Abstract
Background
We report the case of monolateral corneal endotheliitis, which occurred following systemic West Nile virus (WNV) infection.
Methods
A 56-year-old male patient with right eye (RE) endotheliitis, diffuse arthralgias, and diagnosis of previous WNV systemic infection underwent a measurement of best spectacle corrected visual acuity (BSCVA), full ophthalmic examination, biomicroscopy, and in vivo scanning laser confocal microscopy (IVCM), before and after topical immunomodulatory treatment. In addition, a polymerase chain reaction test on aqueous humor was performed to test for WNV RNA sequences.
Results
Photophobia was reported at presentation. A mild corneal haze was noted at the slit lamp exam. BSCVA in RE was 0.1 LogMar, corneal thickness was 667 micron, and confocal microscopy showed stromal folds. No WNV RNA sequences were detected in the aqueous humor. The cytomegalovirus and herpes virus were not tested as the patient refused additional procedures.
One month after topical corticosteroid application in the RE, the patient reported significant improvement in photophobia, BSCVA improved to −0.1 LogMar, and corneal thickness was reduced to 540 microns. In addition, IVCM showed a disappearance of stromal folds.
Conclusions
A presumptive diagnosis of WNV-associated endotheliitis was formulated. Improvement following topical corticosteroid treatment suggests an immune-based pathophysiology.
Introduction
West Nile virus (WNV) is an RNA Flavivirus. Infection is most commonly transmitted to humans through mosquito bites (1). Ocular involvement may occur, most frequently with multifocal choroiditis, retinal vasculitis, and optic neuritis (2). Anterior uveitis was also reported in a single case (3). However, isolated corneal endotheliitis has not been described before.
Here, we describe a case of monolateral corneal endotheliitis following systemic WNV infection, which resolved with topical immunomodulatory treatment. To our knowledge, this is the first reported case of isolated corneal involvement occurring after WNV systemic infection.
Case presentation
A 56-year-old man presented at our Cornea Clinic complaining of blurry vision in his right eye (RE). One year earlier, he had suffered from high fever, diffuse arthritis of the small and large joints, and a nonitching maculopapular rash. WNV infection was diagnosed based on the detection of elevated immunoglobulin-M serum levels and confirmed by a plaque-reduction neutralization test. One month later, he developed blurred vision in his RE, and diffuse arthralgia. An ocular examination that was performed at this time by his ophthalmologist revealed 0 LogMar vision and mild corneal oedema in the RE. The left eye (LE) vision was 0 LogMar, and the clinical exam was unremarkable. Retina and vitreous were reported normal in both eyes (oculi uterque [OU]). Corneal endothelial dystrophy was diagnosed in the RE. The vision in the RE and photophobia worsened over time, to the point he was unable to drive. Approximately 1 year after the symptoms had started, the patient was referred to us. Visual acuity in RE was 0.1 LogMar, and severe photophobia was present. Mild corneal haze with fine Descemet folds was noticed (Fig. 1A, B), but no keratic precipitates or aqueous flare were detected. Hence, we diagnosed endotheliitis in Oculus dexter (OD). oculus sinister (OS) appeared normal, and visual acuity was 0 LogMar (Fig. 1C, D). In vivo confocal microscopy (IVCM, Heidelberg Retina Tomograph II, Cornea module), showed fine stromal folds (Fig. 2A), hyper-reflectivity of the endothelial layer, with poorly defined cell borders (Fig. 2B) in RE; endothelium and stroma in the LE were normal (Fig. 2C, D). Corneal thickness was 667 microns in the RE and 554 microns in the LE. Intraocular pressure was 14 mmHg bilaterally. The remaining ocular exam in the RE, including lens, vitreous, and fundus, was normal. Interestingly, the patient still reported joint pain and stiffness, and reactive (post-viral) arthritis was diagnosed.
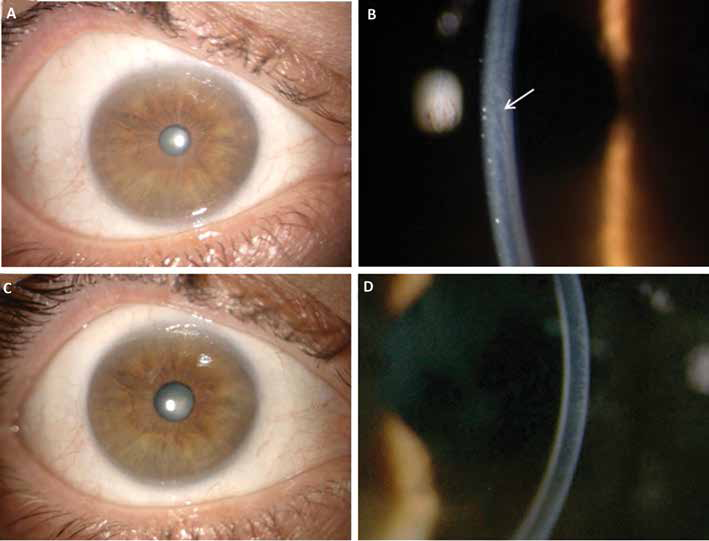
Slit-lamp exam of the affected OD before (
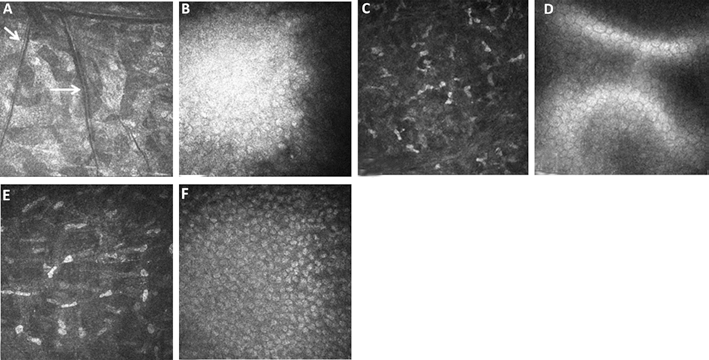
In vivo confocal microscopy images of the corneal stroma and endothelium before (
Therefore, we collected aqueous humor samples, together with blood and urine samples, for WNV detection with real time polymerase chain reaction (RT-PCR) analysis. However, all PCR analyses yielded negative results. Hence, we concluded that the observed endotheliitis may have an autoimmune origin. Topical treatment with dexamethasone sodium phosphate 0.15% 6 times a day in the RE was prescribed and slowly tapered over 1 month. The patient noticed a prompt improvement in his vision within the first 24 hours of treatment. One month later, his vision was −0.1 LogMar and the photophobia had resolved. IVCM revealed that the stromal folds had disappeared, and the endothelium hyper-reflectivity had reduced, suggesting improved endothelial inflammation. (Fig. 2E, F). RE pachimetry was down to 540 microns.
Discussion
WNV infection is a major epidemiologic concern in the Western world. The first case of WNV infection was originally reported in Uganda in 1937. Outbreaks have since been reported in Western countries in the second half of the 20th century. The vast majority of WNV infections are asymptomatic, with severe complications (including meningitis) occurring in approximately 1 out of 150 infected subjects (3). Ocular complications are common and include photophobia, papilledema, chorioretinitis, and conjunctivitis. To the best of our knowledge, no previous report has described the occurrence of ocular endotheliitis after WNV infection. It has been reported that some viruses (i.e., Ebola) can survive in the aqueous humor for months (4). Interestingly, WNV is able to infect human corneal cells (5). Since our patient promptly and effectively responded to topical corticosteroid treatment, we speculate that the pathogenesis may be immune mediated. We acknowledge that it was not possible to rule out herpes or cytomegalovirus infection by performing RT-PCR on aqueous humor samples. Unfortunately, the amount of aqueous humor was not sufficient to test for the presence of cytomegalovirus and herpes, as it was all used for the quantification of WNV, and the patient refused additional procedures. However, history and clinical features of the endotheliitis did not support such etiologies. No nummular endothelial lesions were detected, and the clinical picture improved without the use of antivirals. Finally, ocular symptoms started immediately (1 month) after the clinical onset of the systemic WNV infection. For these reasons, we suggest that WNV should be considered in the differential diagnosis of endotheliitis in patients with confirmed infection and ocular symptoms.
Footnotes
Financial support: No grants or funding have been received for this study.
Conflict of interest: None of the authors has financial interest related to this study to disclose.
