Abstract
Objective/Background
To review the effect of mechanical stretch on hypertrophic scars after burn injuries.
Methods
A systematic review of all controlled trials related to the effect of mechanical stretch on post burn hypertrophic scars was conducted. Studies of conservative scar managements that applied mechanical forces parallel to the scar surface, including stretching exercise, massage, and splinting, were appraised. Eligible studies published in English between 1995 and 2016 were extracted from The Cochrane Library, MEDLINE, CINAHL, Science direct, SPORTDiscus, and Physiotherapy Evidence Database Scale (PEDro). The journals were further screened with inclusion and exclusion criteria. PEDro was selected for further analysis and appraisal.
Results
There were 853 articles identified. After a standardized screening mechanism stipulated, only nine full-text articles were selected for critical appraisal using PEDro. There were five articles of high quality, two of fair quality, and two of poor quality. Detailed training regime and outcomes of nine studies were summarised, including two studies with stretching exercise, six studies with massage, and one study with splinting. The physical parameters of scar assessments and the range of motion on affected areas were compared.
Conclusion
From extensive literature search, there was no strong evidence indicating the positive effect of mechanical stretch using stretching exercise, massage, or splinting on hypertrophic scars. A firm conclusion cannot be drawn for the discrepancy of outcome measures and varied effectiveness. Most of the included studies lacked objective evaluation or control group for comparison. Further high quality studies with larger sample size and using standardized measurements are needed.
Introduction
Hypertrophic scars are severe complications after burn injuries. The concomitant scar contractures will develop and expand to underlying connective tissue and muscles, resulting in limitation in joint range of motion (ROM) and participation of daily activities (
Conservative treatments were preferred in clinical settings to restrain the progression of scar and contracture for their noninvasive and easy-operation properties (
Although many guidelines stressed the importance of implementing mechanical stretch to improve scar texture, prevent or correct scar contracture, and increase ROM, consensus has seldom been reached regarding the detailed protocol and the magnitude of the stretching force. Therefore, this systematic review was conducted to evaluate the quality of published studies and summarise the effectiveness and regime for building up the practical guidelines.
Methods
Search strategy
Articles published from 1995 to 2016 were searched from the electronic database: Cochrane Central Register of Controlled Trials CENTRAL (The Cochrane Library), MEDLINE (1965 to most recent date available), CINAHL (1982 to most recent date available), Science direct, SPORTDiscus (1830+) and the Physiotherapy Evidence Database (PEDro). “Mechanical stretch” after burn injuries was defined as conservative scar managements that applied tensile force parallel to the scar, and stretching exercise, massage, and splinting were included in the analysis. Search syntax following professional standards were developed as: #1: MeSH descriptor: [Burns] explode all trees; #2: burn* or scald* or thermal injur*:ti, ab, kw; #3: MeSH descriptor: [Cicatrix, Hypertrophic] explode all trees; #4: scar* or cicatrix: ti, ab, kw; #5: #1 or #2 or #3 or #4; #6: MeSH descriptor: [splints] explode all trees; #7: MeSH descriptor: [massage] explode all trees; #8: stretch* or splint* or massage*: ti, ab, kw; #9: #6 or #7 or #8; #10: #5 and #9.
To avoid publication bias, additional studies were detected through online clinical trials registered websites (
Screening criteria
Studies were included according to the following criteria: 1) prospective controlled trials with full text available in English, including randomized controlled trial (RCT), non-RCT controlled clinical trials (CCT); 2) outcome measures were physical parameters related to scar and scar contracture; 3) interventions were stretching-, splinting-, and massage related. Subjects after burn injuries were not specified in terms of age, race, severity of injury, and stage of scars. Review articles and studies on the aetiology, laboratory tests, and assessments of scars were excluded. Two review authors independently assessed the title and abstract of articles and selected eligible trials. Then, the full texts were reviewed by the same reviewers to include studies using the prestipulated criteria. The disagreement was resolved by consultation with a third reviewer. The process was summarised through Preferred Reporting Items for Systematic Reviews (PRISMA).
Data extraction and quality assessment
The data was extracted independently by reviewers using a standard form, which contained characteristics of subjects, area and depth of injuries, mode and regime of therapies, and outcomes of scar and contracture from all groups. Study design and analytical methods were also recorded for quality appraisal using the Oxford Centre for Evidence-Based Medicine level of evidence (
Results
There were 853 articles identified from the electronic database followed by strategies and criteria stipulated in the method. After detailed screening of titles, abstracts, and contents, 12 full-text articles matched our selection criteria. Finally, nine studies with full text available were included in the quality assessment. The detailed PRISMA flow chart of the search process was summarised in the diagram (
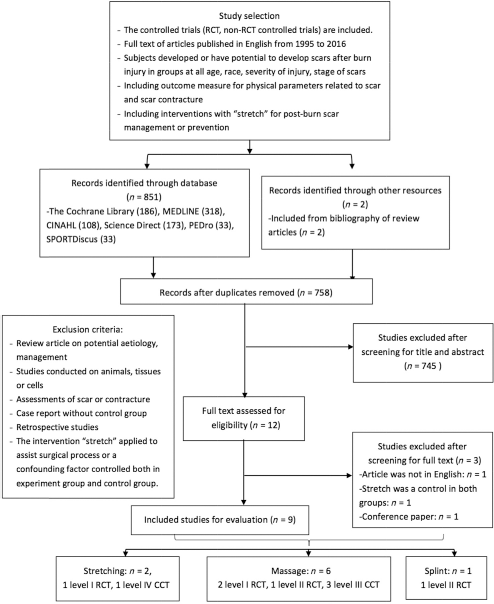
PRISMA flow chart of recruiting eligible studies.
Classification of selected studies
Among the nine evaluated studies, three were three level I RCTs (
PEDro Scoring.
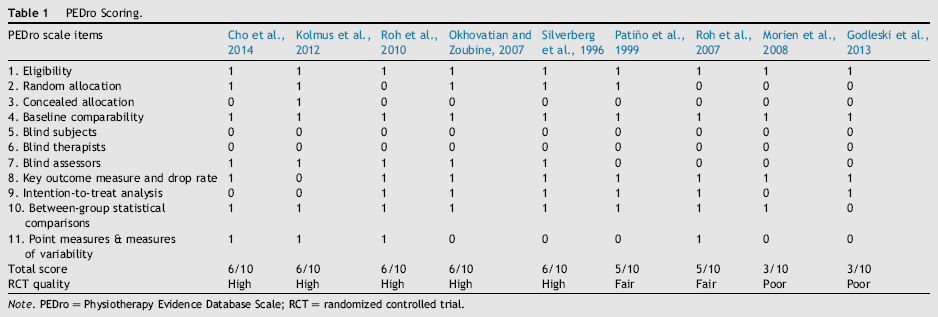
Note. PEDro = Physiotherapy Evidence Database Scale; RCT = randomized controlled trial.
Characteristics of subjects
The selected trials embodied 375 subjects in total, with sample size ranging from 8 to 160 and age ranging from 4 to 64 years old. Four trials specified the location of scars (
Summary of Recruited Subjects and Outcome Measures.
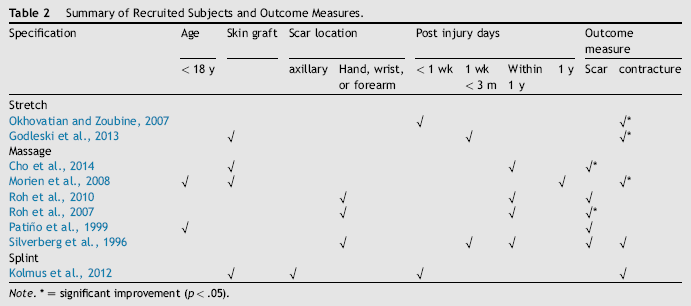
Note.
= significant improvement (p < .05).
Outcomes of Intervention
The duration of intervention ranged from 3 days to 6 months. For the post injury days for initiation treatments (within 48 hours–16 years after the injury), two trials specified the time within 1 week (
Regarding outcome measures, four studies assessed the subjective scar parameters using Vancouver Scar Scale (VSS), modified VSS or Patient and Observer Scar Assessment Scale (POSAS) (
Intervention strategy
Stretching (Table 3)
Stretching, Massage, Splinting Protocols, and Outcomes.
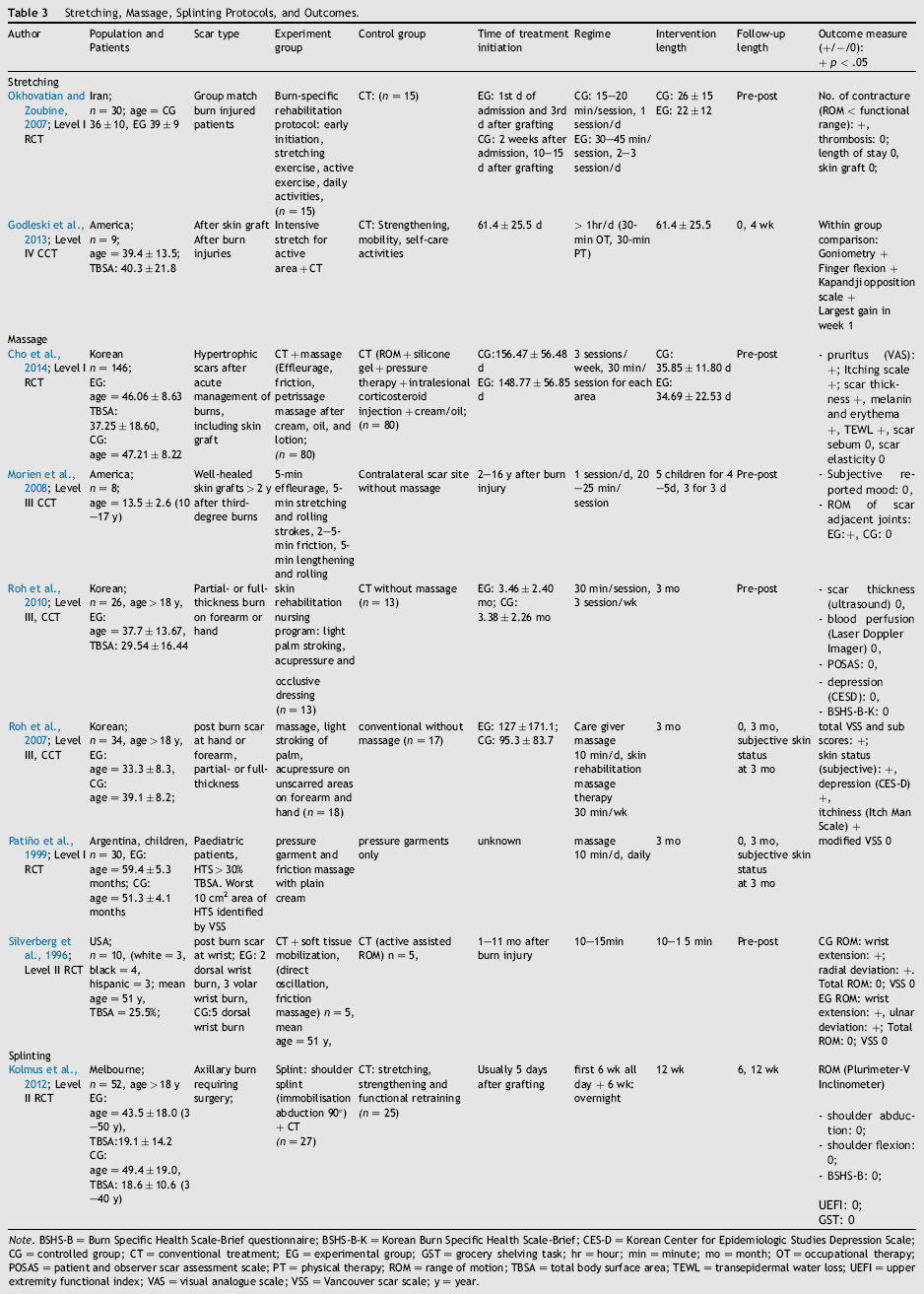
Note. BSHS-B = Burn Specific Health Scale-Brief questionnaire; BSHS-B-K = Korean Burn Specific Health Scale-Brief; CES-D = Korean Center for Epidemiologic Studies Depression Scale; CG = controlled group; CT = conventional treatment; EG = experimental group; GST = grocery shelving task; hr = hour; min = minute; mo = month; OT = occupational therapy; POSAS = patient and observer scar assessment scale; PT = physical therapy; ROM = range of motion; TBSA = total body surface area; TEWL = transepidermal water loss; UEFI = upper extremity functional index; VAS = visual analogue scale; VSS = Vancouver scar scale; y = year.
Among the two articles that examined the effect of stretching on scars and number of contracture, one RCT emphasised the early implementation of stretch exercise within 1 week after skin grafting (
The other CCT explored the effect of a 4-week intensive stretch on active scars in nine patients from 1–3 months after the injury, with more than 1 hour of stretch daily. Weekly changes were compared and largest gain of all measured ROM was found in the 1st week (
Massage (
Table 3
)
There were four studies that examined the effect of massage on scars properties without measuring the limitation in ROM (
For scar parameters, two nonequivalent controlled trials (
With an increased sample size to 146 and comparable study regime to
Another two trials, one level I RCT (
The only experiment that compared both ROM and scar parameter was performed by
Except for
Splinting intervention (
Table 3
)
One level II RCT was identified using splints to stretch and immobilise the shoulder in 90° abduction after axillary burn in 52 adults. Unconscious patients in the Intensive Care Unit were also recruited. In total, 12 (23.1%) subjects dropped out from the study. Compared with conventional treatments composed of stretching using strengthening and functional training, shoulder ROM did not statistically differ after the supplement of static stretching splint after 6 weeks’ all-day and 6 weeks’ night wear (
Discussion
The quality of studies that explored the effect of “mechanical stretch” composed interventions on post burn scars and contractures were varied. Five out of nine studies were rated fair to poor quality for the lack of random allocation, assessor blind, intention to treat, or size of treatment effect measurement procedures. Generally, the subjects demonstrated significant improvement in scar parameters after stretching exercise with early initiation (within 1 week after surgery), and last more than 1 hour daily. The cooperation between a weekly 90-minute massage program and comprehensive conventional intervention would also ameliorate the scar outcomes, such as thickness and erythema. The improvement in ROM limited by scar contracture can be achieved by early initiated stretch exercise on active scar areas or massage comprised with multiple techniques, such as effleurage, stretching, rolling strokes, friction, lengthening, and rolling (
It should be noted that two studies conducted by same author with similar intervention methods exhibited non-significant results after using objective scar measurement tools. The author inferred that this may due to the lack of large sample size and power, overestimate of the results in the trials, or using subjective scar measurements without assessor blinding (
As for early implementation of stretch in post burn patients, it is worth noting that there were also emerging studies verifying the effect of tension reduction in preventing or reducing the severity of scar and related contracture formation (
Although the effects of stretch are not only on scars but also on the underlying soft tissue, such as fascia, tendons, and muscles, it was generally accepted that the improvement in scar pliability and scar contracture would also increase the ROM of adjacent joints (
The conclusion of effectiveness of stretch on scar property and contracture should be drawn carefully for all stretch-incorporated treatments were applied in combination with other treatments, such as active exercise, pressure garment, moisturisation, or functional retraining. And the outcome measures remain incomparable for the inconsistent content or tools. Under these circumstance, it remains a challenge to verify the effect of one intervention modality.
Limitations
The limitation of this systematic review is that only a small number of studies met the inclusion criteria. Most of the studies were not assessed by a blind assessor; thus, it may contribute to assessment bias. Among the nine selected trials, the treatment regime and the outcome measures were varied, thereby adding the difficulty to analyse and interpret the findings. Moreover, there was a lack of clear explanation on the theoretical framework behind mechanical stretching.
Conclusion
Stretch is one of the most commonly used therapeutic techniques adopted for scar management. However, there seems a lack of understanding regarding the exact mechanism of stretching in the improvement of scar conditions. The direction, magnitudes, duration, and frequency of stretching were not clearly defined in the therapy regime, thus arising problems in proving its efficacy. Further high quality clinical trials on scar management are needed to generate the evidence to show its effectiveness. Future research should focus more on comparison among detailed regime of intervention application using a larger sample size. Basic science study should also be conducted to identify the underlying mechanism of stretching on the fibroblasts of the scar tissues.
Footnotes
Acknowledgements
The authors thank all of the researchers who conducted trials involved in the study.
