Abstract
A retrospective light-microscopic study was performed on skin-biopsy specimens from 145 cats with eosinophilic inflammatory dermatoses in order to determine the prevalence of apoptotic epidermal keratinocytes (AKs), the prevalence of eosinophils in close proximity to AKs, and whether there was a difference in the prevalence of AKs or the prevalence of eosinophils in close proximity to AKs based on histopathological reaction pattern. Overall, 62/145 (43%) specimens had AKs. Of the cases in which AKs were seen, 18% had eosinophils in close proximity to the AKs. The specimens were divided into three groups based on histopathological reaction pattern: perivascular-to-interstitial, diffuse, and nodular. No difference in the prevalence of AKs was found among the three histological groups. Because the sample size containing eosinophils in close proximity to AKs was too small to compare the three histological patterns individually, nodular and non-nodular patterns were compared. No difference in the presence of eosinophils in close proximity to AKs was found in these two subsets. More AKs were present if eosinophils were in close proximity to the AKs (range 1–9 with eosinophils near compared to 0–7 without).
Apoptosis is cell death that occurs in a programmed fashion in physiological and pathological processes. 1 Apoptosis is an active process that requires energy and protein synthesis and is comprised of two distinct phases: nuclear condensation and phagocytosis and clearance of fragments by adjacent cells. 2 Apoptosis is under genetic control and occurs via an extrinsic or death receptor pathway and an intrinsic or mitochondrial pathway. 1,2 It can be initiated by several extracellular factors such as hormones, cytokines, chemical, physical and infectious agents, or cytotoxic T lymphocytes. 3 Apoptosis differs from oncosis (oncotic necrosis), or accidental cell death that occurs after cellular injury, and does not result in the release of inflammatory mediators into the surrounding tissues. 1–3 Apoptosis can be recognized by light-microscopy and is characterized by cell shrinkage, margination of nuclear chromatin, and nuclear pyknosis and karyorrhexis. 1,4 Terminal urindinyl transferase nick and labeling (TUNEL) and immunohistochemistry can be used to validate morphological criteria by detecting DNA fragmentation, 2,3 but the specificity of these methodologies has been questioned. 5,6
Anecdotal information indicates that: (i) apoptotic epidermal keratinocytes (AKs) are rarely seen (one or two in a section through a 6-mm skin-biopsy specimen) in normal epidermis, and (ii) AKs may be seen in small numbers in virtually any hyperplastic epidermis. 4 However, more recent studies indicate that AKs are rarely seen in 6 mm skin-biopsy specimens of normal skin from horses (a single AK seen in 2/45 (4%) horses) and cats (a single AK seen in 1/33 (3%) cats). 7–9 In addition, there was no correlation between the number of AKs and the extent of epidermal hyperplasia. 7
Apoptotic epidermal keratinocytes are a key histopathological feature in certain immune-mediated dermatoses, solar-induced dermatitis, and certain viral dermatopathies in dogs, horses, cats, and humans, though they are occasionally found in smaller numbers in other inflammatory dermatoses. 3,4,7,9–13 A recent light-microscopic study looking at the frequency of AKs in various inflammatory dermatoses of the cat reported that – in dermatoses not expected to have high numbers of AKs – ectoparasitic diseases had a higher number of AKs than other inflammatory dermatoses. 9 When examining these cases further, eosinophils were occasionally seen directly adjacent to AKs in flea-bite hypersensitivity, cheyletiellosis, and mosquito-bite hypersensitivity.
Apoptotic epidermal keratinocytes are most commonly reported in association with dermatoses characterized by an interface histopathological pattern. 4,7,9–13 These dermatoses are typically characterized by an exocytosis of lymphocytes, some of which may be seen adjacent to AKs (so-called ‘satellite cell apoptosis’). 4,7,11–13 It has also been reported that neutrophils can be found adjacent to AKs in cases of pemphigus foliaceus and toxic shock-like syndrome in dogs. 3,13,14 Whether or not these activated neutrophils release granule contents and cytotoxic substances that trigger apoptosis is unknown. 3 To our knowledge, the prevalence of eosinophils in close proximity to AKs in eosinophilic dermatoses of any species has not been previously reported. The role of eosinophils in causing apoptosis of epidermal keratinocytes has been called into question by findings of Vogel et al. 9 Because apoptotic cells do not release their cellular components into the surrounding interstitial tissue and are quickly phagocytosed, virtually no inflammatory reaction is incited, making it unlikely that the apoptotic epidermal cells are inducing eosinophil migration. 1,15
Our purposes were to determine: (i) the prevalence of AKs in eosinophilic inflammatory dermatoses of the cat; (ii) the prevalence of eosinophils in close proximity to AKs; and (iii) the association – if any – between the prevalence of AKs and eosinophils in proximity to AKs based on histopathological reaction pattern.
Materials and Methods
A retrospective light-microscopic study of skin-biopsy specimens from 145 cats with eosinophilic inflammatory dermatoses was performed. All biopsy specimens had been submitted to the Pathology Service at the Cornell University College of Veterinary Medicine, processed routinely for histopathological evaluation, and stained with hematoxylin and eosin (H&E). All diagnoses had been established previously via standard clinical, laboratory, and histopathological criteria (Table 1). 4 One author (JSG), who was blinded to the diagnoses, examined all specimens for AKs, and the presence of eosinophils or lymphocytes in close proximity to the AKs.
Prevalence of AKs in eosinophilic inflammatory dermatoses in 145 cats.

One 6 mm section was examined at 400× magnification from each of the 145 specimens. In order to duplicate routine procedures in diagnostic dermatopathology, only one section of tissue from each specimen was examined. If multiple specimens were present on a slide, the section fulfilling the inclusion criteria and containing the least amount of artifact was chosen for evaluation. Specimens were excluded if no epidermis was present, if the epidermis was <6 mm in length, or if eosinophilic dermatitis was not present. Eosinophilic dermatitis was defined as an inflammatory reaction wherein eosinophils were prominent in the cellular infiltrate. Each specimen was examined for the presence, number, and location of AKs within the epidermis. An AK was defined as a keratinocyte with the following characteristics: cell shrinkage, dense eosinophilic cytoplasm, nuclear pyknosis and/or karyorrhexis, and margination of nuclear chromatin (Fig 1). 1,3,4,7 Specimens which contained AKs were then examined for any eosinophils in close proximity to the AK. Close proximity was defined as eosinophils directly adherent to or within 100 μm of the AK. Lymphocytic exocytosis within that field at 400× magnification was also noted.

Skin-biopsy specimen from a cat with flea-bite hypersensitivity. Note the apoptotic epidermal keratinocyte (black arrow) (H&E stain; 400× original).
Statistical analysis
All statistical methods were performed using Statistix 9.0. 16 The prevalence of AKs in eosinophilic dermatoses of the cat and its 95% Wilson score continuity-corrected confidence interval (CI) was calculated. From the cases which had AKs present, the prevalence of eosinophils in close proximity to those AKs was calculated along with the 95% CI. The prevalence of lymphocytes (seen in only 4/145 specimens) in close proximity to the AKs was so low that this was seen as insignificant and excluded from further analysis.
The specimens were separated into three groups based on their histological reaction pattern – perivascular-to-interstitial, diffuse, and nodular – in order to determine whether the presence of AKs or eosinophils in close proximity to AKs was associated with histological pattern. The association between AKs and the three histological patterns was determined based on χ2 test. When analyzing the data containing eosinophils in close proximity to AKs, the sample size was too small to fulfill the assumptions of the χ2 test. The data were dichotomized by comparing the nodular pattern to the other two patterns and tested by Fisher's exact test. Whether or not the presence of eosinophils in close proximity to AKs was associated with the nodular or non-nodular pattern also was tested using the one-sided Fisher's exact test.
The Wilcoxon rank-sum test was used to determine whether the number of AKs was associated with the presence of eosinophils in close proximity. Alpha equals 5% was used for our tests.
Results
One or more AKs were present in 43% (62/145; 95% CI=35%, 51%) of cats with eosinophilic dermatoses (Fig 1) (Table 1). Of the 62 cases that had AKs present, 18% (11/62; 95% CI=10%, 30%) had eosinophils in close proximity (Fig 2) (Table 1). We found no association between the prevalence of AKs and the three histological patterns (χ2=1.74, df=2, P=0.42). Eosinophils being in close proximity to AKs was, likewise, not associated with the nodular or non-nodular histologic patterns (P=0.21, two-sided). A higher number of AKs was associated with having eosinophils in close proximity (the minimum, median (P=0.03, one-sided), and maximum AKs were 1, 2, 9 if eosinophils were in close proximity, and 0, 0, 7 otherwise).
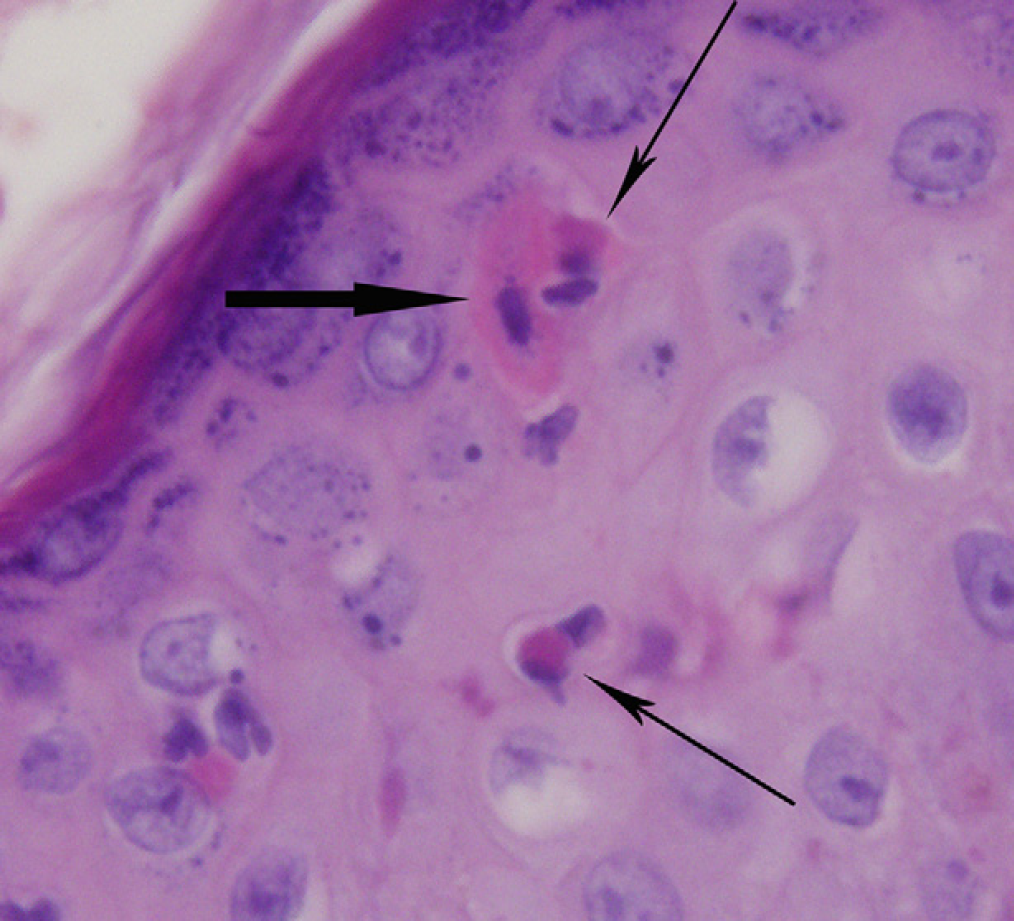
Skin-biopsy specimen from a cat with flea-bite hypersensitivity. Note the apoptotic epidermal keratinocyte (thick black arrow) with infiltrating and adjacent eosinophils (thin black arrows) (H&E stain; 1000× original).
Discussion
Apoptotic epidermal keratinocytes were found in 43% of the skin-biopsy specimens from cats with eosinophilic dermatoses. Of these cases, 18% had eosinophils in close proximity to the AKs. Vogel et al 9 reported this occurrence, but did not determine the prevalence. The significance of this finding is still unclear but might point toward an eosinophil-initiated apoptosis. Histological pattern was not related to the prevalence of either AKs or eosinophils in close proximity to AKs. We also found the number of AKs was slightly higher when eosinophils were in close proximity. This may also add support for the role of eosinophils in inducing apoptosis.
As eosinophils were only seen in proximity to AKs in 18% of our cases, the question arises as to what might be inducing apoptosis in the remainder of the cases examined. No other inflammatory cell type was seen. Neither had the cats had known exposure to any drugs, chemicals, toxins, or infectious agents known to be associated with apoptosis. 1,3,4,10,11 One possible explanation would be artifact of section, wherein serial sections might have demonstrated more eosinophils in proximity to AKs. One of us (DWS) has long noted the same situation in the classical interface dermatoses with lymphocyte-associated apoptosis: many AKs do not have adherent or nearby lymphocytes.
Satellitosis by cytotoxic T-cells is an established trigger for apoptosis; however, other leukocytic infiltrates may play an important role in epidermal apoptosis. 1,6 Cytotoxic substances from neutrophils may induce apoptosis as they have been seen adjacent to AKs in cases of pemphigus in domestic species 3 and toxic shock-like syndrome in dogs. 13,14 Macrophages, after phagocytosis of apoptotic bodies, may also secrete inflammatory mediators under certain circumstances determined by the state of the dying cell, the phagocytic receptors engaged, or downstream signaling pathways that are activated. 17 Eosinophils, specifically, have not been described to incite epidermal keratinocyte apoptosis, but their prevalence in close proximity to AKs in feline eosinophilic dermatoses suggests a possible relationship.
In human literature, the role of eosinophils as perpetrator and victim has been established as they can cause apoptosis as well as become apoptotic and phagocytosed in order to prevent inflammation. Trautmann et al 18 demonstrated that T-cells and eosinophils induce bronchial epithelial cell apoptosis in human patients suffering from asthma. This was shown to occur via secretion of interferon-γ and tumor necrosis factor-α and by triggering death receptors on bronchial epithelial cells. This mechanism is different from the Fas-ligand-mediated apoptotic pathway that occurs in epidermal keratinocytes. These eosinophils also do not release the same cytotoxic proteins as released by neutrophils to cause apoptosis. 18 Interestingly, the actual apoptosis of eosinophils and clearance by macrophages or bronchial epithelial cells is a primary mechanism for the removal of eosinophils from the lungs in asthma and other airway diseases. 19 However, when significant granulocyte apoptosis occurs, necrosis, and inflammation can progress due to insufficient phagocytosis. 19 Egression (the movement of these granulocytes into the airway lumen) may allow for effective removal of these inflammatory cells. One can speculate that if the processes of egression or phagocytosis are incomplete, inflammatory mediators released from the necrosis of apoptotic eosinophils could then lead to further apoptosis of bronchial cells. Whether or not such eosinophil-associated apoptosis occurs in skin keratinocytes is presently unknown.
The TUNEL reaction can be used to detect apoptotic nuclei in tissues; however, this was not performed in our study because we were interested in duplicating the procedures of routine diagnostic histopathology. In addition, the TUNEL reaction is not specific. 5,6,17 Only one H&E section of each specimen was examined which could have lead to AKs being missed. Again, serial histological sections were not performed.
In conclusion, AKs are present in more than two-fifths of skin-biopsy specimens from cats with eosinophilic inflammatory dermatoses. Nearly one-fifth of these cases show eosinophils in close proximity to the AKs. Our study also revealed that a higher number of AKs was associated with having eosinophils in close proximity. Apoptosis of epithelial cells can be induced by inflammatory mediators released from eosinophils in human asthma; however, the mechanism of apoptosis appears to be different than that seen in epidermal keratinocytes. Our study indicates that eosinophils may be involved in triggering apoptosis in epidermal keratinocytes. Further studies are needed to confirm these findings and to elucidate the inflammatory mediators involved in this apoptosis.
