Abstract
Objectives
The unique challenges posed by the Antarctic environment include both physiological and psychological stressors to the individual as well as the limited onsite medical capabilities available to address them. This report compares medical clinic utilization among 3 US Antarctic stations to identify differences in diagnostic frequency and utilization of clinic resources under current medical prescreening regimes for summer and winter seasons.
Methods
Clinic data from 3 Antarctic locations (McMurdo Station, Amundsen-Scott South Pole Station, and Palmer Station) for the 2013−2014 Antarctic year were reviewed for patient encounter frequency by season, and provider-assigned visit diagnostic category. Differences between relative diagnosis frequencies among stations were analyzed, and per-capita clinic utilization was compared.
Results
The McMurdo clinic recorded 1555 patient encounters, with South Pole Station reporting 744 and Palmer with 128 encounters over the year. The most frequent reasons for clinic visits were orthopedic and dermatologic, with increased visits at McMurdo for respiratory illness and at the more remote locations for neurologic complaints and insomnia. Altitude-related visits were reported only at McMurdo and South Pole stations.
Conclusions
The clinic volume predictably correlated with station population. Insomnia and headache complaints, reported only at the South Pole Station, are likely associated with the increased elevation at that site, although they could be attributable to psychological stress from the isolated environment. Although the majority of cases could not be prevented with current screening, we suggest several changes to the current concept of operations that may decrease medical utilization and provide significant improvements to health care delivery on the ice.
Introduction
The unique challenges posed by the Antarctic environment to the human body have been previously well described.1,2 These challenges encompass both physiological and psychological stressors to the individual as well as limited onsite medical capabilities available to address them. Decreased physical activity, exposure to prolonged day and night periods during the progression of the Antarctic year, relative isolation, and severe and often rapid changes in altitude all contribute to changes in cardiovascular, endocrine, circadian, and psychological response. 3 –5 As medical issues arise, health care providers on the ice must utilize available resources to meet the majority of needs at the point of discovery without reliance on remote support.
The University of Texas Medical Branch (UTMB) Center for Polar Medical Operations, through the National Science Foundation’s Antarctic Support Contract, has provided the training and deployment of medical support personnel to all 3 stations of the US Antarctic Program since 2012. These stations vary significantly in accessibility and relative isolation, population, and environmental factors. McMurdo Station (MCM) is the largest community on the continent, located on the coast at 21 m above sea level, whereas Amundsen-Scott South Pole Station (SP) has a field elevation of 2834 m and density altitudes frequently >3353 m.2 Palmer Station (PAL) is located on Anvers Island, north of the Antarctic Circle, and is a coastal station with routine maritime traffic throughout the year. Average station populations by season are reflected in Table 1.
US Antarctic station average populations and clinic medical staffing resources by season
Staffing numbers represent on-the-ground personnel during the 2013−2014 season.
A part-time resource pharmacy technician was shared between McMurdo and Amundsen-Scott South Pole stations.
Each Antarctic station provides primary care via onsite medical clinics, staffed by medical providers year-round. Medical staffing varies significantly with station population, particularly at MCM where station populations undergo the largest seasonal variation (Table 1). Clinic visits range from preventive medicine, such as screening examinations and immunizations required for transfer to the more remote stations, to regular management of known conditions, to more emergent presentations. The majority of medical conditions are managed via the resources available at each clinic, although truly emergent conditions may prompt medical evacuation (MEDEVAC) to more capable facilities, such as MCM, or even off the ice. Alternatively, onsite providers can recommend and implement Medical Administrative Movements (MAMs), which are planned transports to definitive care or further diagnostic testing. MAMS do not involve a medical escort, nor do they require emergent scrambling of resources for evacuation.
Because of the less reliable access of resupply and MEDEVAC resources to all US stations during the winter months, extensive screening for physical and psychological wellness has been instituted. Separate criteria have been established for a spectrum of chronic disease states, but the classification scheme is the same: Patients’ disease control will fit criteria for summer deployment only (least stringent), winter deployment (most stringent), or be deemed unsafe for either. Given the large variations in seasonal population at MCM and SP, a segment of the population who may be deemed unfit for winter deployment will be present for the summer season, implying good but not ideal disease management. Given the scarcity of resources in an austere environment, a desire exists to optimize such screening thresholds to identify individuals who may currently meet screening criteria but will place a disproportionate burden on clinic or evacuation resources. Differences in medical utilization between stations may similarly suggest high or lower-risk locations, which could be useful in medical resource planning.
This report compares medical clinic utilization during the March 2013 to February 2014 Antarctic year to identify differences in relative diagnostic frequency and utilization of clinic resources toward these goals.
Methods
Clinic visit tracking was reviewed using 2 different sources for each Antarctic station. First, medical providers at each station produce weekly situation reports (Sitreps) that record clinic utilization data, MEDEVACs, dental examinations and procedures, laboratory studies, physical therapy utilization, and similar metrics, itemized in Table 2. These deidentified reports are submitted to the Center for Polar Medical Operations in the course of standard operating procedure and, in aggregate, comprise the Sitrep Database. Each station has a secondary Clinic Log for recording additional detail on patient encounters. MCM utilizes a Microsoft Access Clinic Database, in which providers may include information on medical comorbidities, diagnoses given, prescriptions provided, and tests ordered. SP and PAL clinic providers utilize encrypted Microsoft Excel documents for these purposes. Note that Sitreps report the number of individuals who visit the clinic, whether they are seen as a patient encounter or treated for a given diagnosis, and Clinic Logs specifically record patient encounters and the diagnostic categories assigned by providers to that encounter. Categories available for provider selection are detailed in Figure 1 and are assigned by providers on the ice at the point of care. These categories inherently contribute to some of the limitations of this study, as discussed later.
Clinic utilization at 3 Antarctic stations during the 2013−2014 Antarctic year
Data reported are extracted from aggregate, weekly reports (Sitreps) as generated by medical providers at each location. MAM, medical administrative movement; MEDEVAC, medical evacuation.
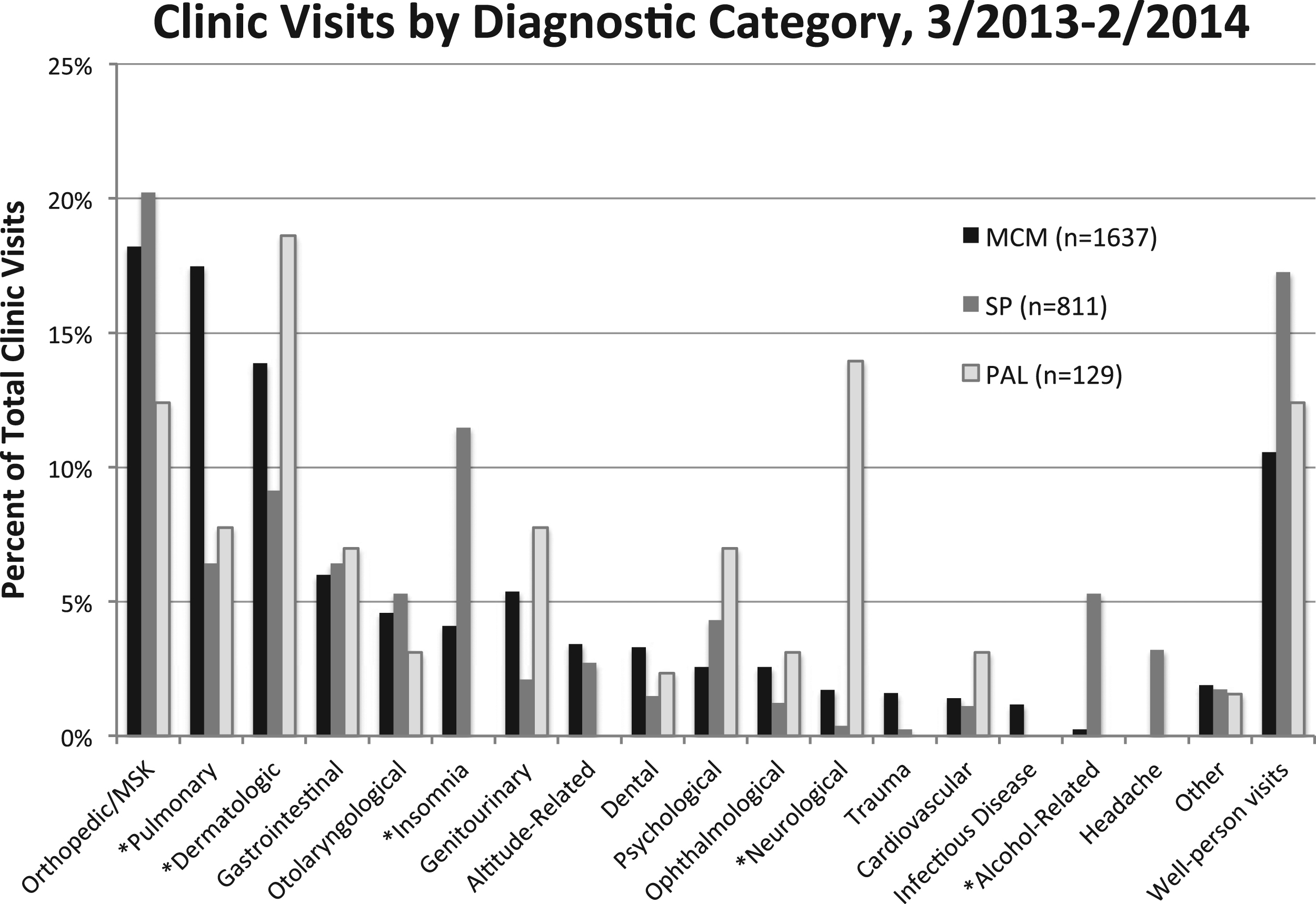
Clinic visits by diagnostic category, 2013−2014. Asterisks denote categories that demonstrate statistically significantly differences in frequency of complaints among the clinics. MCM, McMurdo Station; SP, Amundsen-Scott South Pole Station; PAL, Palmer Station; MSK, musculoskeletal.
All data were reviewed for frequency of clinic visits, diagnostic categories of visit complaints, and date of encounter. Because all sources of visit and encounter data are independent and require duplicate data entry, minor discrepancies between sources were identified. These discrepancies are attributed to medical provider error in duplicate data entry. Because of the coarseness of Sitrep data, repeat visits could not be calculated with accuracy for comparison to Clinic Logs and so are reported from Logs alone. Where disagreement in encounter numbers exists between sources, both are reported. Although Clinic Log diagnostic category data were only systematically collected starting with the 2013−2014 season, limited data from Sitrep reports were available for all US stations for the 2012−2013 year, providing a single-point comparison for total population, total clinic visits, dental, and physical therapy visits.
Descriptive statistics were employed using Microsoft Excel to compare visit trends and diagnostic categories within Antarctic Stations and by seasons. Differences between visit and diagnostic frequency at each location were analyzed using Student’s t tests and χ2 analyses.
Results
According to the aggregate Sitrep Database, MCM clinic saw 576 patients in winter (March−September) and 1298 patients during the summer (October−February) months, for a total of 1874 for the year. During the same time, MCM providers recorded 1555 patient encounters in the Clinic Log. These 1555 encounters were attributed to 658 individuals, with 1637 unique diagnoses and 82 comorbidities (some patients received multiple diagnoses at a single encounter). Inpatient days tracked with population (Table 2), with MCM having markedly higher hospitalization rates than SP or PAL. Orthopedic injuries (particularly muscular strain) were most common (18%), followed by upper respiratory infections (17%) and dermatologic conditions (14%), with gastrointestinal complaints (6%), otolaryngologic concerns (5%), and insomnia (4%) comprising the next most frequent complaints. Additionally, 11% of visits were recorded as well-person examinations, screening visits, or immunizations (Figure 1). A total of 10 MEDEVACs were recorded from MCM, 8 during summer and 2 during winter, for diagnoses including trauma, suicidal ideation, appendicitis, angina, and malignancy. In addition, 27 MAMs took place over the summer, and none during the winter. Per capita rates for MEDEVACs and MAMs were 0.01:1 and 0, respectively, for winter, and 0.01:1 and 0.04:1 for summer months given reported station populations.
The SP Sitrep reported 734 annual visits during the 2013−2014 Antarctic year. According to the SP Clinic Log, there were a total of 744 clinic visits from 212 individual patients. During these visits, 811 clinical diagnoses were identified, with 67 reported comorbid diagnoses. Leading diagnoses again consisted of orthopedic injuries (13%), followed by insomnia (11%) and dermatological complaints (9%), with gastrointestinal, upper respiratory, and alcohol-related issues comprising an additional 17% (Figure 1). A further 17% of visits were recorded as well-person examinations, screening, or immunizations. Only 12 dental examinations or procedures were performed over the year (1% of total visits). Two MEDEVACs were required from SP, both during summer, for atrial fibrillation and renal calculi (per capita rate of 0.02:1 given summer population); additionally, 2 MAMs were performed, also during summer months.
According to Clinic Logs, 71 individuals accounted for 128 patient encounters to the PAL clinic over the course of the 2013−2014 Antarctic year, with 129 recorded diagnoses. During the same period, the Sitrep Database recorded 134 clinic visits. Leading diagnoses consisted of dermatological complaints (19%); neurological issues (14%), primarily malaise and disequilibrium attributed to seasickness from vessel-bound patients; and orthopedic injuries (12%). Pulmonary, gastrointestinal, and genitourinary complaints contributed an additional 23% (Figure 1). A further 12% of visits were attributed to well-person examinations, screening visits, or immunizations. Of note, PAL demonstrated the highest frequency of psychological visits, with 7% of total encounters recorded as psychological or behavioral concerns. Only 1 MEDEVAC was required from PAL, for suicidal ideation (0.03:1 per capita MEDEVAC rate given station population); additionally, 2 MAMs took place, 1 during the winter and 1 during the summer, for rates of 0.04:1 and 0.03:1, respectively.
Orthopedic injuries and dermatologic complaints were the most frequent contributors to clinic utilization across all 3 locales. Orthopedic injuries consisted primarily of muscle strains (including shoulder, low back, and neck) in manual labor positions and contributed much of the physical therapy utilization. Dermatologic cases were dominated by lacerations, contact dermatitis, and fungal nail infections; these dermatological injuries were seen significantly less frequently at SP.
Table 2 provides Sitrep Data including the number of recorded injuries and onsite accidents, clinic procedures during summer and winter months, number of medications given, inpatient days, and diagnostic imagery resources utilized during the 2013−2014 Antarctic year. Month-to-month clinic usage at each site is represented in Figure 2A. When seasonal total visits from Sitrep are normalized by average seasonal station populations, a significant increase in per capita clinic utilization was identified at MCM during winter months (P < .001). Frequent clinic visits by a relatively small number of individuals were noted at SP, with 93 individuals accounting for 637 of the 744 clinic visits. In other words, 44% of the visiting patients were responsible for 86% of visits throughout the year. This corresponded to the highest per capita rate of clinic utilization among the US stations. SP demonstrated no significant change in per capita clinic visits during the winter season (8:1 during the summer, 10:1 during the winter) although this difference was not statistically significant. Similarly, no seasonal variation was noted at PAL, which maintained a utilization ratio of 4:1 throughout the year (Figure 2B).
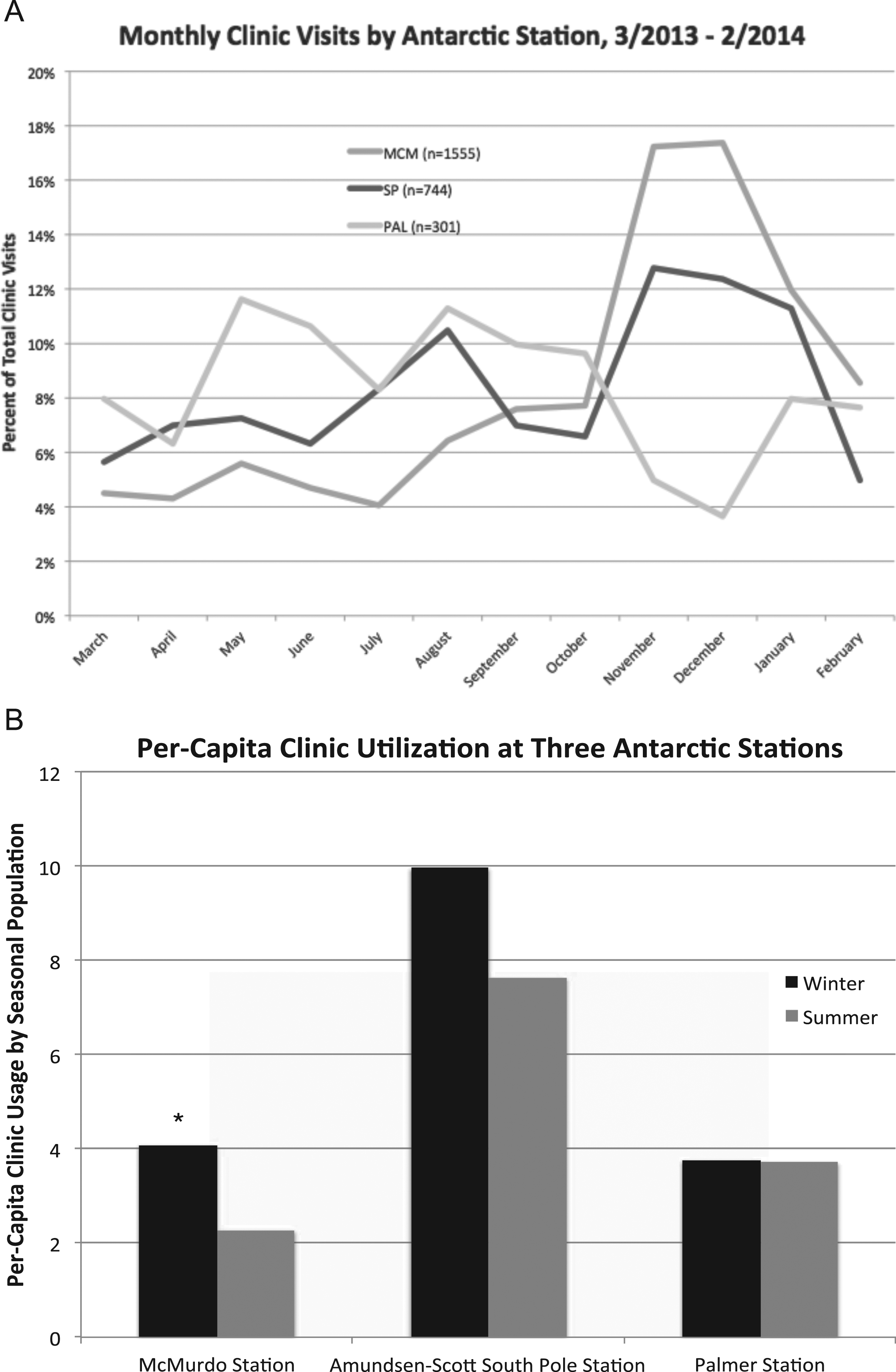
(A) Monthly clinic visits by Antarctic station, March 2013−February 2014. (B) Per capita clinic utilization at 3 Antarctic stations. Note that axis labels represent ratios (visit/population) for each clinic and season. Asterisk denotes statistical significance between winter and summer rates of utilization. MCM, McMurdo Station; SP, Amundsen-Scott South Pole Station; PAL, Palmer Station.
Significantly higher rates of neurological complaints were noted at the PAL clinic (14%) compared with MCM (2%) for the year (MCM vs PAL: P < .001), whereas the SP clinic saw significantly lower neurological complaints over the year (<1%) compared with the MCM clinic (MCM vs SP: P < .01). There was no significant difference in the comparative frequency of altitude-related visits at MCM vs SP clinics, with each accounting for 3% of total visits, despite the fact that SP is located at a significantly higher altitude than the sea-level MCM. However, the only clinic reporting complaints of headache was SP clinic, which also accounted for 3% of cases. In addition, SP clinic saw a significantly higher frequency of insomnia complaints (11%) compared with MCM (4%) over the year (MCM vs SP: P < .001). Conversely, SP saw significantly fewer dermatologic complaints (9%) than MCM (14%) (MCM vs SP: P < .001). Pulmonary-related complaints were significantly lower at both SP and PAL than at MCM (MCM vs SP: P < .001; MCM vs PAL: P < .001). Alcohol-related visits were significantly more frequent at both SP and MCM compared with PAL (SP vs MCM: P < .001; MCM vs PAL: P < .001), with no visits related to alcohol logged at PAL and <1% of all cases being related to alcohol at MCM, compared with 5% at SP (Figure 1).
Limited information was available from the 2012−2013 Antarctic year, with a reported number of 3862 aggregate clinic visits over the 3 sites via Sitreps. This corresponds to a decrease of approximately 30% in clinic usage during the 2013−2014 year compared with the prior year. MCM alone saw 2868 visits during the 2012−2013 year, a 35% higher volume than the number of visits seen the subsequent year. Of note, physical therapy and a dedicated dental provider were unavailable during 2013−2014 Antarctic summer, although visits for these services accounted for 1468 and 447 encounters, respectively, during the 2012−2013 year. The lack of dedicated practitioners for these services may easily account for the between-year difference at MCM.
PAL saw an even more dramatic decrease in overall utilization from 2012−2013, with 180 fewer patients seen in the subsequent year, a 43% decline. In contrast to both MCM and PAL, SP clinic saw increased numbers of patients in 2013−2014 compared with the prior year, with 54 additional patients seen. Despite this increased clinic utilization at the South Pole Clinic, there was a large decrease in the number of dental examinations or procedures performed, with only 12 procedures and examinations recorded over the course of 2013−2014 compared with 38 during the prior year.
Discussion
Clinic volume predictably correlated with station population at MCM and SP, with the increased summer populations bringing increased clinic utilization and higher overall numbers at the more populated stations. In contrast, no such seasonal variation was noted at PAL, consistent with year-round population stability. The predominance of orthopedic and dermatologic complaints across all station locations is in agreement with what has been reported from other Antarctic surveys in the past and is unlikely to be affected by more rigorous screening. 6 –8 However, the spectrum of headache and insomnia (although not directly attributable to altitude effects), combined with explicitly recorded altitude-related visits at SP despite current screening guidelines suggest changes in timing of pretreatment, more aggressive education regarding pretreatment, or tightening of current screening restrictions for individuals with a history of chronic obstructive pulmonary disease (COPD) or tobacco use. Working at altitude may result in a decrease in medical utilization, because of some evidence of delayed onset of symptoms and acclimatization in these patients. 9 A potential change in the medical concept of operations for SP may also involve new arrivals reporting to the clinic within the first hour of arrival, as some evidence has suggested that individuals at risk for development of altitude symptoms may in some cases be identified prior to onset with a simple examination, although the reliability of such examinations and even a prior personal history of acute mountain sickness appears to be low.10,11
The significantly higher rate of pulmonary-related visits at MCM compared with the other 2 clinics is likely attributable to several factors. The increased viral reservoir and communicability within the larger station population likely contributes to clinic utilization, and in fact the “McMurdo Crud” is a well-known phenomenon among station crewmembers. Summer staff are subject to more liberal screening requirements than those who remain over the winter, resulting in a large summer population at MCM consisting of less rigorously screened staff. Although individuals with well-controlled mild-stage COPD or similar structural pulmonary disease may meet summer screening criteria, such individuals may be more susceptible to respiratory virus syndromes, thus both directly contributing to clinic utilization and indirectly by serving as a viral reservoir.12,13 Although the authors believe this reasoning is sound, station clinic data from the 2013−2014 year do not reveal what proportion of pulmonary-related encounters are attributable to patients with a preexisting diagnosis of COPD. Future efforts to examine this relationship could have an impact on screening recommendations.
Neurological complaints accounted for fewer than 3% of cases at MCM and SP, yet they were the second-highest cause of PAL encounters. Although MCM and SP are truly isolated environments during the Antarctic winter, the use of PAL as a year-round maritime port does ensure a degree of physical contact with the outside world. Even so, any psychological benefit gained from contact with vessels may be offset by the comparatively small staff population, more akin to a base camp, resulting in PAL staffers having less total human contact over the course of the Antarctic year. Comparatively, even in the midst of winter the several hundred staff members at MCM may promote greater social stimulation than the population of approximately 30 PAL inhabitants. Previous studies have noted the somatization of symptoms attributable to psychological stress taking on the form of vague complaints, including vague neurological symptoms, insomnia, and headache.14,15 Although many of the neurologic (malaise and disequilibrium) complaints at PAL are attributed by staff to seasickness, the number of nonstaff patients is unknown. If a component of somatization exists, an expansion of the more thorough winter psychological screening to all Antarctica-bound personnel may have a profound effect on stations with smaller populations such as PAL.
Similar nonspecific complaints, such as headache and insomnia, were seen regularly at the SP clinic at a higher frequency than at other clinics. Insomnia was the second-highest cause of SP utilization during the Antarctic year. The field elevation at SP suggests a cohesive explanation because both headache and insomnia are well-known, early heralds of acute mountain sickness.16,17 Although MCM is located at near sea level and the SP station at 2834 m above sea level, both stations report similar relative visits specifically for altitude-related concerns. The altitude-related encounters reported at MCM comprise preventive visits involving premedication for those leaving MCM for SP as well as patients returning from higher elevations receiving follow-up for prior symptoms. All staff assigned to SP receive a briefing on symptoms of altitude sickness and are offered acetazolamide prior to arrival at MCM and before continuing on to SP. Even so, the transition from sea level to altitude is sudden, without an acclimation period, and often of shorter duration than the 24 to 48 hours needed for the preventive benefits of acetazolamide to take effect. 18
The high rate of clinic usage seen at SP may reflect repeat visits by individuals with environmental complaints, such as those susceptible to altitude sickness needing repeat visits for management or proactive closer observation by medical providers. Another potential explanation is that SP offers the most remote environment of the 3 stations, with the greatest degree of physical isolation for its small population during winter months; such repeat visits may represent a need for greater social interaction or again may represent somatization of psychological stress. The significantly lower frequency of dermatological injuries reported at SP is possibly because of comparatively limited environmental exposure, a drier ambient environment, and indoor sequestering of personnel at the remote station. The increased frequency of alcohol-related visits at the SP clinic is likely attributable to the potentiating effects of altitude on alcohol; however, an interpretation with psychological stress as a contributing factor cannot be discounted. Interestingly, normalizing clinic visits by station population revealed a significant increase in the per capita rate of utilization during the winter months at MCM, corresponding to times of greatest isolation and perhaps suggesting that even the larger station population feels the stress of winter isolation. The year-round high utilization seen at SP is likely reflective of several factors: isolation and a harsher environment than the other locales because of altitude effects, plus a lower threshold for medical scrutiny because of the inability to MEDEVAC directly off-continent from the South Pole.
The reasoning behind the decreased usage of the PAL clinic during the 2013−2014 year compared with 2012−2013 is unclear but may be attributable to changes in vessel use of the port, with a decrease in visiting nonstation ship staffers making use of PAL medical services. The beginning of the 2013−2014 Antarctic year coincided with sequestration and the partial US government shutdown, which may have affected shipping traffic and contributed to this decline in clinic utilization.It is worth noting that despite this decline, per capita clinic visits at PAL remained relatively high at a 4:1 ratio for both summer and winter populations through the end of 2014.
Limitations
This study has a number of limitations. First, the separate methods for recording patient encounters in multiple databases unsurprisingly results in discrepancies. The University of Texas Medical Branch obtained the contract for Antarctic medical support in 2012; however, results here were limited to the 2013−2014 year. Unfortunately, recordkeeping was not as precise or redundant in the 2012−2013 period as it was during the following year, limiting the ability to draw further conclusions from comparative analysis of the 2 periods. Additionally, the coarseness of the data did not allow for calculation of on-station prevalence by disease group for either Antarctic year.
Our analysis of Clinic Log data was limited to the diagnostic categories in use by providers, resulting in the grouping of diagnoses with likely disparate causes in an unknown number of cases. This is problematic most clearly in the interpretation of data for altitude-related visits, where encounters for premedication with acetazolamide at MCM are indistinguishable from the frank treatment of AMS at SP, which would both be categorized identically by providers.
The lack of demographic data further limits interpretation of the differences between station clinic utilization patterns reported here, as does the inability to identify the most frequent diagnoses attributed to repeat visits. Finally, Sitreps do not exactly align with the Antarctic year as recorded in the Clinic Logs, resulting in some overlap of clinic encounter recording and further discrepancies between Logs and Sitreps from year to year. Improved tracking logs have been developed and will allow for improved season-to-season and station-to-station comparisons in future studies.
The need for MEDEVACs from all 3 stations demonstrates that medical needs and unanticipated emergent conditions can outstrip clinic resources, even with a prescreened population over limited periods of time. Given the economic cost of unplanned evacuations and the physical risk to emergency responders in an austere environment, further study should be devoted to examining the major causes of MEDEVACs. Even so, these data demonstrate that the overwhelming majority of medical complaints were able to be met by the station clinic resources and staff. Variation in leading diagnoses between stations suggests significant differences in stressors at each station and could warrant further investigation over a longer span of time, in addition to potentially tailored screening criteria to suit each station’s unique environment.
Conclusion
The Antarctic station clinics are active, heavily utilized points of patient contact, administering to a wide variety of pathology and across 3 remote environments. Close quarters, limited social stimulation, and a need for self-sufficiency make Antarctic stations ideal analogs for other extreme environments and remote administration of medical care. Although the majority of identified pathology has been managed successfully on the ice, room for improvement exists, with the potential for tailoring screening criteria to suit the unique environments (both social and geographic) of these different stations. Further advances in screening, improved recognition of pre-emergent conditions, and improved emergency management resources could have significant improvements in healthcare delivery on the ice.
Footnotes
Acknowledgments
Any opinion, finding, and conclusions expressed in this material are that of the authors and do not necessarily reflect the views of the National Science Foundation. The authors acknowledge the contribution of the health care providers at each of the Antarctic station clinics for their dedication to excellent medical care in the most extreme of environments. We also acknowledge the staff of the Center for Polar Medical Operations at the University of Texas Medical Branch in Galveston for their steadfast service in the preventive care and medical screening of those who work at the bottom of the world. The authors would like to thank Dr James Cushman for his extensive review and organization of preliminary Antarctic clinic data prior to this report.
Funding
Finally, we thank the Aerospace Medicine Residency Program at the University of Texas Medical Branch for their support and promotion of medical resident research and fieldwork in extreme environments.
