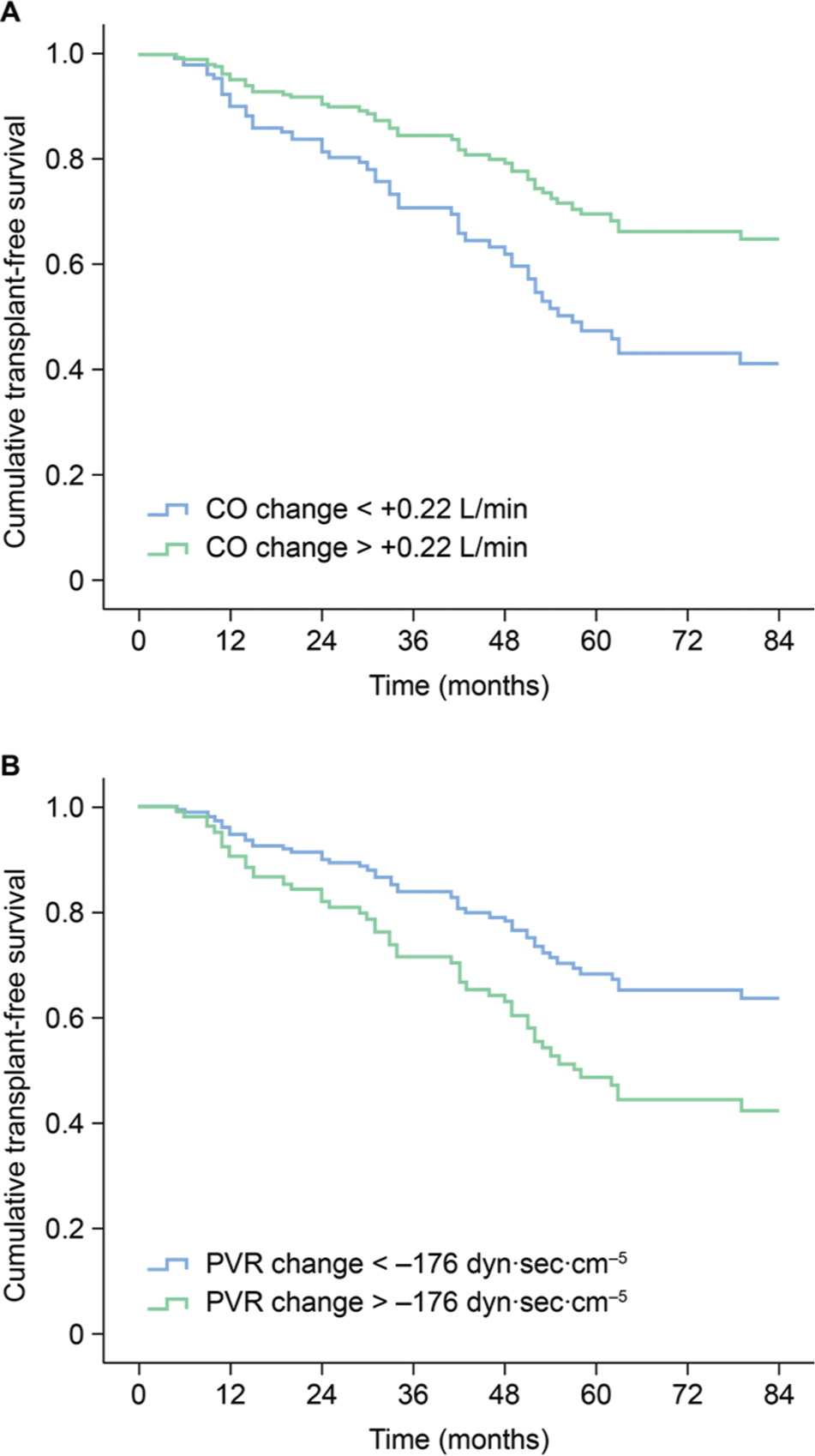
Cox regression plots of predicted transplant-free survival among 122 patients with pulmonary arterial hypertension according to risk group assignation by (A) change in cardiac output (CO) after follow-up of 16 weeks ± 2.5 standard deviations (SDs; group 1 change in CO: less than +0.22 L min−1; group 2 change in CO: more than +0.22 L min−1; P = 0.015) and (B) change in pulmonary vascular resistance (PVR) after 16 weeks ± 2.5 SDs (group 1 change in PVR: less than −176 dyn s cm−5; group 2 change in PVR: more than −176 dyn s cm−5; P = 0.044).
The change in PVR after 16 weeks ±2.5 SDs was not a predictive parameter for transplant-free survival as a continuous variable (Table 3). However, when dividing the patients into 2 groups according to changes in PVR (group 1: less than −176 dyn s cm−5, the median observed decrease; group 2: more than −176 dyn s cm−5), the group with the greater decrease in PVR had a significantly lower risk of dying or undergoing lung transplantation than the group with the smaller decrease in PVR. The adjusted HR for PVR as a dichotomized variable was 1.89 (P = 0.044). Cox proportional hazards analyses showed that the risk group-assigned changes in PVR were significantly related to outcome (Fig. 3). Transplant-free survival at 1, 3, 5, and 7 years was 93.3%, 80.5%, 69.8%, and 64.8%, respectively, in group 1 and was 89.9%, 71.7%, 46.5%, and 42.4%, respectively, in group 2 (log-rank P = 0.029; Fig. 4).
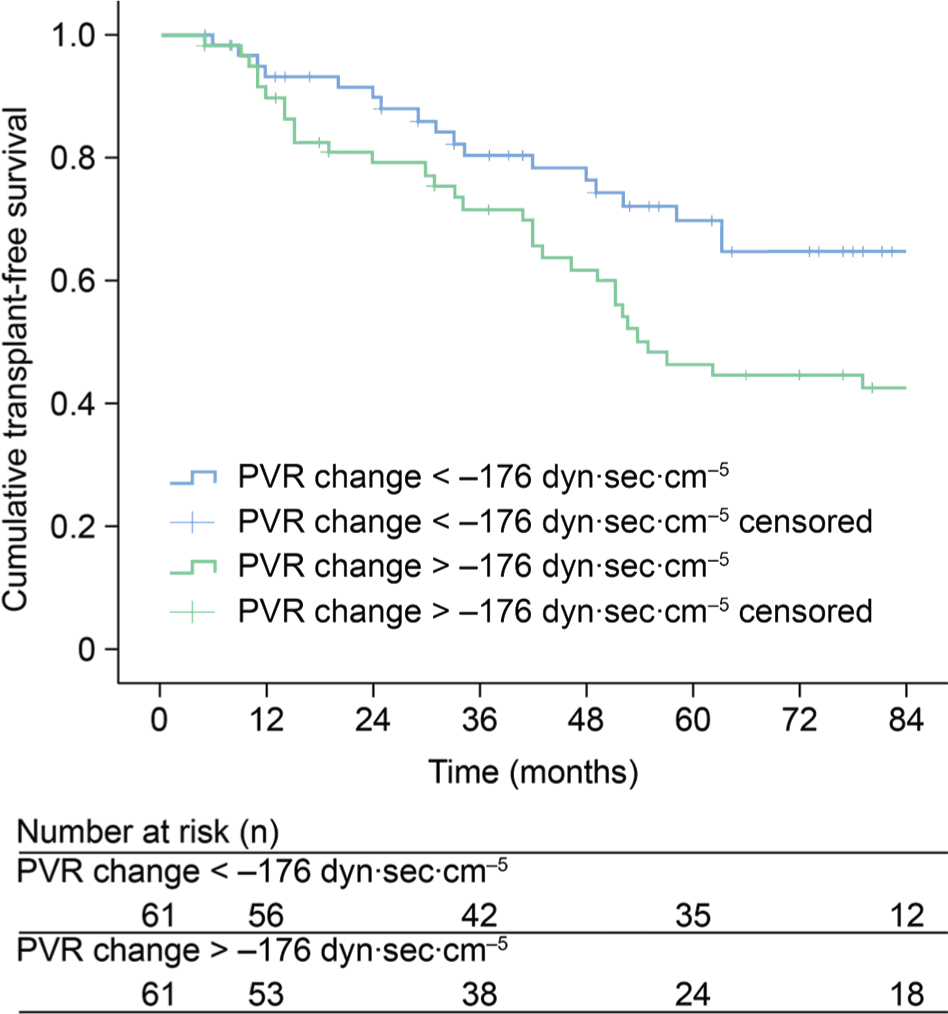
Kaplan-Meier estimates of long-term transplant-free survival in patients with pulmonary arterial hypertension stratified into 2 groups according to change in pulmonary vascular resistance (PVR) after follow-up of 16 weeks ±2.5 standard deviations (group 1 change in PVR: less than −176 dyn s cm−5; group 2 change in PVR: more than −176 dyn s cm−5).
Changes in CO and PVR, but not changes in mPAP, were also significantly associated with transplant-free survival in the subset of 59 patients with follow-up after exactly 12–16 weeks. The adjusted HR was 2.05 (95% CI: 1.26–3.36; P = 0.004) for CO and 1.002 (95% CI: 1.002–1.003; P = 0.047) for PVR. In this patient subset, the HR for CO as a dichotomized parameter was 2.20 (95% CI: 0.98–4.98; P = 0.05), and the HR for PVR as a dichotomized parameter was 2.53 (95% CI: 1.02–6.27; P = 0.045).
Predictive value of changes in WHO functional class and 6MWD for survival
Overall, 65 patients had values for WHO functional class at both baseline and follow-up after 16 weeks ± 2.5 SDs. The distribution of changes in functional class was as follows: 24 patients (37%) improved, 36 (55%) were stable, and 5 (8%) deteriorated. The difference in transplant-free survival was not statistically significant between the 3 groups (log-rank P = 0.058), but a trend toward better transplant-free survival in the improved group was shown. After dichotomization into 2 groups according to change in functional class (group 1: improved; group 2: stable or deteriorated), the difference in transplant-free survival was significant (log-rank P = 0.028). Univariate Cox regression analysis confirmed the results, with short-term change in WHO functional class being a significant predictor of long-term transplant-free survival (HR: 2.9; P = 0.036).
Values for 6MWD at both baseline and follow-up were available for 98 patients. The mean difference was 62 ± 105 m (P < 0.001, paired-sample ttest). The patients were dichotomized into 2 groups according to their change in 6MWD (group 1: <62 m; group 2: >62 m). Transplant-free survival did not differ between the 2 groups (log-rank P = 0.939). Cox regression confirmed the results (HR: 0.976; 95% CI: 0.525–1.817; P = 0.940).
DISCUSSION
The current study showed that individual changes in CO and PVR determined 16 weeks (±2.5 SDs) after initial hemodynamic measurement were highly predictive of long-term transplant-free survival in patients with PAH. In contrast, changes in mPAP did not predict long-term survival in PAH. Of 2 noninvasive parameters assessed, improvement in WHO functional class, but not in 6MWD, was linked to improved long-term survival. Our study cohort consisted of severely ill patients, who had a mean PVR at baseline of 1,109 dyn s cm−5 and of whom 82% were in WHO functional class III or IV. The survival rate in the current analysis was similar to rates reported in the Registry to Evaluate Early and Long-Term PAH Disease Management (REVEAL) and the French PAH registry.3,6 Patient characteristics in our analysis were comparable to those in REVEAL and the French registry in terms of age, gender, and hemodynamics at diagnosis. The proportion of patients in functional class III or IV in the current study (82%) was comparable to that in the French registry study (75%) but was higher than that in REVEAL (54%).
Our data are in line with those from a previous study demonstrating that changes in cardiac index, but not in mPAP, are significantly linked to survival. 22 Data in that study were assessed 6–12 months after the initial RHC, and patients with an improvement in cardiac index of >2.5 L min−1 m−2 showed a significantly better outcome during a 5-year observational period than patients with lesser improvement. The improvement in PVR at 6–12 months was not linked to better survival in that study. However, similar to our results, for reevaluation after exactly 3–4 months a decrease in PVR of more than ~15% was also significantly associated with survival. 22
Generally, baseline hemodynamic variables that reflect right ventricular function (CO, RA pressure, and Sv̄o2) have predictive value superior to that of mPAP or PVR. 15 However, with respect to individual changes in hemodynamic parameters, results vary depending on the time points of follow-up and initial therapy as well as, possibly, differences in statistical analysis. In this regard, the following parameters have been reported to be associated with better outcome during prostanoid treatment: a significant reduction in PVR of >30% relative to baseline after 3 months of treatment; 7 a substantial improvement in PVR, mPAP, and cardiac index reassessed after 12–18 months of treatment; 17 and an improvement in mPAP and cardiac index after the first year of therapy. 8 A decrease in PVR after 4 months of bosentan treatment was also associated with improved long-term outcome after 2 years. 6 Independently of drug treatment, an association with an increased risk of death was reported for increased mean RA pressure, increased PVR, and decreased cardiac index in a univariate analysis and for mean RA pressure and cardiac index in a multivariate analysis when assessed after 6–12 months. 14
The consistent results regarding the cardiac index as a prognostic value emphasize the relevance of improvement in cardiac function as a predictive value for outcome in PAH. The importance of right heart performance for outcome in PAH was supported by a study that included measurements with cardiac resonance tomography (CRT). 12 In that study, changes in stroke volume (determined by CRT or RHC) and mean RA pressure, but not in mPAP, after 1 year of follow-up were associated with survival.
In terms of prognostic value, the noninvasive parameter 6MWD was not as reliable as hemodynamic parameters in the current study. Previous studies of the relationship between short-term changes in 6MWD and long-term outcomes have reported mixed results. For example, the change in 6MWD after 3 months of ambrisentan treatment in randomized controlled trials (n = 370) did not discriminate 2-year survival, 23 and the change in 6MWD determined after 6–12 months of treatment with different PAH therapies was not associated with 5-year outcome in a cohort of 109 patients. 22 Conversely, a retrospective review of 811 patients enrolled in randomized controlled trials of subcutaneous treprostinil found that an increase in 6MWD after 3 months was associated with improved survival at 3 years. 24 A similar connection was shown for improvement in 6MWD and survival during bosentan treatment (n = 103). 6 Reasons for the inconsistency between studies could include differences in patient characteristics, variations in the performance of the 6MWD test, size of the study population, and duration of follow-up.
The results of the current study reaffirm the recommendation of the current European guidelines to perform RHC after 3–4 months of therapy initiation or change in therapy. 15 However, there is no universally accepted guideline about how and when to reassess patients. US guidelines recommend the performance of RHC when clinical deterioration is detected or after 6–12 months in clinically unstable patients. 20 The time period of 3–4 months for reevaluation and timely escalation of therapy is favorable against the background that the strategy of early intervention, before clinical deterioration becomes severe, is demanded in modern PAH management. 19 Currently, a so-called goal-oriented strategy uses noninvasive parameters derived after 3–4 months of treatment for categorizing patients into “stable” or “unstable” groups as a basis for deciding about treatment escalation. 4 Additional inclusion of invasive parameters after 3–4 months of first-line treatment to distinguish stable from unstable patients may be useful. 25 Our study supports the concept of invasive reevaluation 3–4 months after treatment initiation or escalation of therapy for further therapeutic decision making. Furthermore, our analysis provides some evidence for the practice of clinical trials performing RHC 3–4 months after study initiation. Clinical trials studying PAH therapies have been criticized for being short-term studies of usually 12–16 weeks' duration that are not powered to detect a survival benefit. 20 By demonstrating that changes in hemodynamic parameters during this time frame predict long-term survival, our data support the rationale for use of this approach in clinical trials.
The current study also supports the arguments of Nickel et al. 22 to include dynamic changes of individual patients' characteristics into risk score equations. Currently, the scoring systems are mainly derived from baseline variables, either relying solely on hemodynamic variables13,14 or including noninvasively derived parameters as well.3,16 However, their use may be limited because prognosis may change with response to therapeutic interventions. Individual risk assessment should take into account the response to therapy, as ~40% of patients changed their risk category between baseline and follow-up. 22 Thus, there is a “need for assessment at multiple follow-up time-points (dynamic assessment) to evaluate the impact of time-dependent variables on clinical outcomes.” 26 The change in CO and PVR after 3–4 months may be one of these follow-up variables.
Recently, a meta-analysis of data from 10 randomized controlled trials demonstrated that the change in short-term hemodynamic parameters during different PAH-targeted therapies when applied to the National Institutes of Health equation for prediction of prognosis underestimated survival in comparison to the 1-year survival reported in several open-label and registry studies with PAH-specific therapies. 27 This result emphasizes the predictive value of changes in hemodynamic parameters for prognosis but also the need for more accurate risk score systems that include hemodynamic changes in their calculations.
Limitations of the current study include the moderate sample size (n = 122). Additionally, a selection bias cannot be excluded because we selected only patients with PAH for whom hemodynamic data for both time points were available from our registry.
We conclude that change in CO and PVR over 16 weeks (±2.5 SDs) is a strong predictor of long-term survival in patients with PAH, on the basis of real-life data from the single-center Giessen Pulmonary Hypertension Registry.
