Abstract
Background
To evaluate a novel, unofficial, trainee-organized, hospital addiction medicine consultation service (AMCS), we aimed to assess whether it was (1) acceptable to hospital providers and patients, (2) feasible to organize and deliver, and (3) impacted patient care.
Methods
We performed a retrospective descriptive study of all AMCS consultations over the first 16 months. We determined acceptability via the number of referrals received from admitting services, and the proportion of referred patients who consented to consultation. We evaluated feasibility via continuation/growth of the service over time, and the proportion of referrals successfully completed before hospital discharge. As most referrals related to opioid use disorder, we determined impact through the proportion of eligible patients offered and initiated on opioid agonist therapy (OAT) in hospital, and the proportion of patients who filled their outpatient prescription or attended their first visit with their outpatient OAT prescriber.
Results
The unofficial AMCS grew to involve six hospital-based residents and five supervising community-based addiction physicians. The service received 59 referrals, primarily related to injection opioid use, for 50 unique patients from 12 different admitting services. 90% of patients were seen before discharge, and 98% agreed to addiction medicine consultation. Among 34 patients with active moderate-severe opioid use disorder who were not already on OAT, 82% initiated OAT in hospital and 89% of these patients continued after discharge.
Conclusions
Established in response to identified gaps in patient care and learning opportunities, a novel, unofficial, trainee-organized AMCS was acceptable, feasible, and positively impacted patient care over the first 16 months. This trainee-organized, unofficial AMCS could be used as a model for other hospitals that do not yet have an official AMCS.
Introduction
Many hospitalized patients have illnesses caused by substance use disorders. 1 , 2 Inpatient addiction medicine consultation services (AMCS) are associated with improved retention in care and reduced substance use after hospital discharge, 3 – 6 and emerging evidence suggests AMCS may be associated with decreased mortality and readmissions among patients who inject drugs. 7 – 10 AMCS also provide important learning opportunities. Hospital-based medical trainees care for patients with substance use disorders every day, yet describe insufficient training in addiction medicine. 11 –13
In order to fill identified gaps in patient care and training experiences, medical trainees at an academic, tertiary care center in Atlantic Canada organized an unofficial AMCS. Here, we describe the implementation and evaluation of the service over the first 16 months. We aimed to assess whether the novel, trainee-run service was (1) acceptable to hospital providers and patients, (2) feasible to organize and deliver, and (3) impacted patient management during and after hospitalization.
Methods
Setting and participants
This study took place at the Queen Elizabeth II Health Sciences Center (QEII HSC), a 661-bed, university-affiliated, tertiary care center in Halifax, Nova Scotia, Canada. QEII HSC does not have an official AMCS, and inpatient addiction medicine care has been provided through ad hoc phone calls to community-based addiction physicians with outpatient practices nearby.
Project description
Starting in June 2018 with one hospital-based internal medicine resident supervised by one community-based addiction physician, the AMCS was advertised through word-of-mouth and Grand Rounds presentations. More hospital-based trainees and community-based addiction physicians expressed interest, and a team was organized with regular e-mail contact and weekly clinical and educational meetings. As the service is not listed with hospital locating, referrals are received by word-of-mouth or phone calls to hospital-based trainees, or through phone calls/faxes to community-based addiction physicians. Trainee organizers assign referrals to a trainee-supervisor pair. Trainees usually see patients after regular work hours, and review cases by phone. One community-based addiction physician attends the hospital weekly to review patients in person. The unofficial AMCS incorporates motivational interviewing, medications, harm reduction education, training and dispensing of take-home naloxone kits, referrals to community-based services including addiction counseling and harm reduction agencies, education initiatives, and research.
Evaluation plan
This retrospective program evaluation was deemed exempt from requirements for Research Ethics Board approval and individual patient consent by Nova Scotia Health Authority.
To determine whether the trainee-run AMCS was acceptable to hospital providers and patients, we counted the number of referrals received from different admitting services and calculated the proportion of referred patients who consented to consultation once they were approached by AMCS trainees.
To determine whether the service was feasible to organize and deliver outside of regular work hours, we assessed whether the service continued or grew over the evaluation period, and calculated the proportion of consultations successfully completed before patients’ hospital discharge.
To determine whether the AMCS positively impacted patient care, we described a cascade of care among referrals for patients with opioid use disorder by calculating the proportions of eligible patients who were offered and initiated opioid agonist therapy (OAT; methadone, buprenorphine, or slow-release oral morphine) in hospital, and the proportion of patients who continued on OAT after discharge. We identified patients as continuing on OAT after discharge if they either filled their hospital discharge prescription from the AMCS at an outpatient pharmacy (confirmed through the provincial pharmacy information system) or attended their planned post-hospital follow-up visit with their community-based OAT provider (confirmed through report from the community-based OAT provider, who are all members of the program evaluation team).
Results
Over the 16 month study period, June 2018 to September 2019, the unofficial AMCS grew from one hospital-based first-year internal medicine resident and one community-based addiction physician to six hospital-based residents (internal medicine, anesthesia, and psychiatry; 83% men, 17% women) and five community-based addiction physicians (all family medicine-trained; 60% men; 40% women). By September 2019, one resident was in postgraduate year (PGY) 3, four residents were in PGY2, and one resident was in PGY1.
The service received 59 referrals in total for 50 unique patients. Each referral was associated with a separate hospital admission; six patients had referrals from two hospital admissions each, and one patient had referrals from four hospital admissions. Referrals were received from 12 different admitting services, including Internal Medicine, Cardiology, Cardiac Surgery, Acute Pain Service, Psychiatry Consultation-Liaison, and others (Supplement Table 1). Internal Medicine referred most of the patients, and over 25% of referred patients had injection drug use-associated infective endocarditis (Supplement Table 2). Fifty-five (93%) referrals related to opioid use and 56 (95%) related to injection drug use.
Of the 59 total referrals received, AMCS trainees were able to see 53 (90%) before hospital discharge. Among the six unseen referrals, two (33%) of the patients self-initiated discharge against medical advice, three were discharged home by the admitting service, and one was transferred back to their local regional hospital. Out of the 53 consultations successfully initiated before patient discharge, during 52 (98%) the patient consented to proceed with addiction medicine consultation.
Of 55 referrals related to opioid use, for 49 (89%) the patient was successfully approached before hospital discharge (Figure 1). Forty-eight of these 49 (98%) patients consented to addiction medicine consultation; however, two of these patients died from their medical illness soon after being seen. Forty-five of 46 (98%) surviving patients had active moderate-severe opioid use disorder, and OAT was indicated. Eleven of 45 (24%) patients were already on OAT when admitted, but 10 of 11 (91%) of these patients required OAT dose adjustments due to pain or withdrawal. OAT was offered to all 34 remaining eligible patients. Twenty-eight of 34 (82%) patients accepted OAT initiation in hospital. Twenty five of 28 (89%) of these patients continued OAT after discharge (Figure 1).
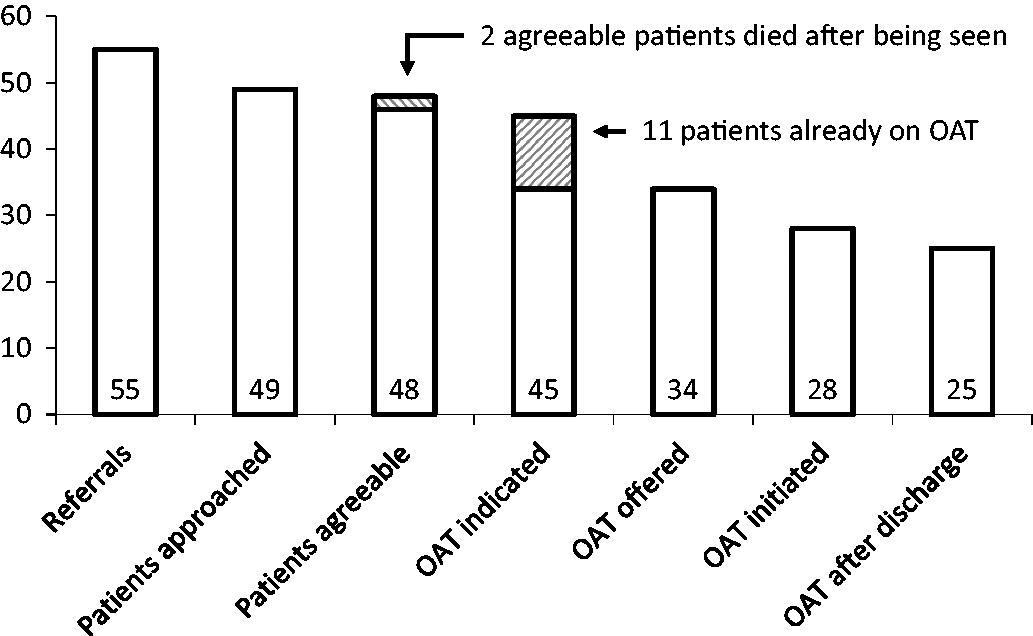
Summary of the cascade of care for patients with opioid use disorder referred to an unofficial hospital addition medicine consultation service, organized by medical trainees. OAT: opioid agonist therapy.
Discussion
We found that a trainee-organized, unofficial AMCS was acceptable to patients and admitting services, feasible to organize and deliver, and impacted patient care at an academic tertiary-care hospital over 16 months. Most referrals related to opioid use disorder, and many patients had injection drug use-associated infective endocarditis. Most eligible patients accepted OAT initiation in hospital, and also continued on OAT after discharge. This trainee-organized, unofficial AMCS could be used as a model for other hospitals that do not yet have an official AMCS.
Multiple factors may have helped the service succeed. The service used existing resources, including take-home naloxone kits provided by a public program, and community partnerships, including hospital in-reach from a local harm reduction agency. The supervising community-based addiction physicians were already well-known in the community, which may have helped build trust between patients and trainees. Because they were involved in in-hospital care, the community-based physicians were able to establish relationships with specific patients and follow-up in their own clinic after discharge, which may have improved the rates of treatment continuation. Residents and hospital pharmacists both rotate across multiple services at QEII HSC, which likely increased awareness of the AMCS.
Some organizational and philosophical challenges to the service exist. The AMCS is “unofficial” in that it is not formally recognized, resourced, or remunerated, nor is it listed with hospital locating at the academic medical center where it is located. Financial resources and administrative support would be important to improve capacity and long-term stability. 14 The AMCS introduced multiple new practices that were unfamiliar to hospital clinicians at the QEII HSC, including treatment of opioid withdrawal with opioids, in-hospital OAT initiation, take-home naloxone kits, and referral to harm reduction and needle exchange services. Treatment of withdrawal and OAT initiation in hospital helps support patients to stay in hospital and participate in their medical care, 15 , 16 which also led to positive feedback for the AMCS from nursing colleagues. Ongoing education sessions and Grand Rounds lectures in multiple hospital departments introduced concepts of harm reduction and trauma-informed care, with which many hospital clinicians were not previously familiar. 17 –19
The most common medical diagnosis was injection drug use (IDU)-associated infective endocarditis. This is an increasingly prevalent problem in North America, in the context of the current opioid crisis. 2 , 20 Many hospital-based physicians are not comfortable providing care to patients who inject drugs, 11 , 12 , 21 and patients with IDU-associated infective endocarditis are particularly vulnerable to poor outcomes if there is suboptimal management of addiction, withdrawal, and pain. 15 , 16 , 21 , 22 Retrospective cohort studies suggest that AMCS are associated with increased rates of OAT, 5 , 8 and that AMCS and OAT are associated with decreased mortality, 7 , 23 overdose 9 , and hospital re-admissions 9 among patients with IDU-associated infective endocarditis. 8 , 10 While these findings on the benefits of AMCS and OAT are encouraging, further higher quality evidence is needed to improve primary and secondary prevention of invasive IDU-associated bacterial and fungal infections. Access to AMCS and to OAT for hospitalized patients also needs to be improve. Recent studies of patients hospitalized with IDU-associated infective endocarditis found only 8% offered OAT in hospital 22 and only 6% receiving OAT 30 days after discharge. 9 The unofficial AMCS evaluated here offered OAT to all 34 eligible patients and 25 (74%) continued on OAT after discharge. Beyond medical complications of OUD, there is a need for hospital-based treatment of other substance use disorders, including alcohol, stimulant, benzodiazepine, and polysubstance use disorders. 24
With 59 referrals over 16 months at a 661-bed hospital, there is likely far more need for addiction medicine consultation that is currently being unaddressed at the QEII HSC (which is the tertiary care referral center for all of Nova Scotia). Local estimates of the prevalence of substance use disorders among QEII HSC inpatients do not exist, but related statistics indicate a high, unmet need. For example, in 2017, Nova Scotia's rate of hospitalizations entirely attributable to alcohol (307 per 100,000 people) was higher than the Canadian average rate (249 per 100,000), and also higher than Nova Scotia's rate of hospitalizations attributable to heart attacks (304 per 100,000). 25 Nova Scotians also report rates of heavy alcohol use and of smoking that are higher than Canadian averages. 25 This AMCS project was informed by a local needs-assessment on the quality of care offered patients with injection drug use-associated infective endocarditis at QEII HSC, which found most were not offered standard-of-care addiction treatment. 26 A recent study in the neighboring province of New Brunswick suggests that hospitalizations for IDU-associated infective endocarditis may be increasing in the region, 20 and local studies in Nova Scotia on IDU-associated infective endocarditis are underway. Local qualitative research has also identified a need for further resources for addiction care and harm reduction in hospitals and emergency departments across Nova Scotia. 27 , 28
In the short-term, the AMCS is recruiting more junior trainees to sustain the service. Over the long-term, the AMCS team is working with government health authority and hospital leadership to develop a business case for a resourced model that could be expanded to include colleagues with lived experience of substance use, social work, pharmacy, and nursing in addition to physicians.
This evaluation has important limitations. With no control group, we were unable to compare outcomes to similar patients who were not referred to the unofficial AMCS. However, the new service was organized to meet an identified need that most patients were not receiving addiction medicine care in hospital. Noting the emerging evidence regarding improved clinical outcomes associated with AMCS in general, we anticipate clinical benefits where the need is met. Because of the multiple informal ways that admitting services contacted the AMCS, we were unable to retrospectively determine the average length of time between a referral being received and a patient being seen. Also, by looking only at OAT status immediately post-discharge, we do not know the proportion of patients who stayed on OAT longer-term. Encouragingly, previous research has shown that hospital patients are more likely to engage in OAT long-term if it is started in hospital. 4 Further, hospitalization provides an opportunity to engage patients with innovative OAT initiation strategies, including buprenorphine micro-dosing. 29 This quantitative evaluation does not fully explain what has enabled the success of the service or how it can be improved. Longer-term follow-up and qualitative evaluations are a focus of ongoing research by our group.
An unofficial, trainee-organized, hospital AMCS was acceptable to providers and patients, feasible to deliver and organize, and positively impacted patient care. The service fills identified gaps in patient care and learning opportunities in addiction medicine. This unofficial trainee-organized AMCS could be used as a model at other hospitals, while building a business case for an official AMCS.
Footnotes
Acknowledgments
The authors would like to acknowledge Patti Melanson, RN, and Natasha Pace for inspiring the the unofficial service.
Disclosure statement
No potential conflict of interest was reported by the author(s).
Author contributions
Research conception and design: TDB, JF, EM, BM, DW; collection of data: TDB, EM, BM, JF, AN, CC, SH, DS, TO, LG. TDB performed the analyses and wrote the first draft. All authors contributed to interpretation of the results and to interim drafts, and approved the final version to be published.
TDB was supported in part by the Ross Stewart Smith Memorial Fellowship in Medical Research by Dalhousie University Faculty of Medicine and the Hui Lee Health Promotion Scholarship from the Canadian Society of Internal Medicine.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
