Abstract
Objective
Freshwater catfish are known to cause painful stings in humans. Stings usually cause mild envenomation and, in some instances, can lead to severe secondary bacterial infections. Sri Lanka is a tropical country where catfish stings are not rare. However, presenting signs and symptoms, complications, and management options are scarce in the literature.
Methods
A retrospective, descriptive, cross-sectional study was conducted by reviewing patient records in the university surgical units and surgical clinic in the teaching hospital in Anuradhapura, Sri Lanka, during 2015.
Results
Ten patients presented to the hospital following catfish stings. The common presenting features following stings were severe pain, swelling, and lymphadenopathy followed by cellulitis. Late complication such as tenosynovitis were also observed.
Conclusions
Routine procedures are sufficient to reduce further complications. However, people who are at high risk of encountering catfish, and travelers visiting tropical countries, should be aware of the possibility of stings and take necessary precautions.
Introduction
Catfish comprise more than 425 genera containing at least 3200 species. The majority are freshwater catfishes that live in tropical countries, and the minority are marine species.1,2 Freshwater catfish are known to inflict painful stings on humans. 3 Stings are a recognized occupational hazard among catfish farmers. 4 Stings can cause mild to severe envenomation or secondary bacterial infection.5,6
Freshwater catfish have 2 pairs of long barbels (maxillary and mandibular) that resemble cat’s whiskers. Despite the common belief that these barbels are harmful, they provide only a sensory function. 2 However, the majority of fresh and saltwater catfish also possess spines with basilar venom glands, which are covered by a thin integumentary sheath associated with their pectoral fins and dorsal fins.7,8 When compressed, the series of sharp recurving rays in the fins breach the victim’s skin and, subsequently, the integumentary sheath also gets damaged. The latter event leads to exposing the venom-containing cells and release of venom into the victim’s skin and underlying tissues.7,9 As a result, an inflammatory reaction may occur that may be later complicated by bacterial superinfection.5,9 Foot injuries occur when the catfish are stepped upon; most of these stings are from the dorsal spine. 9 Pectoral spine stings predominate in disentangling, cleaning, or fileting injuries. 9 Anal fins are involved in reproduction, and are not armed with spines.
Sri Lanka is a tropical country and considered a biodiversity hotspot.
10
There are 91 species of freshwater fish, 50 of which are endemic.
11
Airsac catfish belong to the family

A, Stinging catfish (
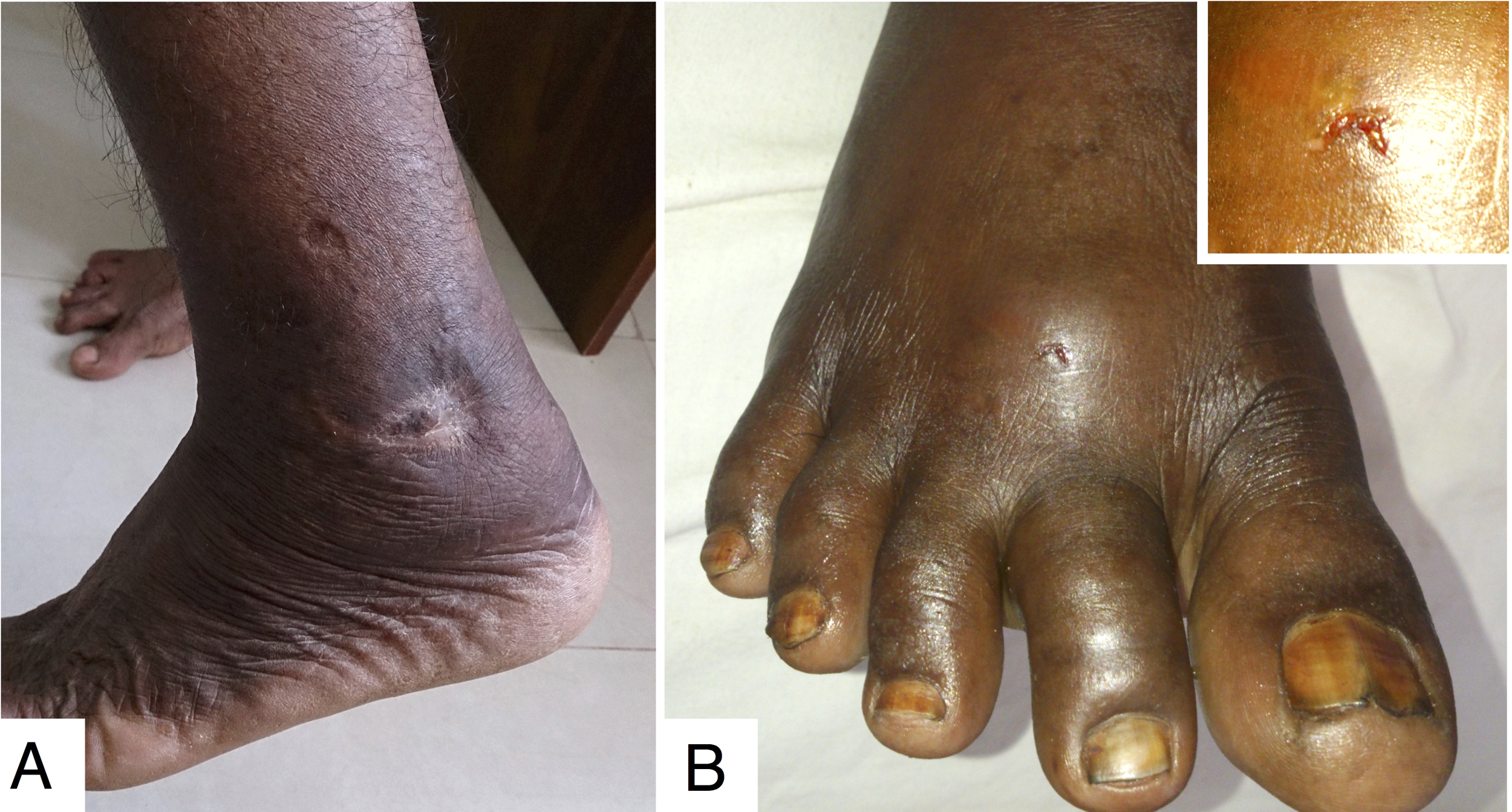
A, Healed wound of patient 6 after 6 months. B, Wound following
There are 103 rivers covering the island, and more than 10,000 ancient manmade lakes and ponds distributed across Sri Lanka.12,13 The majority of the manmade lakes are situated in the North Central Province (NCP). Anuradhapura is the largest district in NCP, and agriculture is the main source of livelihood. Catfish stings are not rare among the majority of agricultural workers and fishermen in the NCP and Sri Lanka. In his 1907 book on hunting, Harry Storey mentioned stinging catfish as, “The hungah is a repulsive-looking beast, slimy bodied, something like the waleya; has long feelers pendent from the mouth, and sting like ‘blazes.’” 14 Two cases of ankylosis of finger joints following catfish sting were reported in Sri Lanka, 1 in 1932 and 1 in 1960.8,15 Nevertheless, reports of the full profile of clinical presentations, management, and consequence related to catfish sting are scarce in the literature.
Methods
A retrospective, descriptive, cross-sectional study was conducted by evaluation of medical records of patients who were reported to be stung by catfish, and presented to the university surgical units and surgical clinic of the teaching hospital in Anuradhapura from January 1 to December 31, 2015. The pain at the time of admission was assessed by the medical officer who initially registered the patient using visual analogue scale (VAS) from no pain (0) to worst pain imaginable (10).
However, it may not reflect the true picture since the pain assessment was done after several hours, and in some instances several days after the incident. Ethical clearance was obtained from the Ethics Review Committee of the Faculty of Medicine and Allied Sciences, Rajarata University of Sri Lanka. The patients’ demographics, stinging incident, signs and symptoms, first aid used, management, and complications were recorded. Descriptive statistics were calculated using Microsoft Excel and a web-based calculator, GraphPad Software QuickCalcs.
Results
All 10 catfish stings presented during dry season (July–September) of the NCP (Table 1). The patients, all male, were 40.9±10.1 (mean±standard deviation [SD]) years. All of them sustained catfish stings while they were in manmade lakes. The majority (7/10) were farmers and the others were a fisherman, a mason, and a police officer. The foot was the most commonly stung part of the body (8/10) while there were 2 hand injuries. Stings to the foot occurred while patients were engaged in activities that disturbed the muddy floor of the lake, such as fishing (while walking inside lake), plucking lotus pods, and removing debris from a sluice gate. Two patients sustained hand injuries, 1 while washing a towel (catfish entangled in it) and the other while inserting his hand into a muddy hole.
Details of 10 catfish stings
Puncture wounds with bleeding were evident in the 4 patients who had foot injuries. All patients experienced pain at the time of the incident, and 8 patients rated the intensity of pain using a VAS (2 missing data). The mean score was 8.25±1.28 (SD). Seven patients had a VAS score of 8 or more. Three patients had experienced nausea at the same time. Five of them experienced a shooting type of pain at the time of sting, which radiated along the limbs. Initial pain lasted for 3 to 72 hours. Six patients reported a burning sensation that later progressed into throbbing. Four patients experienced numbness at the site of sting. One patient with hand injury experienced severe pain (pain score 10/10) and lost consciousness for short duration. All victims had limb swelling and erythema subsequently leading to cellulitis. Six patients developed transient lymphadenopathy in the affected limb. Two patients were admitted to the hospital on the same day of the incident, while others delayed (more than 1 day to maximum of 1 month) seeking hospital care. Of the delayed cases, 2 patients came to the hospital 1 month after the incident. One of them had tenosynovitis in the affected finger and the other had an abscess in the foot.
Pain was successfully managed with either or a combination of paracetamol and diclofenac sodium. Empiric antibiotic (IV or oral) treatment was used to cover both gram positive and anaerobic bacteria. Two patients who had abscesses underwent incision and drainage. One patient developed necrosis around the sting site, which was later debrided. This wound was subsequently treated with peeled skin of papaw (
Discussion
According to our findings almost all the catfish stings occurred during the dry season of the NCP. All the victims were males and the majority were farmers. What are the possible reasons for this pattern? On one hand, during the dry season the water level of the manmade lakes and other water catchment areas are low. As a result, all fish living in the catchment are confined to a smaller area, thus increasing the density of the fish, including stinging catfish. This increases the probability of sustaining a catfish sting for those in the water. During this season, along with skilled fishermen, agricultural workers resort to fishing as part-time work. These workers are not as skilled as fishermen who know how to carefully handle the stinging catfish without injuring themselves. Furthermore, experienced fishermen usually use local remedies that alleviate sting-related complications. We interviewed several fishermen of the Mahakanadarawa Fishermen’s Society and they said that some of them are able to tolerate the pain resulted from catfish stings after successive stings. Haddad et al. reported similar findings in their report as, “all fishermen who had been catfish accident victims reported that ‘the pain diminishes until it is imperceptible’ after successive stings.” 16 This may be a plausible reason for the fewer number of fishermen seeking hospital treatment in our study.
On the other hand, catfish spawning also occurs during the same season, usually in a hole or crevice in the bottom of lakes. If the site of spawning is disturbed by a foot or hand, catfish may feel threatened and consequently attack any offender who disturb their egg mass. 17
In other countries, fishermen, aquarium fish breeders, fishmongers, or anglers frequently sustained hand injuries. 18 –20 These stings to hands occurred while the person were unhooking a fish from a net, cleaning a fish tank, or during a sport called noodling of a fish. 17 Noodling is a popular sport in southern part of the United States where a sportsman catches a freshwater catfish by luring the fish using his or her hand as a bait, near a hole or crevice where the catfish dwells and protects its eggs. As soon as the catfish latches onto the hand, the fisherman grabs the gills and pulls it out with the support of his helper who is known as the spotter. In the present study, injuries were mainly seen in feet and much less in the hands.
Based on our case series, the main initial signs and symptoms of the catfish sting were severe pain (sometimes radiating), burning sensation, swelling, and erythema followed by cellulitis with secondary bacterial infections. The medical officer assessed the patients pain with VAS in 8 patients, however, due to delayed presentation it may be confounded by recall bias. Some tropical catfishes are capable of producing severe pain, which may last for more than 48 hours. 5 In a study done by Huang et al., the severity of the pain was assessed and reported with a pain score. 9
The signs and symptoms associated with catfish stings in our study were less debilitating when compared with reports from other parts of the world. The more serious injuries reported by others include deep lacerations,
17
ulnar nerve damage,
19
or radial artery damage.
21
Stinging catfish are comparatively smaller than aforementioned catfishes (brown bullhead [
In the literature, a wide range of microorganisms have been reported to secondarily infect the wound inflicted by catfish. These include species found in both freshwater and saltwater environment such as
The toxins isolated from the venom glands of catfish have been shown to exhibit hemolytic and neurotoxic properties.
25
Al-Hassan et al showed that “epidermal secretions” of the Arabian gulf catfish (
Pain management was successfully achieved with paracetamol or diclofenac sodium (alone or in combination). Two patients required surgical intervention for the abscesses, and one had a necrotic area around the sting site which was debrided and later dressed with papaw latex-based pulp dressing until full recovery. Papaya latex consists of papain, shown to be effective in facilitating wound healing. 28
In other parts of the world, some described methods for immediate management following catfish stings involved immersing the limb in warm water for approximately 45 minutes. The limb would be elevated and tetanus toxoid given, if indicated. X-rays were taken to identify the spine of the catfish. The wound was thoroughly irrigated, if significant. 7 ,9,29,30 Shiomi et al. revealed 1 hemolytic factor, 2 edema forming factors, and 2 other lethal factors in the venom of oriental catfish. These are heat labile and completely inactivated at 45°C for 10 minutes. This could be the basis for treatment with immersion of sting site in a hot water. 31 However, specific management should be carried out depending on the specific injury sustained.
The main reason for delayed presentation to hospital in our patients was the application of home remedies based on local beliefs. These remedies consist of exposing the sting site to hot vapor emanating from burnt leaves or dried elephant dung, or urinating on the sting site. Exposing the sting site to heat could inactivate the aforementioned heat labile components of venom, and it could explain the scientific basis behind the home remedies. The effectiveness of these remedies may therefore lessen the number of hospital admissions and mask the real burden of stings.
The major limitation of this study is the small sample size and the recall bias associated with VAS score.
Catfish stings are not rare in tropical countries and fishermen, farmers, and travelers are at risk. Travelers visiting tropical countries and people are high risk of sustaining catfish stings should be aware of the possibility of stings and should take necessary precautions.
Acknowledgments: We thank Professor SB Agampodi for the initial support of the study. We thank Ms. T. Wanasinghe, librarian, for her support in retrieving of articles. We are grateful to Mr. CS Senevirathne and Mr. DLC Siththarage of the Department of Pathology for assistance in the preparation of specimens. We would like to thank Dr. S. Nilkantha for providing specimen for illustration, and the Mahakanadarawa Fishermen’s Society for providing live and dead catfish specimen for photographs. We specially thank the editorial team of
Author Contributions: Study concept (SPBT); reviewed the literatures (SPBT), (BTBW); drafted and edited the manuscript (SPBT, BTBW); reviewed all the medical records (SPBT, BTBW, NPS); drew the illustrations (NPS); obtained photographs and did the histological identification (BTBW).
Financial/Material Support: None.
Disclosures: We did not kill any catfish for the present study. All live catfishes bought for photographs were later released to their natural habitats. For histology specimens, we bought dead catfish specimens from the fishermen.
Footnotes
Submitted for publication July 2016.Accepted for publication March 2017.
