Abstract
Unilateral transtibial amputees (TTAs) show subtle gait variations while using different prosthetic feet. These variations have not been detected consistently with previous experimental measures. We introduce a novel measure called Symmetry in External Work (SEW) for quantifying kinetic gait differences between prosthetic feet. External work is the result of changes in kinetic and potential energy of body center of mass (CoM). SEW is computed by integrating vertical ground reaction forces obtained using F-scan in-sole sensors. Since various prosthetic feet have different designs, we hypothesized that SEW will vary with the type of foot used. This hypothesis was tested with a single unilateral TTA using four prosthetic feet (Proprio, Trias+, Seattle Lite and SACH). The Proprio (mean symmetry 94.5% ± 1.1%) and the Trias+ (92.1% ± 2.5%) feet exhibited higher symmetry between the intact and prosthetic limbs, as compared to the Seattle (67.8% ± 19.3%) and SACH (35.7% ± 11.1%) feet. There was also a good agreement in vertical CoM excursion between the intact foot and prosthetic feet with heel-toe foot plate designs. Results indicate that SEW measure may be a viable method to detect kinetic differences between prosthetic feet and could have clinical applications because of relatively low cost instrumentation and minimal subject intervention.
Introduction
Numerous studies have been conducted over the past two decades in an effort to objectively quantify differences among prosthetic feet. Results from these studies have been described in recent review articles.1-4 Some authors have found significant differences in gait characteristics among prosthetic feet, while others have found contradictory results.1-4 Conventional experimental measures, such as energy cost, EMG, walking speed etc., have failed to consistently demonstrate variations in gait between prosthetic feet.5,6 Clinically, differences in gait may be subjectively observed by the clinician and sensed by the patient, but instrumented gait analysis may not always confirm the expected differences with objective data. The following questions should then be raised: (i) Are the right gait parameters being examined? (ii) Is the right instrumentation being applied?, or (iii) Is the information obtained from the combination of gait parameters and testing equipment being processed properly, with the right measures, to appropriately answer the research question?
While various measures should be selected to answer specific research questions, it would be valuable for investigators and clinicians alike if a single valid measure was identified to show differences or similarities consistently among prosthetic foot/ankle assemblies. As new prosthetic technology is introduced with novel materials and microprocessor components, innovative measures of systematic evaluation should be identified. Such measures should accommodate for the unique features introduced in contemporary prosthetic foot technology. A measure that is portable and requires fewer resources than a contemporary gait laboratory would be attractive for specialized facilities and clinicians interested in employing instrumented evaluation tools. We introduce a new measure, Symmetry in External (mechanical) Work (SEW), with the intention to quantify kinetic differences in gait while using various prosthetic feet and to propose its use as a clinically friendly tool for practicing evidence based rehabilitation.
By definition, mechanical work is the change in kinetic and/or potential energy of the body. The energy changes brought about by external forces – mainly ground reaction forces – through displacement of the body center of mass, constitute external work.7 Work done by the muscles to move the joints and overcome muscle and/or tendon viscosity constitutes internal or physiological work.8 Positive work leads to an increase in the energy of the center of mass (CoM) whereas negative work tends to decrease its energy. During level ground walking, the support for body CoM alternates between single limb support and double limb support. According to the inverted pendulum model theory, no external mechanical work (hereafter referred to simply as ‘work’) is done during single limb support, when the stance limb behaves like a rigid inverted pendulum and the CoM moves along an arc about this limb.9-11 Conversely, during double limb support, a significant amount of work is done as the CoM moves from one inverted pendulum to the other (step-to-step transition).2,13 Both positive work and negative work is done during the various phases of a gait cycle (Figure 1). Any deviations in the amount of work from the normative values would imply deviations from the behavior of a perfectly conservative pendulum, and thereby alter the energetics of gait.7
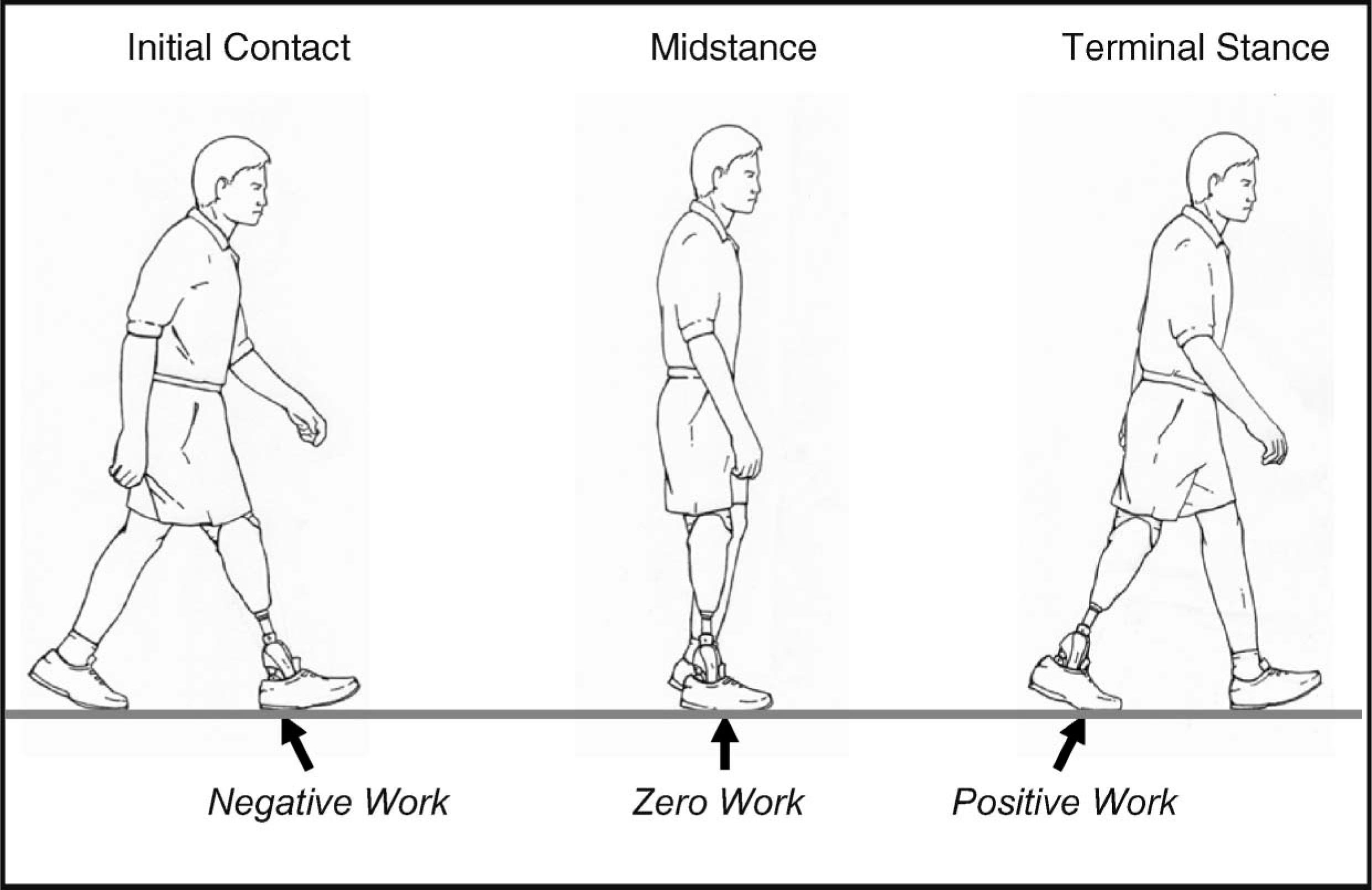
Work done by the prosthetic limb during the stance phase of gait. (Copyright and printed with permission from Advanced Rehabilitation Therapy, Inc. Miami, Florida).
People with unilateral lower limb impairments, particularly amputees, would theoretically not have a perfect pendular energy exchange during the step-to-step transitions due to anatomical and physiological asymmetries between the intact limb and the prosthetic limb. In unilateral transtibial amputees (TTAs), the transition from the intact limb to the prosthetic limb is not the same as the transition from the prosthetic limb to the intact limb, which results in asymmetry in the total work.14 Since prosthetic feet are designed to have different structural and functional characteristics, we hypothesized that the SEW percentage, a measure of total work asymmetry, would vary among prosthetic feet when used by the same amputee under the same conditions. To test the hypothesis, we examined the effects of four prosthetic feet on the symmetry of external work between the intact limb and the prosthetic limb.
Methods
The single subject had a left transtibial amputation due to trauma 35 years prior to enrollment. At the time of testing he was 55 years of age, with body mass 88.9 kg, height 1.67 m, and was using the Ceterus™ foot. He was classified as a K3 functional level amputee using the Medicare Functional Classification Level (MFCL) scale. The study protocol was reviewed and approved by the Institutional Review Board (IRB) at the Miami Veterans Affairs Health Care System and informed written consent was obtained from the subject prior to study enrollment.
A replica of the subject's socket was fabricated for testing purposes. Prosthetic fabrication of the socket, fitting and alignment of each prosthetic foot was performed by the same board certified prosthetist. The subject was tested using the following four prosthetic feet: (i) Proprio (Ossur, Reykjavik, Iceland), (ii) Trias+ (Otto Bock HealthCare GmbH, Duderstadt, Germany), (iii) Seattle Lite (Seattle Systems Inc, Poulsbo, USA) and (iv) SACH (Kingsley Mfg Co, Costa Mesa, USA). Testing order of the prosthetic feet was randomized by drawing. As a result, the Trias+ was tested first, followed by the SACH, Seattle Lite and finally the Proprio foot. An accommodation period of 4–7 days was used to familiarize the subject with each test foot and to determine comfort and alignment. The subject used the same pair of shoes and socks for all data collection sessions. Prior to enrolling in the study, he received gait training from a physical therapist specialized in amputee rehabilitation and gait in order to minimize gait deviations resulting from habit or lack of training. The gait training was based on proprioceptive neuromuscular facilitation resisted gait training program described in detail by Gailey and Clark.15 At the time of fitting each new foot, the same physical therapist evaluated the subject's gait to determine appropriate use of the foot. Additional training was provided for each foot during the evaluation session.
Data collection
The subject walked on a 21-m long level walkway at a self-selected walking speed where vertical ground reaction force (GRF) data were collected using the F-scan (Tekscan Inc, Boston, USA) in-sole pressure measurement system. Data collection and analysis with the F-scan system was done using previously validated methods.16,17 The F-scan system recorded data at 50 Hz for 10 sec and the recording began only after the subject had completed three full strides. The mean of 3–5 representative steps, obtained from two such trials, was used to estimate work values. GRF data were also obtained using two Kistler (Kistler Group, Winterthur, Switzerland) force plates (Type 9286 AA) and Bioware software (version 3.2), as the subject walked over the two masked force plates at a self-selected walking speed. Five successful trials were recorded at a sampling frequency of 50 Hz. A successful trial was defined as one where the subject's entire foot landed on the force plate. The GRF data from force plates were used only to calculate a correction factor for the F-scan data to ensure the accuracy of F-scan forces, as described by Mueller and Strube.16 The subject's walking speed was determined to be 1.25 m/s with the aid of a custom built Tekscan Matscan walkway system (Type 3150L 5×2).
Data analysis
Work per step done by the intact limb and work per step done by the prosthetic limb were calculated. One step was defined as the time interval from the initial contact of one foot to the initial contact of the opposite foot. Acceleration, which was calculated from GRF, was integrated twice to obtain the vertical CoM displacement.7,18 Work due to the force in the vertical direction and the resultant displacement of the CoM was calculated using the line integral:
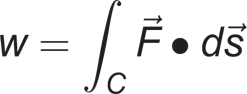

Results
A symmetry index of 100% would mean equal amounts of work done by the two lower limbs. As illustrated in Figure 2, the Proprio foot and the Trias+ foot had a high degree of symmetry between the intact and the prosthetic limb (94.5% ± 1.1% and 92.1% ± 2.5%, respectively). This indicates that the vertical kinetic and potential energy changes in the body CoM caused by the Proprio and Trias+ feet were similar to those produced by the intact foot. The symmetry index demonstrated by these two dynamic elastic response (DER) feet constructed with carbon fiber composite materials did not appear to be substantially different. The Seattle Lite foot had a symmetry index of 67.8% (±19.3%), intermediate between the DER feet and the SACH foot. The symmetry index for the SACH foot was the lowest of all test feet (35.7% ± 11.1%) and represented a substantial asymmetry between the intact and the prosthetic foot. Statistical analysis was not performed on the data because of the single subject design.
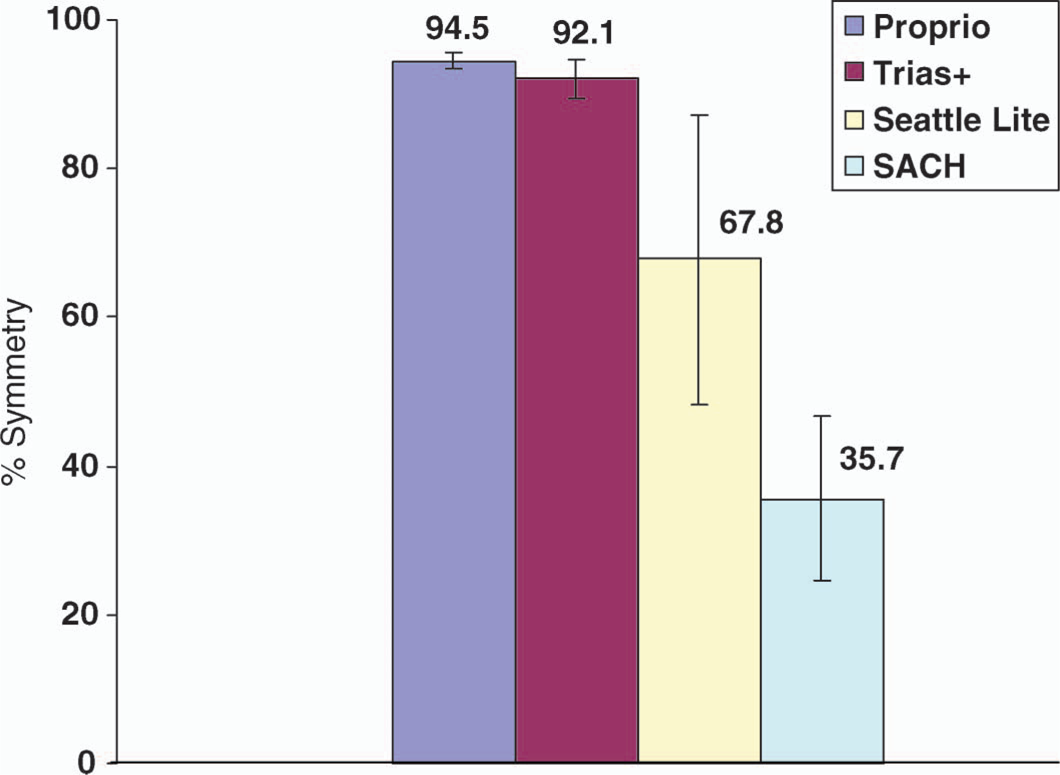
Percentage of symmetry in the amount of work done by the intact limb and the prosthetic limb during level walking at self-selected walking speeds, between four prosthetic foot designs. Vertical bars indicate ± SD from the mean.
Figure 3 shows the vertical CoM displacement trajectory for the intact limb step and the prosthetic limb step, for each of the four test feet. The displacement curves for the Proprio foot and the Trias+ foot were similar to that for the intact foot. The CoM trajectories produced by these two prosthetic feet have a distinct trough (negative displacement) followed by a peak (positive displacement), which is comparable with a typical displacement curve of an able bodied individual walking at a similar speed.20 While ambulating with the SACH and Seattle feet, the negative CoM displacement was not evident during the step with the intact limb. For both the SACH and Seattle feet, the intact limb produced a higher CoM excursion than the prosthetic limb. The maximum vertical excursion of the CoM for the four test feet is shown in Table I.
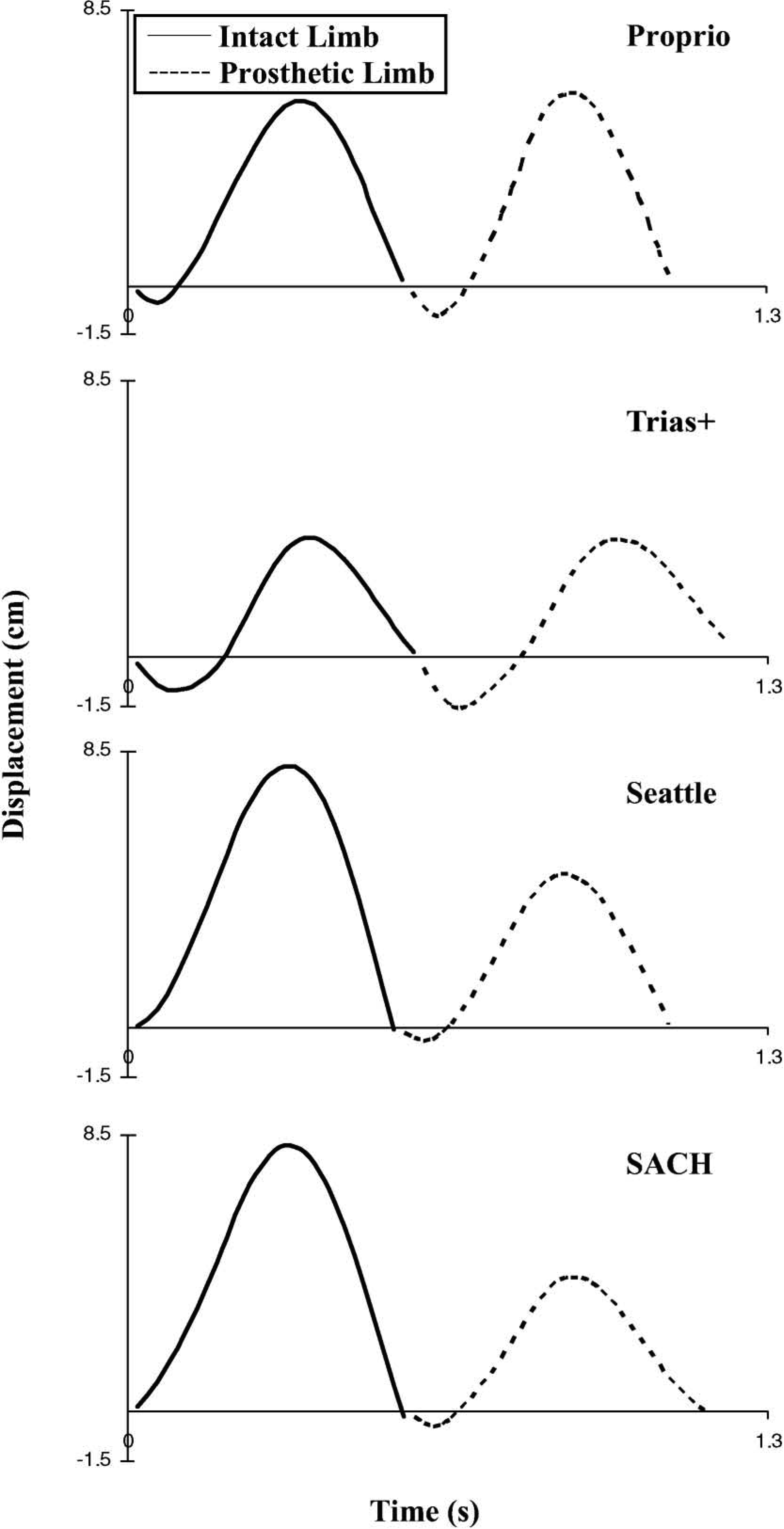
Representative trajectories of vertical CoM displacement for the intact limb step (solid line) and the prosthetic limb step (dashed line), for the four test feet.
Maximum vertical excursion of the center of mass, during a step taken with the intact limb and the prosthetic limb, while using the four test feet. Values are mean (±SD) and are in centimeters. ∗Taken from Gard et al.20.

Discussion
The proposed Symmetry in External Work (SEW) measure is a mathematical manipulation of ground reaction force data which is obtained using relatively simple instrumentation. This measure depends on three variables: The ground reaction forces, the time required to complete a step and the displacement of the body CoM during the step. Traditional methods of kinetic gait analysis involve analyzing forces at discreet points along the force-time curve, typically magnitude of the peak force. The SEW measure, on the contrary, uses the property of integration which allows force, time, and CoM displacement over a step to be combined into a single value. This measure offers unique sensitivity, as any change in one of these three variables would change the value of the line integral and eventually affect gait symmetry.
External work has three components: Work done by the anterior-posterior component of force to increase the forward speed of CoM (WF); Work done by the vertical component of force to cause a sinusoidal movement of the CoM in the sagittal plane (WV); Work done by the medial-lateral component of force and the resulting sideways movement of the CoM (WL).
Cavagna et al.21 reported a high degree of inter-limb symmetry in WV and WF for able-bodied individuals. WL was neglected from analysis as it was found to be much smaller than WV and WF. Tesio et al.14 have shown asymmetry in external work between the sound limb and prosthetic limb steps in transtibial amputees. They found that the forward push generated by the prosthetic limb during the prosthetic to sound transition was much lower than that generated by the sound limb during the sound to prosthetic transition. Our results support their findings regarding the asymmetry in vertical work and provide evidence that this asymmetry is influenced by the design of the prosthetic foot, such as its energy storage and return characteristics and the foot roll factor.
Meinders et al.22 have reported the mechanical efficiency of the SACH and Seattle feet to be 39% and 71%, respectively. The efficiency was calculated as the ratio of energy generated to the energy absorbed during gait. The low efficiency SACH foot had the least symmetry (35.7%) of all the feet tested in this study. The moderate efficiency of the Seattle foot resulted in an intermediate symmetry index of 67.8%. The energy storage and return values for the Trias+ foot or the Proprio foot have not been reported in the literature, hence a direct comparison cannot be made. These two feet have a composite carbon fiber design with dynamic elastic response characteristics, which is similar to the design of the Flexfoot. The 89% efficiency22 of the Flexfoot would therefore imply that the efficiency of the Proprio and the Trias+ is higher than that of the SACH and Seattle feet. In this study, the symmetry indices for the Trias+ and the Proprio foot were found to be 92.1% and 94.5%, respectively.
The CoM excursion with the intact limb step was different for all four test feet (Table I, Figure 3). The differences in CoM excursion indicate a possible gait adaptation strategy employed by the subject to accommodate to the various prosthetic feet. While ambulating with the SACH and Seattle feet, the CoM had a noticeably higher excursion with the intact limb step as compared to the prosthetic limb step. Such asymmetry in CoM displacement has also been reported by Tesio et al.14 There is a mathematical relationship between vertical CoM displacement and the foot roll factor.23 The foot roll factor was used to calculate the Effective Foot Length Ratio (ELFR) for various prosthetic feet by Hansen et al.24 Prosthetic feet with a heel-to-toe foot plate design had a higher EFLR than the feet with shorter keels, such as the SACH and Seattle feet. The EFLR of the physiologic foot was the highest of all feet tested by Hansen et al.24 In this study, the CoM excursion during a step with the heel-to-toe design prosthetic feet was similar to that seen with the intact foot step, resulting in high symmetry. The shorter keel feet resulted in noticeable differences in CoM trajectories and magnitudes between prosthetic foot and the intact foot steps (Table I, Figure 3). The disparity in roll factor between prosthetic feet and the physiologic foot probably contributed to the variations in vertical CoM displacements. The above-mentioned design variables, either in isolation or combination may help explain the observed differences in SEW between feet. Further research across subjects and between prosthetic feet will be required before causal relationships can be established.
Unilateral transtibial amputees develop the ability to adapt to their prosthesis. Clinicians often observe subtle changes in a transtibial amputee's gait among prosthetic feet. However, these changes have not been detected consistently by contemporary measures and instruments.1-4 From the results of this study, it appears that the SEW measure could be used as a clinical tool to distinguish gait variations among prosthetic feet and document the clinically relevant differences. With this measure, limited instrumentation is attached to the patient who is simply asked to walk for 10–20 sec with in-sole sensors. The mathematical calculations can be incorporated into a computer program, such that the SEW values are obtained relatively quickly. The process of integration can be easily done using spreadsheet programs, such as Microsoft Excel, without the need for specialized software. Additionally, the use of SEW to compare prosthetic feet on a single patient has the advantage of eliminating errors that may arise from dissimilar gait patterns between amputee subjects. If multiple prosthetic feet are tested on the same amputee, under the same conditions, and without any physical change in the subject, the variations in SEW would likely be related to variance in prosthetic feet design. Clinicians would thus have an index to differentiate between prosthetic feet, thereby furthering their ability to implement evidence based practice.
Calculating external work with commercially available in-sole sensors, similar to the ones used in this study, would have three limitations: (i) Calculation of WF and WL is not be possible, as such sensors do not measure fore-aft and medio-lateral shear forces, (ii) the properties of the sensors may change over time because of damage due to repeated or excessive loading, and (iii) cost. Despite these limitations, the clinical applicability may be more beneficial to clinicians who do not have the resources for a fully instrumented gait analysis system. Some of the above mentioned limitations might be negated with the advent of improved in-sole sensor technology. Until such technology becomes commercially available, the less expensive and mobile in-sole sensors currently available could be used for clinical applications. To ensure the accuracy of F-scan sensors for research purposes, a correction factor was calculated in this study.16 If the output of an in-sole sensor system is within the margin of error for clinical applications, calculation of such a correction factor would not be required.
It could be argued whether or not symmetry should be used as a benchmark for evaluating prosthetic gait. In a recent review article, Gailey et al.25 found that asymmetry resulting from the tendency of amputees to favor their intact limb over the prosthetic limb can lead to secondary conditions such as degenerative joint disease. Conversely, in 1988 Winter and Sienko26 suggested that amputee gait should not be assessed only on symmetry and that “a new non-symmetrical optimal is being sought by the amputee within the constraints of his residual system and the mechanics of his prosthesis”.26 After extensive review of the literature the term “non-symmetrical optimal”, to our knowledge, has not been discussed. The goal of current prosthetic engineering technology has been to develop prosthetic feet that will mimic the function of a physiologic foot. In this study 95% symmetry was observed with the Proprio foot and 92% symmetry was observed with the Trias+ foot. Prosthetic feet designs of 20 years ago, which lacked the advanced material and engineering technology available today, may have led to conclusions that asymmetry could be an acceptable outcome. The question today should be the reverse, “how do we reduce the asymmetry by the additional 5–8%?” Although transtibial amputees have varying degrees of musculoskeletal compromises that may not permit 100% symmetry for all who wear a prosthesis, we suggest the goal of symmetry become the common outcome, shared between all rehabilitation clinicians.
Conclusion
The Symmetry in External (mechanical) Work (SEW) measure was able to detect differences in gait kinetics between the four prosthetic feet used in this study. This measure has the potential to be clinically friendly and used in patient care facilities to distinguish clinically relevant gait differences among prosthetic feet. The results of this study are based on a single subject case study and further research involving more subjects with a wide variety of feet would prove beneficial for researchers and clinicians.
