Abstract
This report describes the first case of idiopathic hypertrophic osteopathy (HO) in a cat. No causes for the bone pathology were found following evaluation of the physical and laboratory examinations (complete blood count, albumin, creatinine, urea, alkaline phosphatase, alanine aminotransferase, aspartate aminotransferase and γ-glutamyltransferase and urinalysis), and after histopathological evaluation of organs at necropsy. Based on the radiographic, clinical and anatomopathological findings, idiopathic HO was diagnosed.
Hypertrophic osteopathy (HO) or Marie's disease is a syndrome characterised by the formation of subperiosteal new bone (Doige and Weisbrode 1995) especially on the appendicular skeleton (Hime et al 1972). This syndrome is frequently described in dogs, horses, cattle, wild animals and human beings (Brodey 1971, Masegi et al 1994). In these species, HO is generally secondary to chronic pulmonary infiltrative lesions, metastatic or primary neoplasms in the lungs being named HO of pulmonary origin (Hancey and Pass 1972, Doige and Weisbrode 1995, Santos et al 1998). Additionally, there are reports of HO related to sarcoma of urinary bladder, to valvular endocarditis and Spirocerca lupi or Dirofilaria immitis (Brodey 1971) infection in dogs. In humans, this osteopathy is usually secondary to bronchogenic carcinoma. In addition, in humans and horses it is rarely found associated to other pathologies being considered primary or idiopathic (Bhate et al 1978, Mair et al 1996). HO in cats is rare and there are few reports in the literature; three reports refer to pulmonary HO (Gram et al 1990, Grierson et al 2003, Rohr 2003). In a further report, the bone pathology was associated to a malignant tumour of the adrenal gland (Becker et al 1999). To the authors' knowledge, this is the first report of idiopathic HO in a cat.
A young 2.5 kg male mixed breed cat estimated to be less than 6 months of age was found abandoned and presented in lateral recumbency to the Veterinary Teaching Hospital. Physical examination revealed severe difficulty in ambulation with muscle stiffness in all limbs. The appetite was good; defecation and urination were observed to be normal. Palpation revealed extensive hard thickening and pain along all the appendicular skeletal. It was not possible to flex any of the four limbs. Thoracic auscultation was normal. Complete blood count (CBC) and routine serum biochemistry tests (albumin, creatinine, urea, alkaline phosphatase, alanine aminotransferase, aspartate aminotransferase and γ-glutamyltransferase and urinalysis) revealed increased urea 54 mg/dl (reference range 10–30 mg/dl) as the only abnormality. Serum creatinine was 0.6 mg/dl (reference range <1.6 mg/dl) and urinalysis was normal. The urinary specific gravity was low: 1.010 (reference range 1001–1080). In the urinary biochemistry examination the glucose, ketones, and haemoglobin were negative. Urinary sediment examination was unremarkable. Radiographic examination of the appendicular skeleton showed extensive subperiosteal new bone suggestive of HO. The cat was euthanased due to the advanced stage of disease.
The post-mortem examination showed all four limbs to be very thick and hard. The surface was irregular with new bone formation characteristics (Fig 1). At transverse section of long bones, diaphyses appeared to have a double cortical formation. It did not involve the articular surfaces. Severe weight loss was also noted.
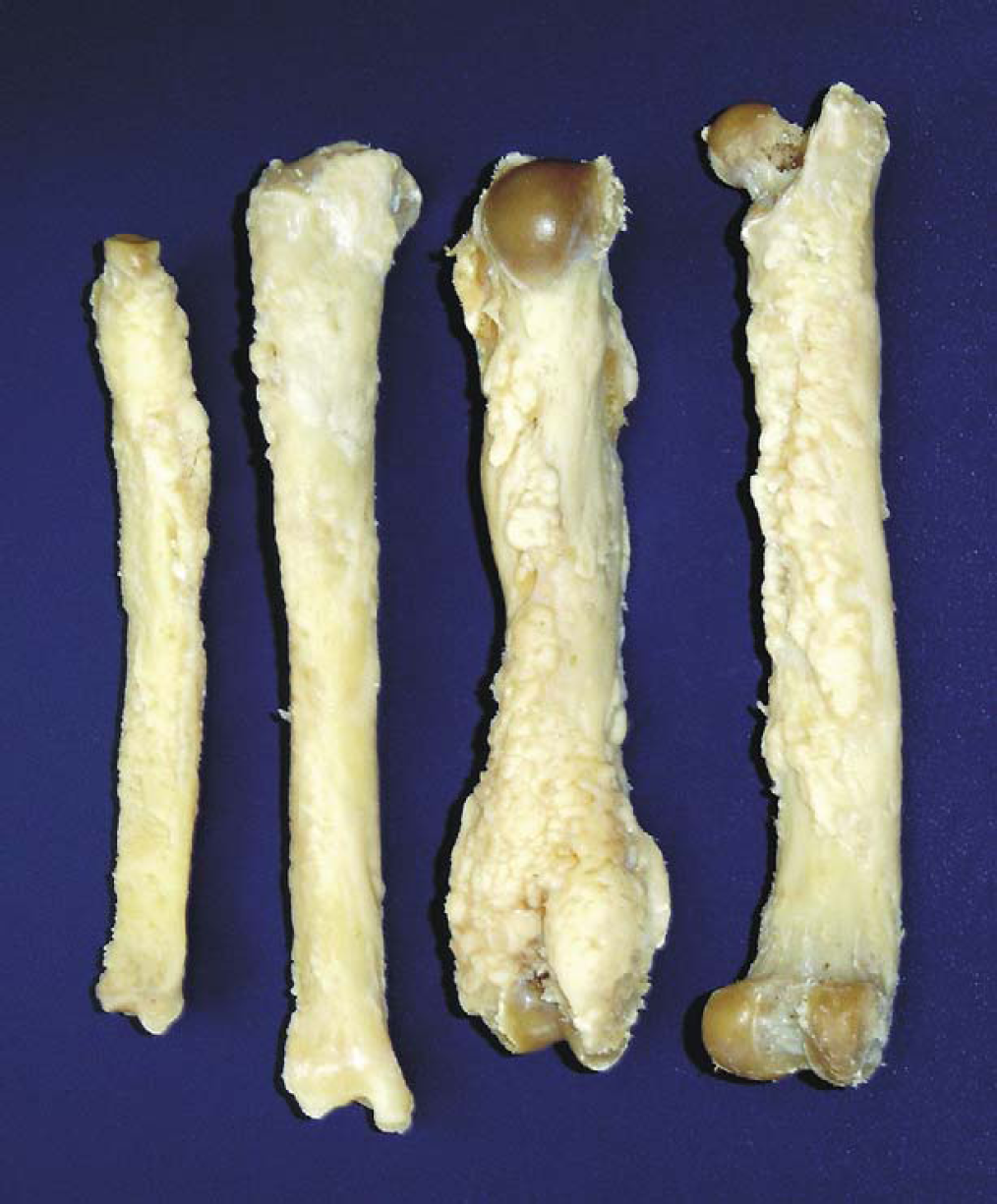
Long bones; cat. Hypertrophic osteopathy. All of the four limbs very thick and hard. The surface is irregular with new bone formation characteristics.
After necropsy, the thoracic limbs and left pelvic bones were macerated and revealed periosteal bone proliferation and double cortex. Lateral radiographs were taken of all the long bones. Radiographic changes included intense and symmetric formation of new subperiosteal bone through all diaphysis and metaphysis of affected bones (Fig 2). In the transverse view of long bones an irregular and increased radiodensity extended from the cortex.

Long bones; cat. Hypertrophic osteopathy. Intense and symmetric formation of new subperiosteal bone through all diaphyses and metaphyses of affected bones.
Bone, liver, kidneys, brain, bladder, heart, lungs, lymph nodes, and spleen were collected for histological evaluation. The bones were decalcified and all the fragments, including the soft tissues, were fixed in 10% neutral buffered formalin, routinely processed and embedded in paraffin. Sections were cut 5 μm thick and stained with haematoxylin and eosin.
Histopathological examination revealed periosteal thickening associated with intense cellularity composed of a large number of osteoblasts. There was new periosteal bone formation (double cortex composed of immature trabecular bone tissue). Bone marrow and highly vascular connective tissue were observed inside this immature bone (Fig 3A). A large number of pyknotic osteocytes (Fig 3B) and osteoclasts were observed in the Howship's lacunae in the mature bone tissue.

Hypertrophic osteopathy; cat. (A) Immature bone tissue with marrow bone and connective tissue adhered to the cortical (haematoxylin and eosin, magnification ×3.90) and (B) a great number of pyknotic osteocytes (haematoxylin and eosin, magnification ×31.2).
The remaining cortex showed an increase in the number of Havers canals (increased porosity). The epiphysis and metaphysis had thin trabecular bone. It is probable that these changes are not related to the periosteal new bone but are secondary to cachexia and decreased mechanical use. The other organs did not contain histopathological lesions.
Clinical signs of lameness and the increase in volume of the limbs and joints were caused by an intense periosteal reaction. An intense proliferation of vascularised connective tissue in the periosteum adjacent to the articular surfaces resulted in joint thickening. The increased urea nitrogen concentration was likely caused by muscular catabolism, however, a renal component could not be ruled out because of the low urine specific gravity.
Several hypotheses have been used to explain the pathogenesis of secondary HO. An important factor that contributes to the development of bone lesions is an increase of blood flow to the limbs. Humoral and neuronal theories have been postulated to explain this increase in blood flow. The humoral theory is based on the relationship between HO and thoracic lesions. These thoracic lesions are thought to cause hypoxia and the formation of arteriovenous shunts in the pulmonary circulation (Ndikuwere and Hill 1989), permitting access of vasoactive substances into the arterial circulation, which then promote an increase in the blood flow to the limbs. Experimentally, shunt induction, however, has not induced bone changes comparable to HO. According to the neuronal theory, nervous stimuli produced by the vagus nerve are responsible for an increase of peripheral blood flow with less tissue oxygen stimulating periosteal proliferation (Jubb et al 1985, Ndikuwere and Hill 1989, Doige and Weisbrode 1995). Despite these theories the pathogenesis of HO is obscure in all species. According to Santos et al (1998), another explanation for HO secondary to pulmonary tumours is the production of growth factors produced by the neoplasm that act on the bone promoting an increase in blood flow and as a consequence promote periosteal reaction. In the present report, the HO was not related to any other identifiable pathology so its pathogenesis cannot be explained by any of these hypotheses. It is unknown which single mechanism or combination of mechanisms is responsible for the skeletal changes in this syndrome.
