Abstract
Abstract
Purpose
Persistent tibial torsion in the older child can be treated with a derotation osteotomy. Distal tibial osteotomy has been recommended due to concerns of peroneal nerve palsy, vascular injury, and compartment syndrome with a proximal tibial osteotomy. However, an osteotomy in the proximal tibia may achieve union more rapidly and skin issues, as described for distal tibial osteotomies, are less likely. This study investigates the safety and efficacy of proximal tibial derotation osteotomies.
Methods
We retrospectively reviewed 43 tibiae in 25 consecutive children with persistent tibial torsion treated with a proximal tibial derotation osteotomy between 1991 and 2006. Patients with concomitant varus or valgus osteotomies were excluded. Diaphyseal fibular osteotomies were performed in five patients, while all patients had a prophylactic anterior compartment fasciotomy.
Results
The mean age at surgery was 10.4 ± 4.0 years and the mean follow-up was 3.2 ± 3.5 years. Patients with internal tibial torsion had a mean preoperative thigh–foot angle (TFA) of −14° ± 6° and a mean postoperative TFA of 8° ± 4°. Patients with external tibial torsion had a mean preoperative TFA of 38° ± 9° and a mean postoperative TFA of 7° ± 5°. The overall mean correction was 26° ± 9°. Major postoperative complications occurred in 4 patients (9%), including one peroneal nerve palsy which resolved, one delayed union requiring revision surgery, and two patients with mild postoperative valgus deformities.
Conclusions
Proximal tibial derotation osteotomy with an anterior compartment fasciotomy is a reliable method for treating tibial torsion with an acceptable complication rate. Given the larger bony surface area and improved soft tissue envelope, proximal tibial derotation osteotomy can be considered as an alternative to a distal tibial derotation osteotomy.
Introduction
Rotational malalignment of the tibia is a common problem in pediatric orthopedics. Internal tibial torsion is generally the result of intrauterine positioning [1]. Since it is physiologic in origin, most children correct with subsequent growth and activity. Older children with persistent internal tibial torsion can benefit from surgical correction. In contrast to internal torsion, external tibial torsion is more often progressive, with a greater proportion of patients requiring surgical treatment [1].
In 1959, Staheli et al. [2] studied 1,000 normal lower extremities of children and adults to establish normal values for the rotational profile. They concluded that the prone thigh–foot angle (TFA), the angle between the long axis of the foot and the long axis of the thigh with the knee flexed at 90° and the ankle in the neutral position, is the most accurate clinical method to determine rotational alignment of the tibia. The normal range is between −5° and 20° [2]. Surgical correction can be considered for significant cosmetic or functional issues, generally with a TFA in excess of −15° or greater than 30° in a child 9 years of age or older [3].
Derotation osteotomies of the tibia are commonly used to treat both internal and external tibial torsion. Osteotomies to correct both angular and rotational deformity at the proximal and distal tibia have also been described [4–17]. Some studies have questioned the safety of proximal tibial osteotomies due to an increased incidence of peroneal nerve palsy, vascular injury, and compartment syndrome [4, 6, 18, 19]. Krengel and Staheli [4] reviewed 52 tibial derotation osteotomies by 14 different surgeons and reported a complication rate of 13% (5 of 39 patients) in proximal osteotomies versus 0% (0 of 13 patients) in distal osteotomies, with complications including two cases each of compartment syndrome and peroneal nerve palsy and one case of deep infection. Their study was limited by the large number of surgeons and the fact that only 13 extremities or 25% of their osteotomies were performed distally [4]. In addition, their proximal osteotomies were typically performed for internal tibial torsion, while their distal osteotomies were for external tibial torsion [4].
We reviewed our experiences with a proximal tibial derotation osteotomy by a single surgeon for internal or external tibial torsion, without concurrent coronal plane correction. The purpose of this study was to revisit the incidence of complications in proximal tibial derotation osteotomies.
Materials and methods
This was a retrospective study of 43 extremities in 25 consecutive pediatric patients who underwent a proximal tibia derotation osteotomy by the senior author at two hospitals between 1991 and 2006. The Institutional Review Board (IRB) at both institutions approved this study. Patients with internal tibial torsion, external tibial torsion, and complex malalignment (combined femoral anteversion and external tibial torsion) were included. Patients were excluded if their derotation osteotomy was performed with concurrent correction of genu valgum or genu varum. This criteria was chosen because of our desire to contrast proximal and distal tibial derotation osteotomies. The inclusion of cases of genu varum or genu valgum in proximal tibia cases could create a bias, since distal tibia osteotomy is not used to correct genu valgum or genu varum.
Our databases at two hospitals were searched for all children treated by the senior author with a tibial osteotomy. Operative reports were screened for patients receiving a pure derotation osteotomy of the proximal tibia. A chart review was performed to obtain the preoperative and postoperative clinical and radiographic information. All radiographs were reviewed. We recorded age at surgery, diagnosis, initial TFA, postoperative TFA, tourniquet duration, cast duration, duration of follow-up, and the complications associated with the proximal tibial osteotomy.
Surgical technique
The patient is placed in a supine position on a radiolucent operating table. A tourniquet was utilized in all cases. The surgical incision is started 1 cm below the tibial tubercle just lateral to the anterior tibial crest. The proximal tibia was exposed subperiosteally, and the osteotomy performed with an oscillating saw. Correction was performed based on the preoperative TFA, with the goal of visually aligning the tibial tubercle with the second ray of the foot. A diaphyseal fibular osteotomy was performed to assist the derotation when the proposed derotation was greater than 20°. The tibial osteotomy was cross-pinned antegrade or retrograde with two smooth Steinmann pins (Fig. 1). An anterior compartment fasciotomy was performed in all cases. The periosteum is closed over the osteotomy, followed by routine skin closure. A long leg cast is placed with the knee positioned in approximately 30° of flexion.
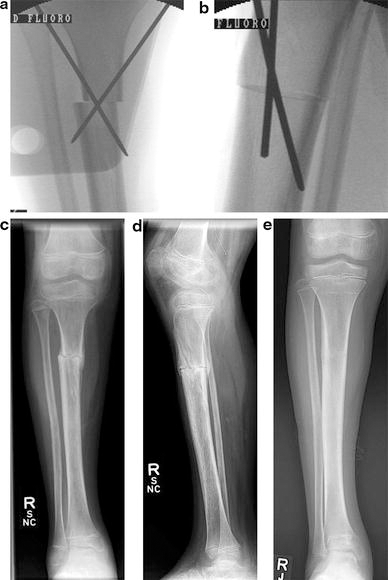
A 9-year-old male with right talipes equinovarus and internal tibial torsion.
Postoperatively, the patients are non-weight-bearing using crutches for 4–6 weeks. When there is radiographic callus formation, a new long leg cast is applied with the knee in extension. Full weight-bearing is allowed until there is satisfactory healing. The pins are then removed in the outpatient clinic.
Results
The mean age at surgery was 10.4 ± 4.0 years. The underlying diagnoses included: seven patients with idiopathic deformities, six patients with talipes equinovarus, four patients with cerebral palsy, four patients with complex malalignment, and one patient each with subtalar coalition, metabolic bone disease, calcaneovalgus feet, and hereditary motor-sensory neuropathy type II. Of the four patients with talipes equinovarus, there were two patients with idiopathic deformities and one each with arthrogryposis multiplex congenita and chromosome 20 disorder. Four of the 11 patients with external tibial torsion originally had complex malalignment. Two had resolved their femoral anteversion with persistence of the external tibial torsion, while two required distal femoral osteotomies as well.
Twenty-four extremities had persistent internal tibial torsion, while 19 extremities had external tibial torsion. Patients with internal tibial torsion had a mean preoperative TFA of −14° ± 6° and a mean postoperative TFA of 8° ± 4°. Patients with external tibial torsion had a mean preoperative TFA of 38° ± 9° and a mean postoperative TFA of 7° ± 5°. The overall mean correction was 26° ± 9°. The mean tourniquet time was 42 min for operations which only included derotation tibial osteotomies. Five cases also underwent diaphyseal fibular osteotomies. Eleven cases had additional procedures: five distal femoral derotation osteotomies, two calcaneal osteotomies, two medial foot releases with cuboid osteotomies, and one of each plantar fascia release, percutaneous tendo-Achilles lengthening, and flexor tenotomies of the fourth and fifth toes. The mean cast duration was 63 ± 31 days, including an outlier at 230 days due to delayed union. Excluding the outlier, the mean cast time was 58 days. The mean follow-up was 3.2 ± 3.5 years.
Complications
There were 4 extremities (9%) that sustained postoperative complications. One patient with cerebral palsy (spastic diplegia) had an apparent peroneal nerve palsy with difficulty of selective control of his tibialis anterior muscle postoperatively. He was treated with an ankle foot orthosis. Upon long term follow-up, he had regained dorsiflexion, with the ability to heel walk symmetrically.
Another patient underwent revision surgery at another facility for a delayed union. One patient with clubfoot and internal tibial torsion had a postoperative valgus deformity of 7°. This patient was later treated with growth modulation staples to correct the deformity. Another child with metabolic bone disease and internal tibial torsion developed a mild tibia valga deformity postoperatively. Hemiepiphysiodesis was recommended, but the family declined. The child had no complaints at 4 years follow-up.
There were no cases of deep infection. There were four cases of skin irritation from either pin sites or pressure sites, which did not require antibiotics. There were no cases of vascular injury or compartment syndrome. There were no cases of loss of tibial derotation correction or overcorrection requiring revision surgery.
Two patients sustained a fracture following complete healing of their tibial derotation osteotomies. One patient had a spiral fracture of the tibia distal to the osteotomy site 3 months postoperatively, which was treated with casting. Another patient sustained a proximal tibial fracture 10 months postoperatively after jumping off a stage. This healed uneventfully with cast immobilization. Due to the timing of these injuries, neither were included in our overall complication rate.
Discussion
Tibial torsion requiring surgical correction has historically been treated with proximal or distal tibial osteotomy. Krengel and Staheli [4] in 1992 questioned the safety of proximal tibial osteotomies. In their review of 52 derotation osteotomies, they incurred a major complication in 5 of 39 (13%) procedures performed proximally versus none of 13 procedures performed distally, and concluded that a proximal level osteotomy is indicated only when a varus or valgus deformity is to be corrected concurrently. However, their retrospective study included 14 different surgeons, presumably with a variety of surgical techniques. Two of their five complications with the proximal site osteotomy were anterior compartment syndrome, and a prophylactic anterior compartment fasciotomy was not routinely performed.
Other reports of pure derotation proximal tibial osteotomies have also been limited. Slawski et al. [5] reported on 255 tibial osteotomies, of which only seven were performed proximally. They grouped 74 total proximal and distal derotation osteotomies in their analysis, and their only peroneal nerve injury was found after a distal tibial derotation osteotomy. They also reported two cases of superficial wound infections, and one case of loss of fixation, without clarifying whether these were in proximal or distal osteotomies. A separate report of 57 derotation osteotomies of the proximal tibia on patients with poliomyelitis utilized O'Donoghue's derotation osteotomy, with a step-cut tibial osteotomy and suture fixation [12]. They reported two patients with intraoperative complications related to the osteotomy technique and one patient each with a traumatic fracture at 6 weeks postoperatively and a heel ulcer [12].
Peroneal nerve injury is an uncommon but serious complication in osteotomies involving the knee. The major cause of the nerve injury is thought to be either direct nerve damage or secondary nerve damage from vascular insult. Steel et al. [18] concluded that, during a proximal osteotomy for genu varum or genu valgum, the nerve damage is caused by arterial occlusion due to compression by external forces. Similarly, Schrock [19] performed a cadaver study which found that, after a proximal tibial osteotomy, the direction and amount of torsion correction was not correlated with peroneal nerve injury. They concluded that the most likely cause of peroneal nerve palsy is ischemia of the nerves and muscles within the tight fascial compartment of the anterior leg, and recommended prophylactic anterior fasciotomy versus fibular osteotomy to release the crural fascia. Clinically, they reported six peroneal nerve palsies in 62 cases (10%), with no palsies in the 16 extremities treated with fibular osteotomy [19].
We investigated the complication rate with derotation osteotomies of the proximal tibia, without varus or valgus correction. Our results found appropriate correction in all 43 tibiae. There was one case of apparent personal nerve palsy which resolved, and no cases of vascular injury or compartment syndrome. We attribute these results to the pure rotational aspect of the osteotomy, as well as the routine use of prophylactic anterior fasciotomies. We generally include a fibular osteotomy when more than 20° of rotational correction is desired. Although plate fixation is an option, we have not had any significant residual rotational deformities with cross-pin fixation.
Pinkowski and Weiner [20] previously reported on proximal tibial osteotomies for both angular and rotational deformities. Utilizing an anterior compartment fasciotomy and distal fibular osteotomy, they reviewed 37 consecutive osteotomies with no cases of compartment syndrome or peroneal nerve palsy. Although our study differed in the use of a midshaft fibular osteotomy, we feel that it supports the safety reported by Pinkowski and Weiner.
Distal tibial derotation osteotomies are not without complications. Peroneal nerve palsy has been reported with combined angular and rotational correction in the distal tibia [5]. The soft tissues can be tenuous, with three cases of skin dehiscence and one case of osteomyelitis in one series of 72 cases [21]. Two studies have found increased complication rates when fibular osteotomy is included [10, 11], with one of these prospectively randomized to ensure that the results were not due to increased initial rotational deformity [10]. A previous literature review reported overall major complication rates of 0–35% and residual deformity rates of 0–39% with distal osteotomy [9].
Two of our patients had a valgus deformity noted after consolidation of their osteotomies. We presume that this deformity is due to a medial overgrowth at the proximal osteotomy site. One patient was treated with growth modulation staples with improvement, while the other refused treatment. Currently, our practice is to monitor all proximal tibial osteotomy patients for valgus deformity, and to treat with guided growth if indicated.
Our study has important limitations. The follow-up time was limited due to the distances that patients had to travel for routine postoperative care. However, the major complications of concern in this study were compartment syndrome and peroneal nerve palsy, both of which are generally present during the early postoperative period. Our study was also limited in that our only measurement of rotation was the TFA. A previous study found a range of error of 5° between TFA and computed tomography (CT) imaging, which does not represent a clinically significant difference [21].
In summary, this study of 43 proximal tibial derotation osteotomies for internal or external torsion by a single surgeon demonstrated that proximal osteotomy is an effective technique with an acceptable complication rate. We recommend prophylactic anterior compartment fasciotomies in all patients. Given concerns with fibular osteotomies and soft tissue issues in distal osteotomies, we feel that proximal tibial derotation osteotomy is a reasonable method for the surgical treatment of tibial torsion.
