Abstract
Wild and exotic animal attacks are not common in the United States. Animal-related injuries in the United States are usually caused by dog bites, followed by cattle and horse injuries. Exotic animal attacks can occur when the animals are provoked, depressed, or housed improperly by owners. We report the case of a 51-year-old woman who sustained multiple systemic traumatic injuries after she was pinned to a fence by an elephant’s trunk. Upon arrival in the emergency department, she was hypothermic with a temperature of 35.1°C (95.1°F), hypotensive to 94/60 mm Hg after 5 L crystalloid, tachycardic at 108 beats/min, and intubated with oxygen saturation of 100%. Tranexamic acid was administered in addition to starting a massive transfusion protocol. Injuries included bilateral multiple rib fractures, left abdominal wall degloving injury, right pneumothorax, right hemothorax, left chest wall puncture wound, grade IV splenic laceration, 3 grade III liver lacerations, retroperitoneal hematoma, and degloving injuries to bilateral posterior thighs requiring more than 30 operations. Why should an emergency physician be aware of this? Several factors need to be considered when evaluating animal-related injuries, including type, age, and sex of the animal. Multisystem traumatic injuries should be assumed when a large animal is involved. Prehospital care and transport time are vital to a patient’s survival in both urban and rural settings. During the initial resuscitation, administering antibiotics tailored to the specific animal can greatly decrease risk of infection and morbidity. Additionally, tetanus immunoglobulin, tetanus toxoid, and rabies immunoglobulin and vaccine may be needed, unless the victim has been previously vaccinated.
Introduction
Wild and exotic animal attacks are not common in the United States. 1 Animal-related injuries in the United States are usually caused by dog bites, followed by cattle and horses. 2 Exotic animal attacks could occur when they are provoked, depressed or housed improperly by owners.
Because exotic animal attacks in the United States are not common, they are not well studied. We report a case of multisystem trauma as the result of an elephant attack.
Case Presentation
A 51-year-old woman with an unknown medical history was brought as a transfer to a tertiary care center as a trauma alert after sustaining a crush injury from an elephant trunk while visiting a local animal preservation ranch. According to the Emergency Medical Services report, the patient was standing near a fence when the Asian elephant wrapped its trunk around her and pinned her against the fence. Initial prehospital vitals were not available as the patient was a transfer. The patient was intubated and given 5 L normal saline before arrival. The paramedic placed a 14G angiocatheter in the right chest wall over the second intercostal space and the midclavicular line owing to decreased breath sounds on the right in the setting of hypotension. Transport time was approximately 1 to 2 hours.
The patient’s initial vital signs in the emergency department were as follows: temperature 35.1°C (95.1°F), blood pressure 94/60 mm Hg, heart rate 108 beats/min, and intubated with oxygen saturation of 100%. Primary survey of the patient revealed her to be intubated but moving all extremities. Her head and neck examination found no traumatic injuries, and heart sounds were tachycardic with 2+ radial pulses bilaterally. The lung examination demonstrated decreased but present breath sounds bilaterally. There were multiple abrasions and contusions over the anterior thorax, with a 4-cm puncture wound in the left axillary region extending inferiorly to the left upper quadrant. The abdomen was distended, with a left lower quadrant degloving injury approximately 4 cm by 4 cm with omentum exposure. The cause of the puncture wound was unknown as the elephant ranch declined to comment on the scene, and we were not able to obtain the contact information of the initial prehospital providers. The lower extremity examination revealed degloving injuries to the bilateral posterior thighs. The pelvis was stable, and the spine examination during logroll was without midline spinal stepoffs or deformities.
As the resuscitation continued, bilateral chest tubes were placed with minimal blood and air return. Initial point-of-care laboratory tests were as follows: hemoglobin 7, hematocrit 19, pH 7.19, pC
On the tertiary survey of the patient, the documented injuries sustained and therapies provided included left abdominal wall degloving injury (Figure 1), bilateral multiple rib fractures (Figure 2), right pneumothorax, right hemothorax, left-side chest wall puncture wound, grade IV splenic laceration, 3 grade III liver lacerations, retroperitoneal hematoma, left radius fracture, and degloving injuries to bilateral posterior thighs. Operations performed included exploratory laparotomy; retroperitoneal exploration; splenectomy; hepatorrhaphy; drainage and debridement of abdominal and thigh degloving injuries; angiogram of the celiac, proper hepatic, right hepatic, middle hepatic, and right renal artery without embolization; open reduction and internal fixation of the left fifth to eighth ribs; repair of lung hernia with Strattice mesh (LifeCell, Bridgewater, NJ); skin grafts to bilateral thighs; and multiple debridements. The patient was brought to the operating room 12 times. Numerous specialties, including trauma surgery, interventional radiology, ophthalmology, orthopedics, plastic surgery, psychiatry, and neurology, were involved in the patient’s care. The patient was discharged after 3 months and is currently doing well in a rehabilitation facility.
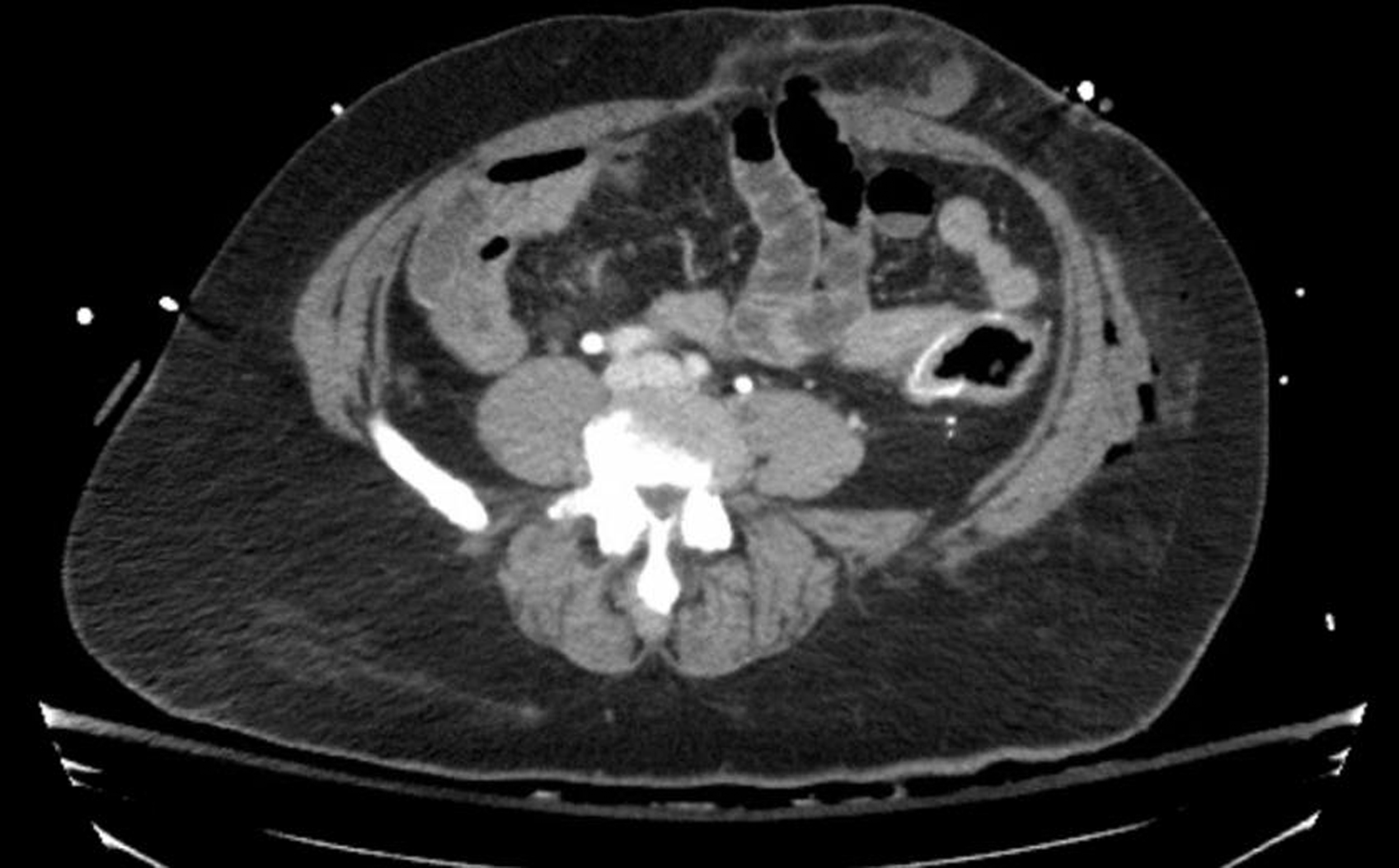
Abdominal computed tomography scan showing abdominal degloving injury with ventral hernia but with no evidence of bowel incarceration.
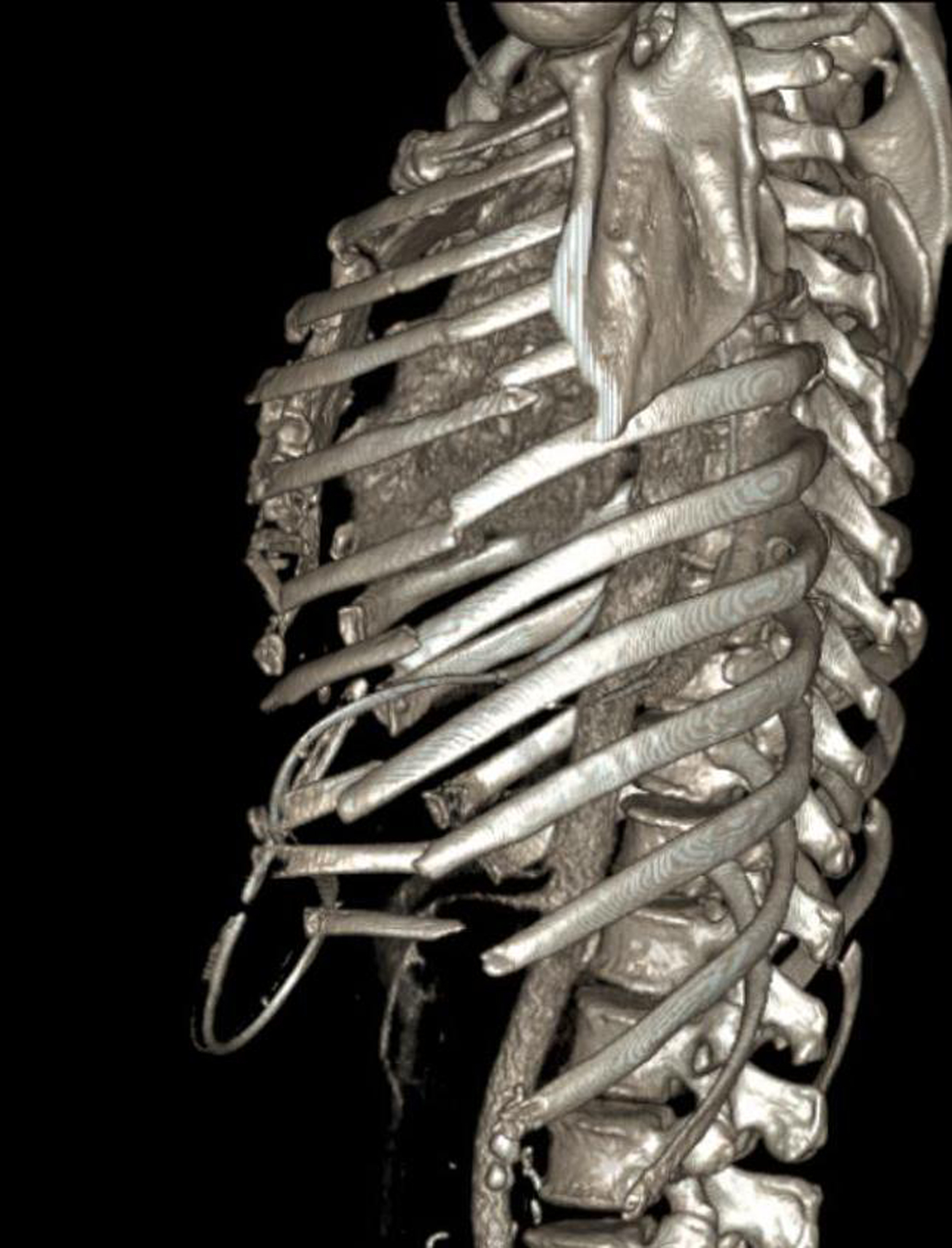
Three-dimensional reconstruction showing multiple bilateral rib fractures.
Discussion
There are many studies on animal bites with specific focus on domestic animals. Most bites are caused by dogs (85%–90%), and the remainder by cats (5%–10%), humans (2%–3%), rodents (2%–3%), and other animals. 2 There have been few studies on animal-related fatalities in the United States. A New Mexico study found 63 deaths caused by animals between 1993 and 2004. 3 The majority of the victims were male (74%) and non-Hispanic white (52%). Of note, 16% of the victims were intoxicated. Horses were the most frequently implicated animal (68%), followed by cattle (14%), dogs (5%), venomous animals (5%), and bear (1 death). 3 Most (67%) occurred in remote places, which delayed treatment.
Langley 4 reported 1943 animal-related fatalities in the United States from 1991 to 2001, which is an average of 177 fatalities per year. Venomous animal encounters were responsible for 39% of fatalities. Many deaths involved transportation incidents, either direct collision with the animal or trying to avoid collision with an animal. The most common transportation-related animal encounter resulting in fatality is with a deer. Although more than 4 million people a year receive dog bites, death rarely results. 18 Another study by Langley and Hunter 5 reports 350 deaths related to animals from 1992 to 1997. Only 5 fatalities were due to an elephant attack.
Exotic animals—such as elephants, rhinoceros, lions, tigers, mountain lions, bears, or buffalo—are responsible for a few deaths each year in the United States. Veterinarians and animal caretakers in zoos and circuses are at most risk for bites, scratches, kicks, crush injuries, goring, trampling, stinging, bucking, throwing, or dragging, and for contracting a zoonotic infection. In the circus, 41 elephant-related incidents have occurred from 1978 to 2004 worldwide. 6 At the time of this report, there were 17 case reports of elephants attacks, with 15 occurring in India, 1 in the Czech Republic, and 1 in Germany. 7 –10 All victims sustained various trampling, goring, tossing, or crushing injuries. The cause of death was usually from trampling of the head and chest. 7
Some potential causes of elephant attacks are disorientation during circus performance or annoyance by the trainer, or being in a state called musth. 7 The elephants are usually between 15 and 20 years of age. Musth occurs during the months of July to September. 5 The case we reported occurred in August. During the time of musth, elephants become aggressive and restless owing to increased testosterone.7,11 The elephants also frighten easily, with unpredictable reactions. 7 During an attack, elephants lower their head and point their tusks at the enemy, or press the victim against an object or against the ground. 8 In the case reported, the victim was pressed against a fence. 7 Younger men have been known to struggle more to escape the trampling attempt and, consequently, sustain even more extensive injuries. 6 Elephants generally kill larger animals with their tusks but lack precision when using them against smaller animals or humans. 6 Asian and African elephants have several differences, such as back shape, tusk length, size. 12 For example, African elephants are usually larger with concave backs and Asian female elephants have short tusks or no tusks. The elephant in this case was an Asian elephant but detailed circumstances and cause of the attack are unknown because the ranch declined to comment.
When evaluating animal-related injuries, several factors need to be considered, including the type, age, and sex of the animal involved. In addition, size of the victim, specific nature and location of wounds, circumstances of the attack, and interval between injury and treatment are also important. 13 Blunt force injuries involve larger animals such as cattle or horses that may kick, crush, or trample a victim, causing head and facial injuries. Vehicle occupants may sustain blunt trauma after collisions with large animals. 13 Multiple body region injuries occur in 32% of cases. 14 Patients with upper extremity injuries must be evaluated for occult head and torso trauma. 14 Zookeepers may be crushed by particularly massive animals, such as elephants. Penetrating injuries usually involve carnivore bites, most often by dogs, with a “hole and tear” pattern. Crush injuries from alligators and sharks are also common. Incised wounds can be complicated by exsanguination and air embolism. Asphyxiation may follow upper airway occlusion or neck and chest compression by animals. 15
Management of these injuries should start at the site of attack, with measures to stop bleeding, fluid and blood transfusion, copious irrigation of wounds, and immediate transport to a trauma center. 16 Our institution used the massive transfusion protocol and administration of tranexamic acid, as the patient was in hemorrhagic shock; she was then transported from the emergency department to the operating room for angiography and packing of abdominal wounds to control the hemorrhage. After initial resuscitation, management consists of standard wound treatment and copious irrigation with debridement. 7
Administration of antibiotics should be routine. The choice of antibiotics should target against animal and human skin flora, claw, tusk, and mouth flora depending on the animal involved. Common bacteria include Streptococcus sp, Staphylococcus aureus, and Pasteurella multocida. Cefazolin and cephalexin are both effective against S aureus and Streptococcus sp and are adequate for P multocida. The standard initial treatment for a uninfected wound is usually amoxicillin-clavulanate (Augmentin), 875 mg plus 125 mg, twice a day for 5 days. 17 Alligator and crocodile bites are usually contaminated with Aeromonas hydrophilia and anaerobic bacteria. Clindamycin or trimethoprim-sulfamethoxazole should be considered. 11 Soil bacteria may also contaminate penetrating injuries. It is prudent to add valacyclovir for monkey bites to cover Herpes simiae. Marine animal injuries should be covered with doxycycline. 17 In our institution, we chose cefazolin and clindamycin for empiric coverage. Tetanus vaccine should be administered to patients if their last tetanus immunization was more than 5 years earlier. Tetanus immunoglobulin should be administered to patients with contaminated wounds and unknown tetanus immunization status. Rabies immunoglobulin and vaccine should be considered, if applicable.
After stabilization of the patient, transfer should be arranged to a tertiary care center if the facility cannot handle a trauma of this magnitude. The patient in our care required more than 30 operations and 7 specialists for her care. She also required extensive physical therapy and psychiatric evaluation for anxiety, depression, and posttraumatic stress syndrome.
Why should an emergency physician be aware of this? Exotic and wild animal attack cases are not common in the emergency department. Prehospital care and transport time are key factors in improving the survival of patients who have sustained injuries from an animal attack. Training sessions should be held for these prehospital care providers and for law enforcement, as they are often not familiar with managing injuries related to wild animal attacks and may also be injured attempting to care for the patient. It is also important to suspect multisystem injuries in victims of large-animal encounters. Management should be tailored to the type of animal involved, the specific nature and location of wounds, the circumstances of the attack, and the interval between the sustained injury and its treatment. Finally, antibiotics, rabies vaccine if applicable, and tetanus administration during initial resuscitation can decrease the risk of infection and its resultant morbidity and mortality.
