Abstract
Depression that is present during pregnancy is associated with poor maternal and infant outcome [1–20]. The unique opportunities afforded by the perinatal period have also been highlighted [21], [22]. Buist et al. [23] state that screening for depression during the perinatal period is a strategy that ‘provides an opportunity to access large numbers of women and facilitate pathways to best-practice care’ (p. s101). However, they also note that a controversy has emerged regarding whether such an approach is premature. Concern has been raised regarding the lack of evidence for the acceptability of an approach involving screening for perinatal depression followed by treatment [24].
How acceptable is it to women to be screened for depressive symptoms during pregnancy, be asked to participate in an additional assessment, and be offered an intervention? Studies report that over 95% of pregnant women are willing to complete a depression screening questionnaire [25], [26]. A much lower proportion of suspected cases appear willing to co-operate with additional assessment and to proceed with an intervention (especially randomization to an intervention), if appropriate. For example, studies have reported that up to a half of eligible pregnant women identified through screening did not complete assessment and agree to randomization [25], [26].
A number of factors make it difficult to draw firm conclusions from the existing studies. Screening has been performed in either problematic or diverse ways depending on the specific purpose of the study. For example, some studies have not specified exactly what pregnant women were screened for [27], have excluded women who currently meet criteria for major depression [26], or have screened for risk factors for subsequent (postnatal) depression, rather than for current depressive symptoms [28], [29]. Other studies [27], [30] have not made it clear when drop outs occurred, making it difficult to determine which aspects of a study design are most likely to elicit drop outs (i.e. screening, interviewing or randomization). Also, low rates of recruitment and retention may reflect the unacceptability of an intervention, rather than the unacceptability of screening. The most commonly provided intervention has been attendance at special antenatal classes [25], [27], [29], [30], which may not be appealing to pregnant women [27].
The present study sought to evaluate the recruitment and retention of depressed pregnant women, identified initially through screening, to a randomized controlled treatment trial involving cognitive behaviour therapy versus routine clinical care.
Method
Overview
This investigation had four key stages: (i) screening of pregnant women for depressive symptoms; (ii) initial assessment of women selected from screening in order to recruit a sample of pregnant women who meet criteria for major depression; (iii) treatment of depressed women involving randomization to one of two treatments: cognitive behaviour therapy (CBT) or routine clinical care (RCC); and (iv) follow-up assessments at 6 weeks following initial assessment (mid assessment), 36 weeks gestation (end assessment) and 4 months postdelivery for all participants (postpartum assessment).
Participants and recruitment procedure
Participants were consecutive pregnant women (12–22 weeks gestation) who were presenting for routine ultrasound scan at one of two clinics. Women were approached by a receptionist and asked to complete the Edinburgh Postnatal Depression Scale (EPDS) [31] while they waited for their scan. An additional question asked women to indicate if they agreed to be contacted by our research co-ordinator if their answers to the EPDS questions suggested that depression may be a problem for them. Women placed the completed form in a secure box placed in the waiting room. Stamped, addressed envelopes were also provided in case women wished to complete the form at home and post us their response.
Women who scored greater than 12 on the EPDS and agreed to be contacted, were phoned by our research co-ordinator, questioned briefly to ensure that they were potentially suitable (e.g. appropriate age and gestation), and invited to attend an initial assessment. This assessment, and the other face to face interviews, were conducted either at our offices or participants' own homes depending on their preference. The interviewer was a woman with postgraduate qualifications in psychology, experience as an interviewer with previous psychological studies involving parents, and a practising mid-wife. Women were potentially eligible for the study if they provided informed written consent and met the following criteria at initial assessment. Inclusion criteria: Currently aged 16 years or over, in the second trimester of pregnancy, meets criteria for major depressive disorder [32], and has a mid-wife/obstetrician/general practitioner (or agrees to be assigned one), with whom we may communicate. Exclusion criteria: Current severe depression, psychotic depression, bipolar I disorder, schizophrenia, severe alcohol or drug dependence, severe medical problems interfering with treatment, a developmental learning disorder or cognitive impairment contraindicating psychotherapy, or currently receiving active treatment (medication or psychotherapy) for a depressive disorder.
Measures
At screening, a cut off of greater than 12 on the EPDS [31] was used because this has been shown to have a sensitivity of 100% (specificity 87%) for identifying cases of major depression amongst pregnant women [33].
At initial assessment, the interviewer evaluated whether inclusion and exclusion criteria were met through conducting a clinical review and completing the relevant sections of the Structured Clinical Interview for DSM-IV axis I disorders (SCID); [34]. The EDPS was repeated as a measure of current depressive severity [31]. The primary outcome measure reported here was the presence/absence of a current diagnosis of a major depressive disorder as assessed by the SCID [34]. This was assessed at end and postpartum assessments. At mid assessment, a postal EPDS was conducted. Treatment received (if any) and satisfaction with treatment was assessed by questionnaire at each assessment.
Treatment
Cognitive behaviour therapy [35] involved 12 sessions of individual therapy of approximately one hour duration. We decided prior to the study to consider treatment completed if at least 8 sessions of CBT were attended. Compensation was provided for childcare expenses associated with attending therapy.
Routine clinical care involved treatment being left to the discretion of the lead maternity provider, in consultation with the participant.
Results
Participant flow
Figure 1 shows a summary of subject flow across the study. Receptionists gave 400 EPDS forms to pregnant women presenting for routine ultrasound scans. A high proportion of these forms were completed and returned to us (92.5% 370/400). Of the women who completed the EPDS, 13.2% (49/370) scored greater than 12. However, despite depression being likely amongst these women, only 30.6% (15/49) agreed to contact from us.
Summary of participants and flow across study design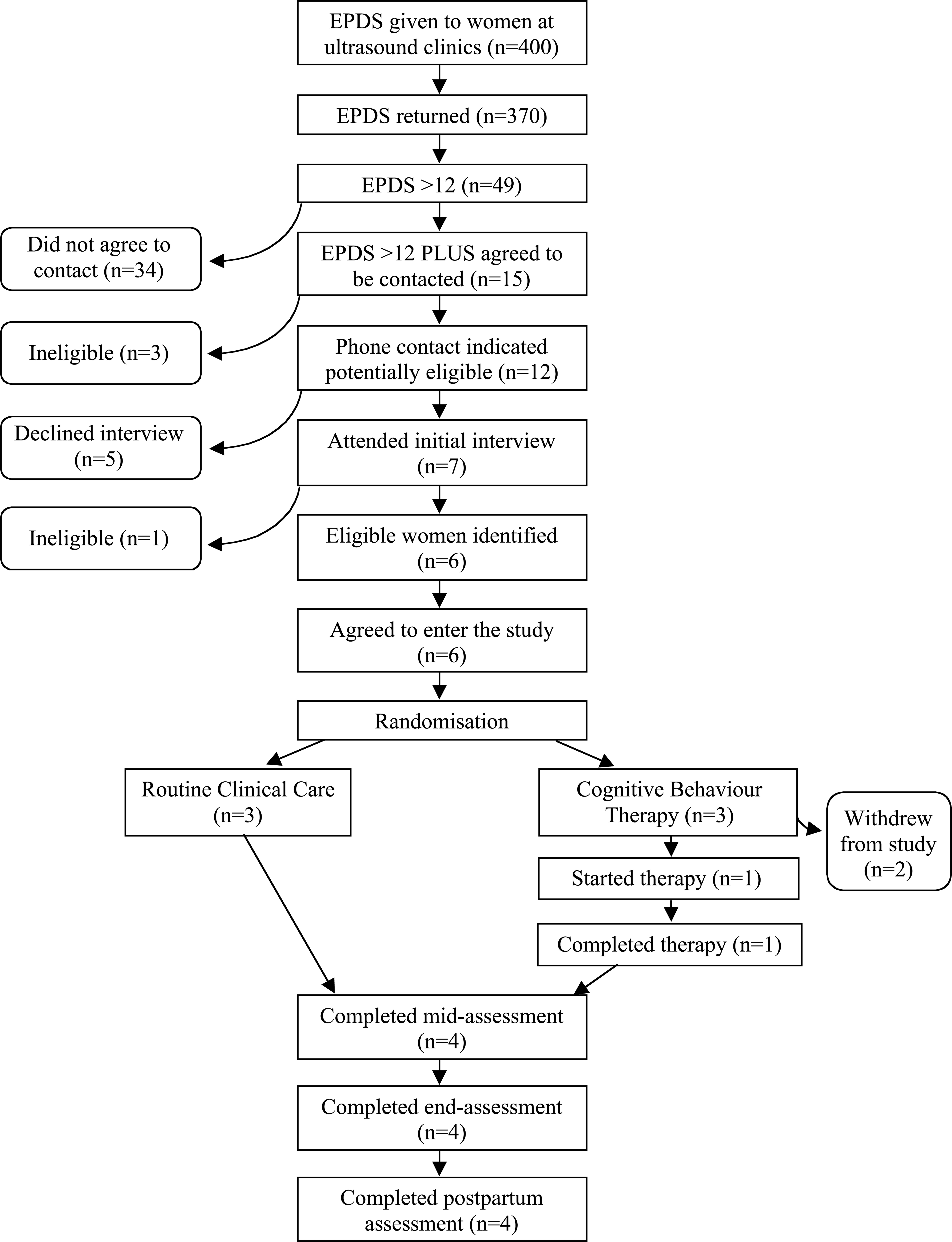
Of these 15 women who agreed to contact, three were ineligible for the study because they were currently on antidepressants (n = 2) or were no longer pregnant (n = 1). A further five women declined the offer of an initial interview for the following reasons: ‘My GP has told me I'm not depressed, considering the circumstances [i.e. being pregnant]’ (n = 1); ‘I don't think I'm depressed enough’ (n = 1); ‘I don't want to be labelled’ (n = 1); ‘I'm too shy’ (n = 1); and no reason offered (n = 1). None of the women contacted reported having had an abnormal ultrasound scan.
Of the seven women who attended an initial interview, all were eligible except for one participant who did not have sustained low mood. All of the six eligible women consented to participate in the study. Three women were randomized to CBT and three were randomized to RCC. Of the three women randomized to CBT, only one commenced therapy. The other two women chose not to commence CBT because they felt that they did not need treatment at the moment and they knew where to get help if they needed it. The one woman who did commence CBT, plus the three women randomized to RCC, completed all subsequent assessments (mid, end and postpartum).
Characteristics of the sample
Total sample at initial screening (n = 370)
Figure 2 shows the distribution of EPDS scores across the 370 participants that completed the EPDS at screening. These scores were not normally distributed. The mean EPDS score was 6.9 (4.9) and the mean gestational age was 16.7 (3.7) for the total sample at screening.
Distribution of EPDS scores at screening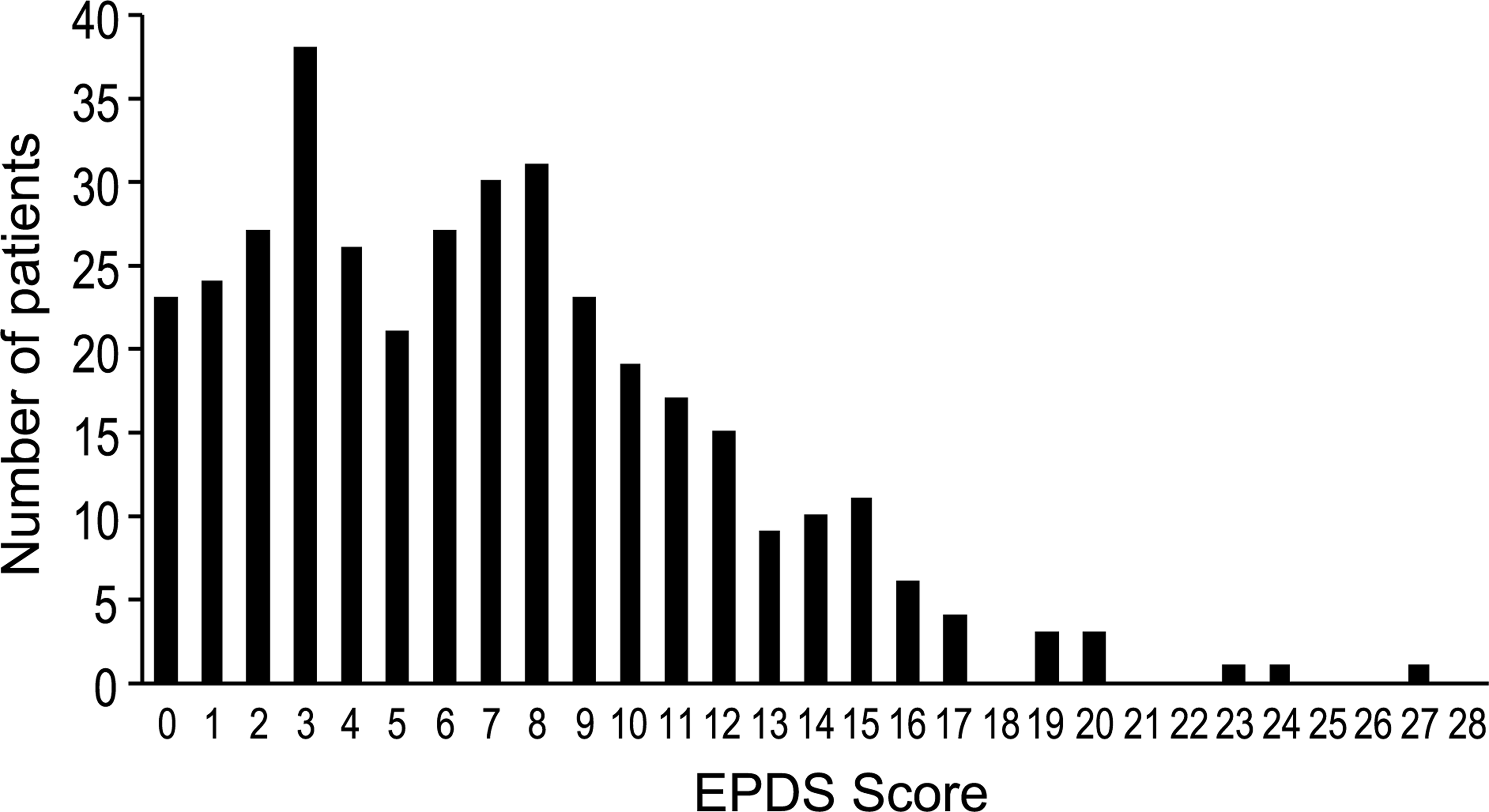
Participants who scored greater than 12 on the EPDS at initial screening (n = 49)
Amongst the 49 women (13.2%) who scored greater than 12 on the EPDS at initial screening, the mean EPDS score was 15.9 (3.0) and the mean gestation was 16.1 (3.3). Women who agreed to be contacted following screening had significantly higher EPDS scores (no contact = 15.2 (2.4), contact = 17.5 (3.7); p = 0.01 using independent samples t-test), and were significantly more likely to have endorsed thoughts of self-harm on item 10 of the EPDS (p = 0.03 using χ2) than those who did not agree to contact.
Treatment received and treatment outcome
The single participant who commenced CBT completed 11 sessions, which she rated as being ‘very valuable’. One of the three participants' randomized to RCC received three sessions addressing her depression with her lead maternity provider, which she rated as being ‘extremely ineffective’. No other assistance for depression was received by any participants over the course of the study. By definition, all participants had a major depressive disorder at initial assessment. By end assessment, none of the participants met criteria for major depressive disorder.
Discussion
The purpose of this study was to evaluate the recruitment and retention of depressed pregnant women to a randomized controlled trial. Women were initially identified through screening for depressive symptoms at a routine ultrasound scan appointment in the second trimester of pregnancy. While the vast majority of women were willing to complete the screening questionnaire, severe losses occurred subsequently. Overall, this was not an effective recruitment strategy.
The present study clarifies which points of a study design are more vulnerable to participants choosing not to continue. As expected [25], [26], the vast majority of women (93% 370/400) completed the EPDS. Also as expected [33], [36], approximately 13% (49/370) of these women scored greater than 12. However, few of these women with ‘probable depression’ [38] were recruited or retained by the trial. Losses occurred primarily at three critical points in the study design.
First, most women who scored greater than 12 on the EPDS did not agree to be contacted following screening. This was the single most likely point for women to choose not to continue with the study. Women who were more symptomatic on the EPDS were significantly more likely to agree to be contacted. Beyond this, the reasons for women stating that they did not wish to be contacted are not clear. As part of our ethical agreement, participants right to withdraw/decline to enter a study without needing to give a reason, was respected. Exploring, in an ethical manner, potential barriers to accepting assistance is an important issue that warrants evaluation in its own right.
Second, even if women did agree to be contacted, most did not attend the initial interview. More commonly this was because they declined the interview rather than because they were ineligible.
Third, even if women did attend the initial interview, were eligible, and were consenting, most women did not receive treatment for their depression. If they had been randomized to CBT, this was because most chose not to commence treatment. If they had been randomized to RCC, this was because most were not treated or referred for their depression by their lead maternity provider.
The results of the present study are consistent with other studies that have reported difficulties recruiting pregnant women to trials involving screening for depressive symptoms and the provision of an intervention [25], [26]. However, some studies have obtained more optimistic recruitment rates. For example, Stamp [28] and Wolman [37], respectively, recruited 80% and 99% of eligible women who could be located. What these studies have in common is that they identified ‘at risk’ pregnant women and offered them an intervention that was of low burden to them (weekly telephone calls from a volunteer or a companion during labour). The issue of the burden of treatment may be especially relevant for pregnant women who already have children, as these women have been noted to be more likely to decline an intervention [30].
It is unclear if the difficulties encountered by the present study are specific to pregnant women, or if they apply more broadly. A comprehensive review of randomized controlled trials of screening for depression in the general adult population concluded that screening can improve outcomes over usual care, especially when combined with system changes ensuring adequate treatment and follow-up [38]. However, many difficulties have been identified with efforts to address unmet psychiatric need [39]. Most published studies evaluating screening for postpartum depression have only indirectly addressed the issue of acceptability [40]. Shakespeare et al. [41] directly assessed acceptability and concluded that routine screening using the EPDS was less than acceptable to the majority of postpartum women interviewed. Certainly studies involving screening and treatment for depression following childbirth have reported variable recruitment rates [e.g. 42–47].
It is important to consider if any methodological factors can account for the present results. Efforts were made to make it easier for women to participate in the study by giving them the option of being seen in their own home (all the women who were assessed chose this option), and providing compensation for childcare for those women randomized to CBT. It is possible that higher rates of acceptance would have been obtained if screening had been conducted by a health professional that the women had a relationship with (e.g. their midwife), rather than by an unknown receptionist offering them a form to fill out. However, a similar study involving endorsement and presentation of the study by the participant's paediatrician also reported major difficulty with recruitment [47].
It is unclear if screening at the time of ultrasound scan was problematic for some women. While women were presenting for routine ultrasound scans, some women may have felt sensitive at this time, which could have influenced their willingness to be contacted about the study. None of the women who agreed to be contacted reported having had an abnormal scan.
The present results may also be specific to a randomized controlled trial and may not generalize to a more naturalistic setting. For example, it could be that the prospect of randomization was unappealing to women, and therefore discouraged them from agreeing to contact following screening. This may be especially relevant for this particular study as it involved a fifty percent chance of participants receiving routine clinical care. However, studies involving screening and treatment for postpartum depression without randomization, have also reported low rates of acceptance of assessment [46], [47]. Robinson and Young concluded that their study illustrated the ‘considerable lack of acceptability of treatment originating from screening that had not been initiated by the client’ (p. 50).
What are the implications of this study? The present study showed that most women who were pregnant and suffering from ‘probable depression’ did not agree to participate in the study. This raises concerns about how representative pregnant women who participate in trials involving screening and randomization to treatment are of pregnant depressed women in general. Thus, the results of treatment trials involving screening and randomization to treatment may not generalize well to the broader population of pregnant depressed women. It is not known if this concern about the generalisability of results is specific to pregnant depressed women, or if it extends to all trials involving screening and treatment. Moreover, the present results may have implications for public health strategy. It should not be assumed that there would be widespread acceptance of help for depression amongst pregnant women identified initially through screening.
Further research is needed into the acceptability of different approaches to identifying and treating depression during pregnancy. In particular, it may be useful to examine the role of mid-wives in the recognition of depression during pregnancy. In the present study, women were happy to complete a screening questionnaire, but were largely unwilling to be contacted by an unknown health professional. Pregnant women may be more willing to do so if such contact was endorsed by their mid-wife. This hypothesis requires evaluation. However, mid-wives themselves may be reluctant to refer women for psychological help. Of the three women randomized to routine clinical care, none were referred for psychological assistance and only one received help for her low mood from her lead maternity provider. This assistance was viewed by the woman as being unhelpful. Despite this, none of the participants in the study remained depressed at end assessment and postpartum assessment.
This trial was not designed to evaluate the effectiveness of CBT versus routine clinical care. Instead, it was designed to evaluate a potential recruitment strategy for such a trial. Although the recruitment strategy was unsuccessful, it is still important to establish if systematic treatment of depression during pregnancy offers advantages over simply recognizing depression and alerting key care givers. If demonstrated, this may help make seeking treatment for depression more acceptable to pregnant women and their care givers.
In conclusion, the present study found that while the vast majority of pregnant women were willing to complete a depression screening questionnaire, most did not agree to additional contact or assessment, and either were not offered treatment or did not accept treatment. This was not an effective recruitment strategy for a randomized controlled psychotherapy trial.
Footnotes
Acknowledgements
This research was supported by the Canterbury Medical Research Foundation.
