Abstract
Keywords
1. Introduction
Lung cancer is the leading cause of cancer related death worldwide in both genders [1]. Despite the improved diagnostic tools and treatment strategy, overall survival is still poor; metastatic recurrence is also the most important cause of death after complete resection. The metastatic process involves a number of steps that unfortunately are not yet completely understood [2]. In particular, several authors postulated that manipulation of the tumour during surgery might promote early spreading [3, 4]. Release of tumour growing factors, surgical stress-related suppression of the innate immunity, reduction of anti-angiogenesis factors and tumour cells shedding in the bloodstream were considered as possible causes; however, the reported results were often contradictory due to the heterogeneity of the study populations.
In 1948 Mandel and Metais demonstrated the presence of circulating free DNA (cfDNA) in the bloodstream and subsequent studies showed a correlation between high cfDNA levels and neoplastic diseases [5–8]. Recently, with the improvement of extraction and quantification methods, the determination of cfDNA is becoming a useful diagnostic and prognostic tool also in lung cancer patients [9, 10]. It has been demonstrated that high preoperative cfDNA levels show a negative impact on long term survival, independently from a patient's age and stage of the disease [11]. However, the explanation of the mechanism involved in cfDNA release still remains uncertain. Several hypotheses (tumour cells lysis, apoptosis, necrosis or active secretory effects of neoplastic cells) have been proposed, but none of them is exhaustive [12, 13]. Furthermore, the relationship between cfDNA levels, disease progression and metastatic spreading is still debated. Based on previous experimental studies on cfDNA plasma levels after surgical procedures, some authors focused on circulating cancer cells and nucleic acids, postulating in animal models that their postoperative increased levels might show an impact on the mechanism of metastatic spreading [14, 15]. However, this hypothesis has not yet been confirmed since there are no clinical studies evaluating the levels of circulating nucleic acids during the early postoperative course; thus, we are not able to assess correctly the potential modifications during follow-up and understand the role of surgical manipulation on their release within the bloodstream.
2. Materials and methods
Twenty-five consecutive patients (17 men – eight women; mean age 62 4 ± 10 years) with lung cancer underwent complete surgical resection. None of them had a previous history of cancer or received induction therapy. Twenty voluntary healthy subjects (10 men – 10 women; mean age 37 ± 15 years) were considered as the control group. After an exhaustive explanation of the objectives of the study, all patients and controls signed an informed consent. Fifteen patients (60%) had squamous cell carcinoma and 10 (40%) had adenocarcinoma. None of them had chronic viral infections. We performed eight right upper lobectomies, six right lower lobectomies, five left upper lobectomies, five left lower lobectomies and one right intrapericardial pneumonectomy; in four lobectomy patients, because of neoplastic ribs invasion, a chest wall resection was required. In all cases a complete hilar and mediastinal lymph node dissection was performed at the end of the procedure. Interlobar fissures were created in all cases with surgical staplers, with the obvious exception of pneumonectomy. No blood transfusions were required. Fifteen patients (60%) were at stage I, seven (28%) at stage II and three (12%) at stage IIIA. A withdrawal of 6 mL peripheral blood was collected in tubes containing EDTA the day of surgery just before induction of anaesthesia, one week and one month postoperatively. The samples were processed to obtain plasma within an hour after the withdrawal of the blood sample. Plasma was separated from the cellular fraction by centrifugation two times at 2500 rpm for 10 minutes at 4°C. The resulting supernatant (plasma) was frozen at-80°C. DNA was extracted from plasma by using QIAamp DNA Mini kit (Qiagen, Italy) according to the supplier's instructions; this provided an elution in a final volume of 50 uL. The DNA was stored at-20°C until it was analysed.
To quantify the plasma circulating DNA we used a real-time quantitative polymerase chain reaction (PCR) approach based on the 5′ nucleotide method. This methodology is based on continuous monitoring of a progressive fluorogenic PCR by an optical system [16]. The PCR system uses two amplification primers and an additional amplicon-specific and fluorogenic hybridization probe, the target sequence of which is located within the amplicon. The probe is labelled with two fluorescent dyes. One server was used as a reporter on the 5′ end (FAM dye; Applied Biosystems, Foster City, CA, USA). The emission spectrum of the dye is quenched by a second fluorescent dye at the 3′ end (TAMRA; Applied Biosystems, Foster City, CA, USA). If amplification occurs, the 5′ to 3′ exonuclease activity of the AmpliTaq (Biosystems, Foster City, CA, USA) DNA polymerase cleaves the reporter from the probe during the extension phase, thus releasing it from the quencher [17]. The resulting increase in fluorescent emission of the reporter dye is monitored during the PCR process.
The real-time PCR was performed on an ABI PRISM 7500 Fast Real Time PCR System (Applied Biosystem, Foster City, CA, USA). Primers and probes were designed to specifically amplify the ubiquitous gene of interest, the ACTB2 single copy gene mapped on 5q11.2 (Gene ID: 345651, Applied Biosystem, Foster City, CA, USA). The amplicon size of the ACTBL2 gene was 67 bp. PCR reaction was carried out on 96-well plate with 20 uL per well using 1X TaqMan Master Mix. After incubation for two minutes at 50°C and 10 minutes at 95°C, the reaction continued for 40 cycles at 95°C for 15 seconds and 60°C for one minute. Each plate consisted of patient samples in triplicates and multiple water blanks as negative control. For construction of the calibration curve on each plate, we used a standard TaqMan Control Human Genomic DNA (Applied Biosystems, Foster City, CA, USA) with appropriate serial dilutions at 100, 10, 1, 0 1, 0 01, and 0 001 ng. All of the data were analysed using the ABI PRISM 7500 software (Applied Biosystems Foster City, CA, USA) to interpolate the standard amplification curve of DNA at a known quantity with amplification cycle threshold of the unknown target sample, obtaining the relative amount of DNA in the experimental sample.
3. Statistical analysis
Quantitative variables were reported as mean ± standard deviation and the differences were analysed with the Student's T test. Correlation analysis was performed between cfDNA levels and quantitative variables (age and tumour dimension). Qualitative variables as stage, pathological nodal status, histology, presence of tumour necrosis, grading, type of surgery (standard vs. extended), and history of smoking were reported as present or absent and used to identify two groups of patients at the three different steps. Differences of cfDNA levels between these groups were assessed by the Student's T test. Statistical analysis was performed with SPSS software (version 17 0, SPSS Inc., USA).
4. Results
The surgical procedure lasted a mean of 88 4 ± 21 3 minutes (range 62 – 115 minutes). After surgery, all patients were recovered in the surgical ward. No major postoperative complications occurred with an uneventful postoperative course in all patients. No adjuvant therapy has been administered before the third blood withdrawal at one month. In all patients the third blood sample was obtained; furthermore, in 14 patients (56%) we were able to collect blood samples at six and 12 months. The median follow-up was 16 months. In the study population and in the control group the mean preoperative level of cfDNA was 23 07 ± 7 4 ng/ml and 7 5 ± 3 4 ng/ml respectively (p=0 0002). After one week the cfDNA bloodstream level was 68 2 ± 36 2 ng/ml (p=0 0006) and after one month the cfDNA values significantly dropped below preoperative levels (9.6 ± 3.1 ng/ml) (p=0.0001). The difference between the cfDNA levels measured one month after surgery and those obtained in healthy subjects did not reach statistical significance (9 6 ± 3 1 ng/ml vs. 7 5 ± 3 4 ng/ml p=0 1). No correlation was found between preoperative and one week cfDNA levels, age (p=0 989 at both time points) and tumour diameter (p=0 925 and p=0 325 at each time point). No other variable considered for statistical analysis showed an impact on cfDNA levels at the different time points of the study (Table 1); the increase of cfDNA values after one week seems absolutely independent from any assessed variable. No statistically significant differences on cfDNA values were reported between pathological stages neither preoperatively nor during the follow-up. After a median follow-up of 16 months no patient showed recurrence; stage III patients underwent adjuvant chemo-radiotherapy. Eighteen patients (72%) were reassessed six months after surgery and 14 (56%) after 12 months showing stable cfDNA levels (Fig.1).
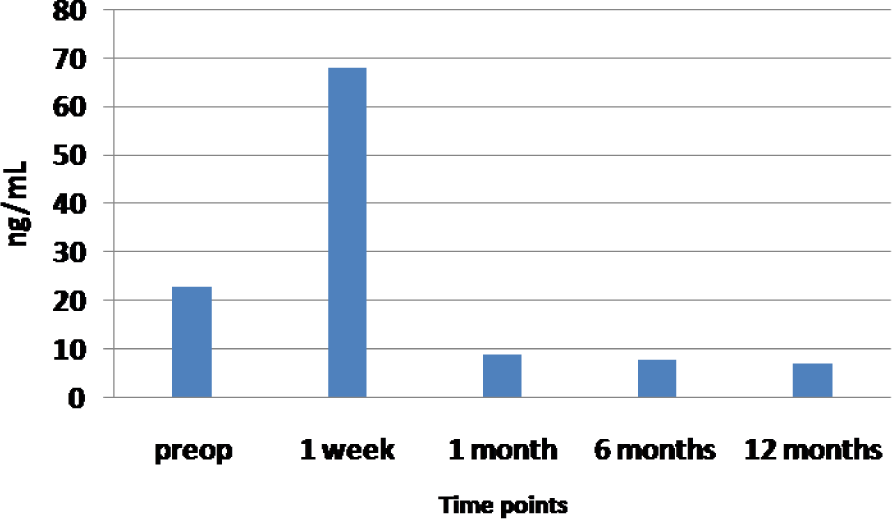
Trend of cfDNA levels in patients undergoing surgery
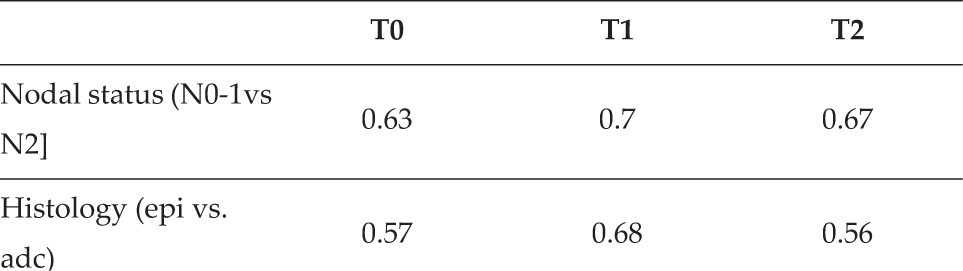
P values of cfDNA levels at three steps according to qualitative variables assessed by independent Student's T test
5. Discussion
Metastatic disease is still the leading cause of death after complete surgical resection of lung cancer. Metastatic spreading involves several steps: the presence in the bloodstream of circulating cancer cells (with their nucleic acids), their passage from blood to distant organs and the growth in the new site. The mechanism of this process is not completely understood yet, although it has been postulated that a reciprocal transition of cancer cells between the epithelial and mesenchymal status should be involved [18]. Several authors suggested that surgical manipulation could promote this cascade already during the immediate postoperative course; many different mechanisms have been advocated to elicit this process, in particular the decrease of immune-competency after surgery, the production of oxygen free radicals by leukocytes or tumour cells shedding into the bloodstream [19, 20]. Cell-free tumour nucleic acids (cfDNA) levels have been proposed as a diagnostic and prognostic tool in several solid cancers. Furthermore, cfDNA determination in lung cancer patients has gained importance during recent years. Yoon and colleagues in 2009 compared cfDNA levels between lung cancer patients and healthy subjects finding higher values in the former group [9]. Paci and colleagues demonstrated that in 151 lung cancer patients cfDNA levels were higher when compared to healthy individuals and that the risk of disease increases with higher cfDNA levels; in particular with a cut-off of 2 ng/ml, higher concentrations are strongly connected with the presence of neoplastic disease [10]. Van der Drift and colleagues in 2010 reported that high cfDNA levels at the time of diagnosis were a prognostic factor for poor survival, although no correlation was found with stage, histology and age [11]. Our study confirms that in the lung cancer population cfDNA levels are higher than in healthy subjects. These molecules might not be produced only from tumour cells degradation; they can also be released by an active secretory mechanism and they can play a role in the metastatic process. In fact, it has been demonstrated in an animal model that haematogenous dissemination of tumours due to surgery seems related to the presence of cfDNA [15]. However, in a study on percutaneous liver biopsy in patients with hepatocarcinoma no relationship was found between this procedure and cfDNA plasma dissemination [21]. Our results show that one week after surgery, cfDNA levels increase, probably due to manipulation, but after one month they drop below preoperative values in all patients and remain stable during the time period of the study. Thus, since all patients show this pattern, if surgical manipulation related release should be involved in the metastatic process, it must be in combination with other variables different from patient to patient (release of tumour growing factors, suppression of innate immunity, reduction of anti-angiogenesis factors, etc.). The absence of statistical significance between the study population one month after surgery and the control group allows us to conclude that the impact of lung manipulation is restricted to the very early postoperative course and cannot influence the metastatic process by itself. The surgical stress entails an increased inflammatory response with determination of high cfDNA levels, but probably the causes and mechanisms of the metastatic process should be researched somewhere else.
Footnotes
All authors declare no conflict of interest.
