Abstract
This paper explores the use of biofeedback to improve gait in Parkinson's disease (PD) and, in particular, reports on the design and testing of a new vibratory orthosis. The orthosis causes a rhythmic vibratory stimulus to be applied to one or other side of the lumbar region. The stimulus is synchronized with stepping through the use of heel-located switches; each switch controls the stimulus to the corresponding side of the body. In the experimental evaluation it was hypothesized that step-synchronized, vibratory stimulation applied to the lumbar region will lead to an increase in walking velocity in patients with idiopathic Parkinson's disease. Subjects were asked to carry out walking trials under two conditions. In one condition, the vibratory orthosis was active; in the other condition the vibratory orthosis was inactive. Walking velocity was measured over a straight, 10 m walkway. A comparison between the two conditions using a paired t-test showed a significant increase in walking velocity when the vibratory orthosis was active, compared with the inactive condition. It was speculated that use of the vibratory orthosis, which stimulates proprioceptive receptors, may lead to an improvement in gait, stability and may support gait re-education in PD patients. It was also suggested that the results may inform future ideas for rehabilitation of similar neurological diseases.
Introduction
Parkinson's disease (PD) is a chronic and progressive disease of the central nervous system that can have a significant impact on patients' activities.1 As the disease progresses, gait becomes slower, and is characterized by shuffling, short steps, and a loss of arm swing.2 The orthotic management of PD patients largely focuses on the improvement of gait pattern.
PD patients have impaired proprioception and movement perception.3,4 It has been proposed that disturbances of proprioceptive regulation underlie, or contribute to motor deficits in PD patients.4 Application of biofeedback may improve the characteristics of gait in PD patients.2,5,6 It has been shown that in PD patients the walking pattern will be improved following a specific instruction or stimulation.2 For example, temporary walking improvements have been reported in PD patients, using visual targets, as well as placing markers on the floor, or giving verbal instructions.2 It has been suggested that in PD patients external sensory cues can provide a trigger that can assist in the moving from one component in a movement sequence to the next.7
Application of noise is one of the recent techniques to be used for proprioceptive stimulation. It has been shown that noisy stimulation (visually, auditory, or vibratory) can enhance the detection and transmission of weak signals in sensory systems, via a mechanism known as stochastic resonance. This phenomenon is based on the concept that the flow of information through a system can be maximized by the presence of a particular non-zero level of noise.8 It has been shown that vibratory devices could ameliorate balance control impairments in diabetic and stroke patients.8
Vibratory modules can be embedded in assistive devices for proprioceptive stimulation. Previously, vibratory insoles have been used to address age-related postural instabilities in a study with elderly subjects.9 Random whole-body vibration, a useful strategy in physical therapy, has also been applied as a tool to improve the postural stability in PD patients.10
The authors hypothesized that step-synchronized, vibratory stimulation will lead to an increase in walking velocity in patients with idiopathic Parkinson's disease. To test this hypothesis, a new orthosis was designed to stimulate the lumbar region with step-synchronized mechanical vibrations.
Methods
Design of the vibratory orthosis
The vibratory orthosis, shown in Figure 1, is a soft lumbar orthosis that can be used to apply mechanical vibrations to each side of the posterior lumbar region. The vibratory orthosis was designed to be placed on lumbar region, as PD patients generally have impaired proprioception in their limbs.11 The fabric part of the orthosis consists of a soft belt with elastic and non-elastic straps, the elastic straps providing the best fit for varying patient sizes.
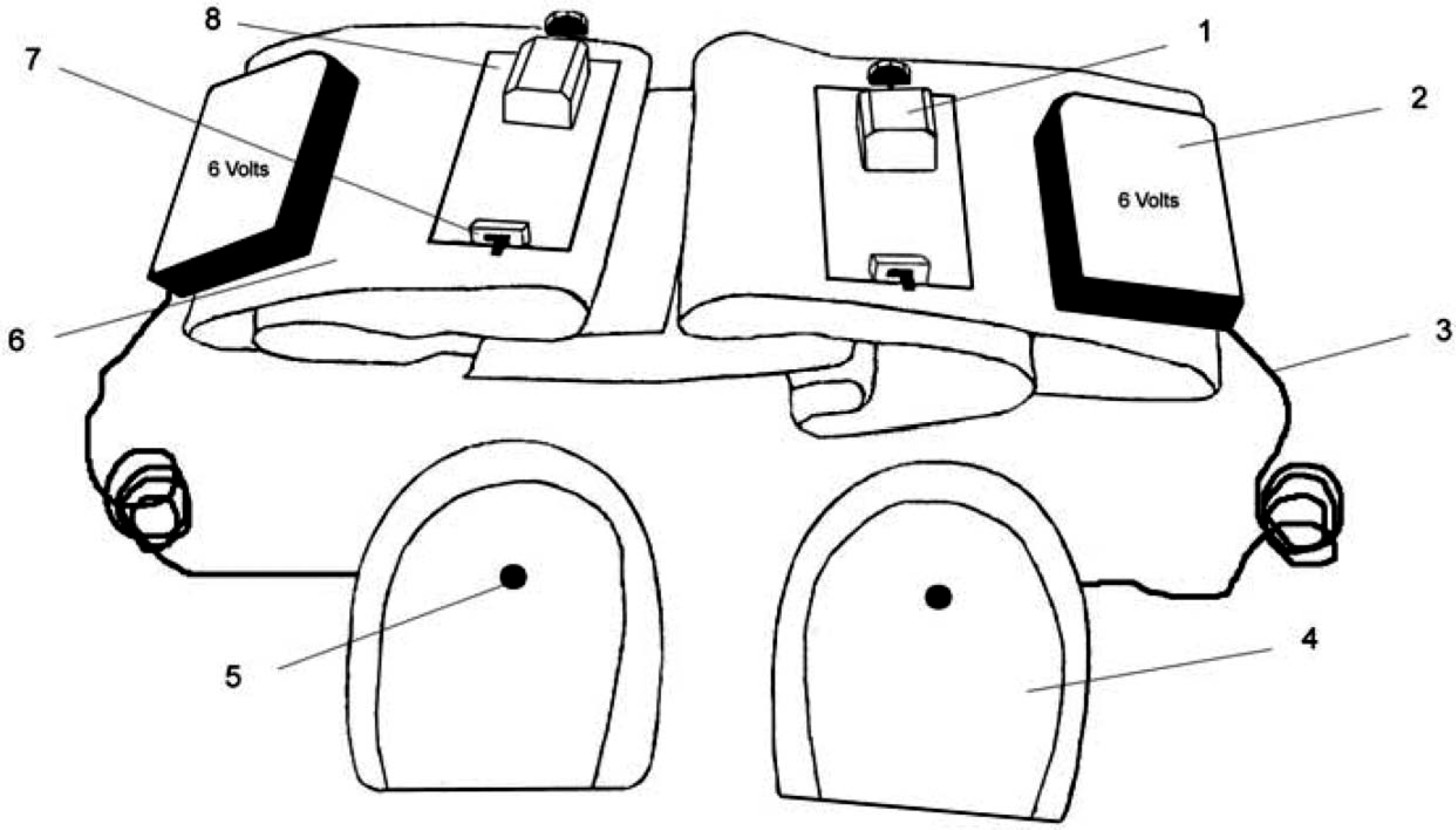
Vibratory orthosis. 1: Vibratory motor, 2: Battery pack, 3: Wire, 4: Heel cup, 5: Micro-switch, 6: Soft belt, 7: Main-power switch, 8: Plastic board.
Loading on micro-switches (positioned underneath polypropylene heel cups and supported by a rubber layer to prevent damage), one located under each heel, activate the small vibratory electro-motors that provide the mechanical vibrations (see Figure 1). As a result, stimulation is applied to the lumbar region on the left side at left foot contact; stimulation is applied to the right lumbar region on right foot contact. Stimulation is terminated when the heel leaves the ground. Thus, the total stimulation time is dependent on the frequency and duration of heel contacts with ground.
Sub-threshold mechanical vibrations applied to the soles of the feet, have been shown to improve quiet-standing balance in healthy subjects and also in patients with diabetes and stroke. The effect of the supra-threshold vibration is complex and depends on the frequency, amplitude, and site of stimulation.6 The choice of vibration frequency, 97 Hz, for the vibratory orthosis was informed by the results of similar studies9,11 together with an understanding of the relationships between stimulation frequency and comfort. A DC motor with a 2 gm weight eccentrically located on the motor shaft was used to create the vibratory inputs. The frequency of the motor system depends on the input voltage and a 6v DC power supply was chosen to provide 97 Hz as the vibratory frequency with a peak-peak amplitude of approximately 0.5mm. The motor is fastened to a small plastic board and connected to the belts. Thin layers of rubber support the motor to prevent the spread of the vibration.
Experimental protocol
All aspects of the study were approved by the Ethics Committee of the Iran University of Medical Sciences (IUMS). All patients signed a written, informed consent before participating in this study. Furthermore, subjects were allowed to withdraw from the study in case of discomfort.
In this experiment, walking velocity was measured in one group of PD patients using a digital chronometer to record time taken to walk over a standard 10 m path. The 10 m walk is a simple clinical test for velocity evaluation, as well as a useful indicator of motor functions during activities of daily living.12
The test was performed on an indoor, level pathway with marked start and end lines. The first and the last steps were excluded from the analyses, since PD patients have problems with initiating and terminating gait.1 An average of two trials for each test was used in the further analyses.
Patients were asked to walk at their preferred walking speed and no encouragement was provided to the subjects during the tests. All tests were evaluated by the same examiner to eliminate inter-rater differences. Tests were performed unshod to eliminate the effects of shoes on the outcomes. Moreover, all patients used the same type of socks to keep the heel cups under their heels.
In order to limit the learning effect, a one-minute familiarization trial was carried out before the tests. Two different conditions were examined. Firstly, the patients walked along a 10 m path without using the vibratory orthosis, and secondly, they repeated the test with the vibratory orthosis. The batteries of the orthosis were replaced regularly to ensure a constant electric voltage during all the tests.
Participants
In this study, patients were selected based on judgmental, i.e., non-probability sampling from those who were referred to Medical Firuzgar Hospital of Tehran during the period of the study. All patients were selected by a thorough neurological evaluation by a neurologist and had a confirmed diagnosis of idiopathic Parkinson's disease, based on the UK Brain Bank criteria.13 Fourteen patients, 12 men and 2 women, participated in the study. Their age was 59.9 ± 9.1 years (mean ± standard deviation [SD]) and their PD duration was 5.9 ± 4.2 years. The inclusion criteria were: (i) Disease severity stage of 2 to 4 based on the Hoehn and Yahr scale14; (ii) existence of mild to moderate walking difficulties that were determined by a score of 1 or 2 on each of the following questions: question 15 of the ADL sub-section and questions 29 and 30 of the motor sub-section in the Unified Parkinson's Disease Rating Scale15; and (iii) achieving a score of at least 24, in the Mini Mental State Exam16 to confirm they were without dementia. Exclusion criteria were the existence of freezing during walking, a history of recent falls, and a history of other neurological, musculoskeletal, and cardiovascular diseases.
Characteristics of PD patients
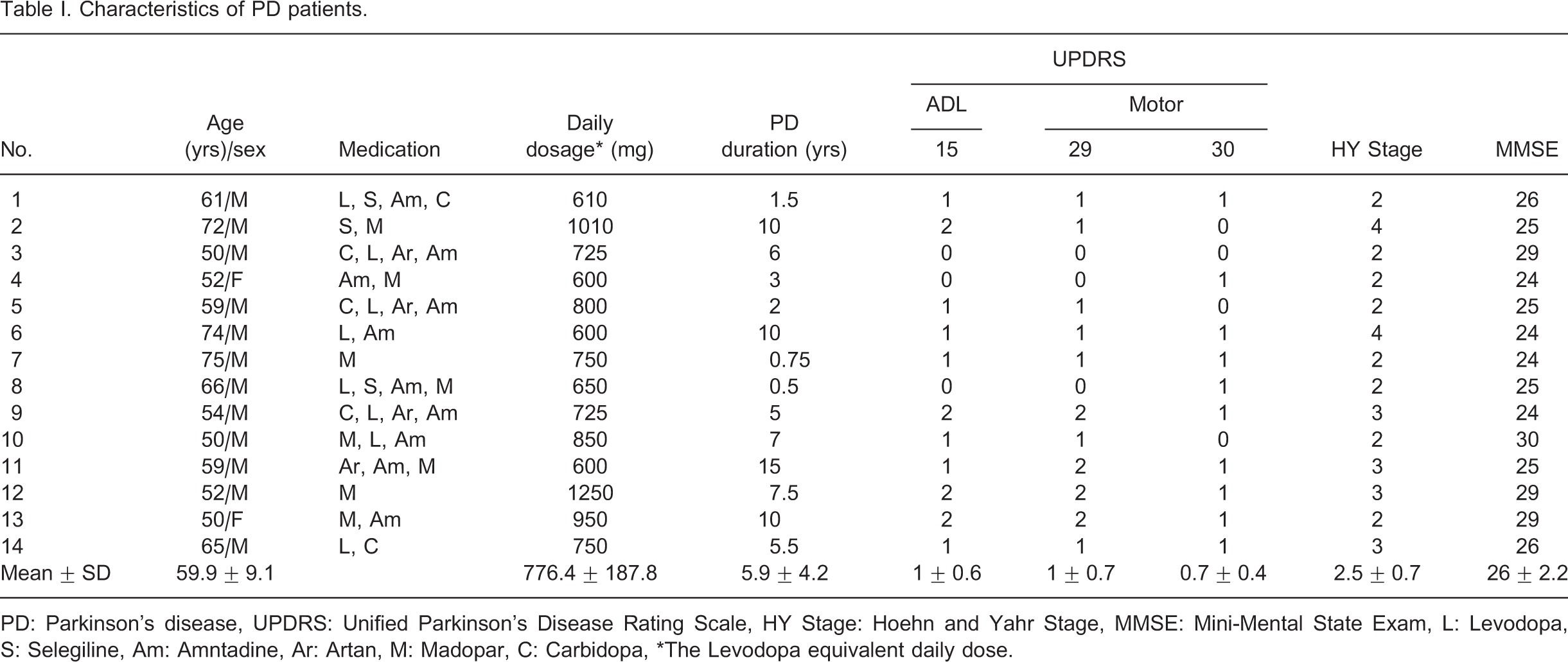
PD: Parkinson's disease, UPDRS: Unified Parkinson's Disease Rating Scale, HY Stage: Hoehn and Yahr Stage, MMSE: Mini-Mental State Exam, L: Levodopa, S: Selegiline, Am: Amntadine, Ar: Artan, M: Madopar, C: Carbidopa, ∗The Levodopa equivalent daily dose.
Statistical analysis
All calculations were carried out using the SPSS software package (version 15). Paired t-test statistics (2-tailed) were used to compare the mean of elapsed walking time in both test conditions. In this study alpha level was set at 0.05.
Results
Results of 10 m walking test with and without the vibratory orthosis
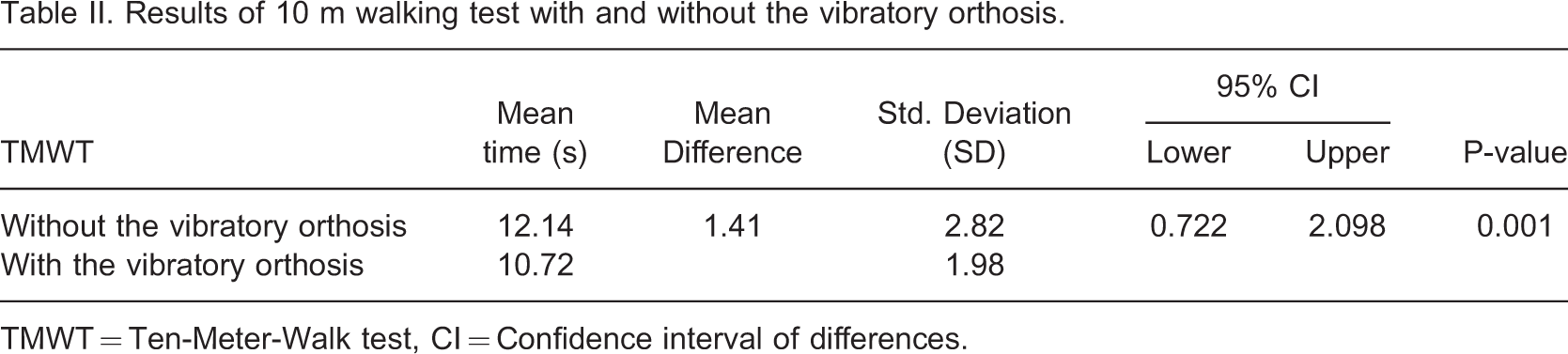
TMWT = Ten-Meter-Walk test, CI = Confidence interval of differences.
The mean elapsed time in the second condition (with the vibratory orthosis) is 1.41 sec shorter than the mean time in the first condition (without the vibratory orthosis). Thus patients walked faster when the vibratory orthosis was active. The findings of the study revealed that there was a significant difference (p = 0.001) in elapsed time to walk along a 10 m path between the two conditions, (with and without the vibratory orthosis).
Discussion
Generally, PD patients do not walk quickly. The results showed that PD patients walked along a 10 m path in less time when they used the vibratory orthosis than when they did not use the orthosis. The results are consistent with several previous studies that also showed an improvement in walking velocity.2,6 However, in contrast to the study reported here and also to other relevant reports in the literature, the Del Olmo and Cudeiro study7 reported walking velocity decreasing when using auditory cues.
In the present study, in order to decrease the learning effect, patients wore the vibratory orthosis and walked for one minute before starting the tests to get familiarized. Moreover, they were given 1 min rest between test trials. Although stride length and cadence were not measured during walking,
An improvement in walking speed resulted from the reduction of stride variability, the major gait unsteadiness in the Peter Novak and Vera Novak study.6 They used vibratory insoles to provide step-synchronized stimulation to the plantar surface of PD patients' feet. The present study which used a different method agreed with the results of their study in terms of showing an improvement in walking velocity. However, the frequency of vibration, the site of vibration, and the assessment tool used were all different.
In a previous study, it has been shown that vibratory stimuli synchronized with gait may enhance gait timing and variability.6 The vibratory orthosis causes a rhythmic vibratory stimulus to each side of the lumbar region that is synchronized with foot placement. The authors speculated that use of the vibratory orthosis may lead to an improvement in gait, stability and may support gait re-education in PD patients.
The results of this study may not be generalizable to the PD population, given the small sample and selection of patients. Only patients with mild to moderate disease severity were included and those who had freezing during walking or history of recent falls were excluded from the study. Further, the participants' cognitive and psychological conditions and some of their clinical characteristics, such as medication type and daily drug dosage, varied. Future studies should be conducted to investigate the possible effect that these may have on the effect of the orthosis on gait. In this short-term non-blinded study, possible learning effects were not completely excluded. A long-term study is needed to show the feasibility in daily use of the vibratory orthosis described here, as well as to identify the optimal frequency and amplitude of vibration.
Conclusion
In this study, the possibility of using a step-synchronized vibratory orthosis to increase walking velocity in PD patients was evaluated in a short-term study. The study showed a significant improvement in walking velocity when using the orthosis compared to the no-orthosis condition. It is worth noting that, although the use of the vibratory orthosis was shown to improve walking velocity, its efficacy needs to be evaluated by a thorough survey regarding patients' satisfaction, and also the daily functional abilities of PD patients using it. Finally, a new orthosis for the rehabilitation of PD patients was introduced that may inform future ideas for rehabilitation of similar neurological diseases.
