Abstract
Background
The predictive value of preimplantation biopsies for long-term graft function is often limited by conflicting results. The aim of this study was to evaluate the influence of time-zero graft biopsy histological scores on early and late graft function, graft survival and patient survival, at different time points.
Methods
We retrospectively analyzed 284 preimplantation biopsies at a single center, in a cohort of recipients with grafts from live and deceased donors (standard and nonstandard), and their impact in posttransplant renal function after a mean follow-up of 7 years (range 1–16). Implantation biopsy score (IBS), a combination score derived from 4 histopathological aspects, was determined from each sample. The correlation with incidence of delayed graft function (DGF), creatinine clearance (1st, 3rd and 5th posttransplant year) and graft and patient survival at 1 and 5 years were evaluated.
Results
Preimplantation biopsies provided somewhat of a prognostic index of early function and outcome of the transplanted kidney in the short and long term. In the immediate posttransplantation period, the degree of arteriolosclerosis and interstitial fibrosis correlated better with the presence of DGF. IBS values between 4 and 6 were predictive of worst renal function at 1st and 3rd years posttransplant and 5-year graft survival. The most important histological finding, in effectively transplanted grafts, was the grade of interstitial fibrosis. Patient survival was not influenced by IBS.
Conclusions
Higher preimplantation biopsy scores predicted an increased risk of early graft losses, especially primary nonfunction. Graft survival (at 1st and 5th years after transplant) but not patient survival was predicted by IBS.
Keywords
Introduction
Facing the reality of the scarcity of kidney donors, preimplantation biopsies (PIBs; time-zero biopsies) are commonly used to refuse a potential deceased donor or to decide whether a single versus double kidney transplantation (KTX) should be performed (1). However, a lack of information about the prognostic importance of these findings in follow-up still remains, and their predictive value regarding long-term graft function often shows conflicting results (2–5). We aimed to analyze the baseline biopsy histological findings, together with patient and donor characteristics, to determine if there were any correlations that could predict long-term outcomes (renal function and graft and patient survival).
Methods
Selection of patients
We analyzed 601 successive kidney transplants (from brain death or live related donors) performed at the Agostino Gemelli Policlinic (Sacred Heart Catholic University, Rome, Italy) between January 1997 and July 2012, using data retrieved from clinical charts. In 284 cases (47%), a PIB had been performed. For each biopsy, a semiquantitative scale previously reported by Karpinski et al (6) and used by Remuzzi (1, 7) was used to obtain intensity (from 0 to 3), of glomerular sclerosis (GS), arteriolosclerosis (AS), interstitial fibrosis (IF) and tubular atrophy (TA). We noticed that around two thirds of biopsies, in each category of histopathological feature (GS, IF, AS or AT), presented grade 0 (absence of pathological findings). The sum of the 4 degrees was named the implantation biopsy score (IBS) (1). To establish comparisons, we determined 2 groups according to IBS: 1 with lower Remuzzi scores, under 4 (IBS 0–3), and another with higher IBS, equal to or greater than 4 (IBS 4–6), with 6 the highest score accepted.
Endpoints
Primary end points were death-censored 5-year graft survival; secondary end points were overall graft and patient survival. Except where indicated, graft losses were censored at death. Minimum follow-up was 1 year; maximum 16 years.
Clinical data
Demographic aspects of recipients and their respective donors (age, sex, weight, height, body mass index) were determined for each donor-recipient pair. Dialysis antecedents were recorded (cause of chronic kidney failure, dialysis duration, re-transplant). Previous diabetes, hypertension or dyslipidemia diagnosis were according to current standard literature definitions (8,9). Donor death cause was registered; cerebrovascular accidents (CVA) included ischemic or hemorrhagic events. Cold ischemia time (CIT) and sum of HLA mismatches for broad antigens of locus A, B and DR serotypes are shown. Creatinine clearance was estimated (estimated glomerular filtration rate [eGFR]) in donors by Cockcroft-Gault formula (at procurement) (10); in recipients, by the abbreviated Modification of Diet in Renal Disease (aMDRD) study equation (at 1st, 3rd and 5th year) (11). Delayed graft function (DGF) was defined as need for dialysis after kidney transplantation (4,12). Immediate graft function was the lack of postoperative dialysis need (4). Primary nonfunction was a never-functioning kidney after transplant, in which dialysis was never discontinued.
Donor classification
Donors were standard or nonstandard; the latter was defined according to the standard for an expanded criteria donor (ECD), which followed United Network for Organ Sharing (UNOS) criteria (age >59 years; or age 50–59 years, PLUS 2 of the following: death caused by cerebrovascular accident [CVA], terminal creatinine >1.5 mg/dL or history of hypertension) (13). We also determined deceased donor score (DDS) which considers 5 donor characteristics and points to each variable, which are then classified into grades (A = 0–9 points; B = 10–19; C = 20–29; and D = 30–39), with grades C and D considered as “marginal” donors (14).
Histological evaluation
Criteria for sample validation were based on glomerular count (≥20, or at least 10 in each kidney from same donor). Biopsy samples were almost always obtained by wedge section; results in ECDs were available at time of organ allocation and helped to accept/reject a donor. Before 2009, readings were performed by each donor center (i.e., the local pathologist); after 2009, donor biopsies were obtained and send to a centrally based pathologist. Readings were from frozen slides, with 2 to 4 hematoxylin-eosin (H&E)-stained sections available for review. The remnant specimens were postfixed in formalin and paraffin-embedded (FFPE) and revaluated with H&E, periodic acid—Schiff, Wright and Masson's trichrome stained sections in all samples in the daily routine.
Statistical analysis
Categorical variables were compared using chi-square and numerical with Student's t-test. Histological grades are discrete variables, but were considered as continuous for statistical analysis, as in previous similar works (4, 15). Correlations for 5-year death-censored graft survival were evaluated by Cox regression and diagnostic accuracy by area under the receiver operator characteristic curve (AUC ROC). Patient and graft survival were analyzed using the Kaplan-Meier method. A p value of 0.05 or less was considered significant.
Bioethical aspects
This was a retrospective study and no intervention was planned before or after study concept. At time of inclusion in the waiting list and at the moment of transplant, informed consent (previously approved by the local ethics committee) was appropriately presented and signed to permit patients to be submitted to any of the proposed interventions, using immunosuppressive protocols approved by the ethics committee of the Catholic University of Rome. Patients were adequately informed by the transplant multidisciplinary team and were free to participate or remove their consent at any of the phases.
Results
Implantation biopsy scores can theoretically vary from 0 (normal kidney) to 12 (remarkable, severe alterations), but an IBS of 7 or more indicates nonviable kidneys (7), so scores in our cohort varied from 0 to 6 because study biopsies included only kidneys accepted for transplant and effectively implanted. Karpinski score for implantation biopsies was originally created for deceased donors; we obtained a cutoff value for IBS plotting all of the values among deceased donors and establishing an AUC ROC. We noticed that the score value 3 had the higher sensitivity and specificity in determining graft loss (AUC = 0.674, p = 0.04); at the same time, we noticed that among live donors (which would be the gold standard for biopsy findings), only 1 zero-hour biopsy had a score of 4.
Demographic characteristics
Table I shows demographic characteristics for each group of recipients (group IBS 0–3: n = 251; group IBS 4–6: n = 33). Mean age among group IBS 4–6, which concentrates ECD, was higher. This agrees with our regional allocation policy, in which old donors can be preferentially allocated to older recipients. Other studied characteristics are available in Table I, but differences between IBS 0–3 or IBS 4–6 were not significant. Donor age and history of hypertension were higher in group 2. Nonstandard donors (by ECD or DDS definitions) were higher in the group with higher IBS values. However, donor creatinine levels (i.e., eGFR at time of allocation), as other donor characteristics, were similar among groups (Tab. I).
Kidney transplant recipient and donor characteristics according to groups defined by implantation biopsy score (IBS)
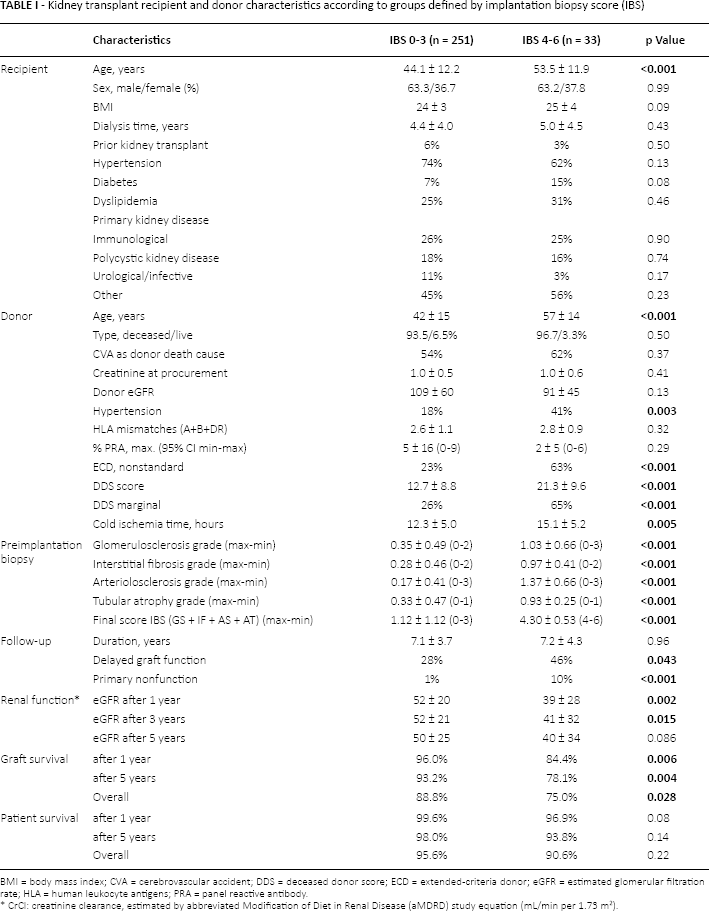
BMI = body mass index; CVA = cerebrovascular accident; DDS = deceased donor score; ECD = extended-criteria donor; eGFR = estimated glomerular filtration rate; HLA = human leukocyte antigens; PRA = panel reactive antibody.
CrCI: creatinine clearance, estimated by abbreviated Modification of Diet in Renal Disease (aMDRD) study equation (mL/min per 1.73 m2).
Donor quality score systems
Sixty-three percent of donors with IBS 4–6 were defined as ECD according to UNOS classification, versus 23% among IBS 0–3 (p<0.001). In our cohort, ECD and DDS were able to predict graft function in all proposed time points (at time of discharge, 6th month, 3rd and 5th year after transplant; data not shown). Relative risk (RR) of graft failure during follow-up (overall) for presence of ECD was 2.3 (p = 0.028, 95% confidence interval [95% CI], 1.1–4.9), and for DDS, 3.3 (p = 0.001; 95% CI, 1.6–7.3). Only DDS (but not ECD) increased RR for patient survival during overall follow-up (RR = 3.5; p = 0.028; 95% CI, 1.1–11.4). Cold ischemia times were superior in group IBS 4–6.
Delayed graft function
DGF was present in 46% of ECD and 28% of standard donors (chi-square p = 0.043, RR 2.1, CI 95% 1.01–4.7). DGF was present in 30% of patients (higher when IBS 4–6); primary nonfunction was higher among IBS 4–6. See Table I for p values. Considering the 4 components of time-zero scores, interstitial fibrosis (IF) of any grade (41.6 vs. 25.8% arteriolosclerosis (AS) IF = 0; p = 0.018, relative risk [RR] = 1.8,95% CI, 1.1–3.1), presence of AS of any grade (53% vs. 23.6% with AS = 0; p<0.001, RR = 3.6, 95% CI, 2.0–6.5) and presence of a final time-zero score above or equal to 4 (46.7% vs. 28.6% for final score <4; p = 0.043, RR = 2.2, 95% CI, 1.0–4.7). DGF and presence of any grade of GS or TA were not significant. Time of CIT longer than 18 hours was associated with DGF (55.6% vs. 26.5% when CIT was <18 hours; p<0.001, RR = 3.4, 95% CI, 1.7–7.1).
Follow-up data
Duration of observation period in years was similar in both groups. Graft function at different times after transplant was estimated by aMDRD function as shown in Table I. In the IBS 0–3 group, eGFR was superior in the 1st, 3rd but not the 5th year. Graft survival (death censored at 1st and 5th year) and graft survival during the study were superior in group IBS 0–3. However, regarding patient survival, differences between groups do not persist (Tab. I).
Implantation biopsy scores: sensitivity and specificity
In 3 situations we analyzed the ability of IBS performance to identify (A) suboptimal donors (nonstandard donors), (B) worst creatinine clearances at discharge after KTX (grades IV-V, eGFR by aMDRD under 30 mL/min) and (C) prediction of graft and patient outcomes at 5 years. In all 3 situations, we saw that IBS ≥4 (or IBS 4–6) presented low sensitivity (SENS) but high specificity (SPEC): (A) SENS 25%, SPEC 94%, odds ratio (OR) P = 5.4 (95% CI, 2.4–12.3), p = 0.001; (B): SENS 28%, SPEC 93%, OR = 5.5 (95% confidence interval (CI), 2.4–12.2), p<0.001; (C) predictive for graft, but not for patient survival; SENS 21%; SPEC 90%, OR = 2.7 (95% CI, 1.1–6.9), p = 0.03. Performance of donor creatinine above 1.5 mg/dL and Creatinine clearance under 55 mL/min in predicting A, B and C outcomes also presented high SPEC and low SENS. Traditional criteria of donor creatinine >1.5 mg/dL (used with other elements) to declare a procured donor as a nonstandard donor, did not predict graft function, graft survival or patient survival. IBS showed a better profile in terms of OR. Regarding survival outcomes, only IBS was able to predict graft losses at 5 years (estimated relative risk of graft loss was 2.7). No donor characteristics predicted patient survival well (see below).
Correlations for death-censored graft survival and accuracy
We analyzed the demographic, clinical, preimplantation biopsies (PIB) features shown in Table I, selecting only those variables that were originally statistically significant among groups. The results can be seen in Table II. We performed a univariate Cox regression considering the whole cohort (284 patients) for each characteristic to identify the hazard ratios (expected beta-value) and respective p values in predicting 5-year death-censored graft survival. For all characteristics, diagnostic accuracy was estimated by c-values (determinate by AUC ROC). In this setting, one can observe that there are many characteristics that are correlated with graft survival, once the p value of Cox analysis is significant. For PIBs, grade of GS, IF and final IBS (GS+IF+AS+AT) showed a significant correlation with 5-year death-censored graft survival. However, significant diagnostic accuracy was shown only for donor history of hypertension, DDS score “marginal,” grade of IF on PIB, group of IBS score and primary nonfunction. Grade of IF presented the highest c-value (0.77) among these variables. Among demographic characteristics, only age of recipient was accurate accurately correlated with 5-year patient survival (c = 0.89, p = 0.02, data not shown). Other advantages of organ quality information to physicians given by PIBs are available online. We present a prediction model of graft survival using biopsy data among other characteristics (Supplementary Tab. I and Fig. 1, available online at www.pointofcarejournals.com/poc/napoc).
(
Correlations for 5-year death-censored graft survival (Cox regression) and diagnostic accuracy (AUC ROC)
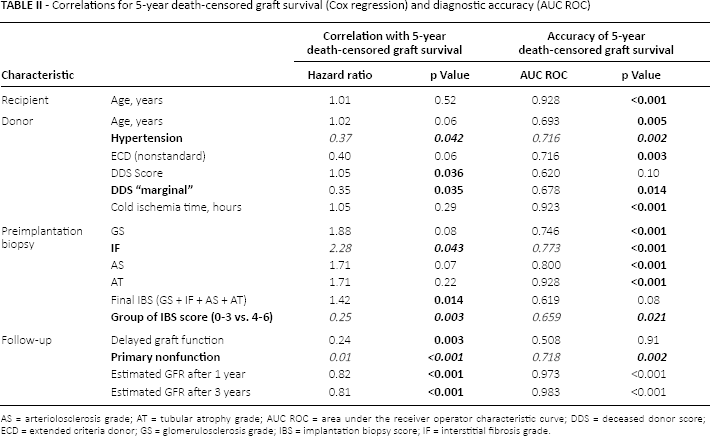
AS = arteriolosclerosis grade; AT = tubular atrophy grade; AUC ROC = area under the receiver operator characteristic curve; DDS = deceased donor score; ECD = extended criteria donor; GS = glomerulosclerosis grade; IBS = implantation biopsy score; IF = interstitial fibrosis grade.
Graft survival
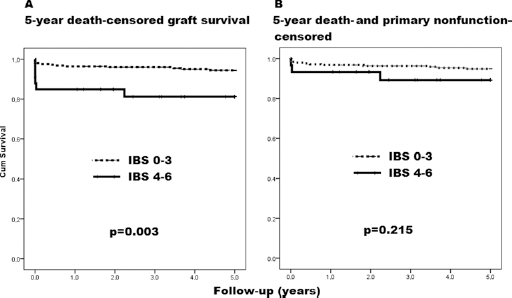
We analyzed 5-year graft survival by Kaplan-Meier analysis, comparing curves between groups IBS 0–3 and IBS 4–6 (Fig. 1). We observes that implantation biopsy scores above or equal to 4 (IBS 4–6) predicted a less favorable graft survival (p = 0.04). A sudden slope before the 1st year was seen during group 2 follow-up, a difference that remained throughout the observation period without significant changes. To explore this finding, we observed the 5-year estimated graft survival, censored for early graft losses, and found that the difference disappeared (Fig. 1). This means that IBS scores are important to predict early graft losses in IBS 4–6, but after these initial losses, the remaining kidneys are lost at a similar rate to that observed in IBS 0–3 during the first 5 years of follow-up.
Discussion
Donor biopsies are useful to give baseline information about histological quality of the donor to make comparisons with subsequent biopsies, helping to discriminate donor-derived lesions from de novo alterations (2). Disparities between need for and availability of organs has increased the use of ECDs (16). In United States, up to 85% of procured ECD kidneys are biopsied (2,17). High grade of glomerulosclerosis is a good predictor of early graft dysfunction (3), so this finding usually leads to organ discharge (18). Despite glomerulosclerosis is an important feature to allocation decision (1), its grade in effectively transplanted kidneys does not seem to be predictive of DGF or long-term kidney function in our series. This is probably an effect of organ procurement practices, selecting better GS scores, avoiding an effect on graft outcome (5, 15). Better prognostic information is given in specific donor subsets (older donors, with hypertension, diabetes, cardiovascular disease or abnormal creatinine) (3,19). In our study, the presence of interstitial fibrosis correlated well with worst results in long-term graft survival (chi-square p = 0.029; RR = 2.23; 95% CI, 1.07–4.64). These findings are similar to those of Lopes et al (15), who found a positive correlation between IF and serum creatinine at 3 and 6 months but no correlation with TA, GS or AS.
Many authors assume that none of the histological variables and scores provide perfect predictions and so results should be interpreted in the context of all available information on donor-recipients (2, 18). A histological score is not the first test used during organ procurement to accept a kidney, but it is used successively to discard one. To establish a prediction ability for IBS score, we needed a cutoff value that could reflect a high specificity (even losing sensitivity to some extent). Some arguments against routine time-zero biopsies are that the performance of the PIB itself can increase the odds of a discard (2, 20) or that the procedure itself generates a further delay in the graft implantation (for collection, process and interpretation), increasing the cold-ischemia time and the risk of DGF (2, 21). Most of recent papers describe the experience in performing PIBs among ECD donors. The strongest point of this work is that PIB was performed not only among ECDs, but also in standard deceased donors. A biopsy in this case was able to identify that at least 5.8% of “standard” deceased donors according to UNOS classification have in fact a histological score ≥4 (11/189). We also observed that ECD donors have a 5 times higher risk of having a preimplant score above 4 when compared with non-ECD donors (p<0.001; RR = 5.5; 95% CI, 2.4–12.3). Using the DDS score (14), we obtained very similar results (5.2% of “standard” deceased donors with final score >4 [9/173]; p<0.001; RR = 5.4; 95% CI, 2.3–12.8).
DGF can be predicted by PIB (5); it increases morbidity and may lead to premature graft failure, longer hospitalization and higher health care costs (this is especially true among ECDs). Regarding the better performance of nonstandard donor scores, we determined the AUC ROC comparing ECD or DDS classification, using final histological score above 4 as the state variable; both AUC ROC were similar (r = 0.695 for ECD and r = 0.698 for DDS, p = 0.001 for both). The same comparison was made using graft outcome at the end of follow-up as state variable; again AUC ROC were similar (c = 0.643 and c = 0.642, p = 0.012 and p = 0.013, for ECD and DDS, respectively). ROC curves for IBS ≥4 present a low c value. However, IBS hallmark information is due to its specificity, which is higher enough that alone it can predict early graft function and long-term graft survival. Another piece of information about IBS is that the SENS of IBS scores ≥4 are 2 to 3 times higher than the SENS of donor creatinine in predicting acute dysfunction. Concluding, our results showed that the most important isolated histological finding, in effectively transplanted grafts, is the grade of IF. IBS 4–6 can determine an increased risk of early graft loss, especially primary nonfunction. Higher IBS grades predict lower graft function until the 3rd postoperative year; but in this cohort is not able not predict graft function at the 5th postoperative year, after this, we probably need a higher number of patients to demonstrate the difference (numerically but not statistically different). Possibly, as graft survival advances, recipient characteristics (including therapy, immunological events and comorbidities) could gain more importance in determining renal function, surpassing any influence of IBS. Moreover, IBS predicts graft survival at 1 and 5 years after transplant, but does not predict patient survival.
A last word about PIBs in live donors. Nowadays, biopsies can be considered a graft survival prediction tool, with high specificity (despite a low sensitivity). Since the cyclosporine era of immunosuppression, we have dramatically reduced the impact of allograft acute rejections, remaining with late losses due to chronic allograft dysfunction (25). This has become the most important problem in solid organ transplants, mediated by a myriad of etiopathological mechanisms and without specific treatment (22, 23). To obtain complete information about chronicity findings at long-term follow-up, a baseline biopsy is essential. This includes the need to perform biopsies not only in deceased ECDs, but also among living elderly donors, young living donors or deceased standard donors (24). Virtually any type of donor can have unsuspected disease (GS, glomerulopathy, chronic vascular disease/AS, TA or IF) only revealed by a PIB. So, presentation of both donor types was intentional, not done unawares. Despite the fact that this was a small proportion of cases (<5% of studied patients), live donors were intentionally included to stress the importance of performing PIBs even in them. Table I shows there was no difference between deceased/live donor proportion (6.6% vs. 3.3%) among groups (chi-square p = 0.5).
Footnotes
Financial support: No grants or funding have been received for this study.
Conflict of interest: None of the authors has any financial interest related to this study to disclose.
