Abstract
Purpose
To report a case of Purtscher-like retinopathy associated with travel at high altitude.
Methods
Case report.
Results
A 67-year-old man presented 2 weeks after acute vision loss in his left eye that occurred while he was hiking in the mountains of South America. Funduscopic examination revealed multiple cotton-wool spots and discrete areas of retinal whitening. Fluorescein angiography demonstrated areas of choroidal fluorescence blocked by retinal whitening, delayed arteriovenous transit time, and late capillary leakage. Spectral-domain optical coherence tomography showed hyperreflectivity in the inner plexiform, inner nuclear, and outer plexiform layers localized to the areas of retinal whitening. These findings were believed to be most consistent with Purtscher flecken, and the patient was diagnosed with Purtscher-like retinopathy.
Conclusions
Purtscher-like retinopathy may be linked to travel at high altitude through retinal vessel dilation and constriction leading to retinal vasospasm and precapillary arteriole occlusion. This proposed mechanism of pathogenesis suggests that Purtscher-like retinopathy may represent a partial central retinal artery occlusion.
Introduction
Purtscher retinopathy is characterized by unilateral or bilateral vision loss ranging from minimal impairment to hand motion acuity that develops within 48 hours after an inciting traumatic event (1). The term Purtscher-like retinopathy is used to describe such presentations not associated with trauma, including acute pancreatitis, renal failure, childbirth, connective tissue disorder, autoimmune disease, and fat embolism syndrome (1).
Fundus findings are typically confined to the posterior pole and include areas of inner retinal whitening known as Purtscher flecken, cotton-wool spots, retinal hemorrhage, and optic disc swelling (1, 2). These findings respect the vascular distribution of the affected areas. On fluorescein angiography (FA), capillary or retinal arteriole nonperfusion, delayed vessel filling, early hypofluorescence, and late leakage are among the most prevalent findings (1). Spectral-domain optical coherence tomography (SD-OCT) demonstrates hyperreflectivity in the inner retina, specifically the inner plexiform, inner nuclear, and outer plexiform layers (3).
We present a case of a 67-year-old man who developed acute monocular vision loss after high altitude exposure and was found to have examination findings most consistent with Purtscher-like retinopathy.
Case report
A 67-year-old man presented 2 weeks after acute vision loss in his left eye. He reported vision loss in his left eye upon awakening 2 days after descending to 3,000 meters from 4,600 meters while hiking in South America. There was no associated eye pain, photophobia, redness, or history of transient visual loss. He denied any falls or other trauma while hiking. The patient had a history of ocular hypertension in the right eye and was followed by a glaucoma specialist; he was prescribed timolol but had not taken it for several months at the time of presentation. Also of note, his glaucoma specialist found no evidence of buried disc drusen on prior visits. His medical history was significant for untreated borderline hypertension and benign prostatic hyperplasia. He had no history of stroke, cardiac disease, hypercholesterolemia, diabetes, or smoking.
The patient's Snellen visual acuity was 20/20 in the right eye and count fingers (pinhole 20/200) in the left eye. A relative afferent pupillary defect was present in the left eye. Intraocular pressure was 20 mm Hg in both eyes and anterior segment examination was unremarkable. Funduscopic examination of the left eye revealed several cotton-wool spots scattered throughout the posterior pole and discrete areas of perifoveal retinal whitening with arteriole attenuation (Fig. 1A). The perifoveal areas of retinal whitening were polygonal in shape with a clear zone between affected retina and adjacent arterioles or venules, consistent with Purtscher flecken. Fluorescein angiography demonstrated areas of choroidal fluorescence blocked by retinal whitening, delayed arteriovenous transit time, and late leakage from retinal vessels in areas of ischemia (Fig. 1, B-D). High-resolution SD-OCT showed localized thickening and perifoveal hyperreflectivity in the inner plexiform, inner nuclear, and outer plexiform layers corresponding with the areas of retinal whitening (Fig. 2A). The right eye was unremarkable. Given these findings, the diagnosis of retinal ischemia due to suspected Purtscher-like retinopathy was made.
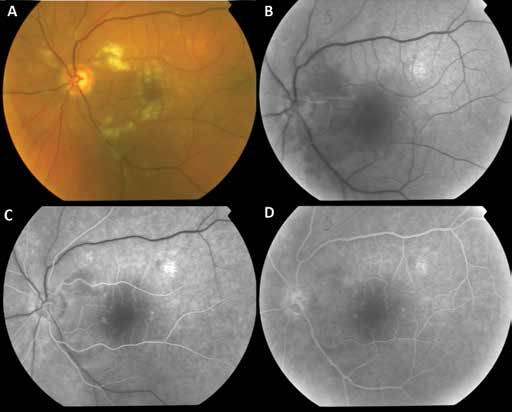
Color fundus photography and fluorescein angiography of the left eye at presentation. (
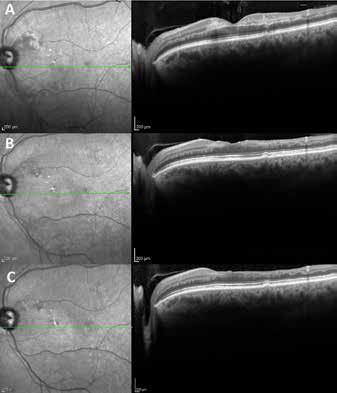
Spectral-domain optical coherence tomography of the left eye. Optical coherence tomography (
Additional laboratory work (complete blood cell, erythrocyte sedimentation rate, C-reactive protein, hemoglobin A1c) returned within normal limits. Echocardiogram and carotid ultrasound were also unremarkable.
The patient chose to pursue treatment with alternative medicine and received several sessions of acupuncture. His vision improved to 20/400 (pinhole 20/40) in the left eye at 2 months follow-up. Fundus examination was notable for mottling of the retinal pigment epithelium (Fig. 3) and thinning of the inner retinal layers was seen on SD-OCT (Fig. 2B). At 1 year, his best-corrected visual acuity was 20/50 with progression of the inner retinal atrophy on SD-OCT (Fig. 2C).
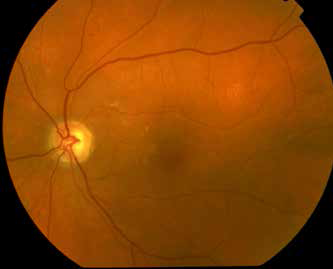
Color fundus photograph at 2 months follow-up shows scattered areas of retinal pigment epithelium mottling.
Discussion
Although the pathogenesis of Purtscher retinopathy remains controversial, it is thought to involve occlusion of precapillary arterioles (1). This is consistent with clinical descriptions of Purtscher retinopathy affecting the inner retinal layers. Suggested mechanisms of precapillary arteriolar occlusion in Purtscher retinopathy include microembolization, leukoembolization, capillary endothelial damage, hyperviscosity, sudden intracranial pressure increase, sudden expansion of retinal veins, and retinal arteriolar spasm (1, 4).
High altitude travel induces physiologic changes that may be implicated in the pathogenesis of Purtscher retinopathy: hypercoagulability leading to embolization and retinal vasospasm. Although the underlying mechanism is poorly understood, within the first few hours of high altitude exposure, there is an increase in platelet count, factor X, and factor XII (5). This hypercoagulable state may have predisposed our patient to a thromboembolic event. Alternatively, the retinal vessel dilation and constriction that occurs with hypoxia while traveling at high altitude is well-reported (6, 7). Prospective observational studies have demonstrated that unacclimated hypoxia produces retinal vasodilation, while unacclimated exercise and hyperventilation leads to vasoconstriction (6, 7). Our patient's unacclimated exposure to high altitudes may have resulted in retinal vasospasm. Either of these mechanisms may have led to the development of Purtscher-like retinopathy in our patient. To our knowledge, this is the first report of Purtscher-like retinopathy presenting in association with high altitude travel.
It is important to recognize that findings in Purtscher retinopathy may closely resemble those found in central retinal artery occlusion (CRAO); however, distinct differences exist. When localized around the fovea, the patchy retinal whitening of Purtscher flecken may appear as a pseudo-cherry-red spot and is seen in 26% of Purtscher cases (1). The areas of unaffected retina intervening between areas of retinal whitening in our patient are more consistent with a pseudo-cherry-red spot than the classic cherry-red spot seen in CRAO. While FA in acute CRAO commonly demonstrates delayed filling of the retinal vasculature, late leakage is generally not seen in CRAO (8). Furthermore, although our patient had an OCT revealing patchy areas of increased reflectivity and thickness of the inner retina, CRAO is characterized by these findings diffusely, along with decreased reflectivity in the outer layer and retinal pigment epithelium (8). The findings in our patient make CRAO less likely and are more consistent with Purtscher-like retinopathy.
Although there have been several case reports of CRAO associated with high altitude exposure, these patients had significant risk factors for developing CRAO at high altitude including intraocular gas bubble (9) and buried optic nerve drusen (10). While our patient was at risk for occlusive vascular events given his age >50 years and borderline systemic hypertension, neither of the aforementioned predisposing factors was present in our patient.
A recent case series reported 3 patients with CRAO resembling Purtscher-like retinopathy (11). The authors hypothesized that a partial occlusive event accounted for the patients’ clinical findings and positive visual recovery; this is in contrast to a complete occlusive event, which would produce the classic clinical findings of CRAO and a negative visual outcome. These cases support the theory proposed by Gass (8, 11) that Purtscher retinopathy may actually represent a subtype of CRAO. In this context, our patient likely experienced a partial occlusion event secondary to the retinal vasospasm produced by exertional activity at high altitude presenting as Purtscher-like retinopathy with significant visual recovery.
Visual outcome in Purtscher retinopathy is variable and there are no standardized guidelines for treatment. Spontaneous visual recovery of a minimum of 2 Snellen lines has been reported to occur in 50% of patients (2). It has also been reported that a rapid reduction in retinal edema seen on OCT within the first 8 weeks is associated with a good prognosis for visual recovery (12). In our case, the patient experienced a speedy and dramatic improvement in vision. It is unclear if acupuncture therapy contributed to the improvement or if this represents spontaneous recovery.
We report an unusual case of Purtscher-like retinopathy presenting after travel at high altitude with significant visual recovery in the setting of acupuncture therapy. Retinal vasospasm at high altitude and recovery suggest that the pathogenesis of Purtscher retinopathy is associated with a partial occlusion of the central retinal artery.
Footnotes
Acknowledgement
The authors thank the patient for granting permission to publish this material.
Financial support: No financial support was received for this submission.
Conflict of interest: None of the authors has conflict of interest with this submission.
