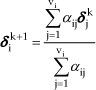Abstract
Aortic dissection is the result of blood intruding into the layers of the aortic wall creating a duplicate channel along the aortic course. This considerably changes aortic morphology and thereby alters blood flow, inducing severe pathological conditions. Endovascular stent-graft placement has become an accepted treatment option for complicated Stanford type B aortic dissection. Stent-graft deployment aims to cover the primary entry, preventing most of the inflow to the false lumen, thereby promoting false lumen thrombosis and true lumen expansion. In recent years the application of this treatment has increased continuously. However, a fast and reasonable prediction for the released stent-graft and the resulting aortic remodelling prior to intervention is still lacking. In this paper, we propose a preliminary study on the fast virtual stent-graft deployment algorithm based on contact mechanics, spring analogy and deformable meshes. By virtually releasing a stent-graft in a patient-specific model of an aortic dissection type Stanford B, we simulate the interaction between the expanding stent-graft and the vessel wall (with low computational cost), and estimate the post-interventional configuration of the true lumen. This preliminary study can be finished within minutes and the results present good consistency with the post-interventional computed tomography angiography. It therefore confirms the feasibility and rationality of this algorithm, encouraging further research on this topic, which may provide more accurate results and could assist in medical decision-making.
1. Introduction
Aortic dissection remains a challenging disease with high morbidity and mortality [1, 2]. It is the result of a tear in the intima of the aorta, allowing blood to flow within layers of the media. The created blood-filled intramural space becomes a false lumen, diverting a considerable amount of blood from the original aorta. The false lumen may compress the true lumen and/or extend into branch arteries, ultimately leading to organ malperfusion. Furthermore, aortic dissections can become aneurismal and ultimately lead to aortic rupture.
Patients with uncomplicated aortic dissection type Stanford B are usually managed medically with anti-hypertensive therapy. If the best medical treatment fails or complications occur (e.g., aortic rupture, end-organ ischemia, persistent pain), surgical treatments or endovascular aortic repair is necessary.
Compared to surgical treatment, thoracic endovascular aortic repair is less invasive, with lower morbidity and mortality [3, 4]. It aims at sealing the primary entry, allowing for false lumen thrombosis in the thoracic aorta and establishing thoracic remodelling. Unfolding of the stent-graft not only leads to an increase in true lumen diameter within the stented segment but also of the downstream aorta, thereby reducing blood pressure and lowering the risk of end-organ ischemia.
The effectiveness of endovascular repair is highly dependent on the released configuration of the stent-graft [5]; a method that can predict this situation prior to intervention could contribute to the success of this treatment.
During the past decade, many studies focused on numerically simulating the process of stent/stent-graft deployment and its interaction with the vessel wall [6-9]. Most of this research was involved approaches related to Finite Element Analysis (FEA), with a focus on detailed deformation of the stent and investigation of local stress at each strut on the metal mesh [10, 11]. These studies provide excellent estimations of the deployed configurations of the stent and offer detailed mechanical analysis of the stent-vessel contact process. However, they are time-consuming. The FEA with deformable meshes requires many computational resources. With the average computational capability, a precise simulation takes days, which is too slow to provide a prediction for endovascular treatment or assist medical decision-making.
Recently, a fast virtual stent deployment algorithm that applies to intracranial aneurysms has been proposed [12, 13]. This algorithm simulates the stent deployment process by using deformable simplex meshes with constraints, which can be presented by a second order differential equation that moves the stent mesh under the effect of internal and external forces. The program finishes within minutes, providing a fast estimation of the released stents when treating intracranial aneurysms. However, this algorithm takes little account for changes in arterial morphology. The stent-graft applied in aortic dissection is not only to prevent bloodstream towards the false lumen, but also to enlarge true lumen diameter, which makes the development of a fast virtual stent-graft deployment algorithm even more challenging.
In this paper, we introduce a method that can simulate stent-graft deployment, including its interaction with the vessel wall, in a fast way. It is based on spring analogy, deformable meshes and contact mechanics. At this preliminary stage, we aim at testing the feasibility of the basic frame of this program and especially focus on investigating its capability in simulating changes in true lumen diameter. Thus, simplifications have been made, like assuming the metal mesh of the stent and the fabric are an integrative body and considering the stent deploys along the radial direction only. The results that we will present have been compared to the post-interventional computed tomography angiography (CTA), which validates the rationality of this approach and confirms its feasibility for application in dissection cases. More precise studies could be achieved by taking account of the more detailed mechanical properties of the stent in the future. However, the current work that confirms the feasibility may encourage further development that can actually apply this approach in assisting medical decision-making.
2. Methodology
Formal consent from the examined patient and approval of the local ethic committee were obtained prior to the examination.
A. Geometry of the Dissected Aorta and Stent-graft
A 78 year old, female patient with expanding Stanford type B aortic dissection was examined by CTA prior and 21 days after stent-graft implantation (Gore TAG device) (Fig. 1a-b).
Both CTA scans were acquired from the same CT-scanner (Aquilion, Toshiba Medical Systems, Inc., Otawara-shi, Japan). The scan and reconstruction parameters were as follows: helical acquisition, Matrix 512×512mm, slice thickness 1mm, kVp 120V, 300mA, FOV 320×320mm, 130ml non-ionic iodinated contrast medium with an iodine content of 300mg/ml at an injection rate of 4ml/s (Iomeprol, Iomeron 350®; Bracco International, Milan, Italy).

(a) and (b) represent cross-sectional images of CT scans from the same patient before and after endovascular aortic repair. (c) displays the reconstructed surface of the patient's dissected aorta. Apart from the primary entry, there are several small re-entries along the abdominal aorta (there were no arrows pointing at the descending aorta, if there were also re-entries in the descending aorta you can write descending and abdominal aorta), a few of which are indicated by arrows. Fig 1 (d) displays the reconstructed surface of the true lumen after treatment. The configuration of the stent-graft and enlargement of true lumen diameter can be appreciated.

(a) represents the true lumen of the studied case and its stented segment (arrow pointed) that has been used for computation. (b) displays the calculated centreline of the stent-graft. (c) represents the stent-graft surface at the initial stage. The lower panel of this picture shows the triangular mesh applied on the stent-graft surface.
The segmentation and surface reconstruction of the aortic dissection were accomplished by a semi-automatic threshold- based segmentation tool (Amira 5.4, Visage Imaging Inc., USA). Detailed views of the reconstructed surface of the aorta are shown in Fig. 1c-d. In Fig. 1c, apart from the primary entry, several re-entry tears are presented along the flap that connects the true and false lumina, and allows for flow exchange between them. Post treatment, as shown in Fig. 1d, a stent-graft was placed distal to the left subclavian artery, covering the primary entry entirely.
In order to study stent-graft deployment effects, we artificially separated the true and false lumen and selected the stented region for further simulation (Fig. 2a). As shown in Fig. 1d, in this case the left subclavian artery was over-stented. To mimic a realistic situation, this artery was removed. The surface of the selected region is discretized with triangular meshes, with a total of 80,000 elements and 40,202 nodes. The original shape of the stent-graft is modelled as a cylinder (Fig. 2c), with an approximate length of 166mm (according to Fig. 1d) and an initial radius of 1.24mm. It is positioned along the centreline of the true lumen segment (Fig. 2b) at the initial stage and expands towards the radial direction during deployment. The surface of the stent-graft is also discretized with triangular meshes, which have 9,324 cells and 4,680 nodes in total.
In clinical application the stent-graft is folded and unfolds when in position. However, since we focus on its deployed state only, we neglect this unfolding process and simulate its expansion directly. Thus, we assume its initial shape is a cylinder with a radius much smaller than the vessel dimensions.
B. Node Connectivity
The program involves three node sets, which respectively consist of the points on the centre line (Pc), the nodes on the meshes of the stent (Ps) and the aortic wall (Pa). In order to simulate the contact process between the stent-graft and the aortic wall, the node connectivity between those three node sets needs to be identified. In this study, each node i∈Ps on the stent-graft mesh is associated with one, or several, nodes {naorta}
i
⊂ Pa on the aortic wall along its radial direction and the movement of the stent node i is only related to this node subset {naorta}
i
. The program for specifying those node sets involves two tiers. First, the stent-graft mesh is considered as a set of rings and the centre of each ring is located along the centreline. In other words, each point p∈Pc on the centreline corresponds to a group of nodes {i}
p
⊂ Ps of the stent mesh. Thus, the radial expansion direction of each node i on the stent-graft mesh can be identified as
C. Mechanical Properties of the Stent-graft and Aorta
The stent-graft experiences a compressive force before unfolding. Thus, during deployment, it possesses an expansion force along the radial direction towards the aortic wall, which decreases during expansion. When the stent-graft touches the aortic wall, the elasticity characteristics of the vessel wall will present an inward resistant stress towards the expanding stent-graft. The deployment process finishes when the inward stress from the aortic wall and the outward stress from the stent reach a balance or the stent fully expands without contacting any boundary.
In this preliminary study, we assume both the inward stress from the aorta and the outward stress of the stent-graft are related to their deformations along the radial direction only and the variations of both are linear. This indicates σa = Kaδ
a
and σ
s
= σ0 - Ksδs, where K denotes the elastic coefficient of the material along the radial direction, δ denotes the radial deformation, σ
0
represents the initial compressive stress experienced by the folded stent-graft and the subscripts a and s denote the parameters for the aorta and stent respectively. At this initial stage of our study, the aortic wall and stent-graft are assumed to present isotropic and linear elastic properties, indicating
Much effort has been invested in revealing the elastic properties of the aortic wall due to correlations with aging and certain diseases [14-17]. The Young's modulus of the vessel wall is usually estimated based on theoretical models, with hemodynamic and geometric parameters measured in vivo [17, 18]. Mosora et al. report the elastic modulus of the aorta as 2~6.5MPa [19]. Considering a diseased aortic wall is slightly stiffer than a healthy one [20], in our study we assume the elastic modulus of the aortic wall is 5MPa.
Regarding the stent-graft, the Gore TAG device is comprised of an ePTFE graft and a self-expanding nitinol support structure. Most of the mechanical strength of the device comes from its metal structure. The approximate elastic modulus of nitinol at body temperature is known to be 83GPa. However, due to the hollow structure of the stent, its overall elastic modulus is difficult to obtain. The structure of the Gore TAG device consists of several wave-like repeating structures along its longitudinal direction. A possible model estimating the mechanical properties of a nitinol stent proposes that the elastic modulus of the stent can be described as Es = 3Ed4/(8π2nr4) [21], where E denotes the elastic modulus of the material, d denotes the diameter of the wire, r represents half the distance between neighbouring stent cells and n is the number of repeating structures. Considering the device applied in this study, where E=83GPa, d=1mm, r=2.3mm and n=14, the elastic modulus of the stent-graft in our study can be calculated as 8MPa.
It should be noted here that in this preliminary study we focus on simulating the stent-vessel contact process, rather than the unfolding and deployment process of the stent structure. Thus, only the radial displacement of the stent-graft has been considered. In other words, the initial length of the stent-graft (approximately 166mm) is the same as that obtained from the post-interventional image. In real applications the stent-graft presents tangential displacement as well during expansion. More accurate simulations, including both the radial and tangential mechanical properties of the stent-graft, shall be conducted in the future, so that the original length of the stent-graft can be applied.
D. Stent-graft Deployment and Interaction with Vessel Wall
In order to simulate the interaction between the stent-graft and the aortic wall without causing any mesh overlap, we introduced a critical distance (ε =0.05mm) to the program and defined the beginning of contact as when the distance between the stent-graft surface and the vessel wall is smaller than this value. When the contact process has been triggered, if the stent expansion force is larger than the aortic wall resistant force, the aortic wall will move outward. Therefore, until the program is finished, there is always a gap of ε between the stent-graft and the aorta. Since ε is a small value, it ensures both the mesh qualities and the rationality of the model design.
When mechanical contact happened at a particular node i of the stent-graft, it evoked contact computations for the target node set {naorta} i on the aorta. The program obeys the abovementioned mechanical properties and calculates the deformation of node i and the node subset {naorta} i . This regional node movement will subsequently influence other nodes on the aortic mesh. The entire grid over the aortic surface is then re-meshed to ensure the integrity of the model. In order to finish this process within a reasonable time, we employed spring analogy to update the meshes instantaneously. This method replaces the triangular mesh with fictitious springs. The equilibrium lengths of the springs are equal to the initial length of the segments. Hook's Law is applied to the displacement of the nodes. Thus, the force is written as:
where δ i is the displacement of node i and α ij is the stiffness between two adjacent nodes i and j, which is taken to be proportional to the inverse of the segment length:
At static equilibrium of the system, the force at every node i has to be zero. Therefore, the iterative equation to be solved reads:
This approach is applied to each node on the stent-graft and the aortic wall involved in the contact process. The whole program will be repeated until the expansion force of each node on the stent-graft reaches a balanced state with the resistant force of their corresponding node set on the aortic wall.
3. Results
The program finished after 201 iterations in this specific case and took approximately 4 minutes on a PC with an i3 processor. The first contact between the stent-graft and the true lumen occurred at the 39th iteration. This initial contact region is represented in Fig. 3a. After another 162 iterations required to compute the contact process, Fig. 3c displays the deployed configuration of the stent-graft within the true lumen, which indicates that the collapsed true lumen (the studied segment) obtains 13.4% more volume by applying the stent-graft device.
Fig. 3d shows the comparison between the simulated result (indicated by the blue curve) and the reconstructed geometry of the post-interventional CTA. The volume difference of the studied segment between the post-interventional CTA and our preliminary result is small, about 9.1% (small measurement error may exist due to the uneven surface of the stented region). Both the simulated result and the reconstructed model of the post-interventional medical scan show similar trends of stent/aorta expansion distribution. Together with the small volume difference this indicates the rationality of our simulation.

The computational results of stent-graft deployment. (a) displays a snapshot when the stent-graft first contacts the aortic wall (arrow pointing at the contact region). (b) snap-shot during stent-graft expansion (the 113 iteration). (c) displays the configuration of the stent-graft and the aorta at the end of deployment. (d) comparison between the simulated results and the actual stented shape of the aorta based on the post-interventional CTA. The blue curve indicates simulated post-treatment configuration of the true lumen.
Furthermore, in Fig. 4, the stent-graft positions and its deployed dimensions have been represented at certain levels (AA‘ and BB’) of the stented region and have been compared to the post-interventional CTA image. The simulated results present similar geometric features to those shown in the orthoslices in Fig. 4 (simulated results have been indicated by light blue curves). The area difference between the post-procedural CTA and the simulation are 4.3% and 8.1% for level AA‘ and BB’ respectively and same deformation patterns of the vessel have been revealed.
In Fig. 3c, the head of the stent-graft is fully deployed without contacting the aortic wall. This result indicates a lack of apposition of the stent-graft to the aortic wall. In fact, the post-procedural CTA reflects bird-beak configuration in the studied case. As shown in Fig. 5, a wedge-shaped gap between the under surface of the stent-graft and the aortic wall is revealed. Indeed, the detection of the bird-beak configuration is of particular importance in the prediction of adverse clinical events after endovascular repair [22]. Our program, although at this preliminary stage, provides reasonable estimations of the post-interventional stent-graft configuration and therefore, as shown in this case, can help to pre-detect adverse clinical events and therefore assist medical decision-making; the aim of this research.

The comparison of the computational results and the post-interventional CTA. The structure on the left-hand side in yellow is the reconstructed model from the post-interventional CTA. The structure next to it is the simulated expanded aortic geometry. Orthoslices at two levels AA' and BB' are displayed on the right-hand side. Blue curves on orthoslice A and B indicate the corresponding cross-sections of the simulated results.

Bird-beak configuration revealed in the post-procedural CTA. (a) reconstructed surface of the aortic arch in a parasagittal plane. (b) magnified image of the stented region. The arrow points at the area of incomplete apposition of the stent-graft (bird beak configuration).
4. Limitations
This study aims to develop a fast virtual stent-graft deployment algorithm, targeting aortic dissection cases and, within a reasonably short time, to propose simulations of the contact process between the device and the vessel wall. The current initial stage of this study tests the feasibility of the program. However, it also possesses several limitations. First, the stent-graft with metal mesh and fabric is considered as an integrative body. Although the elastic property of the stent mesh has been estimated by its material elasticity, wire thickness and stent cell shape, the mechanical behaviour of the stent-graft has been considered homogeneous. Second, in the current study the algorithm is applied to one aortic dissection case only. Further verification of the rationality of the program requires tests on a wider range of subjects and is dependent on the availability of pre- and post-interventional medical scans of the patients. Finally, the initial length of the stent-graft is assigned the same length as that obtained in the post-interventional image. An improvement of the current preliminary work should involve the tangential displacement of the stent-graft and a more accurate initial length of the stent-graft before deployment.
5. Discussions and Future Works
In this paper we proposed an approach to virtually simulate stent-graft deployment in a Stanford type B aortic dissection. This approach is based on contact mechanics and spring analogy. The motivation to develop this approach is to provide a fast and reasonable method to estimate the stented configuration of the true lumen and therefore assist medical decision-making, such as appropriate device-selection.
The stent-graft applied in aortic dissection reshapes the aortic morphology, indicating that a reasonable simulation of stent-graft deployment must involve the mechanical contact process between the device and the vessel wall. However, true and false lumina in aortic dissection represent extremely complex geometries. This brings great challenges to computational simulations, especially under the conditions of low computational cost and fast execution times.
Finite element analysis has been greatly employed in the studies of stent deployment and its contact with the vessel wall [10, 11, 23]. However, it is relatively computationally costly [24]. With the 3D reconstruction of the vessel wall and detailed geometry of the stent mesh, simulations of the contact process would take several hours or days and may require multiple CPUs. To assist clinical application, faster simulations that can provide reliable information, with a time in order of minutes and that require less computational burdens would be useful.
The current work of this fast virtual stent-graft deployment simulation is designed for endovascular aortic repair and is only a preliminary study, which confirms the rationality and feasibility of the proposed approach. Further research would include the various strut patterns of different stents, consider the scalloped flares of the stent-graft's exoskeleton, changes in length of metal mesh during deployment, etc. and incorporate computational fluid studies to present the pre- and post-interventional flow environments. Moreover, apart from validating the results by post-interventional medical scans, a comparison of the corrected morphology of the aorta simulated by the fast algorithm and the finite element analysis should be conducted so that detailed mechanical patterns occurring on the vessel wall could be studied and the rationality of the fast algorithm could be further validated.
Footnotes
6. Acknowledgements
This work was supported in part from the European Community's FP7/2007-2013, grant agreement number 224495 (euHeart project), the Excellent Young Scholars Research Fund of BIT (3160012261201) and the National Nature Science Fund of China (31200704).