Abstract
Komodo dragons (Varanus komodoensis) are the world’s largest lizards, known for killing prey that exceed their body mass. Reports of bites to humans in the popular press suggest high degrees of morbidity and mortality. Reports in the medical literature are lacking. We describe the case of a zookeeper who was bitten by a Komodo dragon, with a resultant mallet finger. We further discuss the various potential mechanisms of Komodo dragon lethality, including sepsis and venom deposition theories that are useful in guiding management.
Introduction
Komodo dragons (Varanus komodoensis) are native to five islands of eastern Indonesia and are the world’s largest extant lizards (Figure 1). 1 Reaching up to 3 m in length and weighing as much as 90 kg, Komodo dragons are carnivores and are known to kill prey exceeding their own body mass, including deer, pigs, and water buffalo. 1 However, the manner in which the lizards kill their prey is subject to debate. Komodo dragons have sharp, serrated teeth, but a relatively weak bite, and prey may escape the initial attack of the lizard; but the prey, if bitten and not immediately killed, may go on to have lethargy and shock after the attack.1,2 Consequently, it is thought that death that does not occur as a result of bleeding or trauma from the bite may be due to an exogenous agent introduced into the prey through the bite. Two theories exist: originally, this delayed death was believed to be due to sepsis induced by pathogenic bacteria introduced into the wound from the saliva of the lizard during the bite; more recently, however, there is evidence that the lizard possesses venom that causes bleeding and cardiovascular collapse in the prey.1,2

An adult captive Komodo dragon.
Komodo dragons are popular exhibits in zoos worldwide, including the in United States. Bites to humans are rare, and the medical literature regarding symptoms and treatment after a bite is sparse. We describe a case of a human who was bitten by a Komodo dragon and was treated with antibiotics, and in whom no signs of envenoming occurred; the patient recovered with limited morbidity.
Case Presentation
A 34-year-old, right-hand dominant female zookeeper was bitten by a juvenile Komodo dragon (weight 1 kg) during a routine training exercise when her finger was mistaken for a piece of food. The animal bit and clenched down for about 3 seconds, then was quickly disengaged with the assistance of a coworker. The patient’s medical history included only high cholesterol and polycystic ovarian syndrome. She received an oral dose of amoxicillin/clavulanate (875 mg) and was transported to the emergency room. Her physical examination was notable for several small lacerations to the distal left fifth digit, the largest being 3 cm overlying the distal interphalangeal (DIP) joint on the dorsal surface (Figures 2 and 3). She was unable to fully extend at the DIP joint, but was neurovascularly intact. The plain X-ray film was unremarkable. The wound was irrigated and allowed to heal by secondary intention. She was discharged home on an 11-day course of oral amoxicillin/clavulanate (875 mg twice daily) and a finger splint with the DIP joint in extension.
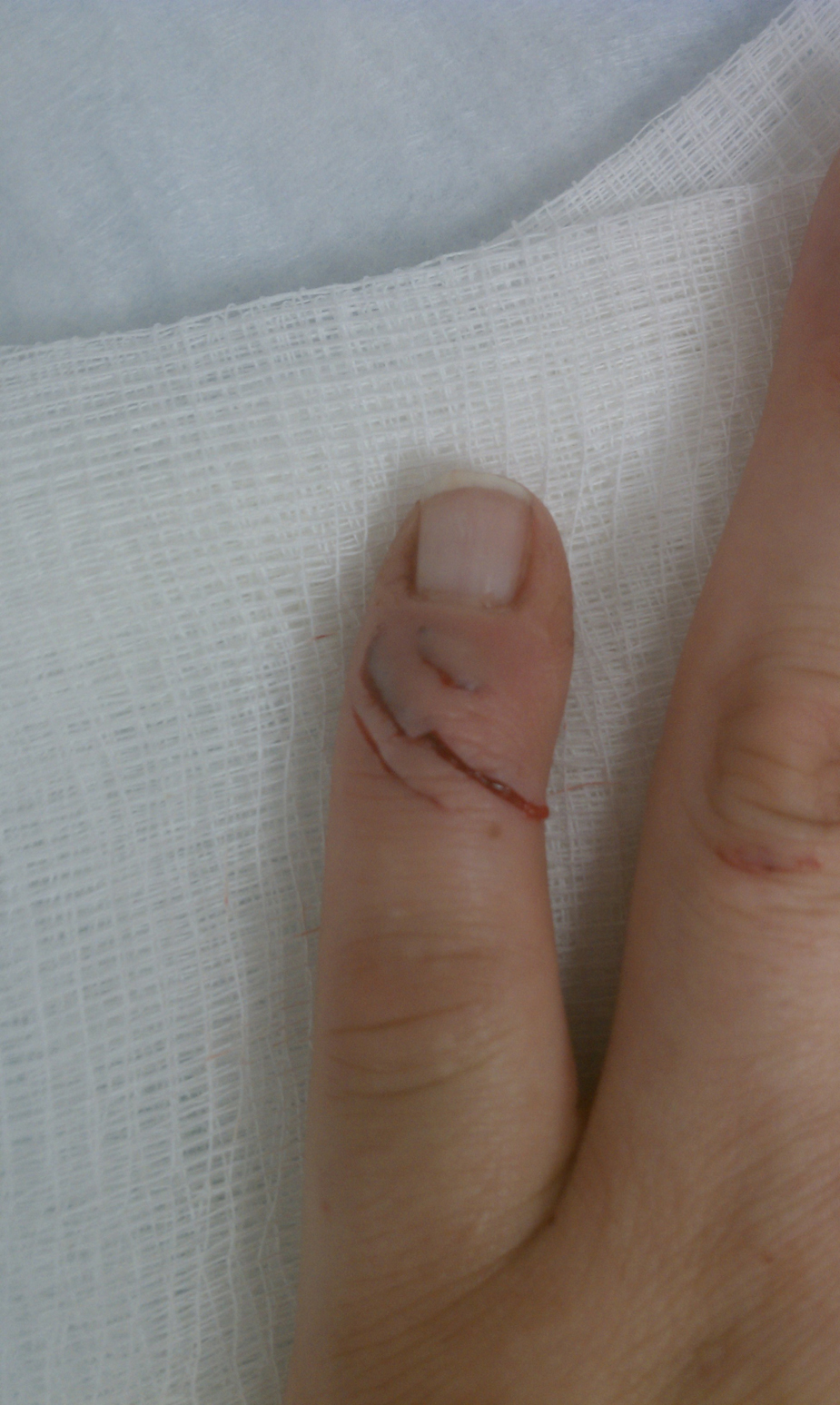
Slashing bite wounds on the extensor surface of the finger.
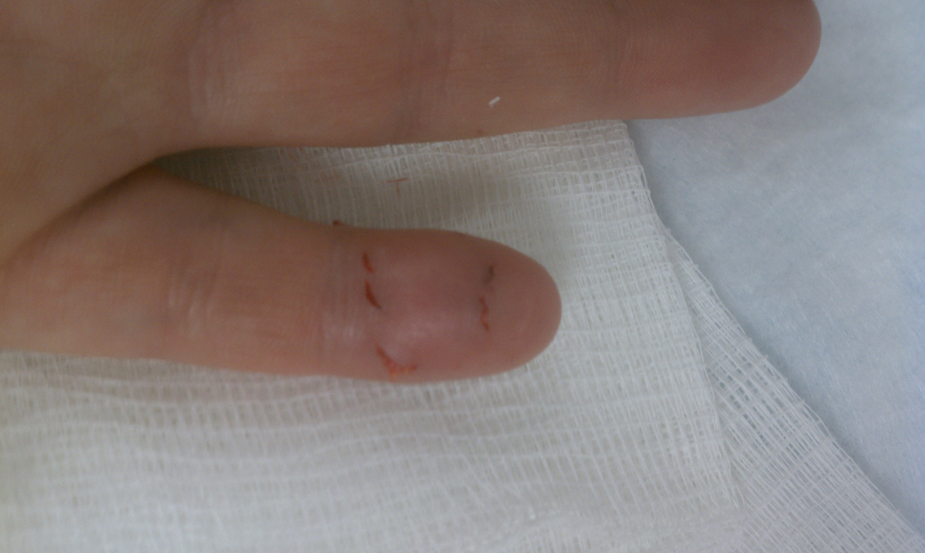
Bite wounds on the palmar surface of the finger.
Several wound checks and follow-up appointments with an orthopedic hand specialist revealed a well-healing wound without signs of infection. The splint was maintained for 5 weeks, after which the orthopedist advised that the patient remove the splint and begin physical therapy. Extensor lag was noted during her therapy sessions, and the orthopedist recommended an additional 4 weeks of splinting. After additional splinting and subsequent physical therapy, the patient did not regain full ability to extend the finger. She recovered with only limited morbidity to the affected hand. The patient’s mallet finger was most likely due to a traumatic tendon injury inflicted by the bite.
Discussion
Medical literature regarding human bites from a Komodo dragon is scarce. A literature search in PubMed revealed no human case reports of Komodo dragon attacks. Populations at risk include those native to the few islands in Indonesia where these lizards reside and zookeepers throughout the world. In the lay literature, there are reports of human attacks resulting in mortality and morbidity, including extensive soft tissue injuries and persistent edematous changes of affected extremities. 3 Although there is no standardized reporting system to quantify the incidence of Komodo dragon bites, attacks appear to be rare, with one lay source reporting 4 deaths over 35 years and 8 injuries within a decade. 3 With curved, serrated teeth, Komodo dragons can inflict large slashing wounds that cause quick, traumatic, hemorrhagic deaths of prey. As much of the prey is larger than the lizard, however, the prey may escape the initial attack with relatively innocuous wounds, but subsequently, lethargy and shock may develop.1,2
It is well established that the mouths of these lizards harbor many bacteria.1,4 One theory of prey demise is based on sepsis. After observing feeding habits of the Komodo dragon, it was thought that prey that did not die quickly from traumatic wounds would die of sepsis due to oral flora introduced into the wound during the bite. 2 A study of wild and captive Komodo dragons showed 57 species of bacteria isolated from their saliva; Escherichia coli, Staphylococcus sp, and Streptococcus sp were the most commonly isolated. 4 In a mouse study, Pasteurella multocida was the only bacteria isolated from dying mice that had been injected with Komodo dragon saliva, and is, therefore, theorized to be one of the primary causes of prey mortality. 4 If a wound is left untreated, it is easy to see how these bacteria could cause local wound infection and potentially sepsis in humans.
More recently, the theory that microbes are the pathogenic agent has been challenged by a venom theory, as venom glands have been isolated from the Komodo dragon. Fry et al 2 described mandibular venom glands and connected ducts that deliver complex venom. The venom delivery mechanism is relatively rudimentary, lacking the hollow fangs characteristic of crotalid snakes or even grooved teeth for funneling venom as seen in the Heloderma lizards, such as the Gila monster (Heloderma suspectum). 2 Analyzed venom reveals a mixture of proteins, some of which are similar to known toxins from other venomous reptiles. These compounds (PLA2 toxins, CRISP, kallikrein, and natriuretic toxins) are expected to cause coagulopathy and hypotension, potentially resulting in death of the prey. 2 The venom is speculated to be deposited by a “grip-and-rip” mechanism: the lizard’s curved, serrated teeth create slashing wounds to allow entry of the venom. 2 Intravenous injection of Komodo dragon venom in rats at 0.1 mg/kg produced hypotension, whereas injection of 0.4 mg/kg intravenously produced hypotensive shock. 2
Venom components appear to have activity similar to that of Heloderma lizards and the venomous monitor lizard, Varanus bengalensis.2,5 Gila monsters are known to have a gripping bite by which they bite and maintain a sustained latch. These heloderms are thought to have evolved their venom for defensive purposes, rather than to aid in digestion or prey immobilization, as is the case with venomous snakes. 6 The effects of Gila monster bites are considered mild compared with envenoming by crotalids, with case reports describing swelling, severe pain, nausea, diaphoresis, emesis, and dizziness. 6 Hypotension and mild coagulopathy appear to be less common, and anaphylactic or anaphylactoid reactions are rarely reported. 6 A report of a monitor lizard bite described local pain with oozing of blood at the bite site, along with dizziness, diaphoresis, nausea, and shortness of breath, which progressed to renal failure and death in 3 days. 5
It is unclear whether the juvenile age of the dragon had an effect on the degree of envenoming in our patient. Some studies of snakes show increased lethality and coagulant activity in the venom of juveniles compared with that of adults,7,8 whereas other studies show no significant differences in enzymatic activity or LD50 between adult and juvenile venom.9,10 There is insufficient evidence on age-related venom changes in Varanus lizards, but that would be an interesting area for further scientific investigation.
Treatment of Komodo dragon bites is primarily supportive. Initial resuscitation includes evaluation of airway, breathing, and circulation, and administration of intravenous crystalloid fluids as needed. There are no first aid measures known to improve outcomes of a venomous reptile bite, and potentially harmful modalities such as venom suction devices, cryotherapy, and electrical therapy should be avoided. Similar to management of crotalid envenoming, nonsteroidal anti-inflammatory drugs would be questionable owing to possible potentiation of the venom’s anticoagulant effects. Opioid analgesics are preferred. Wounds are at a high risk of infection and should be cleansed thoroughly. Based on the bacteria isolated from Komodo dragon saliva, amoxicillin/clavulonic acid is a reasonable choice for antimicrobial therapy for patients who would be candidates for enteral therapy. 11 Doxycycline plus clindamycin could be used for penicillin allergic patients. 11 Radiographs should be obtained to evaluate for fractures or foreign bodies. Tetanus status should be updated as needed. Coagulopathy can be treated with fresh frozen plasma as there is no antivenom available. Similar to prior recommendations for Heloderma and crotalid bites, patients should be monitored for at least 6 hours for the development of systemic symptoms.
Conclusion
This patient sustained a bite from a juvenile Komodo dragon, received immediate care, and did not show evidence of bacterial infection or significant envenomation. Nonetheless, management should include evaluation for venom effects, as well as evaluation of traumatic injuries, proper wound care, and early antibiotic therapy. While healing by secondary intention was successful in this case, adult Komodo dragons often inflict much larger wounds and more extensive trauma.
Footnotes
Acknowledgments
The authors would like to thank Alyssa D. Borek for the use of her photographs and herpetological expertise in preparing this paper.
☆
Presented as an abstract poster at the North American Congress of Clinical Toxicology meeting, October 5, 2012, Las Vegas, NV.
