Abstract
Introduction
Unrepaired annular defects potentially increase the reherniation rate after lumbar discectomies and have been shown to accelerate degenerative changes after discographies.
This is the first study to test an injectable biological substance to repair annular defects in vivo. We used high-density collagen gel in a needle-punctured rat-tail model. Needle puncturing leads to extrusion of NP tissue with subsequent degenerative changes (4). Restoring annular integrity will help retain the NP material and therefore inhibit these changes.
Materials and Methods
We punctured the S3/S4 intervertebral disc (IVD) of 30 athymic rats using an 18-gauge needle. Subsequently high-density collagen (HDC) gel was injected to seal the defect. Riboflavin (RF) was added to increase the stiffness of the collagen gel by inducing chemical cross-link formation.
Animals were subdivided into four groups. The first group was injected with uncross-linked HDC gel (
Animals were sacrificed at 1, 2, 5 (
Results
Over 18 weeks RF cross-linked groups retained significantly more NP tissue in the disc space than the uncross-linked and the control groups according to NP voxel count and histological NP cross-section measurements (
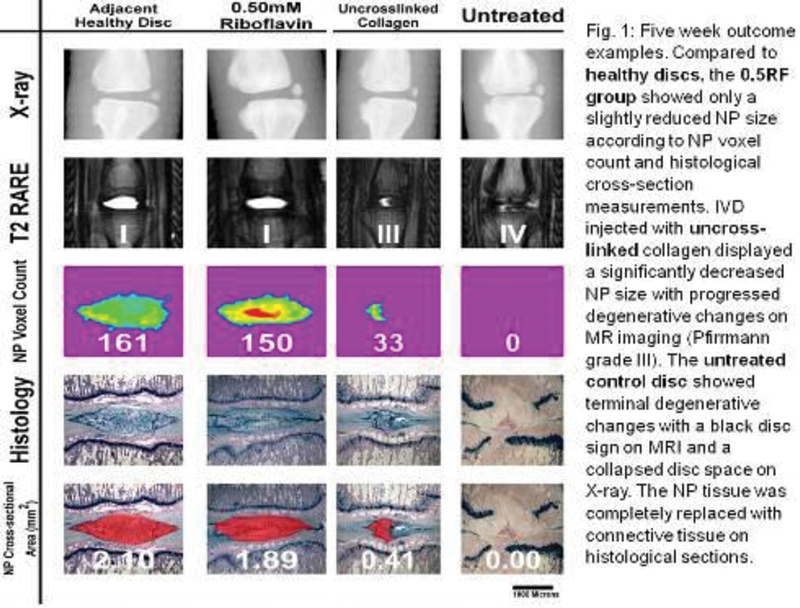
After 18 weeks, the uncross-linked collagen and the control groups showed no residual NP tissue in the disc space, and terminal degenerative changes on histological sections and according to radiological assessments (Fig. 1). MRIs showed black discs, X-rays showed disc height drop of approximately 50% (Fig. 1). Histological sections showed extruded NP tissue in the paravertebral space. The NP in the disc space was replaced by connective tissue. The IVDs of both groups were stiffer then healthy discs and showed reduced damping qualities.
At 1 week, the cross-linked collagen had formed a macroscopically visible patch sealing the defect. FITC-stained cross-linked collagen showed a tight, zipper-like adhesion to the host AF and surrounding scar tissue. At 2 weeks, the collagen gel was infiltrated with host fibroblasts which remodeled the gel into organized fibrous tissue. At 5 weeks, cross-linked collagen formed a fibrous cap which bridged the fibers of the outer anulus and thereby repaired it. This fibrous cap consisted of fibroblasts embedded in a dense fibrous matrix. This fibrous cap was still visible after 18 weeks. In the uncross-linked and control groups, there was no repair tissue visible at the outer part of the AF at any time point. The disrupted annular fibers infiltrated the surrounding scar tissue.
Conclusion
Annular defects induced by needle puncture do not heal over 18 weeks in the described model and lead to extrusion of nuclear tissue, with subsequent degenerative changes affecting the entire IVD.
HDC is capable of repairing annular defects in a rat-tail model, thereby inhibiting these changes and improving the mechanical properties of injured discs. The repair mechanism appears to be induced by host fibroblasts which infiltrate and remodel the injected collagen gel. Annular tissue repair restored the mechanical properties of the injured discs.
Although the presented results are promising, experiments in larger animals with a spinal axial load similar to humans will be necessary to evaluate true clinical potential.
None declared
