Abstract
Purpose
To raise awareness of ophthalmologists that toxoplasmosis should be considered in the differential diagnosis of multifocal or diffuse necrotizing retinitis in nonimmunosuppressed elderly patients.
Methods
Interventional case report with serial color fundus photographs, indocyanine green angiography, fluorescein angiography, optical coherence tomography, and chorioretinal biopsy histology.
Results
A 77-year-old, nonimmunosuppressed man developed extensive multifocal retinochoroiditis with scattered focal hemorrhages and significant vitreous haze. This case posed a significant diagnostic challenge mimicking viral retinitis. Vitreous polymerase chain reaction and chorioretinal biopsy confirmed the diagnosis of toxoplasma retinochoroiditis.
Conclusions
As demonstrated in this case, toxoplasmosis should be considered as a cause of multifocal and/or diffuse necrotizing retinitis in elderly patients even in the absence of obvious systemic immunosuppression.
Keywords
Introduction
Toxoplasma retinitis is the most common cause of posterior uveitis and infectious retinochoroiditis in adults and children, with a lifetime occurrence of approximately 2% of the population (1). As such, ophthalmologists need to be vigilant in rapidly detecting and treating ocular toxoplasmosis before it leads to loss of vision. In the nonimmunosuppressed host, toxoplasma retinitis typically presents as a unifocal lesion with rapid-onset vision loss; in immunosuppressed patients, toxoplasma retinitis can be multifocal, mimicking viral retinitis (2-3-4). We present an atypical case of multifocal toxoplasma retinochoroiditis in a 77-year-old man without known immunosuppression, and describe the diagnosis and treatment course for this case.
Case report
A 77-year-old man was referred from an outside retina physician with a 2-month history of worsening right eye retinitis that did not respond to empirical treatment with a 2-week course of oral corticosteroids and famciclovir. His associated medical conditions included hyperlipidemia, benign prostatic hyperplasia, and gastroesophageal reflux disease. However, the patient had undergone systemic physical examination and a complete metabolic profile including creatine and blood sugar assessments, which were normal. His complete blood count with differential was also within normal limits. There was no known medical history of malnutrition and MRI of the brain was nonrevealing. His surgical history and family history were noncontributory. His ocular history was remarkable for retinitis in his right eye approximately 4 years prior to presentation, but without a confirmed diagnosis and a poor response to empirical antitoxoplasmosis therapy. At the time of presentation, serum toxoplasmosis immunoglobulin M was negative, but immunoglobulin G was positive at 87 IU/mL (upper limit of normal, 8 IU/mL). Rapid plasma reagin for syphilis, purified protein derivative for tuberculosis, chest x-ray, and antinuclear antibody tests were all nonrevealing.
On examination, the right eye detected only hand movement, and corrected vision with habitual refraction of the left eye was 20/25. Pupils were minimally reactive in the right and briskly reactive in the left. Intraocular pressure was normal in both eyes. Slit-lamp revealed quiet sclera/conjunctiva, clear corneas, and deep and quiet anterior chambers. The right eye was pseudophakic with a 3+ vitreous haze score, and the left eye had nonsignificant cataract with no vitreous inflammation. Fundus examination of the right eye showed multifocal superotemporal chorioretinal infiltrates with scattered foci of hemorrhage and areas of chorioretinal pigmentation and atrophy inferiorly as well as an atrophic pale optic disc (Fig. 1A). The left eye fundus examination was normal apart from a small white nonpigmented atrophic scar; there was no sign of active posterior uveitis (Fig. 1B). Indocyanine green angiography (ICG) revealed widespread hypocyanescent lesions mainly attributed to loss of choroid tissue with some leakage noted from the choroidal vessels around the disc of the right eye (Fig. 1C), and an isolated hypocyanescent area adjacent to the superior arcade in the left eye, which corresponds to the nonpigmented atrophic scar seen on the color fundus photograph (Fig. 1D). Optical coherence tomography examination revealed diffuse atrophy and disorganization of retinal layers of the right eye with loss of optic nerve groove (Fig. 1E) and was normal in the left eye (Fig. 1F). Fluorescein angiogram in the right eye was consistent with areas of blocked fluorescence with some late leakage superotemporally and areas of window defect inferiorly (Fig. 1G).
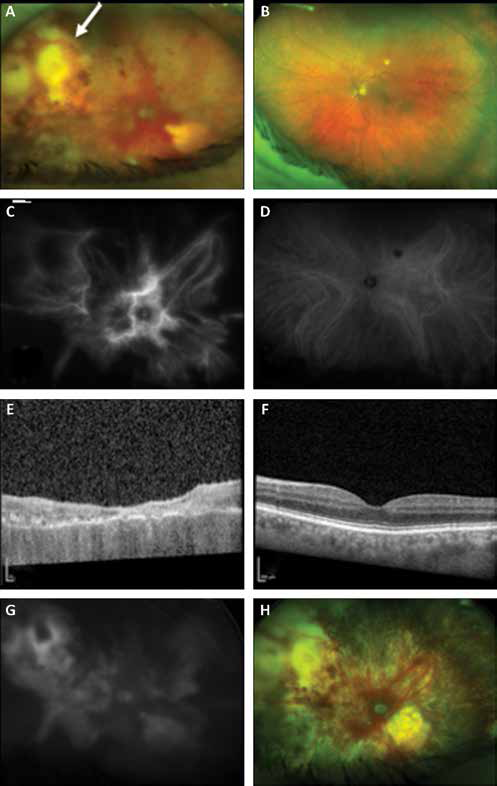
(
To maximize the chance of establishing a diagnosis, simultaneous vitreous and chorioretinal biopsies were undertaken; because of the poor visual potential of the right eye, the potential risks of chorioretinal biopsy surgery in this patient were considered to be minimal. Vitreous biopsy results were negative for cytomegalovirus, herpes simplex virus 1 and 2, and varicella-zoster virus on polymerase chain reaction (PCR), but were positive for Toxoplasma gondii on PCR at 220,000 DNA copies/mL. Flow cytometry analysis showed no evidence of abnormal lymphoid populations. Histologic sections of the chorioretinal biopsy revealed rare cyst forms (20-μm diameter) containing basophilic dot-like structures within the retina, consistent with toxoplasma bradyzoites (Fig. 2). A predominantly plasma cell inflammatory response was seen in the retina as well as a non-necrotizing granulomatous inflammatory reaction with surrounding marked lymphocytic inflammatory infiltrate in the choroid, showing a mixed T-cell (CD3-positive) and B-cell (CD20-positive) immunophenotype. Immunohistochemical stain of the chorioretinal biopsy section for T gondii was positive, highlighting 2 intraretinal cyst forms.
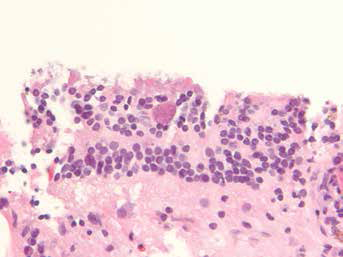
Histologic study of a chorioretinal biopsy revealed rare cyst forms (20 μm in diameter) containing basophilic dot-like structures within the retina, consistent with toxoplasma bradyzoites. A predominantly plasma cell inflammatory response was seen in the retina as well. Hematoxylin & eosin stain, original magnification ×400.
Treatment was commenced with oral trimethoprim/sulfamethoxazole but was switched to oral clindamycin 300 mg QID after 1 week due to worsening of the retinitis and vitreous haze. This change in treatment, as well as the addition of repeat injection of intravitreal clindamycin (1 mg in 0.1 mL), resulted in complete regression of retinitis (Fig. 1H).
Discussion and review of literature
This case of ocular toxoplasmosis is of particular interest due to its unusual phenotypic presentation. Our patient presented with multifocal toxoplasma retinitis, which is not common and is most often seen in immunosuppressed patients; however, he showed no signs of immunosuppression.
It is thought that this association between atypical toxoplasmosis and nonimmunosuppression in elderly patients might be at least partially explained by an age-related decline in T-cell-mediated immune responses as well as possible nutritional deficiencies (5). Increased age has been found to be a risk factor in patients with primary ocular toxoplasmosis but not in recurrent disease. Ongkosuwito et al (1) showed that patients with primary ocular toxoplasmosis were older (median age 44 years; range 14-76 years) than patients with recurrent ocular disease (median age 32 years; range 11-67 years) (p = 0.005).
There are few documented cases in the literature where toxoplasmosis retinitis presented in nonimmunosuppressed elderly patients in a diffuse or multifocal pattern. One retrospective case study showed that of 9 patients with PCR-confirmed atypical toxoplasma retinitis, 8 patients were systemically immunosuppressed, while 1 patient, an 86-year-old woman, had no obvious cause of immunosuppression (2). A separate study reviewed case studies for 7 initially presumed immunocompetent elderly patients with atypically severe (multifocal or diffuse or both) toxoplasmic retinochoroiditis with an age range of 69 to 82 years (median 74 years) (6). While 3 of the 7 patients had intercurrent medical conditions that may be associated with subtle immune dysfunction (diabetes mellitus and hepatitis C), 4 had no obvious cause of systemic immunosuppression (6).
Conclusion
The case presented in this article, as well as the other sparse cases reported in the literature, draw attention to the fact that toxoplasmosis could be a cause of multifocal necrotizing retinochoroiditis that can mimic viral retinitis in elderly patients even in the absence of immunosuppression.
Footnotes
Financial support: No financial support was received for this submission.
Conflict of interest: None of the authors has conflict of interest with this submission.
