Abstract
There is increasing interest in the psychiatric literature in herbal remedies and other alternative treatments (e.g. [1,2]). Herbal medicines appear to be frequently used in developed and developing countries for a range of psychiatric problems [3]. Unfortunately, there have been no studies on the views and experiences of mental health professionals regarding patients' use of herbal treatments and alternative treatments. This area is important to examine because the taking of herbal remedies by patients has implications for psychiatry in several domains, including drug interactions, compliance to ‘conventional’ treatments and patient attitudes towards psychiatrists. Further, psychiatrists may be a useful source of information about adverse events associated with alternative treatments. There have been suggestions that these events are underreported [4].
Of all the so-called ‘nervine’ herbs (herbs taken for psychiatric or neurological reasons), St John's Wort (SJW) is currently attracting the most attention and appears to be extensively used, particularly for depression [4,5]. Across all trials, 50–80% of depressed patients on SJW improved. St John's Wort was most beneficial for mild to moderately severe depression. The herb is generally well tolerated. Side-effects include gastrointestinal symptoms, allergic reactions, fatigue and restlessness [6,7]. Phototoxicity has been reported in two patients on antidepressant doses [8,9]. There have been two case reports of SJW precipitating manic episodes [10,11]. There is negligible published data about interactions of SJW with other psychotropic agents; serotonin syndrome has been described in three patients following concurrent use of sertraline [12], nefazodone [12] and trazodone [13]. There is also an account of a syndrome ‘resembling benzodiazepine intoxication’ in a patient on SJW and paroxetine [14].
The aims of this study were to ascertain psychiatrists' experiences and opinions concerning SJW, particularly in relation to side-effect profile and drug interactions, how the subject of herbal medicine was handled with patients and whether psychiatrists had recommended the use of SJW. It was considered that this information would be useful to health professionals as well as to the users of such remedies.
Method
A 26-item questionnaire was constructed by the authors and mailed in July 1999 to each member of the Royal Australian and New Zealand College of Psychiatrists (RANZCP) residing in Australia or New Zealand. The questionnaire covered demographic features (e.g. age, gender, years in practice), practice description, experience with SJW in patients (including numbers of patients known to have used the herb, perceived effectiveness, adverse events) and how psychiatrists negotiated the subject of alternative treatments with patients.
Results
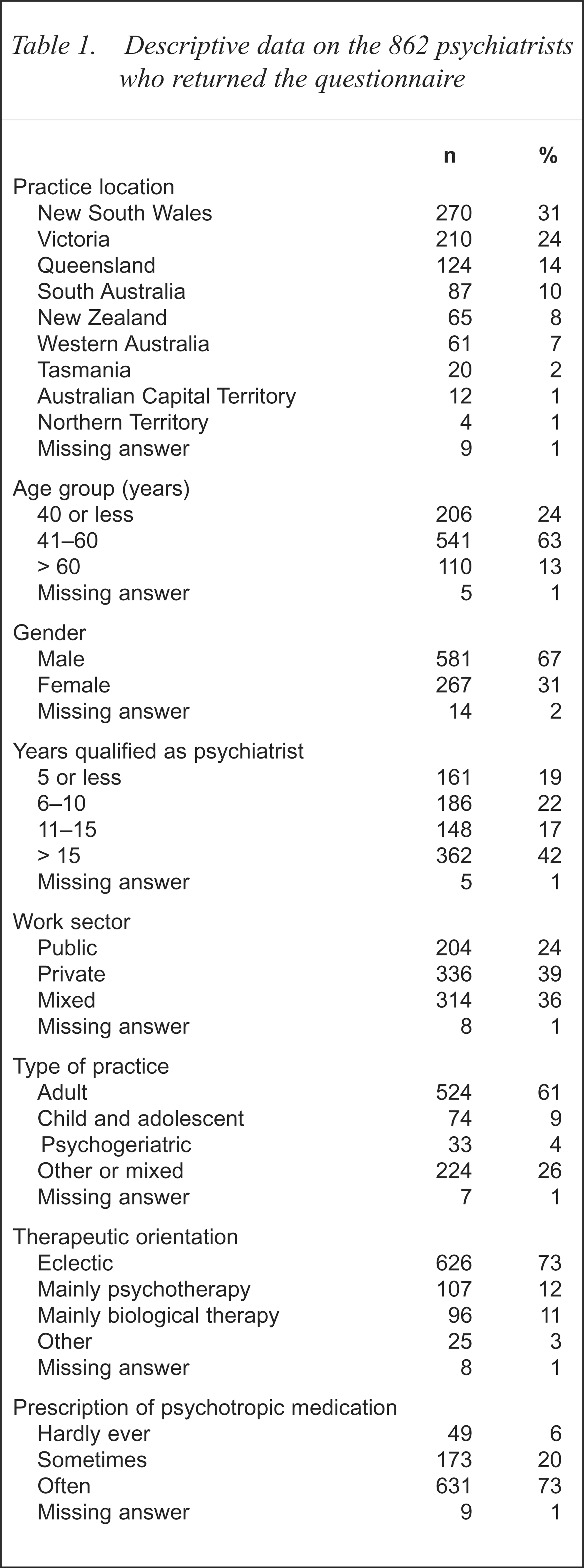
Of the 1910 questionnaires mailed, 862 (45%) were returned. The response rate was fairly uniform across practice locations: New South Wales (47%), Victoria (39%), Queensland (47%), South Australia (47%), Western Australia (46%), Tasmania (50%), ACT (50%), Northern Territory (50%), New Zealand (41%). Descriptive data on the psychiatrists who returned the questionnaire are shown in Table 1. Typically, they were male, aged 41–60 years, had been qualified as a psychiatrist for more than 15 years, practised adult psychiatry, worked at least partly in the private sector, were eclectic in orientation and were not averse to prescribing psychotropic medication.
Descriptive data on the 862 psychiatrists who returned the questionnaire
The majority of psychiatrists (n = 686, 80%) reported that they had patients who had taken SJW; about one-third of respondents (n = 299, 35%) reported more than five of their patients had used SJW. Of those psychiatrists who had patients who had used SJW, almost half (n = 314, 46%) considered it had been helpful in at least one patient; almost one-third (n = 216, 31%) were unsure. Only about one-quarter (n = 162, 24%) of psychiatrists with patients who had used the herb did not believe it had been helpful in any patients.
Twenty-eight per cent (n = 195) of psychiatrists with patients who had used SJW reported side-effects with that treatment and 8% (n = 52) reported drug interactions between SJW and other agents (Table 2).
Adverse events of St John's Wort reported by psychiatrists with patients who had taken the herb
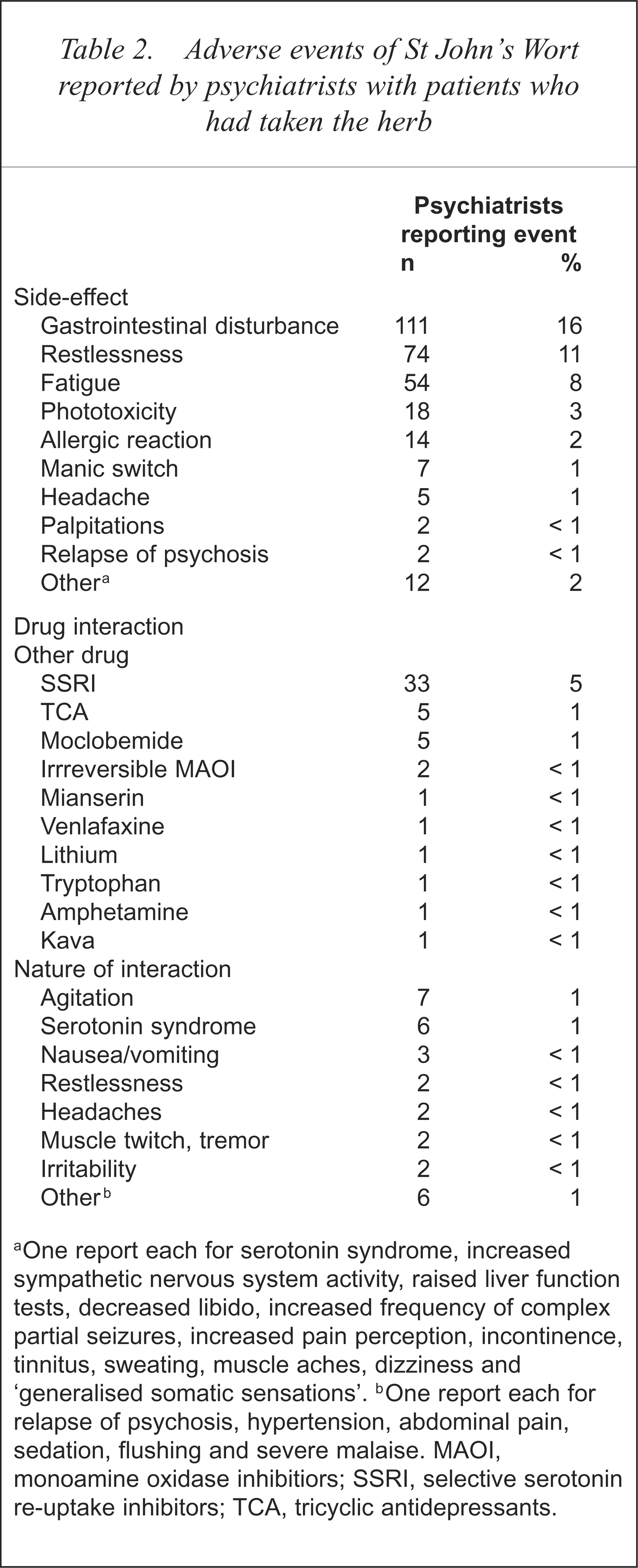
One report each for serotonin syndrome, increased sympathetic nervous system activity, raised liver function tests, decreased libido, increased frequency of complex partial seizures, increased pain perception, incontinence, tinnitus, sweating, muscle aches, dizziness and ‘generalised somatic sensations’.
One report each for relapse of psychosis, hypertension, abdominal pain, sedation, flushing and severe malaise. MAOI, monoamine oxidase inhibitiors; SSRI, selective serotonin re-uptake inhibitors; TCA, tricyclic antidepressants.
A minority of psychiatrists (n = 327, 38%) said that they routinely asked patients if they used SJW or other alternative treatments. If a psychiatrist learned that a patient was taking SJW, most (n = 739, 86%) indicated that they would discuss the pros and cons of its continued use with the patient. Few psychiatrists would disregard this information (n = 31, 4%) or actively discourage the patient taking it (n = 23, 3%). If a patient asked the psychiatrist for information about SJW, about half of respondents (n = 443, 51%) said they would give the patient the information they currently have; a further quarter (n = 201, 23%) would assist the patient in finding that information.
One-quarter (n = 217, 25%) of respondents stated they had recommended SJW to patients. The vast majority of these (n = 202, 93%) had suggested SJW for depression; a minority (n = 62, 29%) had recommended the herb for anxiety. Other conditions for which psychiatrists had recommended SJW to patients included insomnia (n = 7, 3%), and (one case each for) attention deficit disorder, obsessive compulsive disorder, posttraumatic stress disorder, premenstrual syndrome and withdrawal from selective serotonin reuptake inhibitors. Correlates of psychiatrists recommending SJW to patients were examined using logistic regression. Factors significantly (p < 0.01) associated with recommending the herb included: working exclusively in the private sector (1.8 times as likely to recommend), practising in South Australia (1.9 times), having (self-rated) more advanced knowledge about SJW (3.2 times), believing herbal drugs are safer than conventional drugs (2.3 times), having patients who have used SJW (5.4 times), giving or helping patients find information about SJW if asked (3.6 times), willingness to discuss the pros and cons of continued use of SJW in those patients already on it (4.6. times) and having tried a herbal remedy themselves for a health problem (1.7 times). It is of note in this regard that 340 (39%) of psychiatrists reported using herbal remedies themselves.
Psychiatrists considered that SJW appeared to be commonly used by the general public because of community concerns about conventional drugs (n = 736, 85%), ‘New Age’ beliefs (n = 515, 60%), wariness about mental health professionals (n = 477, 55%), the ease with which SJW could be obtained (n = 424, 49%) and ‘good marketing’ (n = 280, 32%). However, most psychiatrists (n = 615, 71%) did not believe that herbal remedies were safer than conventional drugs. The vast majority (n = 745, 86%) believed that psychiatrists and psychiatry trainees should be taught about SJW and other alternative treatments.
Discussion
The limitations of this study include the fact that the information obtained from respondents was anecdotal and retrospective and that the data may not be able to be generalised to settings outside Australia and New Zealand. Nevertheless, the information was gathered systematically, the sample size was large (representing almost half of all practising psychiatrists in the two countries) and there were few missing data.
To the best of our knowledge, this is the only study which has examined the experience and attitudes of psychiatrists regarding herbal treatments and the largest survey of health professionals generally about alternative treatments. One of the major findings was that adverse events associated with SJW appear to be fairly common and potentially serious. Although a cause–effect relationship can not be firmly established on the basis of our data, the study elicited some adverse events which were previously considered exceedingly rare in therapeutic doses (e.g. phototoxicity) and others (e.g. drug interactions) which had not been reported. It would seem that the side-effects of SJW may have been underestimated [4]. In the absence of more substantive data, the survey indicates that the deleterious effects of the herb should be further evaluated and that particular caution should be exercised in combining SJW with other psychotropics. Psychiatrists should report adverse events to appropriate agencies, such as the Adverse Drug Reaction Advisory Committee (ADRAC) for Australian practitioners. Pharmaceutical companies should mention the dangers of using SJW with psychotropics, particularly antidepressants, in their product information. It is worth digressing to note that SJW is an ingredient in new varieties of lipstick, soup and tortilla [15,16]; the present study suggests that this practice is hazardous. Manufacturers thinking of ‘enriching’ foodstuffs with SJW need to be aware of the potential risks.
Another important finding was that many psychiatrists from Australia and New Zealand display positive attitudes towards SJW and alternative treatments, for example being prepared to give advice to patients about SJW, helping them find out more on the herb and believing that psychiatrists and trainees should be taught about alternative treatments. Such behaviours are in keeping with recent calls (e.g. [2,17]) for clinicians to take an active interest in their patients' use of alternative treatments. Nevertheless, it was perhaps surprising that psychiatrists were recommending SJW for a variety of disorders when the evidence supporting this is currently either limited or non-existent. Furthermore, it might be hoped that, in time, more psychiatrists will routinely ask patients about their use of alternative treatments. It would be useful to ascertain whether psychiatrists in other countries share some of the experiences and opinions described in this study.
Acknowledgements
The authors thank C. Knowles for assistance, the Royal Australian and New Zealand College of Psychiatrists for administrative support and the psychiatrists who took part in the survey.
