Abstract
Abstract
Purpose
Among posterior surgical techniques for treating adolescent idiopathic scoliosis (AIS), hybrid constructs with pedicle-screw fixation in the lumbar spine and other anchors in the thoracic spine have been reported to provide to be of more physiological value in postoperative thoracic kyphosis than all-screw constructs. The Universial Clamp (UC) equipped with a soft sublaminar band is a relatively new thoracic anchor that can be used in hybrid constructs. A dedicated reduction tool that applies traction to the sublaminar band permits gentle translation of the thoracic curve to the precontoured fusion rods, which have been previously anchored distally by pedicle screws and proximally by hooks in a claw configuration. The aim of this study was to evaluate radiographic results of AIS treatment using UC hybrid constructs.
Methods
This was a prospective case series in which 29 consecutive patients with Lenke type 1, 2 or 3 AIS operated on by two surgeons in two centers were followed for 24 months. Necessity for anterior release was an exclusion criterion.
Results
A total of 5.4 ± 1.4 UCs were used per patient. The major thoracic curve was reduced from 55 ± 7° to 14 ± 6° at 1 month and 17 ± 6° at 24 months (correction 70%) without complications. In the patients who had less than 20° of T5–T12 kyphosis preoperatively, thoracic kyphosis improved from 14 ± 4° to 20 ± 3° at 3 months and 24 ± 9° at 24 months. In the other patients, preoperative thoracic kyphosis (27° ± 6°) was unchanged by the operation.
Conclusion
UC hybrid constructs appear to safely provide satisfying coronal correction while consistently improving thoracic kyphosis in patients who also have preoperative hypokyphosis. We hypothesize that diminution in thoracic kyphosis was consistently avoided due to the straightforward traction of the spine to the fusion rods into which the chosen kyphosis was contoured by the surgeon before applying the reduction tool to the sublaminar bands.
Introduction
There is no consensus on the ideal posterior surgical technique for treating adolescent idiopathic scoliosis (AIS) [1–3]. Among posterior techniques, procedures using segmental pedicle screws are considered by some scoliosis surgeons as the current standard of excellence based upon the deformity correction it provides in the coronal and axial planes [4–6]. Others prefer hybrid constructs with pedicle-screw fixation in the lumbar spine but not in the thoracic spine [7, 8]. Next to concerns they may have over misplaced pedicle screws [9–11], proponents of hybrid constructs report postoperative thoracic kyphosis to be of more physiological value to patients than all-screw constructs [7, 8], with little difference in coronal or axial correction [12]. A number of thoracic anchors can be used to replace the thoracic pedicle screws in hybrid constructs, including hooks, sublaminar wiring, intraspinous wiring and soft sublaminar bands [3, 13, 14].
We have previously reported our 3-month postoperative results using hybrid constructs, including a recent system of thoracic spinal anchorage, the Universal Clamp (UC) [15]. In that series of 32 patients with Lenke type 1, 2 or 3 AIS operated on with no anterior release, UC hybrid instrumentation safely achieved 73 ± 12% correction, from 55 ± 7° to 14 ± 9°. Among the 12 patients with low values of preoperative thoracic kyphosis, thoracic kyphosis was increased by an average of 9° at 3 months. In the 20 patients with more physiological values of preoperative thoracic kyphosis, there was no statistical difference in kyphosis after the operation. The purpose of this report was to evaluate the same group of patients to determine whether these good initial results were maintained at their 2-year follow-up visit.
Methods
Patients
Consecutive patients with Lenke type 1, 2 or 3 AIS were included in the study by two surgeons in two centers. Exclusion criteria were major lumbar curves, necessity for anterior release, congenital or neuromuscular scoliosis and spinal cord disorders visible on magnetic resonance imaging (MRI) scans.
The preoperative radiographic work-up included whole-spine erect posterior–anterior (PA), whole-spine erect lateral, and supine bending radiographs. Angular measurements were made in terms of Cobb angle by an independent observer with no intraobserver or interobserver verification. The following ratios were calculated:
Preoperative flexibility (PF): PF (%) = [(preoperative erect Cobb angle − supine bending Cobb angle)/preoperative erect Cobb angle] × 100 Postoperative correction: (POC) POC (%) = [(preoperative erect Cobb angle − postoperative erect Cobb angle)/preoperative erect Cobb angle] × 100 Cincinnati correction index (CCI): CCI = POC/PF
Paired-samples t tests were used to analyze differences between preoperative curves and postoperative curves. All statistical tests were two-tailed, and a P value < 0.05 was considered to be significant.
Results
Thirty-two consecutive patients (28 girls, 4 boys) who did not have anterior release were included in the original study. Three of the original patients did not return for the follow-up visit at 2 years. Of these three patients, one has not returned since the 1-year visit, and one each was seen at the 3- and 4-year follow-up, respectively. These three patients were older than the initial cohort of 32 patients (mean age at operation 18 vs. 15 years, respectively) and experienced more change in thoracic kyphosis (mean 7° increase vs. 2° increase at 3 months, respectively), with little difference in the average 3-month coronal thoracic Cobb angle improvement (mean 39° vs. 41°, respectively) or percentage correction (mean 74 vs. 73%, respectively). Twenty-nine (27 girls, 2 boys; average age at operation 14.7 ± 1.6 years) patients were seen at the 2-year follow-up (90.6% follow-up). On average, 5.4 ± 1.4 UCs were used per patient in these 29 patients, and none of the original 32 patients required thoracoplasty.
The average preoperative value of the major thoracic curve of the present 29 patients was 55 ± 7° (range 42–70°). At the 1-month follow-up, the Cobb angle measured 14 ± 6° (range 6–30°), representing an average POC of 75 ± 10%. At the 12-month follow-up, (n = 28 patients), the Cobb angle was 16 ± 6° (range 8–30°), and the average POC had slightly decreased to 71 ± 12%. At the 24-month follow-up (n = 29 patients), the major thoracic Cobb angle was 17 ± 6° (range 5–28°), representing a POC of 70 ± 10%. The average loss in POC was 3 ± 5° (range from a loss of 13° to a gain of 3° in correction) with respect to the Cobb angle at the 1-month follow-up. The course of the thoracic curve Cobb angles is illustrated in Fig. 1.
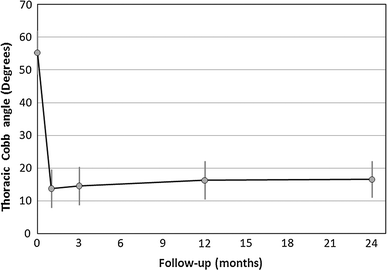
Curve of major thoracic curve Cobb angle. The bars around the mean values (circles) represent ±1 standard deviation (SD)
Preoperative bending films were not obtained in two of the patients. In the other 27, the PF of the main curve was 51 ± 13%. Their average computed CCI was 1.56 ± 0.44 at 1 month, 1.51 ± 0.42 at 3 months, and 1.44 ± 0.39 at 24 months. As shown in Fig. 2, preoperative flexibility had almost no influence on the percentage of thoracic curve correction at 24 months [r2 = 0.11, not significant (NS)]. Figure 3 shows the course of the lumbar curve Cobb angle from preoperative values to the 24-month follow-up. The final lumbar Cobb angle of 8 ± 5° corresponded to a correction of 72 ± 20% of the preoperative lumbar scoliotic curve (36 ± 15°).
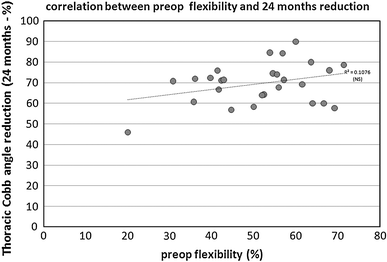
Correlation between preoperative flexibility and major thoracic curve Cobb angle correction at 24 months
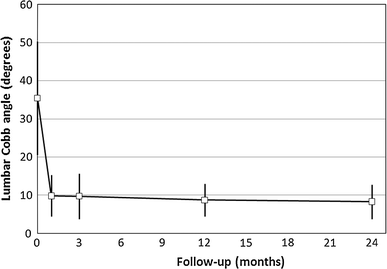
Course of lumbar curve Cobb angle. The bars around the mean values (circles) represent ±1 SD
A preoperative lateral film was not obtained in one of our patients. The average course of thoracic kyphosis and lumbar lordosis in the other 28 patients is shown in Fig. 4. These patients had widely varying values of preoperative thoracic kyphosis. In the 16 patients who had <20° of thoracic (T5–T12) kyphosis on the preoperative film (see Table 1), the average preoperative thoracic kyphosis was 14 ± 4°. Three months and 24 months (2-year follow-up) after the procedure, these 16 patients had an average thoracic kyphosis of 20 ± 3° and 24 ± 9°, respectively; in the other 12 patients, the average preoperative thoracic kyphosis was 27 ± 6°. The average thoracic kyphosis of these 12 patients was unchanged by the operation (24 ± 9° at 3 months postoperatively and 26 ± 10° at 2 years).
Course of lumbar lordosis and of thoracic kyphosis. The bars around the mean values (circles) represent ±1 SD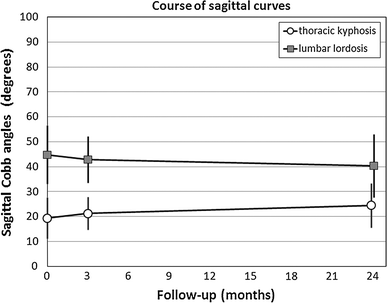
Nonexhaustive comparison of thoracic coronal correction and influence on kyphosis of various types of vertebral constructs in adolescent idiopathic scoliosis
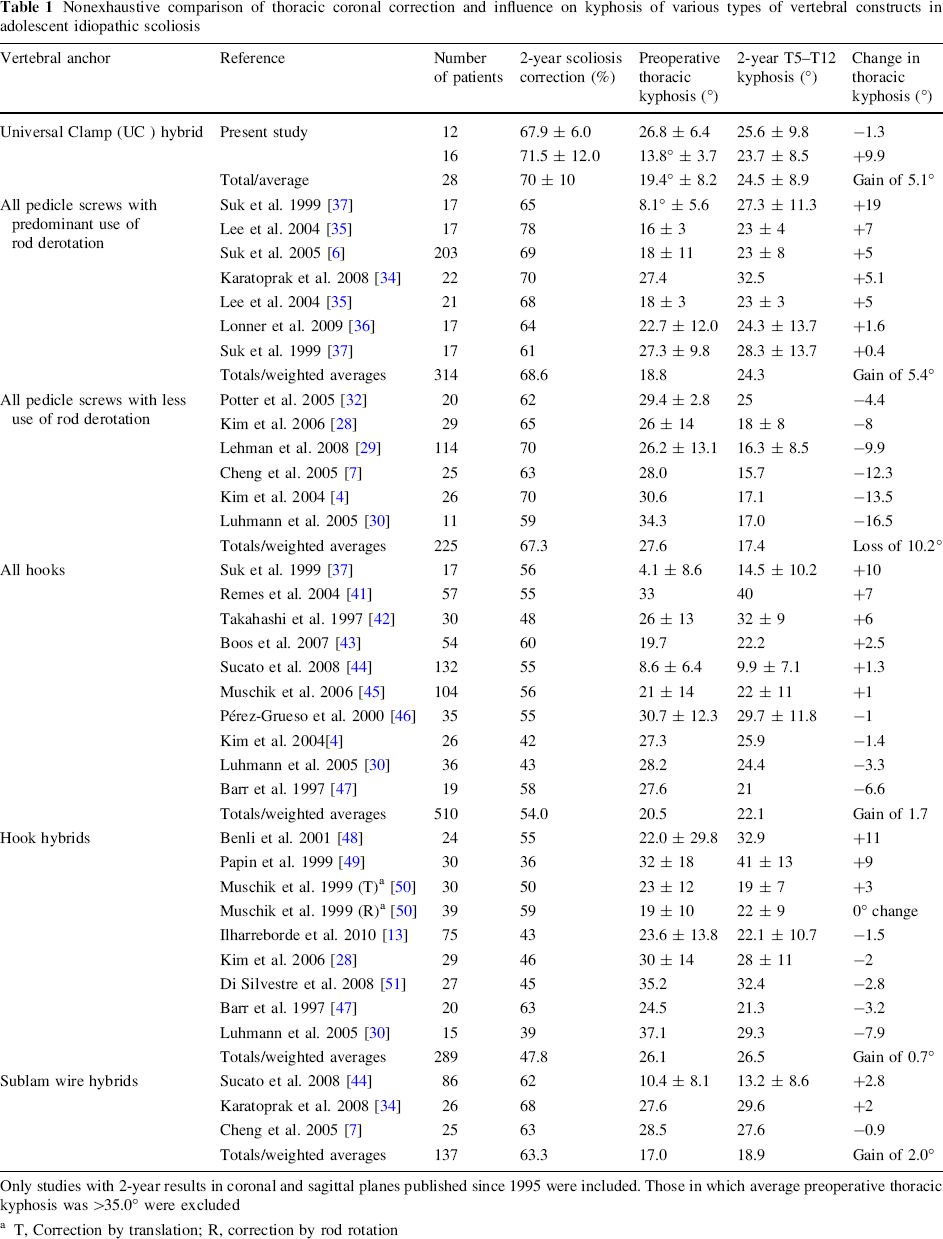
Only studies with 2-year results in coronal and sagittal planes published since 1995 were included. Those in which average preoperative thoracic kyphosis was >35.0° were excluded
T, Correction by translation; R, correction by rod rotation
Conventional hook-claw constructs were used at the proximal extremity of the fusion construct in all of these patients. Proximal hook-claw dislodgement was observed in two patients during the first year of follow-up and in a third patient during the second year. In two patients, proximal hook-claw dislodgement was observed at the 1-year follow-up with no clinical consequences; a third patient had slight proximal prominence at the 2-year follow-up, but an X-ray scan showed that the proximal hook-claws remained correctly anchored. All three patients had fused and none required reoperation. To date, after the minor complications previously reported, there have been no further adverse events involving the UC anchors. All of the instrumented levels fused in our patients.
Figures 5, 6, 7 and 8 illustrate typical results in one of our patients who had a UC hybrid fusion construct.
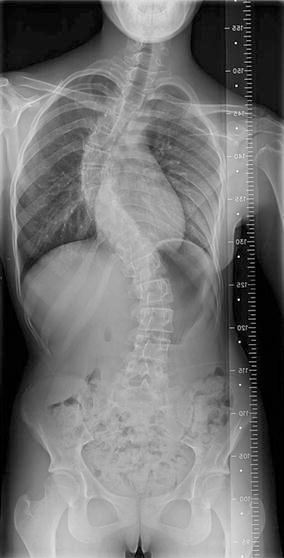
Preoperative view of one of the patients treated for Lenke type 3 adolescent idiopathic scoliosis (AIS)
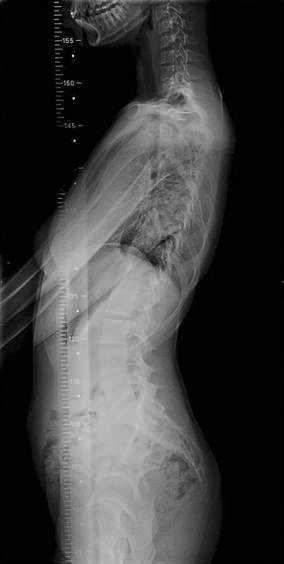
Lateral view of the same patient showing T5–T12 hypokyphosis (7°)
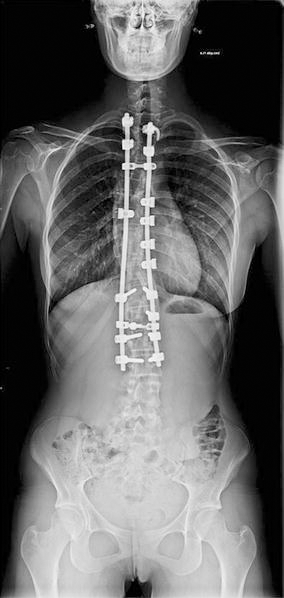
Two-year follow-up view showing the 60% correction achieved
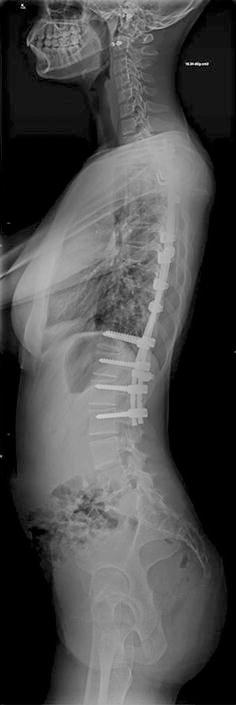
The T5–T12 kyphosis had improved by 13–20° at the 2-year follow-up
Discussion
The intermediate-term observations reported here complete the intraoperative, immediate postoperative and short-term findings on the safety and efficacy of Universal Clamps described by us in an earlier publication for the same cohort of patients [15]. The safety and efficacy of the initial report are confirmed by the 2-year follow-up data reported here.
In terms of safety, there were no complications directly involving the UC anchors between 3 months and 2 years. Mazda et al. reported on a group of 75 AIS patients who received hybrid constructs that included apical and peri-apical UCs and distal pedicle screws. Among their earliest patients, in whom UCs were also used at the most proximal vertebra included in the fusion, these authors reported proximal posterior prominence in 11 patients. leading them to recommend conventional claws at the upper extremity of the constructs. There were no other intermediate-term complications related to the use of the sublaminar UCs in their report [16]. Taking into account this recommendation to use conventional hook-claw devices at the proximal extremity of hybrid constructs, we recorded no intermediate-term UC-related complications. The promising intermediate-term safety results of sublaminar UCs are in contrast to the intermediate-term safety issues of sublaminar wiring [17–19]. La Rosa et al. also noted the safety of UCs used in hybrid constructs with thoracic hooks and lumbar pedicle screws in a series of 15 patients with neurological scoliosis greater than 100° and an average follow-up of 3 years [20]. An apparent superiority in both intraoperative and intermediate-term safety of UCs compared to sublaminar wires has also been discussed by spinal surgeons who reported the use of UCs in the thoracic spine for traumatic vertebral lesions [21]. The latter authors confirmed the absence of implant-related MRI artifacts in the vertebral canal as well as the absence of epidural fibrosis next to the bands, either of which could have otherwise compromised early and intermediate postoperative safety. Even though severe neurological complications after surgical interventions for AIS are rare (none in the present series), it is important to use implants that do not preclude the use of MRI in case postoperative neurological complications do occur (Appendix).
The present 2-year findings confirm the efficacy reported initially in the same cohort of patients. With the UC hybrid constructs, the good correction (71%) of the main thoracic curve from a mean of 55° preoperatively to 16° at 1 year after the operation was only 4 percentage points less than the mean immediate postoperative Cobb angle (14°). Moreover, there was no further loss of the achieved correction between 1 year and 2 years. This confirmed an earlier study by Ilharreborde et al., who reported an average initial thoracic main curve correction from 60° preoperatively to 20° (66% correction) in 75 AIS patients treated with UC hybrid constructs and a subsequent loss of only 2° (3%) at the 2-year follow-up [13]. In the series of 15 patients with more severe, neurological scoliosis >100°, La Rosa et al. achieved a 70% initial reduction (from 107 to 32°) and lost only 7° of correction after an average follow-up of 3 years [20].
The intermediate-term results reported here on the corrective efficacy of the UC in the coronal plane are not inferior to results observed with other spinal anchors that have known safety issues [2, 22–27]. An initial average thoracic curve correction from 54° to 27° (50%) achieved in 75 AIS patients with hook hybrid constructs (before the development of the UC) was followed by a loss of 4° observed 2 years postoperatively [13]. In a series of 78 patients with either idiopathic or neurological scoliosis treated by segmental sublaminar wiring, Luque reported an average reduction from 69 to 20° (72% correction) followed by a 2% loss of correction (mean of <2°) during the treatment period [23]. Kim et al. reported an average main curve correction from 63° preoperatively to 16° postoperatively (76%) in 26 AIS patients treated with segmental pedicle-screw instrumentation compared to a correction from 66 to 33° (50%) in 26 matched patients treated using hook instrumentation. At the 2-year follow-up, the loss of correction was 4° in the pedicle-screw group and 4° in the hook group [4]. The same team reported an average main curve decrease from 62 to 19° (70% correction) in 29 AIS patients with all-pedicle screw constructs and from 60 to 27° (56% correction) in a matched series of patients treated with hybrid constructs that included hooks in the thoracic spine and pedicle screws distally. After 2 years, 3° of correction was lost in the pedicle-screw group and 6° of correction was lost in the hybrid group [28].
Among the present AIS patients who had normal values of thoracic kyphosis preoperatively, there was almost no change in average thoracic kyphosis at the follow-up visits. However, among the patients with low preoperative values of T5–T12 kyphosis, the average T5–T12 kyphosis increased by 6° at 3 months and continued to improve thereafter, attaining an increase of 10° at 2 years. This improvement in thoracic kyphosis confirms previous results on the use of the UC for both AIS and neurologic scoliosis [13, 16, 20], and contrasts with a large body of evidence suggesting that conventional all-pedicle screw constructs tend to worsen flatness of the thoracic spine in AIS [3, 4, 7, 8, 28–33] unless rod derotation is the predominant means used to correct coronal deformity (see Table 1) [6, 34–37]. Based upon a retrospective study of patients with Lenke type 1 AIS treated with all-pedicle screw instrumentation, Quan and Gibson recently concluded that the greater the coronal plane correction achieved with pedicle-screw constructs, the greater the loss of thoracic kyphosis [33]. The authors of a large multicenter analysis of patients with Lenke type 1 AIS surgically treated by a selective thoracic fusion have recommended techniques that lengthen the posterior column in order to maintain or increase thoracic kyphosis [31]. Among the techniques recommended to prevent diminution in thoracic kyphosis, the authors cited contouring kyphosis into the fusion rods. We believe that this is the key to the promising immediate and intermediate-term results observed in the sagittal plane with the UC compared to pedicle screws. Contouring more thoracic kyphosis into fusion rods may increase the difficulty of bringing thoracic pedicle screw heads to the rods, whereas traction of the spine to the fusion rods with the UC sublaminar bands and reduction tool remains just as straightforward regardless of the degree of kyphosis the surgeon decides to precontour into the rods. This also may explain why apical sublaminar wiring can provide significantly better thoracic kyphosis than conventional pedicle screws [7] and why certain pedicle screw systems with special translation-mediating screw heads can also improve hypokyphosis in AIS patients [38, 39].
As shown in Table 1, the thoracic curve correction achieved and maintained in the AIS patients described here appears to be substantially higher than that reported for all-hook and hook hybrid techniques. The results in Table 1 also suggest that the sublaminar wire hybrid techniques, which resemble the UC hybrid technique, provide very satisfying deformity correction without lessening thoracic kyphosis. For various reasons, all-pedicle screw constructs have begun to supplant all-hook, hook hybrid, and wire-hybrid techniques in many countries [5]. Regardless of the deformity-correcting method employed with all-screw constructs, the Cobb angle correction achieved is equivalent to that achieved with UC hybrid devices. The use of rod derotation alone to correct scoliosis is avoided in some units to prevent overcorrection [40]. However, as Table 1 shows, unless rod derotation is used with all-screw constructs, the latter tend to reduce thoracic kyphosis, which is in contrast to the substantial gain in thoracic kyphosis obtained when UC hybrids are used.
We did not report our results on apical vertebral derotation in this paper because they relate to the 2-year outcome on a series patients for whom we have already reported the short-term results [15]. In that preliminary paper, only the coronal and sagittal corrections were reported. The primary objective of the present article was to show to what degree the immediate and 3-month postoperative results were maintained 2 years after the intervention. In our opinion, apical vertebral derotation is important—but difficult to obtain. Systematic preoperative and follow-up computed tomography scans were not performed in these children to avoid exposure to unnecessary radiation. We are currently studying the amount of derotation achieved in UC patients using the new EOS imaging system, which was not available at the time our patients underwent surgery. A sufficient number of patients have not yet undergone EOS imaging and derotation measurement for reliable conclusions to be drawn. This will be the objective of an upcoming report when this study is completed.
Conclusions
The present series of AIS patients treated with hybrid constructs that included proximal hook-claws, apical UCs, and distal pedicle screws was small. However, with data from the 2-year follow-up, it provides still more evidence that these hybrid constructs safely provide satisfying coronal Cobb angle correction while consistently improving thoracic kyphosis in the patients who also have preoperative hypokyphosis. The authors hypothesized that a diminution in thoracic kyphosis was consistently avoided due to the straightforward traction of the spine to the fusion rods into which the chosen kyphosis was contoured by the surgeon before the reduction tool was applied to the sublaminar bands.
Footnotes
Acknowledgments
Funds were received in support of this study from Zimmer Spine, SAS, Bordeaux, France. No other funds were received for this research.
None.
