Abstract

Introduction
Short-lasting unilateral neuralgiform headache with conjunctival injection and tearing (SUNCT) represents a brief headache syndrome first described in 1989 (1). Since its initial description SUNCT has been grouped with other brief duration headache syndromes in which autonomic features are prominent, such as cluster headache, under the general rubric trigeminal autonomic cephalagias (TAC) (2).
This group of conditions shares several features but appear, from a clinical perspective at least, to represent separate, definable disorders. Definitive classification will ultimately be determined by a clearer understanding of the pathophysiological basis underlying this group of conditions.
Although usually occurring without demonstrable structural abnormalities a small number of potentially symptomatic cases of SUNCT have been reported in which vascular malformations in the cerebello-pontine angle (3, 4) or brainstem (5) were discovered.
We describe a case of SUNCT occurring shortly after ischaemic brainstem infarction. To our knowledge this has not been previously described.
Case report
A 63-year-old Caucasian male with a remote history of adult-onset epilepsy and previous left cerebellar infarction presented with acute onset nausea, ataxia, vertigo and a sensory disturbance affecting the left side of the face and right lower quadrant.
All symptoms were maximal at onset. Seven days later left ptosis with miosis developed and novel unilateral headaches commenced. The headaches were stereotyped, lancinating in nature, sited around the left eye, and of brief duration – typically from 20 seconds to three minutes. Associated features included reddening and lacrimation of the left eye with minor nasal congestion. Triggering by tactile or motor stimuli was not reported. Maximum headache frequency was eight per day.
Physical examination confirmed a left Horner's syndrome (Fig. 1), decreased perception of pin prick affecting the left side of the face and right lower limb and flank, and poor tandem gait. Eye movements and facial power were unremarkable. Palatal movements and sensation were normal both on admission and subsequently.

A left Horner's Syndrome is present.
Magnetic resonance (MR) imaging revealed signs of an old left cerebellar infarct (Fig. 2a,b), noted several year previously on CT (Fig. 3), but no new evidence of infarction was seen. MR angiography demonstrated an occluded left vertebral artery but no other abnormality in posterior or anterior extracranial or intracranial circulation (Fig. 4). Haematological and prothrombotic investigations were normal. Biochemical investigation demonstrated moderately elevated cholesterol and triglycerides and an isolated elevation of γ-glutamyltransferase, attributed to ethanol use. Cardiac evaluation was unremarkable.

(a) A coronal T1W MRI demonstrating infarction in the inferior part of the left cerebellar hemisphere (arrowed). (b) An axial T2W MRI demonstrates a left cerebellar infarct (arrowed). The brainstem appears normal.
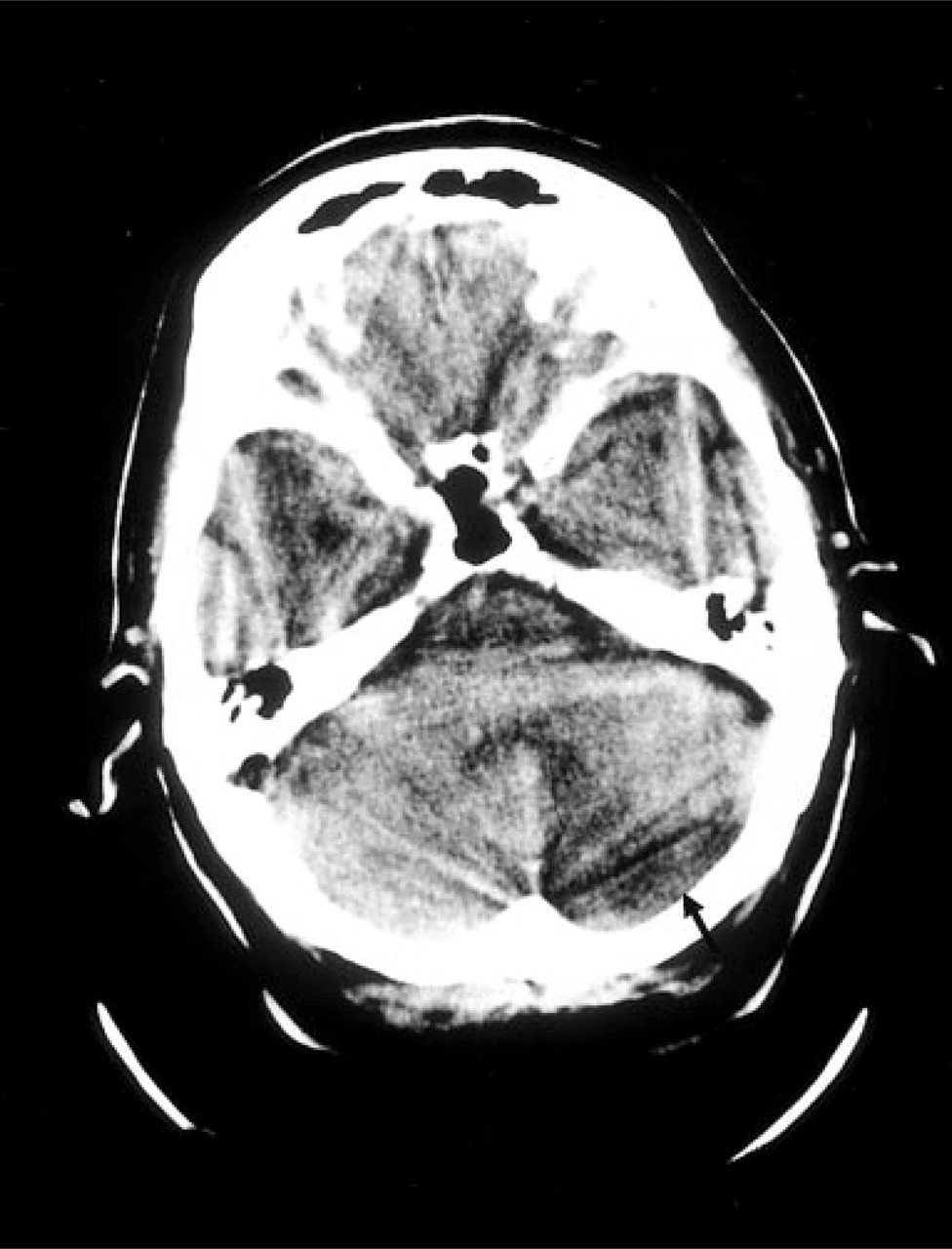
CT evidence of previous left cerebellar infarct (arrowed).

Magnetic resonance angiography reveals absence of flow in the left vertebral artery.
The headache frequency reduced over several weeks, without specific intervention. The Horner's syndrome resolved over approximately one month. The ataxia, nausea, and vomiting resolved over 3 months and the sensory signs settled over 9 months. A cocaine test performed 10 weeks after presentation confirmed complete resolution of the Horner's syndrome.
Discussion
The temporal relationship between the onset of symptoms indicative of caudal brainstem infarction, subsequent SUNCT and Horner's syndrome suggests that these events were linked. Moreover, resolution of the Horner's syndrome was mirrored by cessation of headache. It is intriguing that a delayed and transient Horner's Syndrome, noted several days after the crossed sensory disturbance, heralded the onset of headache and that both resolved in parallel. This suggests that both events shared a common pathophysiological basis, possibly akin to an ischaemic-penumbra. Subsequent resolution of the headache and Horner's presumably reflected recovery from this reversible process.
Although not radiologically apparent, the clinical deficit initially observed suggested involvement of the ascending spinothalamic tract and descending trigeminal fibres at or below their site of entry (and subsequent caudal passage) into the lateral pontine tegmentum. Accepting that a subtle and asymptomatic deficit of palatal power and sensation may have resolved in the days prior to presentation the initial vertigo (and subsequent transient Horner's Syndrome) without apparent IX and X involvement implies a lesion in the lower dorsolateral pons.
Previous reports of symptomatic SUNCT have involved intra-axial and extra-axial vascular lesions with presumed mass effect and a causal relationship not unreasonably inferred from the anatomical location (3–5).
This case demonstrates both an anatomical and temporal relationship between the development and resolution of SUNCT with highly localizing neurological symptoms and signs referable to dorsolateral brainstem tegmentum
The synchronicity of the Horner's syndrome with SUNCT in this case is of particular interest since the autonomic features of SUNCT are thought to represent parasympathetic activation (2). The sympathetic deficit reflected by the Horner's syndrome seen in this case might have contributed to a relative autonomic imbalance resulting in functional parasympathetic excess.
Although the temporal nature of the pain and autonomic features of Cluster Headache are clearly different from SUNCT a similar imbalance between sympathetic and parasympathetic activity would be consistent with the previously observed association between a Horner–like syndrome both with Cluster Headache (6) and trigeminal neuralgia (7).
