Abstract
We present a case of a 57-year-old man who fell while climbing a mountain in California and sustained severe facial trauma. Three firefighters and 2 emergency physicians witnessed the fall and resuscitated the patient. The patient ultimately required a surgical cricothyrotomy performed with a pocket knife and Platypus hydration pack. The physicians made a makeshift positive pressure airway device using the Platypus hydration pack. We believe this is the first case report describing an improvised cricothyrotomy performed in the wilderness using only hiking gear. This report also discusses indications for cricothyrotomy, the challenges of resuscitation in a low-resource environment, and special considerations in a high-altitude setting.
Keywords
Introduction
Cricothyrotomy is indicated in trauma patients who cannot oxygenate or ventilate on their own. Substitutes for airways in wilderness medicine settings are theoretically discussed in academic settings but are rarely used in real resuscitations. A 2013 case report describes a surgical cricothyrotomy on a rock climber in the wilderness using the blade of a multipurpose tool and prehospital equipment. 1 Upon review of the literature, there were no published reports of an improvised cricothyrotomy in a wilderness setting using only hiking gear. This case report describes an improvised cricothyrotomy performed with a pocket knife and Platypus hydration pack by 2 emergency physicians on a climber with facial trauma who fell about 1500 feet. The authors of this article are the 2 emergency physicians who performed the cricothyrotomy and the flight nurse who continued the resuscitation.
Case Presentation
In the summer of 2015, a 57-year-old man fell on a steep slope on a mountain in California while climbing at an elevation of 12,500 feet at approximately 6:00
Three firefighters climbing with their own team reached the patient first and assessed him. They rolled the patient over on the snow where he was found, took off his helmet, and assessed his airway. They noted the patient to have a pulse and spontaneous respirations. No sources of bleeding or obvious limb deformities were found. They kept the patient’s C-spine in a neutral position and called for helicopter rescue.
The physicians reached the patient 15 minutes later (Figure 1). The patient had a pulse and irregular respirations. His face had diffuse contusions, superficial bleeding, and severe swelling. A pupillary examination was unable to be done due to the degree of facial trauma. The patient was making incomprehensible sounds and intermittently spontaneously moving his right upper extremity. He was unable to answer questions or follow commands.

Rescue scene at 11,000 feet.
Because of irregular and gurgling respirations, the patient was suspected to either have an unstable facial fracture or blood in his airway preventing adequate oxygenation and ventilation. Traumatic brain injury was also considered as a cause of irregular respirations. Due to concern for airway obstruction, the physicians decided to perform an improvised surgical cricothyrotomy on the patient although they only had hiking gear and a first aid kit.
The cricothyroid membrane was palpated on the patient. An initial vertical cricothyrotomy incision was performed with a pocket knife followed by deeper horizontal incisions. There was minimal blood loss. A finger covered with a hiking glove palpated inside the incision to confirm entry into the airway. A substitute endotracheal tube was made by removing tubing from the Platypus hydration pack and cutting the tubing to a smaller size. This was inserted into the patient’s airway. Respirations were felt coming into and out of the tube and misting was noted in the tube. The patient then had more regular respirations and equal chest rise and fall. Because he had spontaneous respirations, the rescuers did not blow directly into the tube. The tube was secured with suture from a self-made first aid kit carried by one of the physicians (Figure 2).
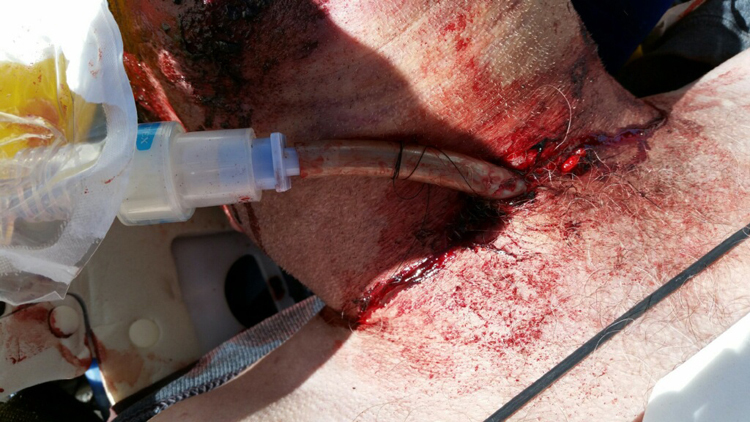
Surgical cricothyrotomy with Platypus tubing. This picture shows the tube after it was connected to the airway equipment on the helicopter.
A Fitbit exercise monitoring device worn by one of the physicians was placed on his right arm in an attempt to monitor his heart rate. Unfortunately, his extremities were too cool and his heart rate was not detected by the device. The patient was on the snow wearing several layers of clothing. The rescue team used their jackets and extra clothes to keep the patient warm and used a pair of pants to bind the patient’s pelvis in case of an unstable pelvic fracture. The entire rescue team then laid their bodies beside and gently on top of the patient to keep him warm given the concern for hypothermia. The temperature at the rescue scene was just below freezing. Helicopter rescue was reported to be on its way but there was no estimated time of arrival.
Thirty minutes after the cricothyrotomy was performed, the patient began having more irregular respirations. Increasing blood was noted within the tube. The physicians were concerned that there could be more blood within the airway, a hemothorax, or pulmonary contusions. There was need for a bag valve device to deliver positive pressure, so an improvised bag valve device was created out of the rest of the Platypus hydration pack and tubing. The improvised endotracheal tube was connected to the extra Platypus tubing and empty 2 L bladder of the hydration pack with duct tape. Then, another small incision was made in the opposite end of the bladder. Another piece of tubing cut from the hydration pack was inserted into this hole. This piece of tubing was held into the bladder with duct tape. The rescue team would blow into this second tube to inflate the bladder, pinch off this tube with pliers to prevent air backflow, and then push down on the inflated bladder to deliver a breath (Figure 3). This worked effectively until a medical helicopter attempted to land at the scene about 1 hour after the patient’s fall. This medical helicopter staffed with a critical care flight nurse and critical care paramedic could not ultimately land because of the weather.

Positive airway pressure device made with Platypus hydration system.
Approximately 45 minutes after the medical helicopter tried to land, another helicopter staffed with an advanced life support paramedic arrived. This helicopter did not land but dropped a rescue stretcher to the ground with ropes. The rescue team helped stabilize the patient’s C-spine with provided blocks and strapped the patient carefully onto the stretcher while the physicians watched his airway. As he was being strapped in, the patient lost a pulse and chest compressions were performed for 2 minutes. The patient regained a pulse and was pulled up into the helicopter using ropes. Advanced cardiac life support (ACLS) resuscitation was continued for a few minutes until this helicopter was able to land at 7000 feet to meet the medical helicopter with the critical care flight nurse.
At 7000 feet, the flight nurse started to care for the patient. The medical helicopter started flying to the nearest trauma center in Redding, California, with an estimated flight time of 25 minutes. The patient was noted to be in ventricular fibrillation and had several shocks administered. Epinephrine was administered per ACLS protocol. For the airway, the flight nurse kept the original tube placed within the airway and removed the rest of the Platypus hydration pack (the remaining tubing and the empty 2 L bladder). The flight nurse used a 6.5-mm endotracheal tube adapter to connect the original tube to the bag valve device and then to the ventilator. The patient was noted to have no resistance in the airways while being bagged initially with a bag valve device. A bougie also confirmed placement in the airway. The patient was then connected to the ventilator and initial end-tidal CO2 was in the teens. When the patient briefly regained a pulse, end-tidal CO2 went up to 80 mm Hg. The flight nurse noted that the rhythm appeared to be a sinus rhythm. Intraosseous access was established. The patient then lost his pulse again and fluctuated between asystole and ventricular fibrillation. Bilateral midclavicular needle decompressions of his chest were done. Hemothorax was noted bilaterally after needle decompressions and the patient did not regain a pulse. The flight nurse continued resuscitation for about 20 minutes. When the patient remained pulseless for 20 minutes, the flight nurse called the medical director. The patient was pronounced dead on the way to the trauma center.
Discussion
This case report illustrates how an improvised cricothyrotomy can be used in the wilderness. The 2013 case report of a cricothyrotomy in the wilderness led to an ethical debate on when cricothyrotomies in the wilderness should be performed.2,3 In our case, there was a clear indication for a cricothyrotomy. The patient had facial trauma with a presumed obstructed airway and there was no standard airway equipment available to oxygenate and ventilate the patient. In addition, both physicians were adequately trained and board certified in emergency medicine with training in trauma, difficult airway, and wilderness medicine. A recent meta-analysis of prehospital airway management describes a success rate of 90.5% for surgical cricothyrotomy with trained prehospital personnel. 4 There were multiple ways in this case that correct placement of the improvised endotracheal tube was confirmed: palpation of the airway by a gloved finger, misting of the tube, palpation of breath coming in and out of the tube, equal and adequate chest rise and fall, bougie, and end-tidal CO2 monitoring.
The previously mentioned 2013 case report discusses a surgical cricothyrotomy performed on a climber who fell 80 feet. The cricothyrotomy was performed by a rescue team that included a physician in a wilderness setting. A multipurpose blade and 6.0-mm cuffed endotracheal tube were used after sedation and paralysis. The patient survived and was able to return to climbing. A case report from 2002 describes a roadside cricothyrotomy done by a bystander physician after a rural rollover motor vehicle accident. This cricothyrotomy was done with a pocket knife and an improvised endotracheal tube was made with ribbed drinking straw from a sports bottle. 5 This report also estimates and compares the resistance of standard endotracheal tubes, sports bottle straws, and ballpoint pens. Using Poiseuille’s equation, the resistance of airway flow will be inversely proportional to the fourth power of the radius of the tube and directly proportional to length. The sports bottle straw in this case was found to have similar airway resistance compared with a standard endotracheal tube. In this case and in a later review of ballpoint pen tubes, most ballpoint pens are considered unsuitable as airway devices because of small diameter and therefore high resistance. 6 In our case, we used a Platypus tube with a measured internal diameter of approximately 6 mm, which is comparable to the diameter and therefore resistance of a size 6 endotracheal tube. The Platypus tube was quite rigid. The consistent delivery of breaths to the patient without resistance indicated that the tubing was not significantly collapsing under the pressure of soft tissue swelling. The length of our original makeshift tube was estimated to be similar to a standard endotracheal tube but was not measured at the scene. When the adapter tubing was used later in our resuscitation, there was increased length and resistance. However, this was necessary for the protection of the providers at the scene due to blood in the airway.
The patient was resuscitated in a hypoxic environment at an elevation of 11,000 feet. Based on altitude, the partial pressure of inspired oxygen was decreased and therefore the baseline oxygen saturation of the patient was decreased as well. Supplemental oxygen would have been helpful at the scene to increase the fraction of inspired oxygen but was not available. In addition, the patient had been climbing for multiple days and was at least partially acclimatized to altitude. He likely had respiratory alkalosis with compensated metabolic acidosis and lower than normal partial pressure of carbon dioxide level. During resuscitation, the improvised bag valve device was made to deliver positive pressure to the airways. It was theorized that using this improvised device would increase positive end-expiratory pressure (PEEP), which could improve oxygenation by clearing debris and blood from the airway and reopening collapsed alveoli. We estimate that we gave about 12 breaths per minute giving a respiratory cycle of 5 seconds. Without knowing the exact resistance of the system and true delivered volume of our breaths, an exact level of PEEP cannot be estimated. However, our respiratory cycle was relatively short and the patient was expiring through our system of tubing. Therefore, we suspect that the patient had some expiratory flow at the beginning of our next delivered breath resulting in PEEP.
Although this is a tragic case that ultimately resulted in death, we illustrate how an improvised surgical cricothyrotomy can be done in the wilderness by properly trained providers carrying a hydration pack and a multipurpose blade. We hope that future providers can use a similar strategy to successfully resuscitate carefully selected patients.
Acknowledgments: This resuscitation was performed and aided by the authors and the following people and organizations: Redding firefighters including Captain Rik Valles, Cody Buick, Aaron Dieck; PHI Air Medical rescue helicopter personnel Tom Coe and Chip Duckett; Tim Mincey and SWS Mountain Guides; and Todd Parsons.
Author Contributions: Study concept and design (CJ, DG), Acquisition of the data (CJ, DG, IP), Analysis of the data (CJ, DG, IP), Drafting of the manuscript (CJ), Critical revision of the manuscript (CJ, DG), Approval of final manuscript (CJ, DG, IP)
Financial/Material Support: None.
Disclosures: None.
Footnotes
Submitted for publication April 2016.
Accepted for publication August 2016.
